Abstract
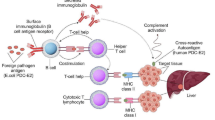
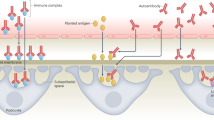
Besides genetic susceptibility, infections due to viruses, bacteria and protozoa have been implicated in the development of autoimmune diseases (AD). AD can be triggered in a genetically susceptible individual by infections that disrupt immunological tolerance towards self-antigens. Pathogens can initiate autoimmunity by way of molecular mimicry, bystander activation, epitope spreading or persistent infection with polyclonal activation. This review covers two main topics: (i) the mechanisms by which an infectious agent can trigger or worsen autoimmunity; and (ii) the correlation between specific infectious agents and AD in humans with special emphasis on multisystem inflammatory syndrome in children (MIS-C).
Similar content being viewed by others
References
Tangye SG, Al-Herz W, Bousfiha A, et al. Human inborn errors of immunity: 2022 update on the classification from the International Union of Immunological Societies Expert Committee. J Clin Immunol. 2022;42:1473–507.
Schoenfeld Y, Isenberg D. The mosaic of autoimmunity. Immunol Today. 1989;10:123–6.
Floreani A, Leung PS, Gershwin ME. Environmental basis of autoimmunity. Clin Rev Allergy Immunol. 2016;50:287–300.
Delogu LG, Deidda S, Delitala G, Manetti R. Infectious diseases and autoimmunity. J Infect Dev Ctries. 2011;5:679–87.
Kivity S, Agmon-Levin N, Blank M, Shoenfeld Y. Infections and autoimmunity - friends or foes? Trends Immunol. 2009;30:409–14.
Kudat H, Telci G, Sozen AB, et al. The role of HLA molecules in susceptibility to chronic rheumatic heart disease. Int J Immunogenet. 2006;33:41–4.
Wanstrat A, Wakeland E. The genetics of complex autoimmune diseases: Non-MHC susceptibility genes. Nat Immunol. 2001;2:802–9.
Galli L, Chiappini E, de Martino M. Infections and autoimmunity. Pediatr Infect Dis J. 2012;31:1295–7.
Anaya J-M, Shoenfeld Y, Rojas-Villarraga A, Levy RA, Cervera R. Autoimmunity: From Bench to Bedside [Internet]. Bogota (Colombia): El Rosario University Press; 2013 Jul 18. PMID: 29087650.
Arbuckle MR, McClain MT, Rubertone MV, et al. Development of autoantibodies before the clinical onset of systemic lupus erythematosus. New Engl J Med. 2003;349:1526–33.
Riphagen S, Gomez X, Gonzalez-Martinez C, Wilkinson N, Theocharis P. Hyperinflammatory shock in children during COVID-19 pandemic. Lancet. 2020;395:1607–8.
Verdoni L, Mazza A, Gervasoni A, et al. An outbreak of severe Kawasaki-like disease at the Italian epicentre of the SARS-CoV-2 epidemic: An observational cohort study. Lancet. 2020;395:1771–8.
McMurray JC, May JW, Cunningham MW, Jones OY. Multisystem inflammatory syndrome in children (MIS-C), a post-viral myocarditis and systemic vasculitis—a critical review of its pathogenesis and treatment. Front Pediatr. 2020;8:626182.
Bartsch YC, Wang C, Zohar T, et al. Humoral signatures of protective and pathological SARS-CoV-2 infection in children. Nat Med. 2021;27:454–62.
Carter MJ, Fish M, Jennings A, et al. Peripheral immunophenotypes in children with multisystem inflammatory syndrome associated with SARS-CoV-2 infection. Nat Med. 2020;26:1701–7.
Lee PY, Day-Lewis M, Henderson LA, et al. Distinct clinical and immunological features of SARS-CoV-2-induced multisystem inflammatory syndrome in children. J Clin Invest. 2020;130:5942–50.
Shulman ST. Pediatric coronavirus disease-2019–associated multisystem inflammatory syndrome. J Pediatric Infect Dis Soc. 2020;9:285–6.
Sharma C, Ganigara M, Galeotti C, et al. Multisystem inflammatory syndrome in children and Kawasaki disease: A critical comparison. Nat Rev Rheumatol. 2021;17:731–48.
Diorio C, McNerney KO, Lambert M, et al. Evidence of thrombotic microangiopathy in children with SARS-CoV-2 across the spectrum of clinical presentations. Blood Adv. 2020;4:6051–63.
Kaushik S, Aydin SI, Derespina KR, et al. Multisystem inflammatory syndrome in children associated with severe acute respiratory syndrome coronavirus 2 infection (MIS-C): A multi-institutional study from New York City. J Pediatr. 2020;224:24–9.
Ouldali N, Toubiana J, Antona D, et al; French Covid-19 Paediatric Inflammation Consortium. Association of intravenous immunoglobulins plus methylprednisolone vs immunoglobulins alone with course of fever in multisystem inflammatory syndrome in children. JAMA. 2021;325:855–64.
Nakra NA, Blumberg DA, Herrera-Guerra A, Lakshminrusimha S. Multi-system inflammatory syndrome in children (MIS-C) following SARS-CoV-2 infection: Review of clinical presentation, hypothetical pathogenesis, and proposed management. Children (Basel). 2020;7:69.
Martínez-García JJ, López-Acosta JR, Arce-Cabrera D, et al. Case report: Multisystem inflammatory syndrome in children associated with COVID-19, macrophage activation syndrome, and incomplete Kawasaki disease. Front Pediatr. 2023;11:1167828.
James JA, Neas BR, Moser KL, et al. Systemic lupus erythematosus in adults is associated with previous Epstein-Barr virus exposure. Arthritis Rheum. 2001;44:1122–6.
Toussirot É, Roudier J. Epstein-Barr virus in autoimmune diseases. Best Pract Res Clin Rheumatol. 2008;22:883–96.
Kang I, Quan T, Nolasco H, et al. Defective control of latent Epstein-Barr virus infection in systemic lupus erythematosus. J Immunol. 2004;172:1287–94.
Author information
Authors and Affiliations
Contributions
Both the authors have contributed equally to the drafting of the article and final edits were done by APR. APR will act as guarantor for this manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Rao, A.P., Patro, D. The Intricate Dance of Infections and Autoimmunity: An Interesting Paradox. Indian J Pediatr (2023). https://doi.org/10.1007/s12098-023-04928-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12098-023-04928-8