Abstract
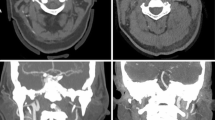
The Morel-Lavallée lesion is an infrequent traumatic lesion that the forensic physician may need to evaluate during examination of a victim. Using a review of the literature and an illustrative case, the objective of this paper is to discuss the medico-legal issues (accountability, functional recovery and healing times, and aftermath) associated with Morel-Lavallée lesions. We describe the case of a 24-year-old motorcycle driver who was hit by a car. Clinically, the right lumbar region had a large 16 × 15 cm ecchymosis with subcutaneous fluid swelling found by palpation. A body scan revealed a Morel-Lavallée lesion among other lesions. On day 7, its thickness was decreased by half. Morel-Lavallée lesions are specifically induced by shearing force with moderate-to-high kinetics in an anatomical area with an underlying fascia. The associated functional disability is globally moderate, but a large lesion or recurrences can extend the time needed to recover. Apart from some exceptions, care without any delay in diagnosis and treatment allows evolution of the lesion without functional consequences, but these lesions are frequently unnoticed in the initial phase.

Similar content being viewed by others
References
Nickerson TP, Zielinski MD, Jenkins DH, Schiller HJ. The Mayo Clinic experience with Morel-Lavallée lesions: establishment of a practice management guideline. J Trauma Acute Care Surg. 2014;76:493–7.
Muneer M, El-Menyar A, Abdelrahman H, Murad MA, Al Harami SM, Mokhtar A, et al. Clinical presentation and management of pelvic Morel–Lavallee injury in obese patients. J Emerg Trauma Shock. 2019;12:40–7.
Bonilla-Yoon I, Masih S, Patel DB, White EA, Levine BD, Chow K, et al. The Morel-Lavallée lesion: pathophysiology, clinical presentation, imaging features, and treatment options. Emerg Radiol. 2014;21:35–43.
Morel-Lavallée VAF. Épanchements traumatiques de sérosité. Arch Générales Médecine Paris. 1853.
Liu M, Liu L, Zhou X, Wu L, Wang J, Qi L, et al. A novel surgical technique for treatment of Morel-Lavallée lesion: endoscopic debridement combined with percutaneous cutaneo-fascial suture. Injury. 2018;49:1630–3.
Moulin C, Barthélémy I, Emering C, D’Incan M. Syndrome de Morel-Lavallée et cytostéatonécrose : deux complications post-traumatiques simulant une dermo-hypodermite infectieuse. Ann Dermatol Vénéréologie. 2017;144:450–4.
Scolaro JA, Chao T, Zamorano DP. The Morel-Lavallée lesion: diagnosis and management. J Am Acad Orthop Surg. 2016;24:667–72.
Lungu E, Michaud J, Bureau NJ. US assessment of sports-related hip injuries. RadioGraphics. 2018;38:867–89.
Khodaee M, Deu RS, Mathern S, Bravman JT. Morel-Lavallée lesion in sports. Curr Sports Med Rep. 2016;15:417–22.
Mellado JM, Bencardino JT. Morel-Lavallée lesion: review with emphasis on MR imaging. Magn Reson Imaging Clin N Am. 2005;13:775–82.
Tejwani SG, Cohen SB, Bradley JP. Management of Morel-Lavallee lesion of the knee: twenty-seven cases in the national football league. Am J Sports Med. 2007;35:1162–7.
Dawre S, Lamba S, Harinatha S, Gupta S, Gupta AK. The Morel-Lavallee lesion: a review and a proposed algorithmic approach. Eur J Plast Surg. 2012;35:489–94.
Greenhill D, Haydel C, Rehman S. Management of the Morel-Lavallée lesion. Orthop Clin North Am. 2016;47:115–25.
Coulibaly NF, Sankale AA, Sy MH, Kinkpe CVA, Kasse AN, Diouf S, et al. Épanchement de Morel-Lavallée en chirurgie orthopédique (À propos de 19 cas). Ann Chir Plast Esthét. 2011;56:27–32.
Anciaux P, Béjui J, Buu-Hoï P, Cantaloube D, Chikhani L, Chodkiewicz JP, et al. Barème indicatif d’évaluation des taux d’incapacité en droit commun. Le concours médical; 2001. http://www.expertisemedicale.be/upload/documents/documentation/Bareme_indicatif_d_evaluation.pdf. Accessed 24 June 2019.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Approval by Ethical Committee is not required for case reports as single case descriptions do not fulfil the criteria of research as defined by the Human Research Act. Patient information has been withheld to protect patient anonymity.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Scanvion, Q., Le Garff, E., Gosset, D. et al. Medico-legal considerations for Morel-Lavallée lesions. Forensic Sci Med Pathol 15, 612–615 (2019). https://doi.org/10.1007/s12024-019-00148-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12024-019-00148-9