Abstract
Background
The objective of this study was to assess Canadian general surgeons’ knowledge of bariatric surgery and perceived availability of resources to manage bariatric surgery patients.
Methods
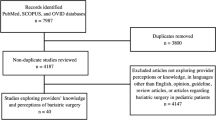
A self-administered questionnaire was developed using a focus group of general surgeons. The questionnaire was distributed at two large general surgery conferences in September and November 2012. The survey was also disseminated via membership association electronic newsletters in November and December 2012.
Results
One hundred sixty-seven questionnaires were completed (104 practicing surgeons, 63 general surgery trainees). Twenty respondents were bariatric surgeons. Among 84 non-bariatric surgeons, 68.3 % referred a patient in the last year for bariatric surgery, 79 % agreed that bariatric surgery resulted in sustained weight loss, and 81.7 % would consider referring a family member. Knowledge gaps were identified in estimates of mortality and morbidity associated with bariatric procedures. The majority of surgeons surveyed have encountered patients with complications from bariatric surgery in the last year. Over 50 % of surgeons who do not perform bariatric procedures reported not feeling confident to manage complications, 35.4 % reported having adequate resources and equipment to manage morbidly obese patients, and few are able to transfer patients to a bariatric center. Of the respondents, 73.3 % reported residency training provided inadequate exposure to bariatric surgery, and 85.3 % felt that additional continuing medical education resources would be useful.
Conclusions
There appears to be support for bariatric surgery among Canadian general surgeons participating in this survey. Knowledge gaps identified indicate the need for more education and resources to support general surgeons managing bariatric surgical patients.
Similar content being viewed by others
References
Steinbrook R. Surgery for severe obesity. NEJM. 2004;350(11):1075–9.
Pories WJ, Swanson M, MacDonald K, et al. Who would have thought it? An operation proves to be the most effective therapy for adult-onset diabetes mellitus. Ann Surg. 1995;222(3):339–50.
PHAC. Obesity in Canada: a joint report from the public health agency of Canada and the Canadian Institute for Health Information. 2011.
PHAC. Obesity in Canada—snapshot. 2009.
WHO, Fact sheet no. 311. 2012.
McGuire S, Shields M, Carroll MD, et al. Adult obesity prevalence in Canada and the United States. NCHS data brief no. 56, Hyattsville, MD: National Center for Health Statistics. Adv Nutr. 2011;2(4):368–9.
Janssen I, Lam M, Katzmarzyk PT. Influence of overweight and obesity on physician costs in adolescents and adults in Ontario, Canada. Obes Rev. 2009;10(1):51–7.
Ahima RS. Digging deeper into obesity. J Clin Invest. 2011;121(6):2076–9.
Must A, Spadano J, Coakley E, et al. The disease burden associated with overweight and obesity. JAMA. 1999;282(16):1523–9.
Fontaine K, Redden D, Wang C, et al. Years of life lost due to obesity. JAMA. 2003;289(2):187–93.
Stewart S, Cutler D, Rosen A. Forecasting the effects of obesity and smoking on U.S. life expectancy. NEJM. 2009;361(23):2252–60.
Dhabuwala A, Cannan R, Stubbs R. Improvement in co-morbidities following weight loss from gastric bypass surgery. Obes Surg. 2000;10:428–35.
Picot J, Jones J, Colquitt JL, et al. The clinical effectiveness and cost-effectiveness of bariatric (weight loss) surgery for obesity: a systematic review and economic evaluation. Health Technol Assess. 2009;13(41):1–190. 215–357, iii-iv.
Dansinger M, Tatsioni A, Wong J, et al. Meta-analysis: the effect of dietary counseling for weight loss. Ann Intern Med. 2007;147:41–50.
Padwal R, Majumdar S. Drug treatments for obesity: orlistat, sibutramine, and rimonabant. Lancet. 2007;369:71–7.
Maggard M, Shugarman L, Suttorp M, et al. Meta-analysis: surgical treatment of obesity. Ann Intern Med. 2005;142(7):547–59.
Sjöström L, Narbro K, Sjöström D, et al. Effects of bariatric surgery on mortality in Swedish obese subjects. NEJM. 2007;357(8):741–52.
Gallagher SF, Banasiak M, Gonzalvo J, et al. The impact of bariatric surgery on the Veterans Administration Healthcare System: a cost analysis. Obes Surg. 2003;13:245–8.
Tanner B, Allen J. Complications of bariatric surgery: implications for the covering physician. Am Surg. 2009;75(2):103–12.
Al Harakeh A. Complications of laparoscopic Roux-en-Y gastric bypass. Surg Clin N Am. 2011;91(6):1225–37.
Eid I. Complications associated with adjustable gastric banding for morbid obesity: a surgeon’s guide. Can J Surg. 2011;54(1):61–6.
Shi X, Karmali S, Sharma A, et al. A review of laparoscopic sleeve gastrectomy for morbid obesity. Obes Surg. 2010;20(8):1171–7.
Herpertz S, Kielmann R, Wolf A, et al. Does obesity surgery improve psychosocial functioning? A systematic review. Int J Obes Relat Metab Disord. 2003;27(11):1300–14.
Jia H, Lubetkin E. The impact of obesity on health-related quality-of-life in the general adult US population. J Public Health. 2005;27(2):156–64.
Avidor, Still C, Brunner M, et al. Primary care and subspecialty management of morbid obesity: referral patterns for bariatric surgery. Surg Obes Relat Dis. 2007;3(3):392–407.
Hedley A. Prevalence of overweight and obesity among US children, adolescents, and adults, 1999–2002. JAMA. 2004;291(23):2847–50.
ASMBS. Estimate of bariatric surgery numbers, 2011–2014. [Web page] 2015 [cited July 13, 2015].
Nguyen NT, Moore C, Stevens M, et al. The practice of bariatric surgery at academic medical centers. J Gastrointest Surg. 2004;8(7):856–60. discussion 860–1.
Nguyen NT, Paya M, Stevens M, et al. The relationship between hospital volume and outcome in bariatric surgery at academic medical centers. Transactions of the meeting of the American Surgical Association. 2004. CXXII(&NA): p. 184–192.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Statement of Informed Consent
Informed consent was obtained from all individual participants included in the study.
Statement of Human and Animal Rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Funding
No external sources of funding were used for this study or its publication.
Rights and permissions
About this article
Cite this article
Hirpara, D.H., Cleghorn, M.C., Kwong, J. et al. Perception and Awareness of Bariatric Surgery in Canada: a National Survey of General Surgeons. OBES SURG 26, 1799–1805 (2016). https://doi.org/10.1007/s11695-015-1975-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-015-1975-1