Abstract
Background
Doublecortin-like kinase 3 (DCLK3), a member of tubulin superfamily, has been proved to be closely associated with the pathogenesis of numerous human tumors. However, the expression pattern and regulatory mechanisms of DCLK3 in gastric cancer (GC) remain unknown.
Materials and methods
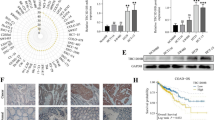
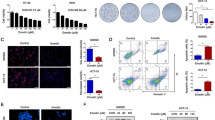
DCLK3 expression in GC cells was assessed by RT-qPCR and western blotting. The correlation between DCLK3 levels and the overall survival of GC patients was assessed via TCGA, ACLBI, and Kaplan–Meier plotter databases. Additionally, key proteins (TCF4) involved in the regulation of DCLK3 on GC progression were screened by ACLBI database. Cell proliferation, ferroptotic cell death, and oxidative stress markers were measured by EdU staining, immunofluorescence, ELISA, and western blotting assays.
Results
DCLK3 was upregulated in GC, and high DCLK3 expression was significantly associated with poor survival of GC patients. Here, DCLK3 knockdown reduced GC cell proliferation, induced ferroptotic cell death, and exacerbated oxidative stress level. Logistic regression analysis showed that TCF4 was an independent prognostic indicator of GC. Mechanistically, DCLK3 promoted TCF4 expression and subsequently upregulated the expression of TCF4 downstream target genes (c-Myc and Cyclin D1). Furthermore, DCLK3 overexpression enhanced GC cell proliferation, but mitigating ferroptotic cell death and oxidative stress. The regulatory mechanism may involve the upregulation of TCF4, c-Myc, and cyclin D1.
Conclusions
Our research suggests that DCLK3 modulates the levels of iron and reactive oxygen and may involve regulation of TCF4 pathway, thereby promoting the GC cell growth, indicating that DCLK3 may use as a prognostic marker and therapeutic target for GC patients.






Similar content being viewed by others
Availability of data and materials
All data generated or analyzed during this study are included in this article.
References
Sung H, Ferlay J, Siegel RL et al (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71(3):209–249. https://doi.org/10.3322/caac.21660
Kumar S, Metz DC, Ellenberg S et al (2020) Risk factors and incidence of gastric cancer after detection of Helicobacter pylori infection: a large cohort study. Gastroenterology 158(3):527–536. https://doi.org/10.1053/j.gastro.2019.10.019
Zhang X, Huang Z, Xie Z et al (2020) Homocysteine induces oxidative stress and ferroptosis of nucleus pulposus via enhancing methylation of GPX4. Free Radic Biol Med 160(20):552–565. https://doi.org/10.1016/j.freeradbiomed.2020.08.029
Chen X, Kang R, Kroemer G et al (2021) Organelle-specific regulation of ferroptosis. Cell Death Differ 28(10):2843–2856. https://doi.org/10.1038/s41418-021-00859-z
Chen X, Yu C, Kang R et al (2021) Cellular degradation systems in ferroptosis. Cell Death Differ 28(4):1135–1148. https://doi.org/10.1038/s41418-020-00728-1
Hassannia B, Van Coillie S, Vanden BT (2021) Ferroptosis: biological rust of lipid membranes. Antioxid Redox Signal 35(6):487–509. https://doi.org/10.1089/ars.2020.8175
Yu H, Guo P, Xie X et al (2017) Ferroptosis, a new form of cell death, and its relationships with tumourous diseases. J Cell Mol Med 21(4):648–657. https://doi.org/10.1111/jcmm.13008
Xia X, Fan X, Zhao M, Zhu P (2019) The relationship between ferroptosis and tumors: a novel landscape for therapeutic approach. Curr Gene Ther 19(2):117–124. https://doi.org/10.2174/1566523219666190628152137
Ma S, Dielschneider RF, Henson ES et al (2017) Ferroptosis and autophagy induced cell death occur independently after siramesine and lapatinib treatment in breast cancer cells. PLoS One 12(8):e0182921. https://doi.org/10.1371/journal.pone.0182921
Fonseca-Nunes A, Agudo A, Aranda N et al (2015) Body iron status and gastric cancer risk in the EURGAST study. Int J Cancer 137(12):2904–2914. https://doi.org/10.1002/ijc.29669
Sakaguchi M, Hisamori S, Oshima N et al (2016) miR-137 regulates the tumorigenicity of colon cancer stem cells through the inhibition of DCLK1. Mol Cancer Res 14(4):354–362. https://doi.org/10.1158/1541-7786
Shan C, Fei F, Li F et al (2017) miR-448 is a novel prognostic factor of lung squamous cell carcinoma and regulates cells growth and metastasis by targeting DCLK1. Biomed Pharmacother 89:1227–1234. https://doi.org/10.1016/j.biopha.2017.02.017
Wang J, Wang S, Zhou J, Qian Q (2018) miR-424-5p regulates cell proliferation, migration and invasion by targeting doublecortin-like kinase 1 in basal-like breast cancer. Biomed Pharmacother 102:147–152. https://doi.org/10.1016/j.biopha.2018.03.018
Galvan L, Francelle L, Gaillard MC et al (2018) The striatal kinase DCLK3 produces neuroprotection against mutant huntingtin. Brain 141(5):1434–1454. https://doi.org/10.1093/brain/awy057
De de Longprez Longprez L (2018) Etude du rôle de la protéine kinase DCLK3 dans les mécanismes de neurodégénérescence dans la maladie de Huntington. Université Paris Saclay (COmUE)
Zhao Y, Zhou H, Shen J et al (2021) MiR-1236–3p inhibits the proliferation, invasion, and migration of colon cancer cells and hinders epithelial-mesenchymal transition by targeting DCLK3. Front Oncol 11:688882. https://doi.org/10.3389/fonc.2021.688882
Liu NQ, Ter Huurne M, Nguyen LN et al (2017) The non-coding variant rs1800734 enhances DCLK3 expression through long-range interaction and promotes colorectal cancer progression. Nat commun 8(1):14418. https://doi.org/10.1038/ncomms14418
Eusebi LH, Telese A, Marasco G et al (2020) Gastric cancer prevention strategies: a global perspective. J Gastroenterol Hepatol 35(9):1495–1502. https://doi.org/10.1111/jgh.15037
Digklia A, Wagner AD (2016) Advanced gastric cancer: current treatment landscape and future perspectives. World J Gastroenterol 22(8):2403–2413. https://doi.org/10.3748/wjg.v22.i8.2403
Song Z, Wu Y, Yang J et al (2017) Progress in the treatment of advanced gastric cancer. Tumor Biol 39(7):1010428317714626. https://doi.org/10.1177/1010428317714626
Chandrakesan P, Yao J, Qu D et al (2017) Dclk1, a tumor stem cell marker, regulates pro-survival signaling and self-renewal of intestinal tumor cells. Mol Cancer 16(1):1–14. https://doi.org/10.1186/s12943-017-0594-y
Weygant N, Qu D, Berry WL et al (2014) Small molecule kinase inhibitor LRRK2-IN-1 demonstrates potent activity against colorectal and pancreatic cancer through inhibition of doublecortin-like kinase 1. Mol Cancer 13(1):1–14. https://doi.org/10.1186/1476-4598-13-103
Chandrakesan P, Weygant N, May R et al (2014) DCLK1 facilitates intestinal tumor growth via enhancing pluripotency and epithelial mesenchymal transition. Oncotarget 5(19):9269–9280. https://doi.org/10.18632/oncotarget.2393
Carli ALE, Afshar-Sterle S, Rai A et al (2021) Cancer stem cell marker DCLK1 reprograms small extracellular vesicles toward migratory phenotype in gastric cancer cells. Proteomics 21(13–14):e2000098. https://doi.org/10.1002/pmic.202000098
Liu ZQ, He WF, Wu YJ et al (2020) LncRNA SNHG1 promotes EMT process in gastric cancer cells through regulation of the miR-15b/DCLK1/Notch1 axis. BMC Gastroenterol 20(1):1–10. https://doi.org/10.1186/s12876-020-01272-5
Kerjan G, Koizumi H, Han EB et al (2009) Mice lacking doublecortin and doublecortin-like kinase 2 display altered hippocampal neuronal maturation and spontaneous seizures. Proc Natl Acad Sci USA 106(16):6766–6771. https://doi.org/10.1073/pnas.0812687106
He YL, Dai XQ, Li S et al (2022) Doublecortin-like kinase 2 promotes breast cancer cell invasion and metastasis. Clin Transl Oncol 25(4):1–12. https://doi.org/10.1007/s12094-022-03018-z
Liu NQ, Ter Huurne M, Nguyen LN et al (2017) The non-coding variant rs1800734 enhances DCLK3 expression through long-range interaction and promotes colorectal cancer progression. Nat Commun 8(1):1–10. https://doi.org/10.1038/ncomms14418
Ferlay J, Colombet M, Soerjomataram I et al (2019) Estimating the global cancer incidence and mortality in 2018: GLOBOCAN sources and methods. Int J Cancer 144(8):1941–1953. https://doi.org/10.1002/ijc.31937
Hou W, Xie Y, Song X et al (2016) Autophagy promotes ferroptosis by degradation of ferritin. Autophagy 12(8):1425–1428. https://doi.org/10.1080/15548627.2016.1187366
Chen X, Yu C, Kang R, Tang DL (2020) Iron metabolism in ferroptosis. Front Cell Dev Biol 8:590226. https://doi.org/10.3389/fcell.2020.590226
Ye Z, Liu W, Zhuo Q et al (2020) Ferroptosis: final destination for cancer? Cell Prolif 53(3):e12761. https://doi.org/10.1111/cpr.12761
Hao S, Yu J, He W et al (2017) Cysteine dioxygenase 1 mediates erastin-induced ferroptosis in human gastric cancer cells. Neoplasia 19(12):1022–1032. https://doi.org/10.1016/j.neo.2017.10.005
Hu X, Miao J, Zhang M et al (2018) miRNA-103a-3p promotes human gastric cancer cell proliferation by targeting and suppressing ATF7 in vitro. Mol Cells 41(5):390–400. https://doi.org/10.14348/molcells.2018.2078
Li C, Tian Y, Liang Y, Li QC (2020) Circ_0008035 contributes to cell proliferation and inhibits apoptosis and ferroptosis in gastric cancer via miR-599/EIF4A1 axis. Cancer Cell Int 20(1):1–15. https://doi.org/10.1186/s12935-021-02122-4
Baj J, Korona-Głowniak I, Forma A et al (2020) Mechanisms of the epithelial-mesenchymal transition and tumor microenvironment in Helicobacter pylori-induced gastric cancer. Cells 9(4):1055. https://doi.org/10.3390/cells9041055
Yamaji Y, Hirata Y (2020) Treatment for Helicobacter pylori appears to reduce the incidence of gastric cancer: eradication effect or screening effect? Gut 69(3):605–606. https://doi.org/10.1136/gutjnl-2018-318206
Chu B, Kon N, Chen D et al (2019) ALOX12 is required for p53-mediated tumour suppression through a distinct ferroptosis pathway. Nat Cell Biol 21(5):579–591. https://doi.org/10.1038/s41556-019-0305-6
MacDonald BT, Tamai K, He X (2009) Wnt/beta-catenin signaling: components, mechanisms, and diseases. Dev Cell 17(1):9–26. https://doi.org/10.1016/j.devcel.2009.06.016
Daniels DL, Weis WI (2005) β-catenin directly displaces Groucho/TLE repressors from Tcf/Lef in Wnt-mediated transcription activation. Nat Struct Mol Biol 12(4):364–371. https://doi.org/10.1038/nsmb912
Klaus A, Birchmeier W (2008) Wnt signalling and its impact on development and cancer. Nat Rev Cancer 8(5):387–398. https://doi.org/10.1038/nrc2389
He MQ, Wan JF, Zeng HF et al (2021) miR-133a-5p suppresses gastric cancer through TCF4 down-regulation. J Gastrointest Oncol 12(3):1007–1019. https://doi.org/10.21037/jgo-20-418
Zhuang K, Yan Y, Zhang X et al (2016) Gastrin promotes the metastasis of gastric carcinoma through the β-catenin/TCF-4 pathway. Oncol Rep 36(3):1369–1376. https://doi.org/10.3892/or.2016.4943
Wang Y, Zheng L, Shang W et al (2022) Wnt/beta-catenin signaling confers ferroptosis resistance by targeting GPX4 in gastric cancer. Cell Death Differ 29(11):2190–2202. https://doi.org/10.1038/s41418-022-01008-w
Funding
This work was supported by the Natural Science Foundation of Inner Mongolia Autonomous Region (grant no. 2022QN08015) and the Inner Mongolia Autonomous Region Priority Academic Science and Technology Research Projects (grant no. NJZY22051 and NJZZ22074).
Author information
Authors and Affiliations
Contributions
Zhi Q Dong made substantial contributions to the conception and design of the present study. Jie Cheng and Yu C Tang designed the research; Jie Cheng, Yu C Tang, Yuan Dong, Rui L Qin, and Zhi Q Dong performed the research; Jie Cheng and Yu C Tang analyzed the data and wrote the paper.
Corresponding author
Ethics declarations
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cheng, J., Tang, Y.C., Dong, Y. et al. Doublecortin-like kinase 3 (DCLK3) is associated with bad clinical outcome of patients with gastric cancer and regulates the ferroptosis and mitochondria function in vitro and in vivo. Ir J Med Sci 193, 35–43 (2024). https://doi.org/10.1007/s11845-023-03430-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11845-023-03430-6