Abstract
Background
Cervical spondylotic myelopathy (CSM) is a common degenerative disease that arises from spinal cord compression and injury. Laminectomy with posterior spinal fusion (LPSF) is one of the most common approaches used to treat patients with CSM. The present study aimed to evaluate predictors of poor clinical outcome in patients with CSM undergoing LPSF.
Methods
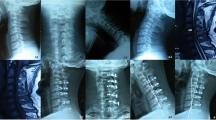
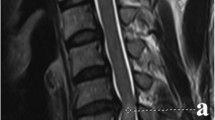
We retrospectively evaluated 157 patients with CSM who underwent LPSF at our center between April 2014 and June 2019. The neurological outcome was assessed using the modified Japanese Orthopaedic Association (mJOA) scale before the surgery and at the last follow-up visit. Based on the clinical outcomes, all patients were divided into two groups [the good group (recovery rates ≥ 75%) and the poor group (recovery rates < 75%)]. The following suggested variables as potential predictors for the poor clinical outcome were compared between the two groups:age, gender, body mass index (BMI), smoking, diabetes, number of laminectomy levels, presence of signal changes in Magnetic Resonance Imaging (MRI), duration of symptoms, preoperative JOA scale, preoperative Pavlov ratio, preoperative cervical curvature, and preoperative cervical range of motion (ROM).
Results
There were 86 males (54.8%) and 71 females (45.2%) with the mean follow-up time of 24.96 ± 1.67 months. Overall, 114 patients (72.6%) had a good clinical outcome. However, 43 subjects (27.4%) failed to achieve a good outcome. According to the binary logistic regression analysis, age (odds ratio [OR], 2.14; 95% confidence interval [95% CI], 1.87–2.63; P = 0.014) and preoperative JOA scale (OR, 3.73; 95% CI 2.96–4.87; p < 0.001) were independent predictors of poor clinical outcome.
Conclusions
The results of the present study showed that age and preoperative JOA scale were predictors of poor clinical outcome in patients with CSM undergoing LPSF. These findings will be of great value in preoperative counseling and management of postoperative expectations.
Similar content being viewed by others
Availability of data and materials
The datasets generated and/or analyzed during the current study are not publicly available due them containing information that could compromise research participant privacy/consent but are available from the corresponding author on reasonable request. All data are available from the corresponding author upon reasonable request. The patient's data included in this manuscript has not been previously reported.
Abbreviations
- CSM:
-
Cervical spondylotic myelopathy
- LPSF:
-
Laminectomy with posterior spinal fusion
- JOA:
-
Japanese Orthopaedic Association
- BMI:
-
Body mass index
- MRI:
-
Magnetic Resonance Imaging
- ROM:
-
Cervical range of motion
- HRQOL:
-
Health-related quality of life
References
Shin JW, Jin SW, Kim SH et al (2015) Predictors of outcome in patients with cervical spondylotic myelopathy undergoing unilateral open-door laminoplasty. Korean J Spine 12:261–266
Lau D, Winkler EA, Than KD, Chou D, Mummaneni PV (2017) Laminoplasty versus laminectomy with posterior spinal fusion for multilevel cervical spondylotic myelopathy: Influence of cervical alignment on outcomes. J Neurosurg Spine 27:508–517
Kwon SY, Shin JJ, Lee JH, Cho WH (2015) Prognostic factors for surgical outcome in spinal cord injury associated with ossification of the posterior longitudinal ligament (OPLL). J Orthop Surg Res 10:94–103
Adogwa O, Huang K, Hazzard M et al (2015) Outcomes after cervical laminectomy with instrumented fusion versus expansile laminoplasty: A propensity matched study of 3185 patients. J Clin Neurosci 22:549–553
Heller JG, Edwards CC, Murakami H, Rodts GE. 2001. Laminoplasty versus laminectomy and fusion for multilevel cervical myelopathy: An independent matched cohort analysis. Spine (Phila Pa 1976) 26: 1330–1336.
Manzano GR, Casella G, Wang MY, Vanni S, Levi AD (2012) A prospective, randomized trial comparing expansile cervical laminoplasty and cervical laminectomy and fusion for multilevel cervical myelopathy. Neurosurgery 70:264–277
Yoon ST, Hashimoto RE, Raich A et al (2013) Outcomes after laminoplasty compared with laminectomy and fusion in patients with cervical myelopathy: a systematic review. Spine (Phila Pa 1976) 38:183.
Highsmith JM, Dhall SS, Haid RW, Rodts GE, Mummaneni PV (2011) Treatment of cervical stenotic myelopathy: a cost and outcome comparison of laminoplasty versus laminectomy and lateral mass fusion. J Neurosurg Spine 14:619–625
Wilson JF, Jiang F, Fehlings M (2019) Clinical predictors of complications and outcomes in degenerative cervical myeloradiculopathy. Indian Spine Journal 2:59
Buell TJ, Buchholz AL, Quinn JC, Shaffrey CI, Smith JS (2018) Importance of sagittal alignment of the cervical spine in the management of degenerative cervical myelopathy. Neurosurg Clin N Am 29:69–82
Epstein NE (2018) High cord signals on magnetic resonance and other factors predict poor outcomes of cervical spine surgery: a review. Surg Neurol Int 9:13
Hirabayashi K, Satomi K (1988) Operative procedure and results of expansive open-door laminoplasty. Spine (Phila Pa 1976) 13:870–876.
Ogino H, Tada K, Okada K et al (1983) Canal diameter, anteroposterior compression ratio, and spondylotic myelopathy of the cervical spine. Spine (Phila Pa 1976) 8:1–15.
Yeh KT, Chen IH, Yu TC et al (2015) Modified expansive open-door laminoplasty technique improved postoperative neck pain and cervical range of motion. J Formos Med Assoc 114:1225–1232
Chen GD, Lu Q, Sun JJ et al (2016) Effect and prognostic factors of laminoplasty for cervical myelopathy with an occupying ratio greater than 50%. Spine (Phila Pa 1976) 41:378–383.
Fujimori T, Iwasaki M, Okuda S et al (2014) Long-term results of cervical myelopathy due to ossification of the posterior longitudinal ligament with an occupying ratio of 60% or more. Spine (Phila Pa 1976) 39:58–67.
Nakashima H, Yukawa Y, Ito K et al (2012) Prediction of lower limb functional recovery after laminoplasty for cervical myelopathy: Focusing on the 10-s step test. European spine journal: official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society 21:1389–1395
Gao R, Yang L, Chen H, et al (2012) Long term results of anterior corpectomy and fusion for cervical spondylotic myelopathy. PLoS One 7:e34811.
Pumberger M, Froemel D, Aichmair A, et al (2013) Clinical predictors of surgical outcome in cervical spondylotic myelopathy: an analysis of 248 patients. Bone Joint J 95-B:966–971.
Nouri A, Tetreault L, Dalzell K, Zamorano JJ, Fehlings MG (2017) The relationship between preoperative clinical presentation and quantitative magnetic resonance imaging features in patients with degenerative cervical myelopathy. Neurosurgery 80:121–128
Nouri A, Tetreault L, Zamorano JJ et al (2015). Role of magnetic resonance imaging in predicting surgical outcome in patients with cervical spondylotic myelopathy. Spine (Phila Pa 1976) 40:171–178.
Tetreault LA, Côté P, Kopjar B et al (2015) A clinical prediction model to assess surgical outcome in patients with cervical spondylotic myelopathy: Internal and external validations using the prospective multicenter AOSpine north american and international datasets of 743 patients. Spine J 15:388–397
Kim B, Yoon DH, Shin HC et al (2015) Surgical outcome and prognostic factors of anterior decompression and fusion for cervical compressive myelopathy due to ossification of the posterior longitudinal ligament. Spine J 15:875–884
Uchida K, Nakajima H, Takeura N et al (2014) Prognostic value of changes in spinal cord signal intensity on magnetic resonance imaging in patients with cervical compressive myelopathy. Spine J 14:1601–1610
Tetreault L, Palubiski LM, Kryshtalskyj M et al (2018) Significant predictors of outcome following surgery for the treatment of degenerative cervical myelopathy: a systematic review of the literature. Neurosurg Clin N Am 29:115-127.e35
Karpova A, Arun R, Davis AM et al (2013) Predictors of surgical outcome in cervical spondylotic myelopathy. Spine (Phila Pa 1976) 38:392–400.
Morio Y, Teshima R, Nagashima H et al (2001) Correlation between operative outcomes of cervical compression myelopathy and mri of the spinal cord. Spine (Phila Pa 1976) 26:1238–1245.
Acknowledgements
We appreciate the clinical Research Development Center of Imam Reza Hospital for their wise advice.
Funding
There was no external source of funding.
Author information
Authors and Affiliations
Contributions
EA, MN, HS, and SRB had the idea for this study. EA, AA, HS, and SA participated in outlining the concept and design. MN, SA, and AA did the data acquisition. EA, SVE, and SH did the statistical analysis and wrote the first draft of the manuscript. EA, SVE, SH, SA, and HS revised the final manuscript. All authors have read and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethics approval and consent to participate
The study received ethics approval by the Kermanshah University of Medical Science Ethics Committee. Written informed consent to participate was obtained from all patients. All methods were carried out in accordance with relevant guidelines and regulations.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Moradi, F., Bagheri, S.R., Saeidiborojeni, H. et al. Predictors of poor clinical outcome in patients with cervical spondylotic myelopathy undergoing cervical laminectomy and fusion. Musculoskelet Surg 107, 77–83 (2023). https://doi.org/10.1007/s12306-021-00731-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12306-021-00731-w