Abstract
Purpose
Calcium carbonate was previously shown to interfere with l-thyroxine absorption. To estimate the magnitude of tablet l-thyroxine malabsorption caused by calcium carbonate, with resulting increase in serum thyrotropin (TSH), we performed a cohort study in a referral care center.
Methods
Fifty postmenopausal hypothyroid l-thyroxine-treated women (age 71.7 ± 5.1 years) who added calcium supplementation (600–1000 mg/day) were considered. They were taking l-thyroxine 45–60 min before breakfast (setting 1). After 4.4 ± 2.0 years from initiation of l-thyroxine therapy, they took calcium supplemaentation within 2 h after l-thyroxine taking (setting 2) for 2.3 ± 1.1 years. Hence, we recommended postponing calcium intake 6–8 h after l-thyroxine (setting 3). We evaluated TSH levels, the prevalence of women with elevated TSH (>4.12 mU/L), total cholesterolemia, fasting glycemia, blood pressure, and the prevalence of hypercholesterolemia, hyperglycemia, and hypertension.
Results
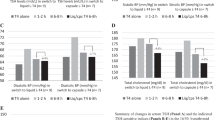
TSH levels were 3.33 ± 1.93 mU/L versus 1.93 ± 0.51 or 2.16 ± 0.54 comparing setting 2 with setting 1 or 3 (P < 0.001, both). In setting 2, 18% women had elevated TSH versus none in setting 1 or 3 (P < 0.01). Total cholesterolemia, fasting glycemia, systolic, and diastolic blood pressure were also significantly higher in setting 2 compared to settings 1 and 3. For every 1.0 mU/L increase within the TSH range of 0.85–6.9 mU/L, total cholesterolemia, glycemia, systolic, and diastolic blood pressure increased by 12.1, 3.12 mg/dL, 2.31, and 2.0 mmHg, respectively.
Conclusions
Monitoring of hypothyroid patients who ingest medications that decrease l-thyroxine absorption should not be restricted to solely measuring serum TSH.




Similar content being viewed by others
References
A. Garmendia Madiaraga, S. Santos Palacios, F. Guillén-Grima, J.C. Galofré, The incidence and prevalence of thyroid dysfunction in Europe: a meta-analysis. J. Clin. Endocrinol. Metab. 99, 923–931 (2014)
J.R. Garber, R.H. Cobin, H. Gharib et al.. Clinical practice guidelines for hypothyroidism for hypothyroidism in adults: cosponsored by the American Association of Clinical Endocrinologists and the American Thyroid Association. Thyroid 22, 1200–1235 (2012)
J. Jonklaas, A.C. Bianco, A.J. Bauer, K.D. Burman, A.R. Cappola, F.S. Celi, D.S. Cooper, B.W. Kim, R.P. Peeters, M.S. Rosenthal, A.M. Sawka, American Thyroid Association Task Force on Thyroid Hormone Replacement. Guidelines for the treatment of hypothyroidism: prepared by the American thyroid association task force on thyroid hormone replacement. Thyroid 24, 1670–1751 (2014)
A. Catalano, N. Morabito, G. Basile, S. Fusco, G. Castagna, F. Reitano, R.C. Albanese, A. Lasco, Fracture risk assessment in postmenopausal women referred to an Italian center for osteoporosis: a single day experience in Messina. Clin. Cases Miner. Bone Metab. 10(3), 191–194 (2013)
N. Singh, P.N. Singh, J.M. Hershman, Effect of calcium carbonate on the absorption of levothyroxine. JAMA 283, 2822–2825 (2000)
J. Ehrenkranz, P.R. Bach, G.L. Snow, A. Schneider, J.L. Lee, S. Ilstrup, S.T. Bennett, S. Benvenga, Circadian and circannual rhythms in thyroid hormones: determining the TSH and free T4 reference intervals based upon time of day, age, and sex. Thyroid 25, 954–961 (2015)
H.B. Burch, K.D. Burman, D.S. Cooper, J.V. Hennessey, A 2013 survey of clinical practice patterns in the management of primary hypothyroidism. J. Clin. Endocrinol. Metab. 99, 2077–2085 (2014)
L. Liwanpo, J.M. Hershman, Conditions and drugs interfering with thyroxine absorption. Best Pract. Res. Clin. Endocrinol. Metab. 23, 781–792 (2009)
P. Colucci, C. Seng Yue, M. Ducharme, S. Benvenga, A review of the pharmacokinetics of levothyroxine for the treatment of hypothyroidism. Eur. Endocrinol. 9, 40–47 (2013)
S. Benvenga, When thyroid hormone replacement is ineffective? Curr. Opin. Endocrinol. Diabetes Obes. 20, 467–477 (2013)
C.R. Schneyer, Calcium carbonate and reduction of levothyroxine efficacy [letter]. JAMA 279, 750 (1998)
I. Zamfirescu, H.E. Carlson, Absorption of levothyroxine when coadministered with various calcium formulations. Thyroid 21, 483–486 (2011)
C.J. Diskin, T.J. Stokes, L.M. Dansby, L. Radcliff, T.B. Carter, Effect of phosphate binders upon TSH and L-thyroxine dose in patients on thyroid replacement. Int. Urol. Nephrol. 39, 599–602 (2007)
S. Benvenga, F. Di Bari, R. Vita, Undertreated hypothyroidism due to calcium oriron supplementation corrected by oral liquid levothyroxine. Endocrine 56, 138–145 (2017)
R. Vita, G. Saraceno, F. Trimarchi, S. Benvenga, Switching levothyroxine from the tablet to the oral solution formulation corrects the impaired absorption oflevothyroxine induced by proton-pump inhibitors. J. Clin. Endocrinol. Metab. 99, 4481–4486 (2014)
R. Vita, F. Di Bari, S. Benvenga, Oral liquid levothyroxine solves the problem of tablet levothyroxine malabsorption due to concomitant intake of multiple drugs. Expert Opin. Drug Deliv. 14, 467–472 (2017)
C. Virili, P. Trimboli, F. Romanelli, M. Centanni, Liquid and softgel levothyroxine use in clinical practice: state of the art. Endocrine 54, 3–14 (2016)
A.M. Formenti, G. Mazziotti, R. Giubbini, A. Giustina, Treatment of hypothyroidism: all that glitters is gold? Endocrine 52, 411–413 (2016)
I.L. Klein, S. Danzi, The cardiovascular system in hypothyroidism. In: Werner and Ingbar’s The thyroid: a fundamental and clinical text, 10th ed, ed. by L.E. Bravermann, D.S. Cooper (Wolters Kluver, Lippincott, Willimas & Wilkins, Philadelphia, 2013), pp. 575–582.
Jahangir Alam, MostNur-E.-TajMokarrama Mukti, Mominul Hoque, Intaz Ali, Mostafa Kamal, SunilC. Mallik, Subhagata Choudhury, Cross sectional evaluation of thyroid hormone levels in non-diabetic and diabetic patients in Bangladeshi population. Asian J. Biol. Sci. 6, 228–233 (2013)
A. Javed, P.B. Balagopal, A. Vella, P.R. Fischer, F. Piccinini, C. Dalla Man, C. Cobelli, P.D. Giesler, J.M. Laugen, S. Kumar, Association between thyrotropin levels and insulin sensitivity in euthyroid obese adolescents. Thyroid 25, 478–484 (2015)
I.M. Benseñor, A.C. Goulart, C. Molina Mdel, É.J. de Miranda, I.S. Santos, P.A. Lotufo, Thyrotropin levels, insulin resistance, and metabolic syndrome: a cross-sectional analysis in the Brazilian Longitudinal Study of Adult Health (ELSA-Brasil). Metab. Syndr. Relat. Disord. 13, 362–369 (2015)
B. Xu, H. Yang, Z. Wang, T. Yang, H. Guo, P. Cheng, W. He, M. Sun, H. Chen, Y. Duan, Elevated thyroid stimulating hormone levels are associated with metabolic syndrome in a Chinese community-based population of euthyroid people aged 40 years and older. J. Biomed. Res 30, 476–482 (2016)
T.N. Le, F.S. Celi, E.P. Wickham 3rd, Thyrotropin levels are associated with cardiometabolic risk factors in euthyroid adolescents. Thyroid 26, 1441–1449 (2016)
H.T. Park, G.J. Cho, K.H. Ahn, J.H. Shin, S.C. Hong, T. Kim, J.Y. Hur, Y.T. Kim, K.W. Lee, S.H. Kim, Thyroid stimulating hormone is associated with metabolic syndrome in euthyroid postmenopausal women. Maturitas 62, 301–305 (2009)
A. Giandalia, G.T. Russo, E.L. Romeo, A. Alibrandi, P. Villari, A.A. Mirto, G. Armentano, S. Benvenga, D. Cucinotta, Influence of high-normal serum TSH levels on major cardiovascular risk factors and Visceral Adiposity Index in euthyroid type 2 diabetic subjects. Endocrine 47, 152–160 (2014)
Y. Zhang, P. Lu, L. Zhang, X. Xiao, Association between lipids profile and thyroid parameters in euthyroid diabetic subjects: a cross-sectional study. BMC Endocr. Disord. 15, 12 (2015)
V. Velkoska Nakova, B. Krstevska, M. Bosevski, Ch. Dimitrovski, V. Serafimoski, Dyslipidaemia and hypertension in patients with subclinical hypothyroidism. Prilozi 30, 93–102 (2009).
L. Petrosyan, Relationship between high normal TSH levels and metabolic syndrome components in type 2 diabetic subjects with euthyroidism. J. Clin. Transl. Endocrinol. 2, 110–113 (2015)
W.X. Jian, J. Jin, L. Qin, W.J. Fang, X.R. Chen, H.B. Chen, Q. Su, H.L. Xing, Relationship between thyroid-stimulating hormone and blood pressure in the middle-aged and elderly population. Singap. Med. J. 54, 401–405 (2013)
D. Liu, F. Jiang, Z. Shan, B. Wang, J. Wang, Y. Lai, Y. Chen, M. Li, H. Liu, C. Li, H. Xue, N. Li, J. Yu, L. Shi, X. Bai, X. Hou, L. Zhu, L. Lu, S. Wang, Q. Xing, W. Teng, A cross-sectional survey of relationship between serum TSH level and blood pressure. J. Hum. Hypertens. 24, 134–138 (2010)
R. Luboshitzky, A. Aviv, P. Herer, L. Lavie, Risk factors for cardiovascular disease in women with subclinical hypothyroidism. Thyroid 12, 421–425 (2002)
Y. Duan, W. Peng, X. Wang, W. Tang, X. Liu, S. Xu, X. Mao, S. Feng, Y. Feng, Y. Qin, K. Xu, C. Liu, C. Liu, Community-based study of the association of subclinical thyroid dysfunction with blood pressure. Endocrine 35, 136–142 (2009)
T. Ittermann, D. Tiller, C. Meisinger, C. Agger, M. Nauck, R. Rettig, A. Hofman, T. Jørgensen, A. Linneberg, J.C. Witteman, O.H. Franco, K.H. Greiser, K. Werdan, A. Döring, A. Kluttig, B.H. Stricker, H. Völzke, High serum thyrotropin levels are associated with current but not with incident hypertension. Thyroid 23, 955–963 (2013)
V.L. Langén, T.J. Niiranen, P. Puukka, J. Sundvall, A.M. Jula, V.L. Langén, T.J. Niiranen, P. Puukka, J. Sundvall, A.M. Jula, Association between thyroid-stimulating hormone and blood pressure in adults: an 11-year longitudinal study. Clin. Endocrinol. 84, 741–747 (2016)
A.E. Hak, H.A. Pols, T.J. Visser, H.A. Drexhage, A. Hofman, J.C. Witteman, Subclinical hypothyroidism is an independent risk factor for atherosclerosis and myocardial infarction in elderly women: the Rotterdam Study. Ann. Intern. Med. 132, 270–278 (2000)
M. Imaizumi, M. Akahoshi, S. Ichimaru, E. Nakashima, A. Hida, M. Soda, T. Usa, K. Ashizawa, N. Yokoyama, R. Maeda, S. Nagataki, K. Eguchi, Risk for ischemic heart disease and all-cause mortality in subclinical hypothyroidism. J. Clin. Endorinol. Metab. 89, 3365–3370 (2004)
N. Rodondi, W.P. den Elzen, D.C. Bauer, A.R. Cappola, S. Razvi, J.P. Walsh, B.O. Asvold, G. Iervasi, M. Imaizumi, T.H. Collet, A. Bremner, P. Maisonneuve, J.A. Sgarbi, K.T. Khaw, M.P. Vanderpump, A.B. Newman, J. Cornuz, J.A. Franklyn, R.G. Westendorp, E. Vittinghoff, J. Gussekloo, Thyroid Studies Collaboration. Subclinical hypothyroidism and the risk of coronary heart disease and mortality. JAMA 304, 1365–1374 (2010)
A. Hassan, A. Altamirano-Ufion, B. Zulfiqar, P. Boddu, Subclinical hypothyroidism and its association with increased cardiovascular mortality: call for action. Cardiol. Res. 8, 31–35 (2017)
Y. Ning, Y.J. Cheng, L.J. Liu, J.D. Sara, Z.Y. Cao, W.P. Zheng, T.S. Zhang, H.J. Han, Z.Y. Yang, Y. Zhang, F.L. Wang, R.Y. Pan, J.L. Huang, L.L. Wu, M. Zhang, Y.X. Wei, What is the association of hypothyroidism with risks of cardiovascular events and mortality? A meta-analysis of 55 cohort studies involving 1,898,314 participants. BMC Med. 15(1), 21 (2017)
N.M.Y. Journy, M.O. Bernier, M.M. Doody, B.H. Alexander, M.S. Linet, C.M. Kitahara, Hyperthyroidism, hypothyroidism, and cause-specific mortality in a large cohort of women. Thyroid 27, 1001–1010 (2017)
K. Inoue, T. Tsujimoto, J. Saito, T. Sugiyama, Association between serum thyrotropin levels and mortality among euthyroid adults in the United States. Thyroid 26, 1457–1465 (2016)
A. Akirov, H. Gimbel, A. Grossman, T. Shochat, I. Shimon, Elevated TSH in adults treated for hypothyroidism is associated with increased mortality. Eur. J. Endocrinol. 176, 57–66 (2017)
S.M. Grundy, J.I. Cleeman, S.R. Daniels, K.A. Donato, R.H. Eckel, B.A. Franklin, D.J. Gordon, R.M. Krauss, P.J. Savage, S.C. Smith Jr et al.. Diagnosis and management of the metabolic syndrome: an American Heart Association/National Heart, Lung, and Blood Institute Scientific Statement. Circulation 112, 2735–2752 (2005)
S. Genuth, K.G. Alberti, P. Bennett, J. Buse, R. Defronzo, R. Kahn, J. Kitzmiller, W.C. Knowler, H. Lebovitz, A. Lernmark, D. Nathan, J. Palmer, R. Rizza, C. Saudek, J. Shaw, M. Steffes, M. Stern, J. Tuomilehto, P. Zimmet, Expert Committee on the Diagnosis and Classification of Diabetes Mellitus. Follow-up report on the diagnosis of diabetes mellitus. Diabetes Care 26, 3160–3167 (2003)
M. Cellini, M.G. Santaguida, C. Virili, S. Capriello, N. Brusca, L. Gargano, M. Centanni, Hashimoto’s thyroiditis and autoimmune gastritis. Front. Endocrinol. 26(8), 92 (2017).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical appral
All procedures performed in studies involving human participants were in accordance with the ethical standards of our institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Morini, E., Catalano, A., Lasco, A. et al. l-thyroxine malabsorption due to calcium carbonate impairs blood pressure, total cholesterolemia, and fasting glycemia. Endocrine 64, 284–292 (2019). https://doi.org/10.1007/s12020-018-1798-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-018-1798-7