Abstract
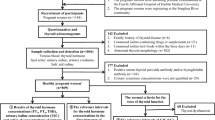
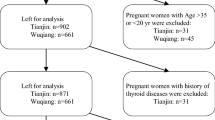
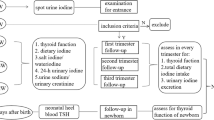
The assessment method of iodine nutrition for pregnant women lacks strong evidence-based medicine. The prevalence of iodine deficiency in pregnant women may be overestimated using urinary iodine concentration (UIC). The reference intervals of UIC-to-urinary creatinine concentration ratio (UIC/UCr) were established using a self-sequential longitudinal study of pregnant women with singleton gestation who were recruited using the criteria of the National Academy of Clinical Biochemistry in Dandong City, which is a long-term iodine-replete area. Nine thousand one hundred sixty-four pregnant women in the first trimester from Dalian City, Dandong City, and Shenyang City were included to verify our proposed reference intervals. UIC and concentrations of urinary creatinine, serum iodine, TSH, FT4, TPOAb, and TgAb were measured. The reference intervals of UIC/UCr were 38.63–489.46 μg/g for the first trimester, 58.48–644.03 μg/g for the second trimester, and 56.27–644.93 μg/g for the third trimester. The prevalence of iodine deficiency was 49.50% using UIC as the indicator (< 150 μg/L), while the prevalence was 3.28% using UIC/UCr (< 38.63 μg/g). The prevalence of iodine excess was 3.21% using UIC as the indicator (> 500 μg/L) while the prevalence was 1.45% using UIC/UCr (> 489.46 μg/g). The highest prevalence of overt hypothyroidism and positive thyroid antibodies was in the group with UIC/UCr < 38.63 μg/g. In contrast to the place of residence and age, BMI was an influencing factor for UIC/UCr. The reference intervals of UIC/UCr were established. UIC/UCr may eliminate the effect of urine volume and reflect the actual prevalence of iodine deficiency in pregnant women.


Similar content being viewed by others
References
Pearce EN, Lazarus JH, Moreno-Reyes R, Zimmermann MB (2016) Consequences of iodine deficiency and excess in pregnant women: an overview of current knowns and unknowns. Am J Clin Nutr 104(Suppl 3):918s–923s. https://doi.org/10.3945/ajcn.115.110429
Xiao Y, Sun H, Li C, Li Y, Peng S, Fan C, Teng W, Shan Z (2018) Effect of iodine nutrition on pregnancy outcomes in an iodine-sufficient area in China. Biol Trace Elem Res 182(2):231–237. https://doi.org/10.1007/s12011-017-1101-4
Sun D, Codling K, Chang S, Zhang S, Shen H, Su X, Chen Z, Scherpbier RW, Yan J (2017) Eliminating iodine deficiency in China: achievements, challenges and global implications. Nutrients 9(4). https://doi.org/10.3390/nu9040361
Zimmermann MB, Andersson M (2012) Update on iodine status worldwide. Curr Opin Endocrinol, Diabetes, Obes 19(5):382–387. https://doi.org/10.1097/MED.0b013e328357271a
Li C, Peng S, Zhang X, Xie X, Wang D, Mao J, Teng X, Shan Z, Teng W (2016) The urine iodine to creatinine as an optimal index of iodine during pregnancy in an iodine adequate area in China. J Clin Endocrinol Metab 101(3):1290–1298. https://doi.org/10.1210/jc.2015-3519
Jahreis G, Hausmann W, Kiessling G, Franke K, Leiterer M (2001) Bioavailability of iodine from normal diets rich in dairy products-results of balance studies in women. Exp Clin Endocrinol Diabetes 109(3):163–167. https://doi.org/10.1055/s-2001-14840
Andersson M, de Benoist B, Delange F, Zupan J (2007) Prevention and control of iodine deficiency in pregnant and lactating women and in children less than 2-years-old: conclusions and recommendations of the Technical Consultation. Public Health Nutr 10(12a):1606–1611. https://doi.org/10.1017/s1368980007361004
Cheung KL, Lafayette RA (2013) Renal physiology of pregnancy. Adv Chronic Kidney Dis 20(3):209–214. https://doi.org/10.1053/j.ackd.2013.01.012
Wang Z, Zhu W, Mo Z, Wang Y, Mao G, Wang X, Lou X (2017) An increase in consuming adequately iodized salt may not be enough to rectify iodine deficiency in pregnancy in an iodine-sufficient area of China. Int J Environ Res Public Health 14(2). https://doi.org/10.3390/ijerph14020206
Shi X, Han C, Li C, Mao J, Wang W, Xie X, Li C, Xu B, Meng T, Du J, Zhang S, Gao Z, Zhang X, Fan C, Shan Z, Teng W (2015) Optimal and safe upper limits of iodine intake for early pregnancy in iodine-sufficient regions: a cross-sectional study of 7190 pregnant women in China. J Clin Endocrinol Metab 100(4):1630–1638. https://doi.org/10.1210/jc.2014-3704
Knudsen N, Christiansen E, Brandt-Christensen M, Nygaard B, Perrild H (2000) Age- and sex-adjusted iodine/creatinine ratio. A new standard in epidemiological surveys? Evaluation of three different estimates of iodine excretion based on casual urine samples and comparison to 24 h values. Eur J Clin Nutr 54(4):361–363. https://doi.org/10.1038/sj.ejcn.1600935
Vejbjerg P, Knudsen N, Perrild H, Laurberg P, Andersen S, Rasmussen LB, Ovesen L, Jorgensen T (2009) Estimation of iodine intake from various urinary iodine measurements in population studies. Thyroid 19(11):1281–1286. https://doi.org/10.1089/thy.2009.0094
CSoPM CSoE (2019) Guideline on diagnosis and management of thyroid diseases during pregnancy and postpartum (2nd edition). Chin J Perinat Med 22(8):505–506. https://doi.org/10.3760/cma.j.issn.1007-9408.2019.08.001
consultation We (2004) Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. Lancet 363(9403):157–163. https://doi.org/10.1016/s0140-6736(03)15268-3
Berghout A, Wiersinga W (1998) Thyroid size and thyroid function during pregnancy: an analysis. Eur J Endocrinol 138(5):536–542. https://doi.org/10.1530/eje.0.1380536
Zimmermann MB (2009) Iodine deficiency. Endocr Rev 30(4):376–408. https://doi.org/10.1210/er.2009-0011
Vermiglio F, Lo Presti VP, Moleti M, Sidoti M, Tortorella G, Scaffidi G, Castagna MG, Mattina F, Violi MA, Crisa A, Artemisia A, Trimarchi F (2004) Attention deficit and hyperactivity disorders in the offspring of mothers exposed to mild-moderate iodine deficiency: a possible novel iodine deficiency disorder in developed countries. J Clin Endocrinol Metab 89(12):6054–6060. https://doi.org/10.1210/jc.2004-0571
de Escobar GM, Obregon MJ, del Rey FE (2007) Iodine deficiency and brain development in the first half of pregnancy. Public Health Nutr 10(12a):1554–1570. https://doi.org/10.1017/s1368980007360928
Angermayr L, Clar C (2018) WITHDRAWN: iodine supplementation for preventing iodine deficiency disorders in children. Cochrane Database Syst Rev 11:Cd003819. https://doi.org/10.1002/14651858.CD003819.pub3
Mills JL, Buck Louis GM, Kannan K, Weck J, Wan Y, Maisog J, Giannakou A, Wu Q, Sundaram R (2018) Delayed conception in women with low-urinary iodine concentrations: a population-based prospective cohort study. Human Reprod (Oxford, England) 33(3):426–433. https://doi.org/10.1093/humrep/dex379
Gao M, Chen W, Sun H, Fan L, Wang W, Du C, Chen Y, Lin L, Pearce EN, Shen J, Cheng Y, Wang C, Zhang W (2019) Excessive iodine intake is associated with formation of thyroid nodules in pregnant Chinese women. Nutr Res (New York, NY) 66:61–67. https://doi.org/10.1016/j.nutres.2019.02.009
Society CN (2016) Chinese residents diet guide 2016. People’s Medical Publishing House
Zhao J, van der Haar F (2004) Progress in salt iodization and improved iodine nutrition in China, 1995--99. Food Nutr Bull 25(4):337–343. https://doi.org/10.1177/156482650402500403
Sun DJ LZ LS (2014) National iodine deficiency disorders surveillance. People's Medical Publishing House
Zhang H, Wu M, Yang L (2019) Evaluation of median urinary iodine concentration cut-off for defining iodine deficiency in pregnant women after a long term USI in China. 16:62. https://doi.org/10.1186/s12986-019-0381-4
Perrine CG, Cogswell ME, Swanson CA, Sullivan KM, Chen TC, Carriquiry AL, Dodd KW, Caldwell KL, Wang CY (2014) Comparison of population iodine estimates from 24-hour urine and timed-spot urine samples. Thyroid 24(4):748–757. https://doi.org/10.1089/thy.2013.0404
Lau CE, Siskos AP, Maitre L, Robinson O, Athersuch TJ, Want EJ, Urquiza J, Casas M, Vafeiadi M, Roumeliotaki T, McEachan RRC, Azad R, Haug LS, Meltzer HM, Andrusaityte S, Petraviciene I, Grazuleviciene R, Thomsen C, Wright J, Slama R, Chatzi L, Vrijheid M, Keun HC, Coen M (2018) Determinants of the urinary and serum metabolome in children from six European populations. BMC Med 16(1):202. https://doi.org/10.1186/s12916-018-1190-8
Wang B, Tang C, Wang H, Zhou W, Chen Y, Zhou Y, Jiang Q (2015) Influence of body mass index status on urinary creatinine and specific gravity for epidemiological study of children. Eur J Pediatr 174(11):1481–1489. https://doi.org/10.1007/s00431-015-2558-9
Acknowledgments
We thank all the physicians of the gynecology and obstetrics clinics from the 13 hospitals and 6 prenatal clinics in Liaoning Province for their contribution. We also thank the residents for participating in this study.
Funding
This work was supported by the 973 Science and Technology Research Foundation, Ministry of Science and Technology, China (Grant no. 2011CB512112); projects of the Liaoning Province University Innovation Team (Grant no. LT2012015); the National Science and Technology Support Program (Grant no. 2014BAI06B00); the Chinese National Natural Science Foundation (Grant no. 81170730); the Liaoning Science Public Research Funds (Grant no. 2014001001/GY2014-A-001); the Research Foundation of the Department of Science and Technology of Liaoning Province Government, China (Grant nos. 2012225020 and 2011225023); and projects of the Key Laboratory of the Endocrine Diseases in Shenyang City (Grant no. F11-244-1-00).
Author information
Authors and Affiliations
Contributions
Jingyi Luo analyzed the data and wrote the paper. Chenyan Li and Xiaomei Zhang collected the samples and data. Zhongyan Shan and Weiping Teng interpreted the results. Weiping Teng contributed to the design of the study.
Corresponding author
Ethics declarations
All the research protocols were approved by the Medical Ethics Committee of China Medical University and were in keeping with the tenets of the Declaration of Helsinki. Informed consent was obtained from every participant before the study was started.
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
ESM 1
(PDF 166 kb)
Rights and permissions
About this article
Cite this article
Luo, J., Li, C., Zhang, X. et al. Reference Intervals of the Ratio of Urine Iodine to Creatinine in Pregnant Women in an Iodine-Replete Area of China. Biol Trace Elem Res 199, 62–69 (2021). https://doi.org/10.1007/s12011-020-02133-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-020-02133-8