Abstract
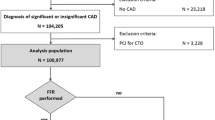
The utilization of FFR remains low. Our study evaluated the per-vessel prognostic value of computational pressure-flow dynamics-derived FFR (caFFR) among patients with stable coronary artery disease. A total of 3329 vessels from 1308 patients were included and analysed. They were stratified into ischaemic (caFFR ≤ 0.8) and non-ischaemic (caFFR > 0.8) cohorts, and the associations between PCI and outcomes were evaluated. The third cohort comprised all included vessels, and the associations between treatment adherent-to-caFFR (PCI in vessels with caFFR ≤ 0.8 and no PCI in vessels with caFFR > 0.8) and outcomes were evaluated. The primary outcome was VOCE, defined as a composite of vessel-related cardiovascular mortality, non-fatal myocardial infarction, and repeat revascularization. PCI was associated with a lower 3-year risk of VOCE in the ischaemic cohort (HR, 0.44; 95% CI, 0.26–0.74; P = 0.002) but not in the non-ischaemic cohort. The risk of VOCE was lower in the adherent-to-caFFR group (n = 2649) (HR, 0.69; 95% CI, 0.48–0.98; P = 0.039).
Graphical Abstract
A novel index that uses coronary angiography images to estimate FFR may have substantial clinical value in guiding management among patients with stable coronary artery disease.




Similar content being viewed by others
Data Availability
Data are available on reasonable request.
Abbreviations
- caFFR:
-
Computational pressure-flow dynamics-derived fractional flow reserve
- CFD:
-
Computational fluid dynamics
- CI:
-
Confidence interval
- CPFD:
-
Computational pressure-flow dynamics
- FFR:
-
Fractional flow reserve
- GEE:
-
Generalized estimating equations
- HR:
-
Hazard ratio
- VOCE:
-
Vessel-oriented composite endpoint
References
De Bruyne B, Pijls NHJ, Kalesan B, Barbato E, Tonino PAL, Piroth Z, et al. Fractional flow reserve–guided pci versus medical therapy in stable coronary disease. N Engl J Med. 2012;367(11):991–1001.
Tonino PAL, De Bruyne B, Pijls NHJ, Siebert U, Ikeno F, van `t Veer M, et al. Fractional flow reserve versus angiography for guiding percutaneous coronary intervention. N Engl J Med. 2009;360(3):213–24.
Sud M, Han L, Koh M, Austin PC, Farkouh ME, Ly HQ, et al. Association between adherence to fractional flow reserve treatment thresholds and major adverse cardiac events in patients with coronary artery disease. JAMA. 2020;324(23):2406–14. https://doi.org/10.1001/jama.2020.22708
Patel MR, Calhoon JH, Dehmer GJ, Grantham JA, Maddox TM, Maron DJ, et al. ACC/AATS/AHA/ASE/ASNC/SCAI/SCCT/STS 2017 Appropriate use criteria for coronary revascularization in patients with stable ischemic heart disease: a report of the American College of Cardiology Appropriate Use Criteria Task Force, American Association for Thoracic Surgery, American Heart Association, American Society of Echocardiography, American Society of Nuclear Cardiology, Society for Cardiovascular Angiography and Interventions, Society of Cardiovascular Computed Tomography, and Society of Thoracic Surgeons. J Am Coll Cardiol. 2017;69:2212–41.
Li J, Elrashidi MY, Flammer AJ, Lennon RJ, Bell MR, Holmes DR, et al. Long-term outcomes of fractional flow reserve-guided vs. angiography-guided percutaneous coronary intervention in contemporary practice. Eur Heart J. 2013;34:1375–83.
Xu B, Tu S, Qiao S, Qu X, Chen Y, Yang J, et al. Diagnostic accuracy of angiography-based quantitative flow ratio measurements for online assessment of coronary stenosis. J Am Coll Cardiol. 2017;70:3077–87.
Fearon WF, Achenbach S, Engstrom T, Assali A, Shlofmitz R, Jeremias A, et al. Accuracy of fractional flow reserve derived from coronary angiography. Circulation. 2019;139(4):477–84.
Masdjedi K, van Zandvoort LJC, Balbi MM, Gijsen FJH, Ligthart JMR, Rutten MCM, et al. Validation of a three-dimensional quantitative coronary angiography-based software to calculate fractional flow reserve: the FAST study. EuroIntervention. 2020;16:591–9.
Li J, Gong Y, Wang W, Yang Q, Liu B, Lu Y, et al. Accuracy of computational pressure-fluid dynamics applied to coronary angiography to derive fractional flow reserve: FLASH FFR. Cardiovasc Res. 2020;116:1349–56.
Ai H, Zheng N, Li L, Yang G, Li H, Tang G, et al. Agreement of angiography-derived and wire-based fractional flow reserves in percutaneous coronary intervention. Front Cardiovasc Med. 2021;8:654392.
Xu B, Tu S, Song L, Jin Z, Yu B, Fu G, et al. Angiographic quantitative flow ratio-guided coronary intervention (FAVOR III China): a multicentre, randomised, sham-controlled trial. Lancet. 2021;398(10317):2149–59.
Chen X, Zhang D, Yin D, Li J, Zhao Z, Wang H, et al. Can “true bifurcation lesion” actually be regarded as an independent risk factor of acute side branch occlusion after main vessel stenting?: a retrospective analysis of 1,200 consecutive bifurcation lesions in a single center. Catheter Cardiovasc Interv. 2016;87(Suppl 1):554–63.
Biscaglia S, Tebaldi M, Brugaletta S, Cerrato E, Erriquez A, Passarini G, et al. Prognostic value of QFR measured immediately after successful stent implantation: the international multicenter prospective HAWKEYE study. JACC Cardiovasc Interv. 2019;12(20):2079–88.
Kogame N, Takahashi K, Tomaniak M, Chichareon P, Modolo R, Chang CC, et al. Clinical implication of quantitative flow ratio after percutaneous coronary intervention for 3-vessel disease. JACC Cardiovasc Interv. 2019;12(20):2064–75.
Piroth Z, Toth GG, Tonino PAL, Barbato E, Aghlmandi S, Curzen N, et al. Prognostic value of fractional flow reserve measured immediately after drug-eluting stent implantation. Circ: Cardiovasc Interv. 2017;10(8):e005233.
Thygesen K, Alpert JS, Jaffe AS, Chaitman BR, Bax JJ, Morrow DA, et al. Fourth universal definition of myocardial infarction (2018). Eur Heart J. 2018;40(3):237–69.
Xie J, Liu C. Adjusted Kaplan-Meier estimator and log-rank test with inverse probability of treatment weighting for survival data. Stat Med. 2005;24(20):3089–110.
Cox DR. Regression models and life-tables. J R Stat Soc Ser B (Methodological). 1972;34(2):187–220.
Zeger SL, Liang KY. Longitudinal data analysis for discrete and continuous outcomes. Biometrics. 1986;42(1):121–30.
Hanley JA, Negassa A, Edwardes MDD, Forrester JE. Statistical analysis of correlated data using generalized estimating equations: an orientation. Am J Epidemiol. 2003;157(4):364–75.
Austin PC. The performance of different propensity score methods for estimating marginal hazard ratios. Stat Med. 2013;32(16):2837–49.
Parikh RV, Liu G, Plomondon ME, Sehested TSG, Hlatky MA, Waldo SW, et al. Utilization and outcomes of measuring fractional flow reserve in patients with stable ischemic heart disease. J Am Coll Cardiol. 2020;75:409–19.
Tu S, Barbato E, Köszegi Z, Yang J, Sun Z, Holm NR, et al. Fractional flow reserve calculation from 3-dimensional quantitative coronary angiography and TIMI frame count: a fast computer model to quantify the functional significance of moderately obstructed coronary arteries. JACC Cardiovasc Interv. 2014;7:768–77.
Papafaklis MI, Muramatsu T, Ishibashi Y, Lakkas LS, Nakatani S, Bourantas CV, et al. Fast virtual functional assessment of intermediate coronary lesions using routine angiographic data and blood flow simulation in humans: comparison with pressure wire - fractional flow reserve. EuroIntervention. 2014;10:574–83.
Tröbs M, Achenbach S, Röther J, Redel T, Scheuering M, Winneberger D, et al. Comparison of fractional flow reserve based on computational fluid dynamics modeling using coronary angiographic vessel morphology versus invasively measured fractional flow reserve. Am J Cardiol. 2016;117:29–35.
Tu S, Westra J, Yang J, von Birgelen C, Ferrara A, Pellicano M, et al. Diagnostic accuracy of fast computational approaches to derive fractional flow reserve from diagnostic coronary angiography: the international multicenter FAVOR pilot study. JACC Cardiovasc Interv. 2019;9:2024–35.
Collet C, Onuma Y, Sonck J, Asano T, Vandeloo B, Kornowski R, et al. Diagnostic performance of angiography-derived fractional flow reserve: a systematic review and Bayesian meta-analysis. Eur Heart J. 2018;39(35):3314–21.
Ahn J-M, Park D-W, Shin E-S, Koo B-K, Nam C-W, Doh J-H, et al. Fractional flow reserve and cardiac events in coronary artery disease. Circulation. 2017;135(23):2241–51.
Belle EV, Rioufol G, Pouillot C, Cuisset T, Bougrini K, Teiger E, et al. Outcome impact of coronary revascularization strategy reclassification with fractional flow reserve at time of diagnostic angiography. Circulation. 2014;129(2):173–85.
Koo BK, Erglis A, Doh JH, Daniels DV, Jegere S, Kim HS, et al. Diagnosis of ischemia-causing coronary stenoses by noninvasive fractional flow reserve computed from coronary computed tomographic angiograms. Results from the prospective multicenter DISCOVER-FLOW (Diagnosis of Ischemia-Causing Stenoses Obtained Via Noninvasive Fractional Flow Reserve) study. J Am Coll Cardiol. 2011;58:1989–97.
Acknowledgements
We thank the medical staff of the Division of Cardiology, Queen Mary Hospital for their support during this study.
Funding
This work was supported by HKU-SZH Fund for Shenzhen Key Medical Discipline, Grant Number: SZXK2020081, and Sanming Project of Cardiology, the university of Hong Kong Shenzhen hospital, Sanming Grant from the Ministry of Health, Shenzhen, China, Grant Number: SZSM201911020.
Author information
Authors and Affiliations
Contributions
Study concept and design: CKLL, LYL, KYL, KHY. Data analysis and interpretation: CKLL, LYL, KYL, YF, SYY. Manuscript drafting: CKLL, LYL, KYL, KHY. Critical revision of the manuscript and intellectual input: CKLL, GC, MW, RW, MZW, QWR, SYY, YKT, HLL, HFT, BX. Guarantor: KHY.
Corresponding author
Ethics declarations
Human Subjects
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000. This study was approved by the ethics committee of the West Cluster Hospital Authority of Hong Kong. The need for informed consent was waived.
Animal Studies
No animal studies were carried out by the authors for this article.
Conflict of Interest
KHY receives research support from Novartis; consultancy fees from service on the Advisory Board/Steering Committee for Abbott Diagnostics, Bayer, Boehringer Ingelheim, Boston Scientific, Medtronic, and Novartis. All other authors report no conflict of interest.
Additional information
Associate Editor Yihua Bei oversaw the review of this article
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Clinical Relevance
This study, to the best of our knowledge, is the first to demonstrate a favourable clinical performance in patients with stable CAD by adhering to values derived by a non-wire-based per-vessel angiography-derived functional assessment. These findings support the use of caFFR and its potential for widespread application in clinical practice.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Leung, C.KL., Lam, LY., Li, KY. et al. Clinical Value of Computational Angiography-derived Fractional Flow Reserve in Stable Coronary Artery Disease. J. of Cardiovasc. Trans. Res. 16, 1166–1176 (2023). https://doi.org/10.1007/s12265-023-10381-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-023-10381-x