Abstract
Background
Individuals construct beliefs about an illness based on their own perceptions, interpretation, and understanding of the illness and its treatment. These beliefs (collectively referred to as “illness cognitions” or “representations”) can have implications for psychological outcomes in family members and carers of an individual with an illness. The aim of this study was to explore young people’s perceptions of their parent’s cancer using the Common-Sense Model of Self-Regulation as a theoretical framework.
Methods
Semi-structured, one-on-one interviews were conducted with young people who had a parent diagnosed with cancer. Interview transcripts were analysed using deductive thematic analysis techniques.
Results
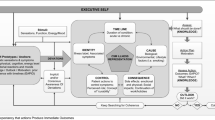
Eleven young people aged 15–24 years participated in the study. Major themes aligned with the dimensions of the Common-Sense Model of Self-Regulation. Young people described their experiences with parental cancer with reference to cognitive representations (beliefs about the illness identity, their understanding or coherence of the illness, and consequences, curability or controllability, timeline, and cause of the illness) and emotional representations (emotional beliefs and subjective feelings about the illness).
Conclusions
Findings indicate that young people’s perceptions of their parent’s cancer can be usefully described within the framework of the Common-Sense Model of Self-Regulation. Future research should investigate the relationships between young people’s illness cognitions, coping strategies, and psychological adjustment following their parent’s cancer diagnosis. This will provide valuable insights for the development of interventions that target specific types of illness cognitions associated with maladaptive coping strategies and poor adjustment.

Similar content being viewed by others
Notes
CanTeen is an Australian support organization for young people affected by cancer, including young people diagnosed with cancer, and young people who have a brother, sister, or parent diagnosed with cancer.
References
Gazendam-Donofrio SM, Hoekstra HJ, van der Graaf WT, et al. Adolescents' emotional reactions to parental cancer: effect on emotional and behavioral problems. J Pediatr Psychol. 2011;36(3):346–59. https://doi.org/10.1093/jpepsy/jsq090.
Pederson S, Revenson TA. Parental illness, family functioning, and adolescent well-being: a family ecology framework to guide research. J Fam Psychol. 2005;19(3):404–19. https://doi.org/10.1037/0893-3200.19.3.404.
Visser A, Huizinga GA, van der Graaf WT, Hoekstra HJ, Hoekstra-Weebers JE. The impact of parental cancer on children and the family: a review of the literature. Cancer Treat Rev. 2004;30(8):683–94. https://doi.org/10.1016/j.ctrv.2004.06.001.
Huizinga GA, Visser A, Zelders-Steyn YE, Teule JA, Reijneveld SA, Roodbol PF. Psychological impact of having a parent with cancer. Eur J Cancer. 2011;47(Suppl 3):239–46. https://doi.org/10.1016/S0959-8049(11)70170-8.
Compas BE, Worsham NL, Ey S, Howell DC. When mom or dad has cancer: II. Coping, cognitive appraisals, and psychological distress in children of cancer patients. Health Psychol. 1996;15(3):167–75. https://doi.org/10.1037/0278-6133.15.3.167.
Patterson P, McDonald FEJ, Orchard P. A new Australian online and phone mental health support service for young people living with cancer. Aust Psychiatry. 2014;22(2):165–9. https://doi.org/10.1177/1039856213519144.
Patterson P, McDonald FEJ, White KJ, Butow PN, Walczak A. Levels of unmet needs and distress in AYAs impacted by familial cancer. Psycho-Oncology. 2016;26(9):1285–92. https://doi.org/10.1002/pon.4421.
Krattenmacher T, Kuhne F, Ernst J, Bergelt C, Romer G, Moller B. Parental cancer: factors associated with children's psychosocial adjustment - a systematic review. J Psychosom Res. 2012;72(5):344–56. https://doi.org/10.1016/j.jpsychores.2012.01.011.
Su YH, Ryan-Wenger NA. Children's adjustment to parental cancer: a theoretical model development. Cancer Nurs. 2007;30(5):362–81; quiz 82-3. https://doi.org/10.1097/01.NCC.0000290817.37442.e6.
Ellis SJ, Wakefield CE, Antill G, Burns M, Patterson P. Supporting children facing a parent's cancer diagnosis: a systematic review of children's psychosocial needs and existing interventions. Eur J Cancer Care (Engl). 2016;26(1). https://doi.org/10.1111/ecc.12432.
McDonald FEJ, Patterson P, White KJ, Butow PN, Costa DSJ, Kerridge I. Correlates of unmet needs and psychological distress in adolescent and young adults who have a parent diagnosed with cancer. Psycho-Oncology. 2016;25(4):447–54. https://doi.org/10.1002/pon.3942.
Hagger MS, Koch S, Chatzisarantis NLD, Orbell S. The common sense model of self-regulation: meta-analysis and test of a process model. Psychol Bull. 2017;143(11):1117–54. https://doi.org/10.1037/bul0000118.
Joice S. Self-management following stroke. Nurs Stand. 2012;26(22):39–46. https://doi.org/10.7748/ns2012.02.26.22.39.c8919.
Gray SE, Rutter DR. Illness representations in young people with chronic fatigue syndrome. Psychol Health. 2007;22(2):1–16. https://doi.org/10.1080/14768320600774595.
Hagger MS, Orbell S. A meta-analytic review of the common-sense model of illness representations. Psychol Health. 2003;18(2):141–84. https://doi.org/10.1080/088704403100081321.
Hoving JL, van der Meer M, Volkova AY, Frings-Dresen MHW. Illness preceptions and work participation: a systematic review. Int Arch Occup Environ Health. 2010;83(6):595–605. https://doi.org/10.1007/s00420-010-0506-6.
Petrie KJ, Weinman J. Why illness perceptions matter. Clin Med. 2006;6(6):536–9. https://doi.org/10.7861/clinmedicine.6-6-536.
Diefenbach MA, Leventhal H. The common-sense model of illness representation: theoretical and practical considerations. J Soc Distress Homeless. 1996;5(1):11–37. https://doi.org/10.1007/BF02090456.
Browning KK, Wewers ME, Ferketich AK, Otterson GA, Reynolds NR. The self-regulation model of illness applied to smoking behavior in lung cancer. Cancer Nurs. 2010;32(4):E15–25. https://doi.org/10.1097/NCC.0b013e3181a0238f.
Leventhal H, Phillips LA, Burns E. The common-sense model of self-regulation (CSM): a dynamic framework for understanding illness self-management. J Behav Med. 2016;39(6):935–46. https://doi.org/10.1007/s10865-016-9782-2.
Leventhal H, Phillips LA, Burns E. Modelling management of chronic illness in everyday life: a common-sense approach. Psychol Top. 2016;25(1):1–18.
Moss-Morris R, Weinman J, Petrie KJ, Horne R, Cameron LD, Buick D. The revised Illness Perception Questionnaire (IPQ-R). Psychol Health. 2002;17(1):1–16. https://doi.org/10.1080/08870440290001494.
Moss-Morris R, Petrie KJ, Weinman J. Functioning in chronic fatigue syndrome: do illness perceptions play a regulatory role? Br J Health Psychol. 1996;1(1):15–25. https://doi.org/10.1111/j.2044-8287.1996.tb00488.x.
Kemp S, Morley S, Anderson E. Coping with epilepsy: do illness representations play a role? Br J Clin Psychol. 1999;38(1):43–58. https://doi.org/10.1348/014466599162656.
Corbett T, Groarke A, Walsh JC, McGuire BE. Cancer-related fatigue in post-treatment cancer survivors: application of the common sense model of illness representations. BMC Cancer. 2016;16(1):919. https://doi.org/10.1186/s12885-016-2907-8.
Del Castillo A, Godoy-Izquierdo D, Vazquez ML, Godoy JF. Illness beliefs about cancer among healthy adults who have and have not lived with cancer patients. Int J Behav Med. 2011;18:342–51. https://doi.org/10.1007/s12529-010-9141-6.
Dempster M, McCorry NK, Brennan E, Donnelly M, Murray LJ, Johnston BT. Illness perceptions among carer-survivor dyads are related to psychological distress among oesophageal cancer survivors. J Psychosom Res. 2011;70:432–9. https://doi.org/10.1016/j.jpsychores.2010.07.007.
Fortune DG, Smith JV, Garvey K. Perceptions of psychosis, coping, appraisals, and psychological distress in the relatives of patients with schizophrenia: an exploration using self-regulation theory. Br J Clin Psychol. 2011;44(3):319–31. https://doi.org/10.1348/014466505X29198.
Bogosian A, Moss-Morris R, Bishop FL, Hadwin J. Development and initial validation of the perceptions of parental illness questionnaire. J Health Psychol. 2014;19(7):931–42. https://doi.org/10.1177/1359105313482164.
Yu H, Lingler JH, Sereika SM, Erlen JA. Characteristics and correlates of caregivers' perceptions of their family members' memory loss. Nurs Res. 2017;66(3):240–5. https://doi.org/10.1097/NNR.0000000000000220.
Scerri J, Saliba T, Saliba G, Scerri CA, Camilleri L. Illness perceptions, depression and anxiety in informal carers of persons with depression: a cross-sectional survey. Qual Life Res. 2019;28(2):451–60. https://doi.org/10.1007/s11136-018-2009-y.
Graham L, Dempster M, McCorry NK, Donnelly M, Johnston BT. Change in psychological distress in longer-term oesophageal cancer carers: are clusters of illness perception change a useful determinant? Psycho-Oncology. 2016;25(6):663–9. https://doi.org/10.1002/pon.3993.
Gatzoyia D, Kotsis K, Koullourou I, Goulia P, Carvalho AF, Soulis S, et al. The association of illness perceptions with depressive symptoms and general psychological distress in parents of an offspring with autism spectrum disorder. Disabil Health J. 2014;7(2):173–80. https://doi.org/10.1016/j.dhjo.2013.10.008.
United Nations Educational Scientific and Cultural Organisation. What do we mean by “youth”? 2017. http://www.unesco.org/new/en/social-and-human-sciences/themes/youth/youth-definition/. Accessed 21 Oct 2018.
Sawyer SM, Azzopardi PS, Wickremarathne D, Patton GC. The age of adolescence. Lancet Child Adolesc Health. 2018;2(3):223–8. https://doi.org/10.1016/S2352-4642(18)30022-1.
Australian Institute of Health and Welfare. Young Australians: their health and wellbeing 2011. Canberra: Australian Institute of Health and Welfare; 2011. Report No.: Cat. no. PHE 140
Heffernan E, Coulson NS, Henshaw H, Barry JG, Ferguson MA. Understanding the psychosocial experiences of adults with mild-moderate hearing loss: an application of Leventhal’s self-regulatory model. Int J Audiol. 2016;55(Suppl 3):S3–S12. https://doi.org/10.3109/14992027.2015.1117663.
Braun V, Clarke V. Successful qualitative research: a practical guide for beginners. Thousand Oaks: SAGE Publications; 2013.
Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3(2):77–101. https://doi.org/10.1191/1478088706qp063oa.
Maynard A, Patterson P, McDonald FEJ, Stevens G. What is helpful to adolescents who have a parent diagnosed with cancer? J Psychosoc Oncol. 2013;31(6):675–97. https://doi.org/10.1080/07347332.2013.835021.
Cassidy T, McLaughlin M, Giles M. Benefit finding in response to general life stress: measurement and correlates. Health Psychol Behav Med. 2014;2(1):268–82. https://doi.org/10.1080/21642850.2014.889570.
Cassidy T. Benefit finding through caring: the cancer caregiver experience. Psychol Health. 2012;28(3):250–66. https://doi.org/10.1080/08870446.2012.717623.
Cassidy T, Giles M, McLaughlin M. Benefit finding and resilience in child caregivers. Br J Health Psychol. 2014;19(3):606–18. https://doi.org/10.1111/bjhp.12059.
Semino E, Demjen Z, Demmen J, et al. The online use of violence and journey metaphors by patients with cancer, as compared with health professionals: a mixed methods study. BMJ Support Palliat Care. 2015;7(1):60–6. https://doi.org/10.1136/bmjspcare-2014-000785.
Miller RS. Speak up: 8 words and phrases to ban in oncology! Oncol Times. 2010;32(12):20. https://doi.org/10.1097/01.COT.0000383777.50536.b2.
Granger K. Having cancer is not a fight or a battle. Kings Place: The Guardian; 2014.
James D. It’s time to stop seeing cancer as an enemy we can wage war against - you can't fight a battle that's not fair. London: The Sun; 2018.
Cooper C. Mind your language: 'Battling' cancer metaphors can make terminally ill patients worse. London: The Independent; 2014.
Semino E. Whether you 'battle' cancer or experience a ‘journey’ is an individual choice. The Conversation. 2015. https://theconversation.com/whether-you-battle-cancer-or-experience-a-journey-is-an-individual-choice-39142. Accessed 8 Oct 2018.
Tomasetti C, Li L, Vogelstein B. Stem cell divisions, somatic mutations, cancer etiology, and cancer prevention. Science. 2017;355(6331):1330–4. https://doi.org/10.1126/science.aaf9011.
Phillips F, Lewis FM. The adolescent’s experience when a parent has advanced cancer: a qualitative inquiry. Palliat Med. 2015;29(9):851–8. https://doi.org/10.1177/0269216315578989.
Karnilowicz W. Identity and psychological ownership in chronic illness and disease state. Eur J Cancer Care (Engl). 2011;20(2):276–82. https://doi.org/10.1111/j.1365-2354.2010.01220.x.
Acknowledgements
The authors would like to thank Paige Fletcher, who is a research assistant at Flinders University, for her assistance with coding interview transcripts. The authors especially thank the young people who participated in this research for their willingness to share their experiences.
Funding
This study was funded by the Flinders Foundation, with the support of its donors and partners.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fletcher, C., Wilson, C., Flight, I. et al. Illness Cognitions Among Adolescents and Young Adults Who Have a Parent with Cancer: a Qualitative Exploration Using the Common-Sense Model of Self-regulation as a Framework. Int.J. Behav. Med. 26, 531–541 (2019). https://doi.org/10.1007/s12529-019-09793-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12529-019-09793-4