Abstract
Objective
To observe the clinical effect of acupoint sticking therapy with Mian Tan Gao (facial paralysis paste) plus electroacupuncture (EA) for treating peripheral facial paralysis and its influence on patients’ facial nerve functions, facial disability index and clinical symptoms and signs.
Methods
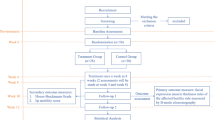
A total of 96 peripheral facial paralysis patients were allocated into an observation group, a medicine group and an EA group by simple randomization, with 32 cases in each group. Patients in the medicine group were treated with oral mecobalamine and prednisone acetate; patients in the EA group were treated with EA on the basis of the medicine treatment; while patients in the observation group were treated with acupoint sticking therapy with Mian Tan Gao (facial paralysis paste) plus EA. After 4-week treatment, the clinical efficacy, the adverse events, and the scores of House-Brackmann (H-B) facial nerve function grading scale, visual analog scale (VAS), clinical symptoms and signs, and facial disability index (FDI) were compared.
Results
After 4-week treatment, the total effective rate was 96.9% in the observation group, higher than 68.7% in the medicine group and 75.0% in the EA group (both P<0.05). After 4-week treatment, the scores of H-B grading scale, VAS and clinical symptoms and signs in the three groups dropped significantly compared with those before treatment, and the scores in the observation group were lower than those in the medicine group and EA group (all P<0.05). After 4-week treatment, the facial disability index-physical function (FDIP) in the FDI in the three groups increased significantly, with a higher value in the observation group compared with that in the medicine group and EA group (both P<0.05). The facial disability index-social function (FDIS) in the FDI dropped significantly, with a lower score in the observation group compared with that in the medicine group and EA group (both P<0.05). However, the comparisons of the items above between the medicine group and the EA group showed no statistical significance (all P>0.05). The between-group comparison of the adverse event across the three groups showed no statistical significance (P>0.05).
Conclusion
Acupoint sticking therapy with Mian Tan Gao (facial paralysis paste) plus EA can decrease H-B grade, reduce pain severity and improve clinical symptoms and signs as well as the facial disability condition in peripheral facial paralysis patients. This method produced more significant efficacy compared with oral medicine and medicine plus EA.
摘要
目的: 观察面瘫膏穴位贴敷加电针对周围性面瘫患者面神经功能、面部残疾及临床症状与体征的影响。 方法: 共纳入周围性面瘫患者96例, 按简单随机化方法分为观察组、药物组和电针组, 每组32例。药物组予以口 服甲钴胺与醋酸泼尼松治疗, 电针组于此基础上加用电针治疗, 观察组予以面瘫膏穴位贴敷加电针治疗。比较三 组患者治疗4周后的临床疗效, 观察不良反应, 以及治疗前后House-Brackmann(H-B)面神经功能分级量表评分、疼 痛视觉模拟量表(VAS)评分、临床症状与体征评分, 以及面部残疾指数评分(FDI)情况。 结果: 治疗4周后, 观察组 的总有效率96.9%, 高于药物组的68.7%和电针组的75.0%(均P<0.05)。 治疗4周后, 3组的H-B分级评分、VAS评分及 临床症状与体征评分均较治疗前下降, 且观察组评分均低于药物组和电针组(均P<0.05)。 治疗4周后, 3组FDI评分 中躯体功能评分(FDIP)较治疗前提高, 且观察组高于药物组和电针组(均P<0.05); 社会生活功能评分(FDIS)较治疗 前降低, 且观察组低于药物组和电针组(均P<0.05); 而药物组与电针组的以上各项评分差异均无统计学意义(均 P>0.05)。 三组不良反应发生率差异无统计学意义(P>0.05) 结论: 面瘫膏穴位贴敷加电针治疗周围性面瘫, 能 降低H-B分级, 减轻疼痛程度, 改善临床症状与体征以及面部残疾状况, 疗效优于口服药物及药物加电针治疗。
Similar content being viewed by others
References
Luijmes RE, Pouwels S, Beurskens CH, Kleiss IJ, Siemann I, Ingels KJ. Quality of life before and after different treatment modalities in peripheral facial palsy: a systematic review. Laryngoscope, 2017, 127(5): 1044–1051.
Wang YN, Zhang LJ, Lü GY, Wang ZQ. AMSTAR assessment of the methodological quality of systematic reviews of the therapeutic effect of acupuncture on peripheral facial paralysis: meta-analyses of the literature. Shanghai Zhenjiu Zazhi, 2018, 37(5): 105–110.
Zhao XY, Li J, Wang JX, Zhang PX. Jin Bohua’s experience of peripheral facial paralysis diagnosed and treated by Yifeng (TE 17). Zhongguo Zhen Jiu, 2017, 37(1): 69–71.
Qu F, Yan HX, Liu YW, Chen PS, Guan HL, Zhou HW, Peng QY, Huang Z. Clinical observation of peripheral facial neuritis treated with acupuncture combined with kinesio taping. Zhongguo Kangfu Yixue Zazhi, 2017, 32(4): 424–427, 450.
Yusufu Z, Zhang QJ. Experience of Professor Zhang Qiu-juan in treating peripheral facial paralysis. Zhongguo Zhongyi Jizheng, 2017, 26(1): 62–64.
Wu HY, Zhang Y, Zhou CJ. Effect analysis of facial penetration electric acupuncture combined with mild moxibustion in treatment of peripheral facial paralysis. Hubei Zhongyiyao Daxue Xuebao, 2017, 19(2): 78–81.
Wang QC. Therapeutics of Acupuncture and Moxibustion. 2nd Edition. Beijing: China Press of Traditional Chinese Medicine, 2007: 69.
Jia JP, Chen SD. Neurology. 7th Edition. Beijing: People’s Medical Publishing House, 2013: 339.
Zhang T. Efficiency of acupuncture combined with cupping therapy in treating patients with acute peripheral facial paralysis. Shiyong Linchuang Yiyao Zazhi, 2018, 22(19): 63–66.
Jin MB, Xu P, Zhang YX, Su L. Effect of acupuncture combined with pricking and cupping therapy on acute stage of peripheral facial paralysis and its effect on H-B classification. Zhonghua Zhongyiyao Xuekan, 2017, 35(10): 2667–2669.
Sun Y, Geng J, Yang K, Wang XY, Jiang WW, Zhao Y. Clinical observation of staging treatment with various acupuncture therapies mainly on Yifeng (TE 17) point for peripheral facial paralysis. Guangzhou Zhongyiyao Daxue Xuebao, 2018, 35(2): 256–260.
Dong ZY, Zhang BQ, Guo XQ. Acupuncture combined with herbal-cake partitioned moxibustion is superior to routine acupuncture in the treatment of peripheral facial paralysis. Zhen Ci Yan Jiu, 2019, 44(2): 131–135.
López Garciarena I, Sinovas Varona I. Peripheral facial paralysis, a presentation of Lyme disease. Emergencias, 2017, 29(1): 65–66.
Cao RJ, Qiu XH, Xie XK. Special penetration needling for refractory peripheral facial paralysis. Zhongguo Zhen Jiu, 2018, 38(3): 269–272.
Wang B, Yang JH, Chen F, Hu J, Liu DX, Jiang AP, Ye H, Wu CS, Cao JP, Li X. Evaluation of therapeutic effect of different Chinese medicine treatments on peripheral facial paralysis. Zhongyi Zazhi, 2017, 58(22): 1929–1933.
Zhang J, Tian Y, Jiang XY. Therapeutic observation on 33 cases of peripheral facial paralysis treated with electroacupuncture plus Bu Yang Huan Wu Tang and Qian Zheng San. Hunan Zhongyi Zazhi, 2017, 33(9): 97–99.
Ye X. Clinical Study on Electroacupuncture Treatment of Peripheral Facial Paralysis. Wuhan: Master Thesis of Hubei University of Chinese Medicine, 2018.
Ruan C. Observations on the therapeutic effect of different waveforms electroacupuncture on convalescence-stage peripheral facial paralysis. Shanghai Zhenjiu Zazhi, 2017, 36(7): 795–798.
Chen NH, Qin Y. Therapeutic observation on acupoint sticking with artificial She Xiang (Moschus) plus acupuncture for treating peripheral facial paralysis. Renmin Junyi, 2017, 60(12): 1197–1198, 1214.
He GZ, Yang JB, Mao HF, Zhang AX. Curative effect of gangliosides and Jia Wei Qian Zheng San on facial neuritis: a clinical observation. Zhongyiyao Daobao, 2015, 21(13): 26–28.
Shi FZ, Wang YL. Clinical observation on integrated Western and Chinese medicine for the treatment of Bell’s facial paralysis. Shanxi Zhongyi, 2017, 33(2): 38–39.
Acknowledgments
This work was supported by The Fourth Batch Research and Training Project for National Outstanding Talent of Traditional Chinese Medicine (Clinical or Basic) [第四批 全国中医(临床、基础)优秀人才研修项目]
Author information
Authors and Affiliations
Corresponding author
Additional information
Conflict of Interest
The authors declare that there is no potential conflict of interest in this article.
Statement of Informed Consent
Informed consent was obtained from all individual p articipants.
Rights and permissions
About this article
Cite this article
Feng, Lm., Zeng, Tt., Hou, Wg. et al. Clinical observation on acupoint sticking therapy plus electroacupuncture for treating peripheral facial paralysis. J. Acupunct. Tuina. Sci. 18, 445–451 (2020). https://doi.org/10.1007/s11726-020-1213-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11726-020-1213-9
Keywords
- Acupuncture Therapy
- Electroacupuncture
- Acupoint Sticking Therapy
- Facial Paralysis
- Visual Analog Scale
- Pain Measurement