Abstract
Objectives
Nutritional status is one of the factors that affects disease progression, morbidity and mortality in elderly patients with dementia. The present study aimed to evaluate the effect of acetylcholinesterase inhibitor (AchEI) therapy on nutritional status and food intake in the elderly.
Design, setting and participants
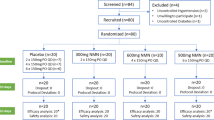
Newly diagnosed patients with dementia, who underwent comprehensive geriatric assessment (CGA) and were followed at regular intervals, were retrospectively evaluated. A total of 116 patients, who began to receive AchEI therapy and completed 6-month follow-up period under this treatment, were enrolled in the study.
Measurements
Socio-demographic characteristics and data on comorbidity, polypharmacy, cognitive function, depression, activities of daily living and nutritional status (weight, Body Mass Index (BMI), Mini Nutritional Assessment (MNA)-Short Form) were recorded.
Results
The mean age of the patients was 78.0±8.9 years. There was no significant difference between baseline and 6-month BMI, weight and MNA scores of dementia patients who received AchEI therapy (p>0.05). With regard to the relation between changes in BMI, weight and MNA on the 6th month versus baseline, and donepezil, rivastigmine and galantamine therapies, no difference was determined (p>0.05). However, no worsening in food intake was observed (kappa: 0.377). When the effects of each AchEI on food intake were compared, food intake in rivastigmine treated patients was not decreased as much as it was in galantamine or donepezil treated patients (p<0.05).
Conclusion
AchEI therapy has no unfavorable effect on nutritional status or weight in elderly patients with different types of dementia, but it seems that food intake is better in those treated by rivastigmine patch.




Similar content being viewed by others
References
Orsitto G. Different components of nutritional status in older inpatients with cognitive impairment. J Nutr Health Aging. 2012;16(5):468–71.
Volicer L, Seltzer B, Rheaume Y, Karner J, Glennon M, Riley ME, Crino P. Eating difficulties in patients with probable dementia of the Alzheimer type. J Geriatr Psychiatry Neurol. 1998;2(4):188–95
Sergi G, De Rui M, Coin A, Inelmen EM, Manzato E. Weight loss and Alzheimer’s disease: temporal and aetiologic connections. Proc Nutr Soc. 2013;72(1):160–5.
Uwano C, Suzuki M, Aikawa T et al. Rivastigmine dermal patch solves eating problems in an individual with advanced Alzheimer’s disease. J Am Geriatr Soc. 2012;60(10):1979–80.
Schofield PW, Finnie S, Yong YM. The role of olfactory challenge tests in incipient dementia and clinical trial design. Curr Neurol Neurosci Rep. 2014;14(9):479
Claggett MS. Nutritional factors relevant to Alzheimer’s disease. J Am Diet Assoc 1989;89:392e6
Khater MS, Abouelezz NF. Nutritional status in older adults with mild cognitive impairment living in elderly homes in Cairo, Egypt. J Nutr Health Aging. 2011;15(2):104–8
Roqué M, Salvà A, Vellas B. Malnutrition in community-dwelling adults with dementia (NutriAlz Trial). J Nutr Health Aging. 2013;17(4):295–9.
Vellas B, Lauque S, Gillette-Guyonnet S et al. Impact of nutritional status on the evolution of Alzheimer’s disease and on response to acetylcholinesterase inhibitor treatment. J Nutr Health Aging. 2005;9(2):75–80.
Guerin O, Soto ME, Brocker P, Robert PH, Benoit M, Vellas B; REAL. FR Group. Nutritional status assessment during Alzheimer’s disease: results after one year (the REAL French Study Group). J Nutr Health Aging. 2005;9(2):81–4.
Lam B, Hollingdrake E, Kennedy JL, Black SE, Masellis M. Cholinesterase inhibitors in Alzheimer’s disease and Lewy body spectrum disorders: the emerging pharmacogenetic story. Hum Genomics. 2009;4(2):91–106.
Baskys A, Cheng JX. Pharmacological prevention and treatment of vascular dementia: approaches and perspectives. Exp Gerontol. 2012;47(11):887–91
Boeve BF, Josephs KA, Drubach DA. Current and future management of the corticobasal syndrome and corticobasal degeneration. Handb Clin Neurol. 2008;89:533–48.
Droogsma E, van Asselt DZ, van Steijn JH, Schuur T, Huinink EJ. Effect of longterm treatment with galantamine on weight of patients with Alzheimer’s dementia. J Nutr Health Aging. 2013;17(5):461–5.
American Psychiatric Association, Diagnostic and Statistical Manual of Mental Disorders 4th ed., text rev.; DSM-IV-TR, 2000
Soysal P, Isik AT, Buyukaydin B, Kazancioglu RA. Comparison of end-stage renal disease and Alzheimer’s disease in the elderly through a comprehensive geriatric assessment. Int Urol Nephrol. 2014;46(8):1627–32.
Dina Zekrya, Bernardo Hermont Loures Valleb, Claudia Lardia et al. Geriatrics index of comorbidity was the most accurate predictor of death in geriatric hospital among six comorbidity scores. Journal of Clinical Epidemiology. 2010;63:1036–1044.
Babacan-Yildiz G, Isik AT, Ur E et al. COST: Cognitive State Test, a brief screening battery for Alzheimer disease in illiterate and literate patients. Int Psychogeriatr. 2013;25:403–12.
Folstein MF, Folstein SE, McHugh PR. Mini-Mental State. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 1975;12:189–198
Alexopoulos GS, Abrams RC, Young RC, et al. «Cornell Scale for Depression in Dementia». Biological Psychiatry. 1988;23(3): 271–284.
Mahoney F. Barthel D. «Functional evaluation: the Barthel Index». Md Med J. 1965;14:61–65
Lawton, M.P., Brody, E.M. Assessment of older people: Self-maintaining and instrumental activities of daily living. The Gerontologist. 1969;9(3):179–186.
Zarit S.H., Reever K.E., Bach-Peterson J. Relatives of the impaired elderly: correlated of feelings of burden. Gerontologist. 1980;20, 649–655.
Vellas B, Guigoz Y, Garry PJ et al. The Mini Nutritional Assessment (MNA) and its use in grading the nutritional state of elderly patients. Nutrition. 1999;15(2):116–22.
Soysal P, Isik AT, Ugur A, Kazancioglu R, Ergun F, Babacan Yildiz G. Vitamin B12 and folic acid levels are not related to length of stay in elderly inpatients. Nutrition. 2013;29(5):757–9.
Saka B, Kaya O, Ozturk GB, Erten N, Karan MA. Malnutrition in the elderly and its relationship with other geriatric syndromes. Clin Nutr. 2010;29(6):745–8.
Herrmann N, Lanctôt KL, Hogan DB. Pharmacological recommendations for the symptomatic treatment of dementia: the Canadian Consensus Conference on the Diagnosis and Treatment of Dementia Alzheimers Res Ther. 2013;8:5.
Stewart JT, Gorelik AR. Involuntary weight loss associated with cholinesterase inhibitors in dementia. J Am Geriatr Soc. 2006;54(6):1013–4.
Raskind MA, Peskind ER, Wessel T, Yuan W. Galantamine in AD: A 6-month randomized, placebo-controlled trial with a 6-month extension. The Galantamine USA-1 Study Group. Neurology. 2000;27;54(12):2261–8.
Gillette-Guyonnet S, Cortes F, Cantet C, Vellas B; REAL.FR Group. Long-term cholinergic treatment is not associated with greater risk of weight loss during Alzheimer’s disease: data from the French REAL.FR cohort. J Nutr Health Aging. 2005;9(2):69–73.
Kaiser MJ, Bauer JM, Ramsch C et al. MNA-International Group Validation of the Mini Nutritional Assessment short-form (MNA-SF): a practical tool for identification of nutritional status. J Nutr Health Aging. 2009;13(9):782–8
Cortes F, Portet F, Touchon J, Vellas B. Six and 18-month changes in mild to moderate Alzheimer’s patients treated with acetylcholinesterase inhibitors: what can we learn for clinical outcomes of therapeutic trials? J Nutr Health Aging. 2007;11(4):330–7
Cortes F, Gillette-Guyonnet S, Nourhashemi F. Recent data on the natural history of Alzheimer’s disease: results from the REAL.FR Study. J Nutr Health Aging. 2005;9(2):86–93.
de Toledo-Morrell L, Dickerson B, Sullivan MP et al. Hemispheric differences in hippocampal volume predict verbal and spatial memory performance in patients with Alzheimer’s disease. Hippocampus 2000;10, 136–142. 33
Ober BA, Jagust WJ, Koss E et al. Visuoconstructive performance and regional cerebral glucose metabolism in Alzheimer’s disease. J Clin Exp Neuropsychol 1991;13, 752–772
Lyketsos CG, Lopez O, Jones B et al. Prevalence of neuropsychiatric symptoms in dementia and mild cognitive impairment: results from the cardiovascular health study. JAMA 2002;288, 1475–1483.
Dando R, Roper SD. Acetylcholine is released from taste cells, enhancing taste signalling. J Physiol. 2012;1;590(Pt 13):3009–17.
Jia YX, Li JQ, Matsui T et al. Neurochemical regulation of swallowing reflex in guinea pigs. Geriatr Gerontol Int. 2001;1:56–61.
Lee JH, Sevigny J. Effects of body weight on tolerability of rivastigmine transdermal patch: a post-hoc analysis of a double-blind trial in patients with Alzheimer disease. Alzheimer Dis Assoc Disord. 2011;25(1):58–62.
Nakamura Y, Imai Y, Shigeta M et al. A 24-week, randomized, double-blind, placebo-controlled study to evaluate the efficacy, safety and tolerability of the rivastigmine patch in Japanese patients with Alzheimer’s disease. Dement Geriatr Cogn Dis Extra. 2011;1(1):163–79..
Wilson MM, Thomas DR, Rubenstein LZ et al. Appetite assessment: simple appetite questionnaire predicts weight loss in community-dwelling adults and nursing home residents. Am J Clin Nutr. 2005;82(5):1074–81
Tully MW, Lambros Matrakas K, Musallam K. The eating behavior scale: a simple method of assessing functional ability in patients with Alzheimer’s disease. J Nutr Health Aging. 1998;2(2):119–21
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Soysal, P., Isik, A.T. Effects of acetylcholinesterase inhibitors on nutritional status in elderly patients with dementia: A 6-month follow-up study. J Nutr Health Aging 20, 398–403 (2016). https://doi.org/10.1007/s12603-015-0603-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-015-0603-z