Abstract
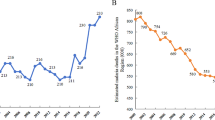
Although malaria burden and its active foci have sharply declined after the implementation of elimination programme since 2010, it is still considered as a major public health problem in southeast Iran. This descriptive-analytical study aimed to determine 10-years of malaria epidemiological trends in Bashagard County. Data were collected from 7 selected malarious region of the county based on active and passive surveillance of clinical cases. For diagnosis of malaria, the examination of microscopic slides and rapid diagnostic test, were used. In total, 237 malaria cases were found from 2009 to 2018. Plasmodium vivax was the dominant parasite species and identified in 232 (97.9%) individuals. Males were infected more than females and the majority of malaria cases (67.4%) were recorded from rural areas. Although about 98% of malaria cases were indigenous, they have decreased form 200 cases in 2009 to zero indigenous transmission in 2018. During the study period, malaria cases had decreased significantly by about 99% and the incidence rate had declined from 5.47/1000 cases in 2009 to 0.002/1000 in 2018. The incidence of malaria, especially indigenous cases, in Bashagard County has decreased dramatically in the past 10 years. However, there is still probability of malaria re-introduction and outbreak in the county due to climatical and geographical conditions. Therefore, it is necessary to implement an active surveillance system to detect and treat malaria cases quickly, during the elimination phase in this county.






Similar content being viewed by others
References
Ashley EA, Pyae Phyo A, Woodrow CJ (2018) Malaria. Lancet 391:1608–1621
Azari-Hamidian S, Norouzi B, Harbach RE (2019) A detailed review of the mosquitoes (Diptera: Culicidae) of Iran and their medical and veterinary importance. Acta Trop 194:106–122
Battle KE, Gething PW, Elyazar IR et al (2012) The global public health significance of Plasmodium vivax. Adv Parasitol 80:1–111
Cohen JM, Moonen B, Snow RW et al (2010) How absolute is zero? An evaluation of historical and current definitions of malaria elimination. Malar J 9:213
Cotter C, Sturrock HJ, Hsiang MS et al (2013) The changing epidemiology of malaria elimination: new strategies for new challenges. Lancet 382(9895):900–911
Edrissian GH (2006) Malaria in Iran: past and present situation. Iran J Parasitol 1(1):1–4
Forero DA, Chaparro PE, Vallejo AF et al (2014) Knowledge, attitudes and practices of malaria in Colombia. Malar J 13:165
Gething PW, Elyazar IR, Moyes CL et al (2012) A long neglected world malaria map: Plasmodium vivax endemicity in 2010. PLoS Negl Trop Dis 6(9):e1814
Ghahremani L, Azizi M, Moemenbellah-Fard MD et al (2019) Malaria preventive behaviors among housewives in suburbs of Bandar-Abbas City, south of Iran: interventional design based on PRECEDE model. Pathog Glob Health 113(1):32–38
Hanafi-Bojd AA, Vatandoost H, Philip E et al (2010) Malaria situation analysis and stratification in Bandar Abbas County, southern Iran, 2004–2008. Iran J Arthropod Borne Dis 4(1):31–41
Hanafi-Bojd AA, Azari-Hamidian S, Hassan V et al (2011) Spatio-temporal distribution of malaria vectors (Diptera: Culicidae) across different climatic zones of Iran. Asian Pac J Trop Med 4(6):498–504
Hanafi-Bojd AA, Vatandoost H, Oshaghi M et al (2012) Entomological and epidemiological attributes for malaria transmission and implementation of vector control in southern Iran. Acta Trop 121(2):85–92
Hemami MR, Sari AA, Raeisi A et al (2013) Malaria elimination in Iran, importance and challenges. Int J Prev Med 4(1):88–94
Hormozgan Meteorological administration. Available at http://hormozganmet.ir/. Accessed 10 March 2021.
Howes RE, Battle KE, Mendis KN et al (2016) Global epidemiology of Plasmodium vivax. Am J Trop Med Hyg 95(6 Suppl):15–34
Joshi A, Banjara M (2008) Malaria related knowledge, practices and behaviour of people in Nepal. J Vector Borne Dis 45(1):44–50
Kafil H (2017) Malaria in Iran: is the elimination phase? Ann Trop Med Public Health 10(4):1062
Keiser J, Utzinger J, De Castro MC et al (2004) Urbanization in sub-saharan Africa and implication for malaria control. Am J Trop Med Hyg 71(2 Suppl):118–127
Madani A, Soleimani-Ahmadi M, Davoodi SH et al (2017) Household knowledge and practices concerning malaria and indoor residual spraying in an endemic area earmarked for malaria elimination in Iran. Parasit Vectors 10(1):600
Musoke D, Miiro G, Ndejjo R et al (2018) Malaria prevention practices and associated environmental risk factors in a rural community in Wakiso district, Uganda. PLoS ONE 13(10):e0205210
Nateghpour M, Jamshidi Makiani M, Mohseni G et al (2010) First case of imported Plasmodium ovale from Iran. Iran J Med Sci 35(3):264–266
Nejati J, Tabatabaei SM, Salehi M et al (2017) Some probable factors affecting the malaria situation before and at the beginning of a pre-elimination program in southeastern Iran. J Parasit Dis 41(2):503–509
Norouzinejad F, Ghaffari F, Raeisi A (2016) Epidemiological status of malaria in Iran, 2011–2014. Asian Pac J Trop Med 9(11):1055–1061
Rakhshani F, Ansari Moghadam A, Alemi R et al (2003) Knowledge, perceptions and prevention of malaria among women in Sistan va Baluchestan, Islamic Republic of Iran. East Mediterr Health J 9(3):248–256
Robert V, Macintyre K, Keating J et al (2003) Malaria transmission in urban sub-Saharan Africa. Am J Trop Med Hyg 68(2):169–176
Sanei-Dehkordi A, Soleimani-Ahmadi M, Jaberhashemi SA et al (2019) Species composition, seasonal abundance and distribution of potential anopheline vectors in a malaria endemic area of Iran: field assessment for malaria elimination. Malar J 18(1):157
Schapira A, Zaim M, Raeisi A et al (2018) History of the successful struggle against malaria in the Islamic Republic of Iran. Shayan Gostar Publ Tehran, Tehran, pp 27–28
Shivalli S, Pai S, Akshaya KM et al (2016) Construction site workers’ malaria knowledge and treatment-seeking pattern in a highly endemic urban area of India. Malar J 15:168
Singh MP, Saha KB, Chand SK et al (2017) Factors associated with treatment seeking for malaria in Madhya Pradesh, India. Trop Med Int Health 22(11):1377–1384
Smith DL, Hay SI, Noor AM et al (2009) Predicting changing malaria risk after expanded insecticide-treated net coverage in Africa. Trends Parasitol 25(11):511–516
Soleimani-Ahmadi M, Vatandoost H, Shaeghi M et al (2012) Field evaluation of permethrin long-lasting insecticide treated nets (Olyset®) for malaria control in an endemic area, southeast of Iran. Acta Trop 123(3):146–153
UCSF (2015) Global Health Group. Eliminating malaria in Iran. https://globalhealthsciences.ucsf.edu/sites/globalhealthsciences.ucsf.edu/files/pub/iran2015-final.pdf. Accessed 10 Oct 2020
UNDP (2017) Intensified malaria control in high burden provinces towards falciparum elimination. http://www.ir.undp.org/content/iran/en/home/operations/projects/health_and_development/Malaria.html. Accessed 20 Oct 2020
Van Dorp L, Gelabert P, Rieux A et al (2020) Plasmodium vivax malaria viewed through the lens of an eradicated European strain. Mol Biol Evol 37(3):773–785
Vatandoost H, Raeisi A, Saghafipour A et al (2019) Malaria situation in Iran: 2002–2017. Malar J 18(1):200
WHO (2010) Basic malaria microscopy, Part II: Tutor's guide
WHO (2013). Malaria in the Eastern Mediterranean Region 2013
WHO (2016) WHO malaria terminology 2016. https://apps.who.int/iris/bitstream/handle/10665/208815/WHO_HTM_GMP_2016.6_eng.pdf. Accessed 10 March 2021
WHO (2020) World Malaria Report 2020. https://www.mmv.org/sites/default/files/uploads/docs/publications/World_Malaria_Report_2020.pdf. Accessed 25 Feb 2021
Wickremasinghe R, Fernando SD, Thillekaratne J et al (2014) Importance of active case detection in a malaria elimination programme. Malar J 13:186
Acknowledgements
The authors of this article are grateful for the support of the director and the staff of Bashagard Health Center who cooperated and participated in this study.
Funding
This research has been funded by the Research Deputy of Hormozgan University of Medical Sciences (Project No. 24/145).
Author information
Authors and Affiliations
Contributions
MZ drafted the manuscript. HF designed the study. SAJ coordinated in the field research activities and data collection. MSA and ASD designed the study, coordinated in field activity, collected data, trained field researcher and drafted the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethics approval and consent to participate
This study has been registered and approved by Hormozgan University of Medical Sciences Ethical Committee (Code No: IR.HUMS.REC.1397.398). Study registration date: Jan 20, 2020.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zare, M., Farshidi, H., Soleimani-Ahmadi, M. et al. Significant decline of malaria incidence in a low socioeconomic area in the southeast of Iran: 10 years field assessment during malaria elimination programme. J Parasit Dis 45, 986–994 (2021). https://doi.org/10.1007/s12639-021-01391-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12639-021-01391-0