Summary
Purpose
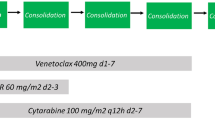
To analyze the effectiveness of decitabine combined with low-dose Ara‑C, aclarubicin, and rhG-CSF (DCAG) as a salvage therapy in patients with relapsed/refractory (R/R) acute myeloid leukemia (AML).
Patients and methods
This single-centered retrospective study included patients with relapsed/refractory AML between January 2013 and June 2020. The response rate and survival were calculated, and their correlations with clinical characteristics were estimated.
Results
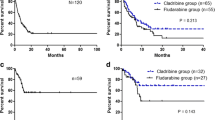
Thirty-seven patients were enrolled. The overall response rate (ORR) was 56.8% with a complete remission (CR) rate of 51.4%. For patients with non-refractory and refractory AML, the CR rates were 87.5% and 30.4%, respectively (p < 0.001). No remission was found in four primary refractory AML. The incidence of infections was 73%, wherein 13.5% had severe infection, and 2.7% with treatment-related mortality. The median overall survival (OS) and relapse-free survival (RFS) were 10.6 (7.7–13.5) months and 5.0 (2.8–7.2) months, respectively. Patients in the poor risk category had a shorter OS (P = 0.004). The OS and RFS of patients with a recurrence time of < 6 months were shorter (P = 0.018 and P < 0.001, respectively).
Conclusions
The DCAG regimen was an effective and well-tolerated therapeutic alternative for R/R AML, particularly in non-refractory patients. Patients in the poor risk category and early relapse were adverse factors for remission rate and survival.






Similar content being viewed by others
References
Döhner H, Estey E, Grimwade D, et al. Diagnosis and management of AML in adults:2017 ELN recommendations from an international expert panel. Blood. 2017;129(4):424–47.
Walter RB, Othus M, Brunett AK, et al. Resistance prediction in AML: analysis of 4601 patients from MRC/NCRI,HOVON/SAKK,SWOG and MD Anderson Cancer Center. Leukemia. 2015;29(2):312–20.
Cui L, Liu Y, Pang Y, et al. Emerging agents and regimens for treatment of relapsed and refractory acute myeloid leukemia. Cancer Gene Ther. 2020;27(1-2):1–14.
Ganzel C, Sun Z, Cripe LD, et al. Very poor long-term survival in past and more recent studies for relapsed AML patients: The ECOG-ACRIN experience. Am J Hematol. 2018;93(8):1074–81.
Kim TK, Gore SD, Zeidan AM. Epigenetic therapy in acute myeloid leukemia: current and future directions. Semin Hematol. 2015;52(3):172–83.
Negrotto S, Ng KP, Jankowska AM, et al. CpG methylation patterns and decitabine treatment response in acute myeloid leukemia cells and normal hematopoietic precursors. Leukemia. 2012;26(2):244–54.
Jiang X, Wang Z, Ding B, et al. The hypomethylating agent decitabine prior to chemotherapy improves the therapy efficacy in refractory/relapsed acute myeloid leukemia patients. Oncotarget. 2015;6(32):33612–22.
Song LX, Xu L, Li X, et al. Clinical outcome of treatment with a combined regimen of decitabine and aclacinomycin/cytarabine for patients with refractory acute myeloid leukemia. Ann Hematol. 2012;91(12):1879–86.
Megías-Vericat JE, Martínez-Cuadrón D, Sanz MÁ, et al. Salvage regimens using conventional chemotherapy agents for relapsed/refractory adult AML patients: a systematic literature review. Ann Hematol. 2018;97(7):1115–53.
Tiong IS, Wei AH. New drugs creating challenges in acute myeloid leukemia. Genes Chromosomes. Cancer. 2019;58(12):903–14.
Thol F. What to use to treat AML: the role of emerging therapies. Hematology Am Soc Hematol Educ Program. 2021;2021(1):16–23.
Tawfik B, Sliesoraitis S, Lyerly S, et al. Efficacy of the hypomethylating agents as frontline, salvage, or consolidation therapy in adults with acute myeloid leukemia (AML). Ann Hematol. 2014;93(1):47–55.
Stahl M, DeVeaux M, Montesinos P, et al. Hypomethylating agents in relapsed and refractory AML:outcomes and their predictors in a large international patient cohort. Blood Adv. 2018;2(8):923–32.
Ritchie EK, Feldman EJ, Christos PJ, et al. Decitabine in patients with newly diagnosed and relapsed acute myeloid leukemia. Leuk Lymphoma. 2013;54(9):2003–7.
Lee SR, Yang DH, Ahn JS, et al. The clinical outcome of FLAG chemotherapy without idarubicin in patients with relapsed or refractory acute myeloid leukemia. J Korean Med Sci.2009;24(3):498–503.
Wang LJ, Ding J, Zhu CY, et al. Clinic outcome of FLAG regimen treating patients with refractory and relapse acute myeloid leukemia. J Exp Hematol. 2016;24(1):19–24.
Martin MG, Welch JS, Augustin K, et al. Cladribine in the treatment of acute myeloid leukemia: a single-institution experience. Clin Lymphoma Myeloma. 2009;9(4):298–301.
Price SL, Lancet JE, George TJ, et al. Salvage chemotherapy regimens for acute myeloid leukemia: is one better efficacy comparison between CLAG and MEC regimens. Leuk Res. 2011;35(3):301–4.
Trifilio SM, Rademaker AW, Newman D, et al. Mitoxantrone and etoposide with or without intermediate dose cytarabine for the treatment of primary induction failure or relapsed acute myeloid leukemia. Leuk Res. 2012;36(4):394–6.
Kohrt HE, Patel S, Ho M, et al. Second-line mitoxantrone, etoposide, and cytarabine for acute myeloid leukemia: a single-center experience. Am J Hematol. 2010;85(11):877–81.
Fan CH, Yu MJ, Mai MY, et al. Efficacy of HAA regimen in the treatment of 64 patients with refractory/relapsed acute myeloid leukemia. Chin J Hematol. 2016;37(2):100–4.
Li L, Zhang X, Yu H, et al. Low-dose hypomethylating agent decitabine in combination with aclacinomycin and cytarabine achieves a better outcome than standard FLAG chemotherapy in refractory/relapsed acute myeloid leukemia patients with poor-risk cytogenetics and mutations. Onco Targets Ther. 2018;11:6863–70.
Chen Y, Dai M, Liu Q. Efficacy and safety of DAC combined with CAG regimen (decitabine in combined with aclacinomycin, cytarabine and G‑CSF) as a second induction regimen compared with Non-DAC regimen for acute myeloid leukemia who failed the first course of standard induction IA chemotherapy. Blood. 2019;134((sup1):5104–5104.
Wang L, Luo J, Chen G, et al. Chidamide, decitabine, cytarabine, aclarubicin, and granulocyte colony-stimulating factor (CDCAG) in patients with relapsed/refractory acute myeloid leukemia: a single-arm, phase 1/2 study. Clin Epigenetics. 2020;12(1):132.
Kadia TM, Jain P, Ravandi F, et al. TP53 mutations in newly diagnosed acute myeloid leukemia: Clinicomolecular characteristics, response to therapy, and outcomes. Cancer. 2016;122(22):3484–91.
Hunter AM, Sallman DA. Current status and new treatment approaches in TP53 mutated AML. Best Pract Res Clin Haematol. 2019;32(2):134–44.
Rücker FG, Schlenk RF, Bullinger L, et al. TP53 alterations in acute myeloid leukemia with complex karyotype correlate with specific copy number alterations, monosomal karyotype, and dismal outcome. Blood. 2012;119(9):2114–21.
Hou HA, Chou WC, Kuo YY, et al. TP53 mutations in de novo acute myeloid leukemia patients: longitudinal follow-ups show the mutation is stable during disease evolution. Blood Cancer J. 2015;5(7):e331.
Welch JS, Petti AA, Miller CA, et al. TP53 and Decitabine in Acute Myeloid Leukemia and Myelodysplastic Syndromes. N Engl J Med. 2016;375(21):2023–36.
Acknowledgements
We thank the staff at the Department of Hematology, The First Hospital of Jilin University, for their assistance with this work.
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Y. Fu, L. Su, Y. Li and Y. Tan declare that they have no competing interests.
Ethical standards
Ethics approval: This study was approved by the Ethics Committee of The First Hospital of Jilin University (approval number: 2023–515) and conducted in accordance with the Declaration of Helsinki. Consent to participate: Informed consent was obtained from all individual participants included in the study. Consent to publish: All the participants had consented to the submission to the journal.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fu, Y., Su, L., Li, Y. et al. Decitabine combined with low-dose cytarabine, aclarubicin and rhG-CSF regimen may be a potential alternative for relapsed/refractory acute myeloid leukemia: A single-center study. memo (2023). https://doi.org/10.1007/s12254-023-00933-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12254-023-00933-x