Abstract
The COVID-19 pandemic has had a significant impact on global health, with millions of people affected by the disease. Recent studies have shown that environmental factors such as air quality, temperature, and humidity can impact the survival and transmission of the virus, leading to differences in the rate of spread and severity of the disease in different regions. In this global cross-sectional study, we analyzed the relationship between environmental factors and the transmission and survival of the virus in 167 cities distributed all over the world. We used a dataset containing daily COVID-19 data for 167 cities from 01/05/2020 to 01/01/2022, along with variables related to atmospheric and environmental conditions. We found an expected positive relationship between increases in atmospheric NO2 concentration and increases in the infective rate of COVID-19. We also found an unexpected negative relationship between PM10 and COVID-19 spread, which was stronger in unpolluted cities, and indicating a likely stronger and faster deactivation of the viruses by the absorption to the larger than to the smaller particles, to PM10 more than to PM2.5. Although a complete analysis would require taking into account the restrictions in the city and the immunization status of the population, and the variance of COVID-19 spread explained by PM10 was small, only up to approx. 2%, these results contribute to a better understanding of the impact of particles on the spread of COVID-19 and other respiratory viral diseases thus informing public health policies and interventions aimed at mitigating the impact of these pandemics.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The COVID-19 pandemic has had a significant impact on global health, with millions of people affected by the disease. While the initial focus was on identifying the virus and developing effective treatments and vaccines, it is now clear that multiple environmental and social factors play a critical role in the transmission and spread of the disease, leading to differences in the rate of spread and severity of the disease in different cities and regions. Ahmed et al. (2021) found that higher population density is associated with the quick spreading of COVID-19, while GDP (PPP) and PM2.5 are linked with fewer cases. Lim et al. (2021) found that the duration of sunshine and ozone level positively correlate with COVID-19 cases in two regions of the Republic of Korea. Suvvari et al. (2021) reviewed studies related to the environmental effect on COVID-19 and found that atmospheric temperature, ventilation, climate change, and humidity have been studied to understand the effect of these factors on COVID-19 spread. Karim et al. (2022) observed that meteorological factors may show a substantial role in the spread of COVID-19.
Multiple environmental and social factors play a critical role in the transmission and spread of diseases. Research suggests that higher temperatures and humidity levels may reduce the stability of the SARS-CoV-2 virus, potentially leading to decreased transmission rates (He et al. 2021; Morris et al. 2021). Conversely, colder and drier conditions may enhance the virus’s viability and promote its spread (Landier et al. 2021). The impact of temperature and humidity on COVID-19 prevalence can vary across different cities due to variations in weather conditions. Air pollution, including particulate matter (PM2.5 and PM10) and toxic gases, can weaken the respiratory system, making individuals more susceptible to respiratory infections like COVID-19 (Bianconi et al., 2020; Lee et al. 2021). Cities with higher levels of air pollution may experience increased COVID-19 prevalence and severity. The concentration of pollutants in the air can vary significantly between cities due to variations in industrial activities, traffic, and geographical factors (Querol et al. 2008). While significant progress has been made in understanding the potential associations between air pollution, especially nitrogen dioxide (NO2), and particulate matter, and the prevalence and severity of COVID-19 (Zang et al. 2022), there are still several unknowns that require further exploration.
NO2, a common air pollutant, has gained attention due to its potential influence on respiratory health and viral infections (Chauhan et al. 2003). NO2 is primarily released from combustion processes, including vehicle emissions, industrial activities, and power generation (Cuevas et al. 2014). High levels of NO2 have long been associated with adverse respiratory health effects, including increased susceptibility to respiratory infections and exacerbation of respiratory conditions (Huangfu and Atkinson 2020). Prolonged exposure to NO2 can cause airway inflammation, oxidative stress, and compromise lung function, making individuals more vulnerable to respiratory viruses, including SARS-CoV-2, the virus responsible for COVID-19 (Baldasano 2020). NO2 exposure has been shown to disrupt immune system function, particularly the innate immune response, which plays a crucial role in early defense against viral infections. Exposure to NO2 may impair the immune system’s ability to mount an effective defense against SARS-CoV-2, potentially leading to increased transmission rates (Di Ciaula et al. 2022). Furthermore, the COVID-19 pandemic has led to widespread lockdowns and reduced economic activities, resulting in significant reductions in air pollution levels, including NO2. Studies have shown that decreased NO2 levels during lockdown periods are associated with improved air quality (Saha et al. 2022). Cleaner air may thus indirectly reduce the transmission of respiratory infections, including COVID-19, by improving respiratory health and reducing the susceptibility of individuals to viral infections at the same time, indicating better lockdown accomplishment (Ravindra et al. 2022).
Some research has suggested that elevated levels of PM2.5 and PM10 may also contribute to higher COVID-19 prevalence, severity, and mortality rates (Meo et al. 2021). The interaction between air pollution and the virus could potentially exacerbate respiratory symptoms, impair immune responses, and increase susceptibility to respiratory infections. Both PM2.5 and PM10 have been associated with inflammation, oxidative stress, and compromised lung function (Leikauf et al. 2020; Thangavel et al. 2022). These effects could make individuals more vulnerable to SARS-CoV-2. The smaller size of PM2.5 particles allows them to penetrate deeper than PM10 into the respiratory system, potentially reaching the lungs’ sensitive regions and causing more severe respiratory impacts (Marshall, 2013). This characteristic may contribute to a greater association between PM2.5 and COVID-19 severity compared to PM10 (Bourdrel et al. 2021). Further investigations are needed to elucidate the precise mechanisms, establish causality, and identify the specific threshold levels and durations of exposure. Additionally, as in the case of NO2, we could expect a positive correlation between both PM2.5 and PM10 with the transmission rate when the concentration of these particles increases, and there is no effective lockdown. However, particulate matter, specifically PM10 and PM2.5, could also adsorb and inactivate viruses, including SARS-CoV-2 (Wathore et al. 2020). While it is known that certain surfaces can facilitate viral attachment and persistence, the specific interactions between particulate matter and viruses, and their impact on viral inactivation, are still not well understood.
Particulate matter, including PM10 and PM2.5, can act as surfaces for viral particles to attach to (Wathore et al. 2020). The surface properties of these particles, such as their composition and charge, may influence viral adsorption. However, the extent to which particulate matter serves as a viable surface for viral attachment and subsequent inactivation is still uncertain. Some studies suggest that viruses can remain viable on surfaces, including particulate matter, for varying periods, and the conditions required for viral inactivation are complex and can depend on multiple factors. Environmental conditions such as temperature, humidity, and exposure to UV radiation may affect the viability and persistence of viruses on particulate matter surfaces (Kampf et al. 2020).
The inactivation of viruses on particulate matter surfaces might occur due to several factors, including physical processes (e.g., desiccation, degradation), chemical reactions, or interactions with other substances present on the particles (Fernández-Raga et al., 2021; Guo et al. 2021). Furthermore, the time that these particles remain suspended in the air and can be inhaled also plays a key role in the transmission rate. If a particle adsorbs several viruses and falls to the soil, it diminishes the risk of inhaling these viruses. As each individual PM10 particle has more surface area and possibilities of adsorbing viruses and less time of permanence in the air, we can hypothesize that these larger particles may reduce the possibilities of virus transmission even more than PM2.5.
Overall, while there is ongoing research exploring the potential interactions between particulate matter and viruses, including SARS-CoV-2, the ability of PM10 and PM2.5 to adsorb and inactivate viruses is not yet firmly established. It is important to continue studying this topic to gain a more comprehensive understanding of the dynamics between particulate matter and viral inactivation, which can inform public health strategies for mitigating viral spread and transmission. In this study, we aimed to analyse which was the relationship of urban environmental factors listed in the next Materials and methods section including temperature, humidity and air pollution with COVID-19 transmission rates in 167 cities distributed all over the world with the main objective of assessing whether the air pollutants, NO2 and particulate matter, increase or decrease COVID-19 transmission rate.
Materials and methods
Data
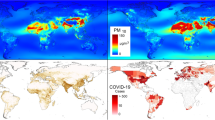
We conducted a global cross-sectional study using city-level data (Table 1, Fig. 1). We gathered a database containing covid data for 167 cities around the world. The dataset contained the daily data of covid for 2 years, from 01/05/2020 to 01/01/2022.
The database contains the following variables:
-
Date: daily data from 01/05/2020 to 01/01/2022.
-
Country: 27 different countries.
-
City: 167 different cities.
-
Location key: Unique identifier code for each city, 167 different locations key.
-
Latitude: Latitude of the city.
-
Longitude: Longitude of the city.
-
Density: Population density of the city.
-
T0_Covidcases: Cases of covid notified the current day.
-
T0_Deaths: Deaths of covid notified the current day.
-
T0_Covidcum: Cumulative cases of covid.
-
T0_Deathscum: Cumulative deaths of covid.
-
Rt: Transmission rate, Cumulative covid case count for the last 7 days/(Cumulative covid case count for the last 14 days - Cumulative covid case count for the last 7 days).
-
T1_CovidIncrease: Rate of increase of covid cases compared to yesterday’s covid cases.
-
T7_CovidIncrease: Rate of increase of covid cases compared to the number of cases 7 days ago.
-
T14_CovidIncrease: Rate of increase of covid cases compared to the number of cases 14 days ago.
-
PM10: Atmospheric particulate matter with a diameter less than 10 μm and more than 2.5 μm in EU EPA standard units.
-
Humidity: Concentration of humidity in %.
-
O3: Measurement of the concentration of O3 in EU EPA standard units.
-
Wind Measurement of wind speed in km/h.
-
PM25: Measurement of the atmospheric particulate matter with a diameter less than 2.5 μm in EU EPA standard units.
-
NO2: Measurement of the concentration of NO2 in EU EPA standard units.
-
Pressure: Measurement of the pressure in hPa.
-
Temp: Measurement of the temperature in ºC.
-
Precipitation: Measurement of the precipitation in mm.
-
CO: Measurement of the concentration of CO in EU EPA standard units.
For the variables PM10, Humidity, O3, Wind_speed, PM2.5, NO2, Pressure, Temp, Precipitation and C0 we had 6 measures:
-
T0_var is the median value of the variable measured during the current day.
-
T1_var is the average of the median variable measure of the current day and the previous day.
-
T3_var is the average of the median measurement of the variable of the current day and 3 previous days.
-
T7_var is the average of the median measurement of the variable of the current day and 7 previous days.
-
T14_var is the average of the median variable measurement of the current day and 14 previous days.
-
T30_var is the average of the median variable measurement of the current day and 30 previous days.
The covid data was extracted from JHU CSSE COVID-19 Data (https://github.com/CSSEGISandData/COVID-19/tree/master/csse_covid_19_data#daily-reports-csse_covid_19_daily_reports) and the variables of environmental and atmospheric conditions were extracted from World’s Air Pollution website (https://waqi.info/#/c/2.6/0/2z).
Initially we had a total of 112,929 records in a database from 01/01/2020 to 01/01/2022.
We then selected a final database after considering several consistency and integrity checks:
-
Data only from 1/05/2020 on since this was the date when data started to be collected in a more rigorous way.
-
Eliminate those locations that had data recorded less than 200 days.
-
Eliminate records with more than 50 missing values per row in pollution or climate variables.
-
Delete extreme weather data, transmission and increase rates.
-
Delete records that have negative daily covid cases.
Once we had taken into account these considerations, we did multiple imputation of the data using an EM (Expectation-maximization) algorithm in two steps:
-
Expectation step (step E): In this expectation step, using the observed available data from the dataset, we tried to estimate the missing data values.
-
Maximization step (step M): We used the now complete data prepared in the expectation step to update the parameters.
The final database had 69,200 records, 38.72% less than the initial number of records.
Statistical methods
We employed linear mixed-effects models to explore the association between environmental variables and the transmission rate (Rt) of COVID-19, while considering potential sources of error associated with different countries and cities (i.e., nested random factors, city within country). A total of seven models with increasing complexity were fitted to assess the significance of the predictors on the response variable (i.e., the natural logarithm of Rt multiplied by 100). The simplest models tested the effects of the average of median city air concentrations of NO2, PM2.5 and PM10 and their respective interactions with their anomalies (i.e., deviations from their mean; models M1, M2 and M3). We then fitted two models (M4 and M5) combining the effects of NO2 and PM2.5, and NO2 and PM10 while also including their respective interaction with their anomalies. Finally, we fitted two more models (M5 and M6) resembling M4 and M6 but also including air concentrations O3, air humidity and temperature and their respective anomalies. These predictors encompassed the average of median city air concentrations of PM2.5, PM10, O3, NO2, humidity, and temperature, as well as their anomalies (deviations from the mean) in the 14 days preceding the current Rt observations. Interactions between the averages and anomalies of the same variables (e.g., PM2.5 × anomaly PM2.5) were fitted to examine whether the anomalies exhibited distinct effects on Rt depending on the average values of the corresponding variable.
Notably, all models were repeated using PM10 instead of PM2.5, consistently showing lower Bayesian Information Criterion (BIC) values when utilizing PM10. To fit these models, the “lme” function from the “nlme” package in R (Pinehiro et al. 2018) was employed. A temporal correlation structure of order one (AR1) was implemented by specifying the argument “correlation = corAR1()”. This temporal autocorrelation structure allowed for observations at time t to be affected by previous observations (time t-1). Maximum likelihood estimation was used for model fitting. The BIC was computed using the “BIC” function to identify the best-performing model among the nine candidate models. Response curves were generated using the “visreg” package in R (6. Breheny et al. 2017). All statistical analyses were conducted using R statistical software version 4.1.1 (R Core Team 2021).
Results and discussion
Our study found a positive relationship of the transmission rate of COVID-19 with NO2concentration. This finding is consistent with previous research that has shown NO2 to be an agent that directly damages the respiratory system, especially in vulnerable populations such as children (Ghanbari Ghozikali et al. 2016; Pfeffer et al. 2019; Bahrami Asl 2018; Chen et al. 2019; Kowalskaet al. 2020; To et al. 2020). Additionally, exposure to NO2 has long been associated with an increased likelihood of contracting viral infections (Zhu et al. 2020). But more than that, NO2 is significantly related to human activity and mobility, so to higher probability of COVID-19 spread due to increased human contact. The direct effect of NO2 causing injury to human health can facilitate the expansion and damage caused by COVID-19, while infected people with stronger COVID infections can be a more powerful source of contamination to others, increasing the probability of transmission.
Importantly, these results also show the effective role of lockdown during the COVID outbreak (Wang and Penuelas 2021; Xing et al. 2021). Recent studies have shown that lockdowns in 2019 and 2020 established to fight COVID-19 reduced atmospheric NO2 concentrations in 65 studied cities around the world Cooper et al. 2022). They also confirm the initial observations that linked ambient concentrations of NO2 to the spread of the COVID-19 pandemic across Europe, China, and the United States (Zhu et al. 2020; Bashir et al. 2020; Fattorini and Regoli 2020; Jiang et al. 2020; Li et al. 2020; Ogen 2020; Zoren et al. 2022a), and differ from the very few that like those of Zoran et al. (2020a); Bashir et al. (2020) report either no association or a negative one between NO2 and daily death counts. In China, Zhu et al. (2020), observed that a 10-µg/m3 increase in NO2 is associated with a 6.94% (95% CI: 2.38–11.51) increase in the daily counts of COVID-19 confirmed cases in 120 cities. These findings are consistent with those of Jiang et al. (2020) and Li et al. (2020), who used the same method described for PM. Jiang et al. (2020) found a significant positive association between NO2 and COVID-19 in Wuhan and XiaoGan (Wuhan RR = 1.056, CI:1.053–1.059; XiaoGan RR = 1.115, CI = 1.095–1.136), but not in Li et al. (2020) found a significant linear correlation in Wuhan (R2 = 0.329, p < 0.001) and XiaoGan (R2 = 0.158, p < 0.05). Taking into account this scientific evidence, it can be stated that exposure to NO2 not only harms human health and increases the risk of respiratory diseases, but it is also an indicator of human activity driving to human connectivity that triggers the spread of COVID-19.
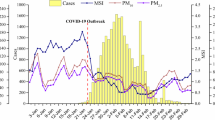
Surprisingly, our findings reveal a negative correlation between PM10 levels and the spread of COVID (Fig. 2). This negative correlation is even more pronounced in less polluted cities. Unlike the relationships observed with NO2, these results are not consistent with previous reports and the expected effects of lockdown, which would decrease both transmission and pollution linked to human activity. Although there are a few studies that have not found evidence linking PM10 particles to the spread of COVID-19 (Bontempi 2020), most studies have reported a significant association between ambient concentrations of PM10 and the COVID-19 pandemic in the most affected countries, including China, Italy, and the United States (Zhu et al. 2020; Bashir et al. 2020; Coccia 2020; Fattorini and Regoli 2023; Yao et al. 2020; Zoran et al. 2020b). For example, Wannaz et al. (2021) studied the relationships between the presence of PM2.5 and PM10 particles in the low atmosphere and the spread of COVID-19 in the city of Arequipa, Peru. They observed a significant correlation between day concentrations of PM10 particles and the number of new COVID-19 cases registered in the next 18 days, particularly after 15–18 days. The authors hypothesized that the COVID-19 virus might circulate attached to coarse particle PM10, acting as a vector of infection. However, the study also observed that the decrease in PM10 was mainly observed on Sundays, coinciding with a radical drop in human activity, mobility, and direct transmission facilities. Thus, it cannot be ruled out that the positive relationship between PM10 and COVID-19 spread they found could simply be also an indicator of increased human activity as it is the case for NO2. Moreover, some studies have observed that in general PM directly induces inflammation in lung cells and thus can increase the susceptibility and severity of the COVID-10 in humans (Comunian et al. 2020).
Instead, our finding of a negative relationship might indicate a lower suspension time of PM10 particles in the air than that of viral particles. In fact, the SARS-CoV-2 virus, responsible for COVID-19, has a diameter of approximately 60–140 nm whereas the diameter of PM10 particles ranges from 2.5 to 10 micrometers. The adsorption of viral particles would favour a lower permanence of the virus in the air. The contrary pattern, i.e. the possibility that PM particles might promote a longer permanence of viral particles in the atmosphere has been hypothesized to explain reported positive relationships (Anugerah et al. 2021). Meo et al. (2021), analyzing a global database reporting data from December 2019 to September 30, 2021, concluded that there is a possible causal link between increasing particulate matter PM2.5 and PM10 in the atmosphere and increasing incidence and mortality of COVID-19. However, several studies have observed that the suspension time of PM particles in the air, prior deposition, and the possibility of resuspension strongly depend on several variables, such as climate, human activities, sources of emission, and the particle material (Kauhaniemi et al. 2011; Kupainen et al. 2016; Tohidi et al. 2022; Zhang et al. 2022).
Several studies that have observed direct relationships between proxies indicating more human mobility and human contacts with PM concentrations in the lower atmosphere by comparing lockdown versus non-lockdown periods and/or under different levels of human/traffic/industrial activity (Setti et al. 2020; Tung et al. 2021; Choi and Kim 2022; Gorrochategui et al. 2022; Pala et al. 2022). Nonetheless, these relationships are not very clear or significant because the source of PM particles is not only the urban (traffic, industrial) origin. Other factors related to climate, such as wind, precipitation, or atmospheric pressure can also play a role that can distort the direct relationships between lockdown and PM concentrations (Bera et al. 2022; Gilardi et al. 2022). Furthermore, little information is available about the virus’s suspension capacity by itself and its absorption to particles of PM10, which may increase or decrease the mean time of air suspension of COVID-19 virus. It is not clear whether the COVID virus remains suspended in the air longer by itself or when attached to a PM10 particle, although it seems that when attached, it is able to travel greater distances, as observed in road dust (Alex et al., 2023). There is indirect evidence suggesting that high concentrations of air pollutants, associated with low wind speeds, may promote a longer permanence of viral particles in the polluted air of cities (Coccia, 2020). However, it is not clear either, and it would be essential to know if the attachment/absorption of viral particles on PM10 deactivates the virulence of the virus and how this depends on environmental conditions such as sunlight or temperature levels, and the specific material of each PM10 (coal, organic matter, silicates, clays, lime, etc.). Our results could be due to the viral particle adsorption on PM reducing COVID infectivity by mechanisms related to molecular alterations that limit the virus’ ability to interact with human cells and penetrate them (Woodby et al. 2021). Furthermore, sunlight and photochemical reactions on PM with absorbed virus could trigger heating and/or deactivate the virus’s virulence capacity, as hypothesized by some authors (Edge and Truscott 2021). The viability and virulence of COVID-19 virus stuck on the particulate surface are not yet confirmed (Srivastava 2021) and surely depend on the particle material. Thus, although the structural/compositional changes of virus capsid when absorbed on a PM10 particle and their impacts on virus virulence level remain to be fully understood, our results are compatible with a reduced infectivity of COVID-19 by viral absorption on PM10.
In this regard, certain studies have observed that SARS-CoV-2 virus absorbed on PM10 particles from different fuels combustion deactivates the virus, thus reducing transmission. However, this positive effect is counterbalanced by the negative impact of these particles on host oxidative stress and immunity (de la Fuente et al. 2022). Effectively, PM10 pollution can have more health effects by itself: lowering the body’s immune system and making people more susceptible to infection, resulting in a potential increase in the spread rate. But on the other side, PM10 pollution can also decrease the rate of spread of infections, possibly due to behavioral changes in response to air pollution levels. When pollution is high, and thus the presence of PM10 is also high, the protective measures such as reducing outdoor activities are higher, reducing the spread rate. Conversely, when pollution is low, people may leave protective measures, increasing outdoor activities and taking more contact with PM10 particles.
We can conclude that most studies, including the present one, demonstrate non-neutral interactions between PM2.5 and primarily PM10 particles and the spread of viruses, particularly in areas with high population density and significant pollution levels. The effects of PM particles on COVID spread can vary depending on the chemical composition of the particles and the specific environmental and climatic conditions of the location. These factors determine the duration of particle persistence in the atmosphere and the likelihood of resuspension as well as deactivation potential. It is important to consider these local conditions when assessing the positive or negative impacts of PM particles on the transmission of viruses like COVID-19. Although a complete analysis would require taking into account the restrictions in the city and the immunization status of the population, and although our models explain small part of the variance, up to approximately 2%, these results will contribute to a better understanding of the environmental factors that impact the spread of COVID-19 thus informing public health policies and interventions aimed at mitigating the impact of these pandemics, particularly in regions that are vulnerable to the effects of environmental factors.
Data availability
Available on request.
References
Ahmed J, Jaman MH, Saha G, Ghosh P (2021) Effect of environmental and socio-economic factors on the spreading of COVID-19 at 70 cities/provinces. Heliyon 7:e06979. https://doi.org/10.1016/j.heliyon.2021.e06979
Alex FJ, Tan G, Kyei SK, et al 2023 Transmission of viruses and other pathogenic microorganisms via road dust: emissions, characterization, health risks, and mitigation measures. Atmos Pollut Res, 14(1).
Anugerah AR, Muttaqin PS, Purnama DA (2021) Effect of large-scale social restriction (PSBB) during COVID-19 on outdoor air quality: evidence from five cities in DKI Jakarta Province, Indonesia. Environ Res 197:11164. https://doi.org/10.1016/j.envres.2021.111164
Bahrami Asl F, Leili M, Vaziri Y, Salahshour Arian S, Cristaldi A, Conti O, G., et al (2018) Health impacts quantification of ambient air pollutants using AirQ model approach in Hamadan, Iran. Environ Res 161:114–121. https://doi.org/10.1016/j.envres.2017.10.050
Baldasano JM (2020) COVID-19 lockdown effects on air quality by NO2 in the cities of Baecelona and Madrid (Spain). Sci Total Environ 741:140353
Bashir MF, Ma BJ, Bilal Komal B, Bashir MA, Farooq TH, Iqbal N et al (2020) Correlation between environmental pollution indicators and COVID-19 pandemic: a brief study in Californian context. Environ Res 187:109652. https://doi.org/10.1016/j.envres.2020.109652
Bera B, Bhattacharjee S, Sengupta N, Saha S (2022) Variation and dispersa lof PM10 and PM2.5 during COVID-19 lockdown over Kolkata metropolitan city, India investigated throught HYSPLIT model. Geosci Frontieres 13:1011291. https://doi.org/10.1016/j.gsf.2021.101291
Bianconi V, Bronzo P, Banach M, Sahebkar A, Mannarino MR, Pirro M (2020) Particulate matter pollution and the COVID-19 outbreak: results from Italian regions and provinces. Arch Med Sci 16:985–992
Bontempi E (2020) First data analysis about possible COVID-19 virus airborne diffusion due to air particulate matter (PM): the case of Lombardy (Italy). Environ Res 186:109639. https://doi.org/10.1016/j.envres.2020.109639
Bourdrel T, Annesi-Maesano I, Alahmad B, Maesano BA, Bind MA (2021) The impact of outdoor air pollution on COVID-19: a review of evidence from in vitro, animal, and human studies. Eur Respir Rev 30:200242
Breheny P, Burchett W (2017) Visualization of regression models using visreg. - R J 9:56–71. https://journal.r-project.org/archive/2017/RJ-2017-046/RJ-2017-046/
Chauhan AJ, Inskip HM, Linaker CH, Smith S, Schreiber J, Johnston SL et al (2003) Personal exposure to nitrogen dioxide (NO2) and the severity of virus-induced asthma in children. Lancet 361:1939–1944
Chen J, Zeng J, Shi C, Liu R, Lu R, Mao S et al (2019) Associations between short-term exposure to gaseous pollutants and pulmonary heart disease-related mortality among elderly people in Chengdu, China. Environ Health 18:64. https://doi.org/10.1186/s12940-019-0500-8
Choi W, Kim KY (2022) Correlation between COVID-19 infection rate and atmospheric environmental factors in Seoul Metropolitan City, South Korea. https://doi.org/10.21203/rs.3.rs-1383594/v2. Research Square
Coccia M (2020) Factors determining the diffusion of COVID-19 and suggested strategy to prevent future accelerated viral infectivity similar to COVID. Sci Total Environ 10:729: 138474. https://doi.org/10.1016/j.scitotenv.2020.138474
Comunian S, Dongo D, Milani C, Palestini P (2020) Air pollution and COVID-19: the role of particulate matter and increase of COVID-19s morbidity and mostality. Int J Environ Res Public Health 17:4487. https://doi.org/10.3390/ijerph17124487
Cooper MJ, Martin RV, Hammer MS, Levelt PF, Veefkind P, Lamsat LN et al (2022) Global fine-scale changes in ambient NO2 during COVID-19 lockdowns. Nature 601:380–387. https://doi.org/10.1038/s41586-021-04229-0
R Core Team (2021) R: A Language and Environment for Statistical Computing. Version 4.1.1. https://www.R-project.org
Cuevas CA, Notario A, Adame JA, Hilboli A, Richter A, Burrows JP et al (2014) Evolution of NO2 levels in Spain from 1996 to 2012. Sci Rep 4:5887
De la Fuente J, Armas O, Barroso-Arévalo S, Gortázar C, García-Seco T, Buendia-Andrés et al (2022) Good and bad get together: inactivation of SARS-CoV-2 in particulate metter pollution from different fuels. Sci Total Environ 844:157241
Di Ciaula A, Bonfrate L, Portincasa P, Appice C, Belfiore A, Binetti M et al (2022) Nitrogen dioxide pollution increases vulnerability to COVID-19 through altered immune function. Environ Sci Pollut Res Int 29:44404–44412
Edge R, Truscott (2021) COVID-19 and the ethhicity link – is there a photochemical link? Photochemical Photobiological Sci 20:183–188. https://doi.org/10.1007/s43630-020-00004-8
Fattorini D, Regoli F (2020) Role of the chronic air pollution levels in the Covid-19 outbreak risk in Italy. Environ Pollut Barking Essex 264:114732. https://doi.org/10.1016/j.envpol.2020.114732
Fattorini D, Regoli F (2023) Role of the chronic air pollution levels in the Covid-19 outbreak risk in Italy. Environ Pollut 264:114732. https://doi.org/10.1016/j.envpol.2020.114732
Fernandez-Raga M, Díaz-Marugán L, García Escolano M, Bort C, Fanjul V (2021) SARS-CoV-2 viability under different metereological conditions, surfaces, fluids and transmission between animals. Environ Res 192:110293
Ghanbari Ghozikali M, Heibati B, Naddafi K, Kloog I, Oliveri Conti G, Polosa R et al (2016) Evaluation of chronic obstructive pulmonary disease (COPD) attributed to atmospheric O3, NO2, and SO2 using air Q model (2011–2012 year). Environ Res 144:99–105. https://doi.org/10.1016/j.envres.2015.10.030
GiIardi F, Nava S, Calzolai G, Pazzi G, Chiari M, Faggi A et al (2022) PM10 variation, composition, and source analyses in Tuscany (Italy) following the COVID-19 lockdown restrictions. Atmospheric Chem Ohysics 22:9987–10005. https://doi.org/10.5194/acp-22-9987-2022
Gorrochategui E, Hernandez I, Pérez-Gabucio E, Lacorte S, Tauler R (2022) Temporal air quality (NO2, O3, and PM10) changes in urban and rural stations in Catalonia during COVID-10 lockdown: an association with human mobility and satellite data. Environ Sci Pollut Res 29:18905–18922. https://doi.org/10.1007/s11356-021-17137-7
Guo L, Yang Z, Zhang L, Wang S, Bai T, Xiang Y et al (2021) Systematic review of the effects of environmental factors on virus inactivation: implications for coronavirus disease 2019. Int J Environ Sci Technol 18:2865–2878
He Z, Chin Y, Yu S, Huang J, Zhang CJP, Zhu K et al (2021) The influence of average temperature and relative humidity on new cases of COVID-19: time-series analyses. JMIR Public Health Surveillance 7:e20495
Huangfu P, Atkinson R (2020) Long-term exposure to NO2 and O3 and all-cause and respiratory mortality. A systematic review and meta-analysis. Environ Int 144:105998
Jiang Y, Wu X-J, Guan Y-J (2020) Effect of ambient air pollutants and meteorological variables on COVID-19 incidence. Infect Control Hosp Epidemiol 1–11. https://doi.org/10.1017/ice.2020.222
Kampf G, Todt D, Pfaender S, Steinmann E (2020) Persistence of coronaviruses on inanimate surfaces and their inactivation with biocidal agents. J Hosp Infect 104:246–251
Karim MR, Akter MB, Haque S, Akter N (2022) Do Temperature and Humidity Affect the Transmission of SARS-CoV-2?-A Flexible Regression Analysis, Annals of Data Science, Springer, vol. 9(1), 153–173. https://doi.org/10.1007/s40745-021-00351-y
Kauhaniemi M, Kukkonen J, Härkönen J, Nikmo J, Kangas L, Omstedt G et al (2011) Evaluation of road dust suspension model for the prediction of PM10 in a Street canyon. Atmos Environ 45:3646–3654. https://doi.org/10.1016/j.atmosenv.2011.04.05
Kowalska M, Skrzypek M, Kowalski M, Cyrys J (2020) Effect of NOx and NO2 concentration increase in ambient air to daily bronchitis and asthma exacerbation, silesian voivodeship in Poland. Int J Environ Res Publ Health 17(3):754. https://doi.org/10.3390/ijerph17030754
Kupainen K, Ritola R, Stojilijkovic A, Pirjola L, Malinen A, Niemi J (2016) Contribution of mineral dust sources to Street side ambient and suspensión PM10 samples. Atmos Environ 147:178–189. https://doi.org/10.1016/j.atmosenv.2016.09.059
Landier J, Paireau J, Rebauet S, Legendre E, Lehot L, Fontanet A et al (2021) Cold and dry winter conditions are associated with greater SARS-CoV-2 transmission at regional level in western countries during the first epidemic wave. Sci Rep 11:12756
Lee YG, Lee PH, Choi SM, An MH, Jang AS (2021) Effects of air pollutants on airway diseases. Int J Environ Res Public Health 18:9905
Leikauf G, Kim SH, Jang AS (2020) Mechanisms of ultrafine particle-induced respiratory health effects. Exp Mol Med 52:329–337
Li H, Xu X-L, Dai D-W, Huang Z-Y, Ma Z, Guan Y-J (2020) Air pollution and temperature are associated with increased COVID-19 incidence: a time series study. Int J Infect Dis IJID off Publ Int Soc Infect Dis 97:278–282. https://doi.org/10.1016/j.ijid.2020.05.076
Lim YK, Kweon OJ, Kim HR, Kim TH, Lee MK (2021) The impact of environmental variables on the spread of COVID-19 in the Republic of Korea. Sci Rep 11:5977. https://doi.org/10.1038/s41598-021-85493-y
Marshall J (2013) PM 2.5. PNAS 110:8756
Meo SA, Al-khlaiwi T, Ullah CH (2021) Effect of ambient air pollutants PM2.5 and PM10 on COVID-19 incidence and mortality: observational study. Eur Reviews Med Pharmacol Sci 25:7553–7564. https://doi.org/10.26355/eurrev_202112_27455
Morris DH, Yinda KC, Gamble A, Rossine FW, Huang Q, Bushmaker T et al (2021) Mechanistic theory predicts the effects of temperature and humidity on inactivation of SARS-CoV-2 and other enveloped viruses. eLife 10:e65902
Ogen Y (2020) Assessing nitrogen dioxide (NO2) levels as a contributing factor to coronavirus (COVID-19) fatality. Sci Total Environ 726:138605. https://doi.org/10.1016/j.scitotenv.2020.138605
Pala D, Casella V, Larizza C, Malovini A, Bellazzi R (2022) Impact of COVID-10 lockdown on PM concentrations in an Italian Northern City: a year-by-year assessment. PlosOne 17:e0263265. https://doi.org/10.1371/journal.pone.0263265
Pfeffer PE, Donaldson GC, Mackay AJ, Wedzicha JA (2019) Increased chronic obstructive pulmonary disease exacerbations of likely viral etiology follow elevated ambient nitrogen oxides. Am J Respir Crit Care Med 199:581–591. https://doi.org/10.1164/rccm.201712-2506OC
Pinheiro J, Bates D, DebRoy S, Sarkar D, authors EISPACK, Heisterkamp S et al (2018) nlme: linear and nonlinear mixed effects models.-R package ver. 3.1–137. https://cran.r-project.org/web/packages/nlme/nlme.pdf
Querol X, Alastuey A, Moreno T, Viana MM, Castillo S, Pey J et al (2008) Spatial and temporal variations in airborne particulate matter (PM10 and PM2.5) across Spain 1999–2005. Atm Environ 42:3964–3979
Ravindra K, Singh T, Vardhan S, Shrivastrava A, Singh S, Kumar P, Mor S (2022) COVID-19 pandemic: what can we learn for better air quality and human. Health? Health 15:187–198
Saha L, Kumar A, Kumr S, Korstaf J, Srivastava S, Bauddh K (2022) The impact of the COVID-19 lockdown on global air quality: a review. Environ Sust 5:5–23
Setti L, Passarini F, De Gennaro G, Barbieri P, Pallavicini A, Ruscio M et al (2020) Searching for SARS-COV-2 on particulate matter: a possible early indicator of COVID-19 epidemic recurrence. Int J Environ Res Publ Health 17(9):2986. https://doi.org/10.3390/ijerph17092986
Srivastava A (2021) COVID-19 and air pollution and meteorology-an intrincate relationship: a review. Chemosphere 263:128297. https://doi.org/10.1016/j.chemosphere.2020.128297
Suvvari TK, Kutikuppala LV, Jonna S, Kashif MS (2021) Impact of environmental factors on COVID-19 pandemic: a narrative review. MGM J Med Sci 8:151–154. https://doi.org/10.4103/mgmj.mgmj_10_21
Thangavel P, Park D, Lee YC (2022) Recent insights into particulate matter (PM2.5)-mediated toxicity in humans: an overview. Int J Environ l Res Public Health 1:7511
To T, Zhu J, Stieb D, Gray N, Fong I, Pinault L et al (2020) Early life exposure to air pollution and incidence of childhood asthma, allergic rhinitis and eczema. Eur Respir J 55. https://doi.org/10.1183/13993003.00913-2019
Tohidi R, Farahani VJ, Sioutas C (2022) Real-time measurements of mineral dust concentration in coarse particulate matter (PM10-2.5) by emplying a novel optical-based technique in Los Angeles. Sci Total Environ 838:156215. https://doi.org/10.1016/j.scitotenv.2022.156215
Tung NT, Cheng PC, Chi KH, Hsiao TC, Jones T, Bérube K et al (2021) Particulate matter and SARD-CoV-2: a posible modelo f COVID-19 transmission. Sci Total Environ 750:141532. https://doi.org/10.1016/j.scitotenv.2020.141532
Wang R, Penuelas J (2021) Monitoring compliance in pandemic management with air pollution data: a lesson from COVID-19. Environ Sci Technol 55(20):13571–13574. https://doi.org/10.1021/acs.est.1c03818
Wannaz ED, Valdivia AEL, Reyes Larico JA, Salcedo Peña J, Valenzuela Huillca C (2021) PM10 correlates with COVID-19 infections 15 days later in Arequipa Perú. Environ Sci Pollut Res 28:39648–39654. https://doi.org/10.1007/s11356-021-13408-5
Wathore R, Gupta A, Bherwani H, Labhasetwar N (2020) Understanding air and water borne transmission and survival of coronavirus: insights and way forward for SARS.CoV-2. Sci Total Environ 749:141486
Woodby B, Arnold MM, Valacchi G (2021) SARS-CoV-2 infection, COVID-19 pathogenesis, and exposure to air pollution: what, vol 1486. is the connection? Annals of New York Academy of Sciences, pp 15–38
Xing X, Xiong Y, Yang R, Wang R, Wang W, Kan H et al (2021) Predicting the effect of confinement on the COVID-19 spread using machine learning enriched with satellite air pollution observations. Proc Natl Acad Sci 118(33):e2109098118. https://doi.org/10.1073/pnas.2109098118
Yao Y, Pan J, Wang W, Liu Z, Kan H, Qiu Y, et (2020) Association of particulate matter pollution and case fatality rate of COVID-19 in 49 Chinese cities. Sci Total Environ 741:140396. https://doi.org/10.1016/j.scitotenv.2020.140396
Zang ST, Luan J, Li L, Yu HX, Wu QJ, Chang Q, Zhao YH (2022) Ambient air pollution and COVID-19 risk: evidence from 35 observational studies. Environ Res 204:112065
Zhang D, Li H, Luo XS, Huang W, Pang Y, Yang J et al (2022) Toxicity assessment and heavy metal components of inhalable particulate matters (PM2.5& PM10) during a dust storm invading the city. Process Saf Environ Prot 162:859–866. https://doi.org/10.1016/j.psep.2022.04.065
Zhu Y, Xie J, Huang F, Cao L (2020) Association between short-term exposure to air pollution and COVID-19 infection: evidence from China. Sci Total Environ 2020(727):138704. https://doi.org/10.1016/j.scitotenv.2020.138704
Zoran MA, Savastru RS, Savastru DN, Tautan MN (2020b) Assessing the relationships between ground levels of ozone (O3) and nitrogen dioxide (NO2) with coronavirus (COVID-19) in Milan, Italy. Sci Total Environ 740:140005
Zoran MA, Savastru RS, Savastru DM, Tautan MN (2022a) Cumulative effects of air pollution and climate drivers on COVID-19 multiwaves in Bucarest, Romania. Process effects of air pollution and climate drivers on COVID-19 multiwaves in Bucharest, Romania
Funding
Open Access funding provided thanks to the CRUE-CSIC agreement with Springer Nature. This research was funded by the Catalan government grant AGAUR-2020PANDE00117.
Open Access funding provided thanks to the CRUE-CSIC agreement with Springer Nature.
Author information
Authors and Affiliations
Contributions
JP designed the research. SC gathered the data. MF, SC, LLB, JS and JP conducted the statistical analyses. JP and JS drafted the manuscript. All authors discussed the results and the implications, revised the manuscript, provided key guidance, and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
None.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Penuelas, J., Fernández-Martínez, M., Cobo, S. et al. Does urban particulate matter hinder COVID-19 transmission rate?. Air Qual Atmos Health (2024). https://doi.org/10.1007/s11869-024-01574-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11869-024-01574-7