Abstract
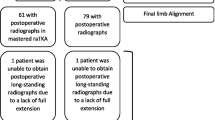
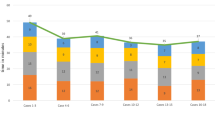
Robotic-assisted total knee arthroplasty (RATKA) has been shown to achieve more accurate component positioning and target alignment than conventional jig-based instrumentation; however, concerns remain regarding its adoption since it is associated with steep learning curves, higher operational costs, and increased surgical time. This study aims to compare the operating times of three cohorts of patients undergoing simultaneous bilateral TKA, i.e., first 50 RATKA, last 50 RATKA (at the end of 1 year), and 50 conventional TKA. This prospective cohort study was conducted at a single high-volume tertiary care center by a single experienced surgeon on 150 patients (300 knees), who were allotted into three equal cohorts of 50, between February 2020 and December 2021. Simultaneous bilateral TKAs were done in all three groups and operative times recorded. We describe the technique for optimizing the surgical time of SB-RATKA for efficient operative room logistics. The operating times of the two robotic-assisted TKA cohorts were compared with the operating times of the conventional SB-TKA cohort. The mean age of the study population was 59(±6.2) years with the majority of females (82%). The mean coronal deformity was comparable between the cohorts. The mean operating time in the conventional CTKA, initial 50 RATKA, and final 50 RATKA cohorts were 115.56 (±10.7), 127.8 (±26), and 91.66 (±13.5) min, respectively, all of which showed a statistically significant difference (p < 0.001). The mean operating times of the final 50 RATKA at the end of 1 year improved by about 36 min with all the SB-RATKA cases being completed in under 120 min. The efficiency of SB-RATKA improved significantly with time and experience, resulting in shorter operational times within a year, revealing the potential of robotic-assisted surgery to surpass conventional approaches in TKA in terms of operating room efficiency.





Similar content being viewed by others
Data availability
No datasets were generated or analyzed during the current study.
Code availability
Not applicable.
Abbreviations
- RATKA:
-
Robotic-assisted total knee arthroplasty
- CTKA:
-
Conventional total knee arthroplasty
- SB-RATKA:
-
Simultaneous bilateral robotic-assisted TKA
- SB-CTKA:
-
Simultaneous bilateral conventional TKA
- ACB:
-
Adductor canal block
- UPS:
-
Uninterrupted power supply
- OR:
-
Operating room
References
Hampp EL, Chughtai M, Scholl LY et al (2019) Robotic-Arm Assisted total knee arthroplasty demonstrated greater accuracy and precision to plan compared with manual techniques. J Knee Surg 32:239–250. https://doi.org/10.1055/s-0038-1641729
Kort N, Stirling P, Pilot P, Müller JH (2022) Robot-assisted knee arthroplasty improves component positioning and alignment, but results are inconclusive on whether it improves clinical scores or reduces complications and revisions: a systematic overview of meta-analyses. Knee Surg Sports Traumatol Arthrosc 30:2639–2653. https://doi.org/10.1007/s00167-021-06472-4
Nam CH, Lee SC, Kim J-H et al (2022) Robot-assisted total knee arthroplasty improves mechanical alignment and accuracy of component positioning compared to the conventional technique. J Exp Orthop 9:108. https://doi.org/10.1186/s40634-022-00546-z
Kayani B, Konan S, Pietrzak JRT, Haddad FS (2018) Iatrogenic bone and soft tissue trauma in robotic-arm assisted total knee arthroplasty compared with conventional jig-based total knee arthroplasty: a prospective cohort study and validation of a new classification system. J Arthroplasty 33:2496–2501. https://doi.org/10.1016/j.arth.2018.03.042
Khlopas A, Chughtai M, Hampp EL et al (2017) Robotic-arm assisted total knee arthroplasty demonstrated soft tissue protection. Surg Technol Int 30:441–446
Song E-K, Seon J-K, Yim J-H et al (2013) Robotic-assisted TKA reduces postoperative alignment outliers and improves gap balance compared to conventional TKA. Clin Orthop Relat Res 471:118–126. https://doi.org/10.1007/s11999-012-2407-3
Masilamani ABS, Jayakumar T, Mulpur P et al (2023) Functional alignment is associated with increased incidence of pre-balance, reduced soft-tissue release, and post-operative pain compared to mechanical alignment in patients undergoing simultaneous bilateral robotic-assisted TKA. J Robot Surg 17:2919–2927. https://doi.org/10.1007/s11701-023-01732-6
Mulpur P, Masilamani ABS, Prakash M et al (2022) Comparison of patient reported outcomes after robotic versus manual total knee arthroplasty in the same patient undergoing staged bilateral knee arthroplasty. J Orthop 34:111–115. https://doi.org/10.1016/j.jor.2022.08.014
Song E-K, Seon J-K, Park S-J et al (2011) Simultaneous bilateral total knee arthroplasty with robotic and conventional techniques: a prospective, randomized study. Knee Surg Sports Traumatol Arthrosc 19:1069–1076. https://doi.org/10.1007/s00167-011-1400-9
Kayani B, Konan S, Tahmassebi J et al (2018) Robotic-arm assisted total knee arthroplasty is associated with improved early functional recovery and reduced time to hospital discharge compared with conventional jig-based total knee arthroplasty: a prospective cohort study. Bone Joint J 100(B):930–937. https://doi.org/10.1302/0301-620X.100B7.BJJ-2017-1449.R1
Khlopas A, Sodhi N, Hozack WJ et al (2020) Patient-reported functional and satisfaction outcomes after robotic-arm-assisted total knee arthroplasty: early results of a prospective multicenter investigation. J Knee Surg 33:685–690. https://doi.org/10.1055/s-0039-1684014
Bhimani SJ, Bhimani R, Smith A et al (2020) Robotic-assisted total knee arthroplasty demonstrates decreased postoperative pain and opioid usage compared to conventional total knee arthroplasty. Bone Jt Open 1:8–12. https://doi.org/10.1302/2633-1462.12.BJO-2019-0004.R1
Marchand RC, Sodhi N, Anis HK et al (2019) One-year patient outcomes for robotic-arm-assisted versus manual total knee arthroplasty. J Knee Surg 32:1063–1068. https://doi.org/10.1055/s-0039-1683977
Zhang J, Ndou WS, Ng N et al (2021) Robotic-arm assisted total knee arthroplasty is associated with improved accuracy and patient reported outcomes: a systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-021-06464-4
Mancino F, Rossi SMP, Sangaletti R et al (2022) A new robotically assisted technique can improve outcomes of total knee arthroplasty comparing to an imageless navigation system. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-022-04560-9
Mancino F, Cacciola G, Malahias M-A et al (2020) What are the benefits of robotic-assisted total knee arthroplasty over conventional manual total knee arthroplasty? A systematic review of comparative studies. Orthop Rev 12:8657. https://doi.org/10.4081/or.2020.8657
Jung HJ, Kang MW, Lee JH, Il KJ (2023) Learning curve of robot-assisted total knee arthroplasty and its effects on implant position in Asian patients: a prospective study. BMC Musculoskelet Disord 24:332. https://doi.org/10.1186/s12891-023-06422-w
Siebert W, Mai S, Kober R, Heeckt PF (2002) Technique and first clinical results of robot-assisted total knee replacement. Knee 9:173–180. https://doi.org/10.1016/s0968-0160(02)00015-7
Vermue H, Luyckx T, Winnock de Grave P et al (2022) Robot-assisted total knee arthroplasty is associated with a learning curve for surgical time but not for component alignment, limb alignment and gap balancing. Knee Surg Sports Traumatol Arthrosc 30:593–602. https://doi.org/10.1007/s00167-020-06341-6
Kayani B, Konan S, Huq SS et al (2019) Robotic-arm assisted total knee arthroplasty has a learning curve of seven cases for integration into the surgical workflow but no learning curve effect for accuracy of implant positioning. Knee Surg Sports Traumatol Arthrosc 27:1132–1141. https://doi.org/10.1007/s00167-018-5138-5
Grau L, Lingamfelter M, Ponzio D et al (2019) Robotic arm assisted total knee arthroplasty workflow optimization, operative times and learning curve. Arthroplast Today 5:465–470. https://doi.org/10.1016/j.artd.2019.04.007
Kellgren JH, Lawrence JS (1957) Radiological assessment of osteo-arthrosis. Ann Rheum Dis 16:494–502. https://doi.org/10.1136/ard.16.4.494
Hopper AN, Jamison MH, Lewis WG (2007) Learning curves in surgical practice. Postgrad Med J 83:777–779. https://doi.org/10.1136/pgmj.2007.057190
Yotsumoto F, Sanui A, Ito T et al (2022) Cumulative summation analysis of learning curve for robotic-assisted hysterectomy in patients with gynecologic tumors. Anticancer Res 42:4111–4117. https://doi.org/10.21873/anticanres.15909
Schopper C, Proier P, Luger M et al (2022) The learning curve in robotic assisted knee arthroplasty is flattened by the presence of a surgeon experienced with robotic assisted surgery. Knee Surg Sports Traumatol Arthrosc:1–8. https://doi.org/10.1007/s00167-022-07048-6
Patel K, Judd H, Harm RG et al (2022) Robotic-assisted total knee arthroplasty: Is there a maximum level of efficiency for the operating surgeon? J Orthop 31:13–16. https://doi.org/10.1016/j.jor.2022.02.015
Coon TM (2009) Integrating robotic technology into the operating room. Am J Orthop (Belle Mead NJ) 38:7–9
Mahure SA, Teo GM, Kissin YD et al (2022) Learning curve for active robotic total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 30:2666–2676. https://doi.org/10.1007/s00167-021-06452-8
Bell C, Grau L, Orozco F et al (2022) The successful implementation of the Navio robotic technology required 29 cases. J Robot Surg 16:495–499. https://doi.org/10.1007/s11701-021-01254-z
Savov P, Tuecking L-R, Windhagen H et al (2021) Imageless robotic handpiece-assisted total knee arthroplasty: a learning curve analysis of surgical time and alignment accuracy. Arch Orthop Trauma Surg 141:2119–2128. https://doi.org/10.1007/s00402-021-04036-2
Thiengwittayaporn S, Uthaitas P, Senwiruch C et al (2021) Imageless robotic-assisted total knee arthroplasty accurately restores the radiological alignment with a short learning curve: a randomized controlled trial. Int Orthop 45:2851–2858. https://doi.org/10.1007/s00264-021-05179-y
Vanlommel L, Neven E, Anderson MB et al (2021) The initial learning curve for the ROSA® Knee System can be achieved in 6–11 cases for operative time and has similar 90-day complication rates with improved implant alignment compared to manual instrumentation in total knee arthroplasty. J Exp Orthop 8:119. https://doi.org/10.1186/s40634-021-00438-8
Ali M, Phillips D, Kamson A et al (2022) Learning curve of robotic-assisted total knee arthroplasty for non-fellowship-trained orthopedic surgeons. Arthroplast Today 13:194–198. https://doi.org/10.1016/j.artd.2021.10.020
Naziri Q, Cusson BC, Chaudhri M et al (2019) Making the transition from traditional to robotic-arm assisted TKA: What to expect? A single-surgeon comparative-analysis of the first-40 consecutive cases. J Orthop 16:364–368. https://doi.org/10.1016/j.jor.2019.03.010
Peersman G, Laskin R, Davis J et al (2006) Prolonged operative time correlates with increased infection rate after total knee arthroplasty. HSS J 2:70–72. https://doi.org/10.1007/s11420-005-0130-2
Cacciola G, Bosco F, Giustra F et al (2022) Learning curve in robotic-assisted total knee arthroplasty: a systematic review of the literature. Appl Sci 12. https://doi.org/10.3390/app122111085
Acknowledgements
Nil.
Funding
There is no funding source.
Author information
Authors and Affiliations
Contributions
CRediT author statement. ABSM: conceptualization, methodology, writing—reviewing, editing, and final approval. PM: conceptualization, writing—reviewing, editing, and final approval. TJ: writing—original draft, data curation, investigation, and formal analysis. SB: data curation, writing—reviewing, and editing. KH: writing—reviewing, editing, and final approval. RV: writing—reviewing, editing, and final approval. AVGR: conceptualization, writing—reviewing, editing, and final approval.
Corresponding author
Ethics declarations
Conflict of interests
The authors declare that they have no conflict of interest.
Ethical approval
Obtained: institutional ethics committee approval.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Consent to participate
Obtained.
Consent to publish
Obtained.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Masilamani, A.B.S., Mulpur, P., Jayakumar, T. et al. Operating room efficiency for a high-volume surgeon in simultaneous bilateral robotic-assisted total knee arthroplasty: a prospective cohort study. J Robotic Surg 18, 188 (2024). https://doi.org/10.1007/s11701-024-01947-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11701-024-01947-1