Abstract
Introduction
Malignant cerebral edema develops in a small subset of patients with hemispheric strokes, precipitating deterioration and death if decompressive hemicraniectomy (DHC) is not performed in a timely manner. Predicting which stroke patients will develop malignant edema is imprecise based on clinical data alone. Head computed tomography (CT) imaging is often performed at baseline and 24-h. We determined the incremental value of incorporating imaging-derived features from serial CTs to enhance prediction of malignant edema.
Methods
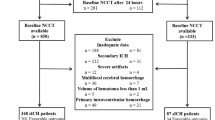
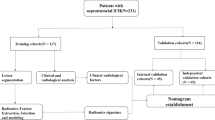
We identified hemispheric stroke patients at three sites with NIHSS ≥ 7 who had baseline as well as 24-h clinical and CT imaging data. We extracted quantitative imaging features from baseline and follow-up CTs, including CSF volume, intracranial reserve (CSF/cranial volume), as well as midline shift (MLS) and infarct-related hypodensity volume. Potentially lethal malignant edema was defined as requiring DHC or dying with MLS over 5-mm. We built machine-learning models using logistic regression first with baseline data and then adding 24-h data including reduction in CSF volume (ΔCSF). Model performance was evaluated with cross-validation using metrics of recall (sensitivity), precision (predictive value), as well as area under receiver-operating-characteristic and precision-recall curves (AUROC, AUPRC).
Results
Twenty of 361 patients (6%) died or underwent DHC. Baseline clinical variables alone had recall of 60% with low precision (7%), AUROC 0.59, AUPRC 0.15. Adding baseline intracranial reserve improved recall to 80% and AUROC to 0.82 but precision remained only 16% (AUPRC 0.28). Incorporating ΔCSF improved AUPRC to 0.53 (AUROC 0.91) while all imaging features further improved prediction (recall 90%, precision 38%, AUROC 0.96, AUPRC 0.66).
Conclusion
Incorporating quantitative CT-based imaging features from baseline and 24-h CT enhances identification of patients with malignant edema needing DHC. Further refinements and external validation of such imaging-based machine-learning models are required.


Similar content being viewed by others
References
Battey TW, Karki M, Singhal AB, Wu O, Sadaghiani S, Campbell BC, Davis SM, Donnan GA, Sheth KN, Kimberly WT. Brain edema predicts outcome after nonlacunar ischemic stroke. Stroke. 2014;45(12):3643–8. https://doi.org/10.1161/STROKEAHA.114.006884.
Broocks G, Flottmann F, Scheibel A, Aigner A, Faizy TD, Hanning U, Leischner H, Broocks SI, Fiehler J, Gellissen S, Kemmling A. Quantitative lesion water uptake in acute stroke computed tomography is a predictor of malignant infarction. Stroke. 2018;49(8):1906–12. https://doi.org/10.1161/STROKEAHA.118.020507.
Krieger DW, Demchuk AM, Kasner SE, Jauss M, Hantson L. Early clinical and radiological predictors of fatal brain swelling in ischemic stroke. Stroke. 1999;30:287–92.
Hacke W, Schwab S, Horn M, Spranger M, De Georgia M, von Kummer R. ‘Malignant’ middle cerebral artery territory infarction: clinical course and prognostic signs. Arch Neurol. 1996;53:309–15.
Berrouschot J, Sterker M, Bettin S, Köster J, Schneider D. Mortality of space-occupying (‘malignant’) middle cerebral artery infarction under conservative intensive care. Intensive Care Med. 1998;24:620–3.
Vahedi K, Hofmeijer J, Juettler E, Vicaut E, George B, Algra A, Amelink GJ, Schmiedeck P, Schwab S, Rothwell PM, Bousser M-G, van der Worp HB, Hacke W. Early decompressive surgery in malignant infarction of the middle cerebral artery: a pooled analysis of three randomised controlled trials. Lancet Neurol. 2007;6:215–22. https://doi.org/10.1016/S1474-4422(07)70036-4.
Silver FL, Norris JW, Lewis AJ, Hachinski VC. Early mortality following stroke: a prospective review. Stroke. 1984;15:492–6. https://doi.org/10.1161/01.STR.15.3.492.
Heinsius T, Bogousslavsky J, Van Melle G. Large infarcts in the middle cerebral artery territory. Etiology and outcome patterns. Neurology. 1998;50:341–50.
Hofmeijer J, Algra A, Kappelle LJ, van der Worp HB. Predictors of life-threatening brain edema in middle cerebral artery infarction. Cerebrovasc Dis (Basel, Switzerland). 2008;25:176–84. https://doi.org/10.1159/000113736.
Thomalla G, Hartmann F, Juettler E, Singer OC, Lehnhardt F-G, Köhrmann M, Kersten JF, Krützelmann A, Humpich MC, Sobesky J, Gerloff C, Villringer A, Fiehler J, Neumann-Haefelin T, Schellinger PD, Röther J. Prediction of malignant middle cerebral artery infarction by magnetic resonance imaging within 6 hours of symptom onset: a prospective multicenter observational study. Ann Neurol. 2010;68:435–45. https://doi.org/10.1002/ana.22125.
Dhar R, Yuan K, Kulik T, Chen Y, Heitsch L, An H, Ford A, Lee JM. CSF volumetric analysis for quantification of cerebral edema after hemispheric infarction. Neurocrit Care. 2015. https://doi.org/10.1007/s12028-015-0204-z.
Broocks G, Flottmann F, Ernst M, Faizy TD, Minnerup J, Siemonsen S, Fiehler J, Kemmling A. Computed tomography-based imaging of voxel-wise lesion water uptake in ischemic brain: relationship between density and direct volumetry. Invest Radiol. 2018;53(4):207–13. https://doi.org/10.1097/RLI.0000000000000430.
Minnerup J, Wersching H, Ringelstein EB, Heindel W, Niederstadt T, Schilling M, Schäbitz W-R, Kemmling A. Prediction of malignant middle cerebral artery infarction using computed tomography-based intracranial volume reserve measurements. Stroke. 2011;42:3403–9. https://doi.org/10.1161/STROKEAHA.111.619734.
Kauw F, Bennink E, de Jong H, Kappelle LJ, Horsch AD, Velthuis BK, Dankbaar JW, Investigators D, follows Diaa. Intracranial cerebrospinal fluid volume as a predictor of malignant middle cerebral artery infarction. Stroke. 2019;50:1437–43. https://doi.org/10.1161/strokeaha.119.024882.
Dhar R, Chen Y, Hamzehloo A, Kumar A, Heitsch L, He J, Chen L, Slowik A, Strbian D, Lee JM. Reduction in Cerebrospinal Fluid Volume as an Early Quantitative Biomarker of Cerebral Edema After Ischemic Stroke. Stroke. 2020;51(2):462–7. https://doi.org/10.1161/STROKEAHA.119.027895.
Ong CJ, Gluckstein J, Laurido-Soto O, Yan Y, Dhar R, Lee JM. Enhanced detection of edema in malignant anterior circulation stroke (EDEMA) score: a risk prediction tool. Stroke. 2017;48(7):1969–72. https://doi.org/10.1161/STROKEAHA.117.016733.
Thoren M, Azevedo E, Dawson J, Egido JA, Falcou A, Ford GA, Holmin S, Mikulik R, Ollikainen J, Wahlgren N, Ahmed N. Predictors for cerebral edema in acute ischemic stroke treated with intravenous thrombolysis. Stroke. 2017;48(9):2464–71. https://doi.org/10.1161/STROKEAHA.117.018223.
Dhar R, Chen Y, An H, Lee JM. Application of machine learning to automated analysis of cerebral edema in large cohorts of ischemic stroke patients. Front Neurol. 2018;9:687. https://doi.org/10.3389/fneur.2018.00687.
Chen Y, Dhar R, Heitsch L, Ford A, Fernandez-Cadenas I, Carrera C, Montaner J, Lin W, Shen D, An H, Lee JM. Automated quantification of cerebral edema following hemispheric infarction: application of a machine-learning algorithm to evaluate CSF shifts on serial head CTs. Neuroimage Clin. 2016;12:673–80. https://doi.org/10.1016/j.nicl.2016.09.018.
Saito T, Rehmsmeier M. The precision-recall plot is more informative than the ROC plot when evaluating binary classifiers on imbalanced datasets. PLoS One. 2015;10(3):e0118432. https://doi.org/10.1371/journal.pone.0118432.
Park J, Goh D-H, Sung J-K, Hwang Y-H, Kang D-H, Kim Y. Timely assessment of infarct volume and brain atrophy in acute hemispheric infarction for early surgical decompression: strict cutoff criteria with high specificity. Acta Neurochir. 2012;154:79–85. https://doi.org/10.1007/s00701-011-1178-z.
Broocks G, Kemmling A, Aberle J, Kniep H, Bechstein M, Flottmann F, Leischner H, Faizy TD, Nawabi J, Schon G, Sporns P, Thomalla G, Fiehler J, Hanning U. Ischemic lesion water uptake in acute stroke: Is blood glucose related to cause and effect? J Stroke. 2019;21(3):347–9. https://doi.org/10.5853/jos.2019.01935.
Diprose WK, Diprose JP, Wang MTM, Tarr GP, McFetridge A, Barber PA. Automated measurement of cerebral atrophy and outcome in endovascular thrombectomy. Stroke. 2019;50(12):3636–8. https://doi.org/10.1161/STROKEAHA.119.027120.
Liu Y, Chen PC, Krause J, Peng L. How to read articles that use machine learning: users’ guides to the medical literature. JAMA. 2019;322(18):1806–16. https://doi.org/10.1001/jama.2019.16489.
Counsell C, Dennis M. Systematic review of prognostic models in patients with acute stroke. Cerebrovasc Dis. 2001;12(3):159–70. https://doi.org/10.1159/000047699.
Kimberly WT, Bevers MB, von Kummer R, Demchuk AM, Romero JM, Elm JJ, Hinson HE, Molyneaux BJ, Simard JM, Sheth KN. Effect of IV glyburide on adjudicated edema endpoints in the GAMES-RP Trial. Neurology. 2018;91(23):e2163–9. https://doi.org/10.1212/WNL.0000000000006618.
Vorasayan P, Bevers MB, Beslow LA, Sze G, Molyneaux BJ, Hinson HE, Simard JM, von Kummer R, Sheth KN, Kimberly WT. Intravenous glibenclamide reduces lesional water uptake in large hemispheric infarction. Stroke. 2019;50:3021–327. https://doi.org/10.1161/strokeaha.119.026036.
Horsch AD, Dankbaar JW, Stemerdink TA, Bennink E, van Seeters T, Kappelle LJ, Hofmeijer J, de Jong HW, van der Graaf Y, Velthuis BK, investigators D. Imaging findings associated with space-occupying edema in patients with large middle cerebral artery infarcts. AJNR Am J Neuroradiol. 2016. https://doi.org/10.3174/ajnr.A4637.
Jo K, Bajgur SS, Kim H, Choi HA, Huh PW, Lee K. A simple prediction score system for malignant brain edema progression in large hemispheric infarction. PLoS One. 2017;12(2):e0171425. https://doi.org/10.1371/journal.pone.0171425.
Hoelter P, Muehlen I, Goelitz P, Beuscher V, Schwab S, Doerfler A. Automated ASPECT scoring in acute ischemic stroke: comparison of three software tools. Neuroradiology. 2020. https://doi.org/10.1007/s00234-020-02439-3.
Ramos LA, van der Steen WE, Sales Barros R, Majoie C, van den Berg R, Verbaan D, Vandertop WP, Zijlstra I, Zwinderman AH, Strijkers GJ, Olabarriaga SD, Marquering HA. Machine learning improves prediction of delayed cerebral ischemia in patients with subarachnoid hemorrhage. J Neurointerv Surg. 2019;11(5):497–502. https://doi.org/10.1136/neurintsurg-2018-014258.
Ho KC, Speier W, El-Saden S, Liebeskind DS, Saver JL, Bui AA, Arnold CW. Predicting discharge mortality after acute ischemic stroke using balanced data. AMIA Annu Symp Proc. 2014;2014:1787–96.
Ge Y, Wang Q, Wang L, Wu H, Peng C, Wang J, Xu Y, Xiong G, Zhang Y, Yi Y. Predicting post-stroke pneumonia using deep neural network approaches. Int J Med Inform. 2019;132:103986. https://doi.org/10.1016/j.ijmedinf.2019.103986.
Funding
This work was supported by grants from the National Institutes of Health to JML (R01NS085419), RD (K23NS099440), DM (P30NS098577) and LH (K23NS099487).
Author information
Authors and Affiliations
Contributions
All authors were involved in study concept and design and in critical revision of the manuscript for important intellectual content. AH, AK, YC and LH were involved in data acquisition and cleaning. HMF performed the data analysis. RD was involved in interpretation of results and in drafting the manuscript, along with HMF. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
No authors have any conflicts of interest to disclose.
Informed consent
All research was conducted under approval of the institutional ethics review board and all subjects or legally authorized representatives provided informed consent for data collection.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This work was performed at Washington University in St. Louis.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Foroushani, H.M., Hamzehloo, A., Kumar, A. et al. Quantitative Serial CT Imaging-Derived Features Improve Prediction of Malignant Cerebral Edema after Ischemic Stroke. Neurocrit Care 33, 785–792 (2020). https://doi.org/10.1007/s12028-020-01056-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-020-01056-5