Abstract
Aims and Objectives
Dexmedetomidine is a relatively new, potent, and highly selective α2-adrenergic receptor agonist used for perioperative sympatholytic, analgesia, and sedation. We conducted this study to evaluate the effects of dexmedetomidine as an adjunct to local anaesthesia for maxillofacial soft tissue injuries as day care in the emergency department on patient hemodynamics and analgesic efficacy.
Materials and Methods
Eighty patients gave informed consent to participate in the study. They were divided into Groups P and D, each of which consisted of 40 participants. Patients received saline injections in Group P, and Group D received dexmedetomidine (DEX) with local anaesthesia infiltration to both groups. Hemodynamic parameters, duration of surgery, pain of first rescue analgesia, Pain score, patient satisfaction, and surgeons satisfaction were recorded and quantified using unpaired t tests or Mann–Whitney and ANOVA tests. Data and qualitative data parameters were compared using Chi-square test. A P value < 0.05 was considered significant.
Results
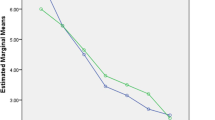
Our study showed statistically significant reduced heart rate, systolic, and diastolic blood pressures in DEX compared to the placebo group where none had hypotension or bradycardia in clinical settings. The dexmedetomidine group had shorter operative time and decreased need for analgesia due to lower VAS scores. Patient and surgeon satisfaction were superior in the DEX group compared to the other groups.
Conclusion
Dexmedetomidine effectively suppresses the hemodynamic stress response during minor surgical procedures. We conclude that dexmedetomidine is an effective medication to be used in the emergency room for day-care procedures, as a potent analgesic, anxiolytic providing hemodynamically stable patients, with minimal side effects. We summarise that considering the above properties of dexmedetomidine can be incorporated into ERAS (early return after surgery) protocol, making it an optimal drug of choice as an alternative to moderate sedative drugs, in managing soft tissue injuries of maxillofacial region.






Similar content being viewed by others
References
Kretlow JD, McKnight AJ, Izaddoost SA (2010) Facial soft tissue trauma. Semin Plast Surg 24(4):348–356
Aveta A, Casati P (2008) Soft tissue injuries of the face: early aesthetic reconstruction in polytrauma patients. Ann Ital Chir 79(6):415–417
Etemadi Sh M, Kaviani N, Salimian K, Tajmiri G (2022) Effect of dexmedetomidine added to lidocaine cartridge on the level of patient sedation, cooperation, and patient and surgeon satisfaction during mandibular third-molar extraction surgery: a randomized double-blind controlled trial. Int J Dent 2:1–8. https://doi.org/10.1155/2022/4722674
Mishra N, Birmiwal KG, Pani N, Raut S, Sharma G, Rath KC (2016) Sedation in oral and maxillofacial day care surgery: a comparative study between intravenous dexmedetomidine and midazolam. Natl J Maxillofac Surg 7(2):178–185
Ustün Y, Gündüz M, Erdoğan O, Benlidayi ME (2006) Dexmedetomidine versus midazolam in outpatient third molar surgery yakup. J Oral Maxillofac Surg 64(9):1353–1358
Gertler R, Brown HC, Mitchell DH, Silvius EN (2001) Dexmedetomidine: a novel sedative-analgesic agent. Proc (Bayl Univ Med Cent) 14(1):13–21. https://doi.org/10.1080/08998280.2001.11927725. (PMID: 16369581; PMCID: PMC1291306)
Singaram M, Udhayakumar RK (2016) Prevalence, pattern, etiology, and management of maxillofacial trauma in a developing country: a retrospective study. J Korean Assoc Oral Maxillofac Surg 42(4):174–181
Procedural Sedation in the Emergency Department (2023) Policy statement by the American College of Emergency Physicians, pp 1–2
Bakshi SG, Paulin SV, Bhawalkar P (2020) A randomised controlled trial to evaluate the peri-operative role of intraoperative dexmedetomidine infusion in robotic-assisted laparoscopic oncosurgeries. Indian J Anaesth 64(9):784–789. https://doi.org/10.4103/ija.IJA_664_20. (Epub 2020 Sep 1. PMID: 33162573; PMCID: PMC7641074)
Wusiman P, Maimaitituerxun B, Saimaiti A, Moming A (2020) Epidemiology and pattern of oral and maxillofacial trauma. J Craniofac Surg 31(5):e517–e520
Shepherd JP, Shapland M, Pearce NX, Scully C et al (1990) Pattern, severity and aetiology of injuries in victims of assault. J R Soc Med 83(2):75–77
Khan TU, Rahat S, Khan ZA, Shahid L, Banouri SS et al (2022) Etiology and pattern of maxillofacial trauma. J PLoS ONE 17(9):1–10. https://doi.org/10.1371/journal.pone.0275515
Gursoytrak B, Kocaturk O, Koparal M, Gulsun B (2019) Assessment of effect of submucosal injection of dexmedetomidine on postoperative symptoms. J Oral Maxillofac Surg 78(3):366–371
Fasil F, Saundattikar G, Jawale RH (2022) Study of hemodynamic effects of preoperative single-bolus dexmedetomidine in elective laparoscopic surgeries. J Pharmacol Pharmacother 13(1):85–91
Fritsch G, Danninger T, Allerberger K, Tsodikov A, Felder TK, Kapeller M et al (2014) Dexmedetomidine added to ropivacaine extends the duration of interscalene brachial plexus blocks for elective shoulder surgery when compared with ropivacaine alone: a single-center, prospective, triple-blind, randomized controlled trial. Reg Anesth Pain Med 39(1):37–47
Raghu R, Indira P, Swetha A (2019) Effects of preoperative single bolus dose of dexmedetomidine on perioperative hemodynamics in elective laparoscopic cholecystectomy. Indian J Clin Anaesth 6(1):47–54
Kumar S, Kushwaha B, Prakash R et al (2014) Comparative study of effects of dexmedetomidine and clonidine premedication in perioperative hemodynamic stability and postoperative analgesia in laparoscopic cholecystectomy. Internet J Anesthesiol 33(1):600–606
Gadve VR, Shenoi R, Vats V, Shrivastava A (2018) Evaluation of anxiety, pain, and hemodynamic changes during surgical removal of lower third molar under local anesthesia. Ann Maxillofac Surg 8(2):247–253
Schäfers M, Geis C, Svensson CI, Luo ZD, Sommer C (2003) Selective increase of tumour necrosis factor-alpha in injured and spared myelinated primary afferents after chronic constrictive injury of rat sciatic nerve. Eur J Neurosci 17(4):791–804
Koch A, Zacharowski K, Boehm O et al (2007) Nitric oxide and pro-inflammatory cytokines correlate with pain intensity in chronic pain patients. Inflamm Res 56:32–37
Li S, Yang Y, Yu C, Yao Y, Wu Y, Qian L, Cheung CW (2015) Dexmedetomidine analgesia effects in patients undergoing dental implant surgery and its impact on postoperative inflammatory and oxidative stress. Oxid Med Cell Longev. https://doi.org/10.1155/2015/186736
Bhanot E, Tilvawala K, Shah V (2015) A comparative study of dexmedetomidine and midazolam for intravenous sedation in dental procedures. Indian J Appl Res 5(10):221–224
Venn RM, Hell J, Grounds RM (2000) Respiratory effects of dexmedetomidine in the surgical patient requiring intensive care. Crit Care 4(5):302–308
Garip L, Verbist J, Stragier H, Meyns J, Mesotten D, Vundelinckx J (2022) A comparative study of patient satisfaction about anesthesia with dexmedetomidine for ambulatory dental surgery. BMC Res Notes 15(1):376–383
Perrott JL, Co MT, Reynolds SC, Gunning DJ (2012) Dexmedetomidine as a procedural sedative for percutaneous tracheotomy: case report and systematic literature review. Case Rep Crit Care. https://doi.org/10.1155/2012/659415
Elsawy A (2021) Dexmedetomidine is an excellent additive to local anaesthesia for postoperative analgesia in bilateral third Molar teeth extraction surgery. Al-Azhar Int Med J. https://doi.org/10.21608/aimj.2021.66816.1430
Wang L, Zhou Y, Zhang T, Huang L, Peng W (2020) Comparison in sedative effects between dexmedetomidine and midazolam in dental implantation: a randomised clinical trial. Biomed Res Int. https://doi.org/10.1155/2020/7082597
Author information
Authors and Affiliations
Contributions
UH helped in conception and design of the work, literature search, interpretation of data, data analysis, manuscript editing. CS contributed to data collection, revising it critically for important intellectual content. AS was involved in final approval of the version to be published. AMK drafted the article. SSJ prepared the manuscript. AI analysed the data.
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hemavathi, U., Sreekanth, C., Shetty, A. et al. Evaluation of Analgesic Efficacy of Dexmedetomidine as an Adjuvant to Local Anaesthesia in Maxillofacial Soft Tissue Injuries: A Prospective Randomised Clinical Trial. J. Maxillofac. Oral Surg. (2024). https://doi.org/10.1007/s12663-024-02122-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12663-024-02122-7