Abstract
Objective
This study aimed to establish a nomogram model to predict the mortality risk of patients with dangerous upper gastrointestinal bleeding (DUGIB), and identify high-risk patients who require emergent therapy.
Methods
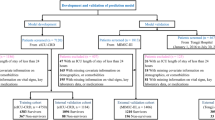
From January 2020 to April 2022, the clinical data of 256 DUGIB patients who received treatments in the intensive care unit (ICU) were retrospectively collected from Renmin Hospital of Wuhan University (n=179) and the Eastern Campus of Renmin Hospital of Wuhan University (n=77). The 179 patients were treated as the training cohort, and 77 patients as the validation cohort. Logistic regression analysis was used to calculate the independent risk factors, and R packages were used to construct the nomogram model. The prediction accuracy and identification ability were evaluated by the receiver operating characteristic (ROC) curve, C index and calibration curve. The nomogram model was also simultaneously externally validated. Decision curve analysis (DCA) was then used to demonstrate the clinical value of the model.
Results
Logistic regression analysis showed that hematemesis, urea nitrogen level, emergency endoscopy, AIMS65, Glasgow Blatchford score and Rockall score were all independent risk factors for DUGIB. The ROC curve analysis indicated the area under curve (AUC) of the training cohort was 0.980 (95%CI: 0.962–0.997), while the AUC of the validation cohort was 0.790 (95%CI:0.685–0.895). The calibration curves were tested for Hosmer-Lemeshow goodness of fit for both training and validation cohorts (P=0.778, P=0.516).
Conclusion
The developed nomogram is an effective tool for risk stratification, early identification and intervention for DUGIB patients.
Similar content being viewed by others
References
Kamboj AK, Hoversten P, Leggett CL. Upper Gastrointestinal Bleeding: Etiologies and Management. Mayo Clin Proc, 2019,94(4):697–703
Hreinsson JP, Jonsson A, Bjornsson ES. Acute upper gastrointestinal bleeding: a population-based, five-year follow-up study. Scand J Gastroenterol, 2021,56(1):1–5
Emergency physicians of Chinese Medical Association. Expert consensus on emergency diagnosis and treatment process of acute upper gastrointestinal hemorrhage. Chin J of Critical Care Med, 2021,35:865–873
Costable NJ, Greenwald DA. Upper Gastrointestinal Bleeding. Clin Geriatr Med, 2021,37(1):155–172
Oakland K. Changing epidemiology and etiology of upper and lower gastrointestinal bleeding. Best Pract Res Clin Gastroenterol, 2019,42–43:101610
Laine L, Barkun AN, Saltzman JR, et al. ACG Clinical Guideline: Upper Gastrointestinal and Ulcer Bleeding. Am J Gastroenterol, 2021,116(5):899–917
Emergency physicians of Chinese Medical Association. Expert consensus on emergency diagnosis and treatment process of acute upper gastrointestinal bleeding. Chin J Emerg Med, 2021,30(1):15–24
Laursen SB, Oakland K, Laine L, et al. ABC score: a new risk score that accurately predicts mortality in acute upper and lower gastrointestinal bleeding: an international multicentre study. Gut, 2021,70(4):707–716
Samuel R, Bilal M, Tayyem O, et al. Evaluation and management of non-variceal upper gastrointestinal bleeding. Dis Mon, 2018,64(7):333–343
Liu S, Zhang X, Walline JH, et al. Comparing the Performance of the ABC, AIMS65, GBS, and pRS Scores in Predicting 90-day Mortality Or Rebleeding Among Emergency Department Patients with Acute Upper Gastrointestinal Bleeding: A Prospective Multicenter Study. J Transl Int Med, 2021,9(2):114–122
Blatchford O, Murray WR, Blatchford M. A risk score to predict need for treatment for upper-gastrointestinal haemorrhage. Lancet, 2000,356(9238):1318–1321
Custovic N, Husic-Selimovic A, Srsen N, et al. Comparison of Glasgow-Blatchford Score and Rockall Score in Patients with Upper Gastrointestinal Bleeding. Med Arch, 2020,74(4):270–274
Rockall TA, Logan RF, Devlin HB, et al. Risk assessment after acute upper gastrointestinal haemorrhage. Gut, 1996,38(3):316–321
Saltzman JR, Tabak YP, Hyett BH, et al. A simple risk score accurately predicts in-hospital mortality, length of stay, and cost in acute upper GI bleeding. Gastrointest Endosc, 2011,74(6):1215–1224
Yaka E, Yilmaz S, Dogan N, et al. Comparison of the Glasgow-Blatchford and AIMS65 scoring systems for risk stratification in upper gastrointestinal bleeding in the emergency department. Acad Emerg Med, 2015,22(1):22–30
Budimir I, Gradišer M, Nikolić M, et al. Glasgow Blatchford, pre-endoscopic Rockall and AIMS65 scores show no difference in predicting rebleeding rate and mortality in variceal bleeding. Scand J Gastroenterol, 2016,51(11):1375–1379
Martínez-Cara JG, Jiménez-Rosales R, Úbeda-Muñoz M, et al. Comparison of AIMS65, Glasgow-Blatchford score, and Rockall score in a European series of patients with upper gastrointestinal bleeding: performance when predicting in-hospital and delayed mortality. United European Gastroenterol J, 2016,4(3):371–379
Dogru U, Yuksel M, Ay MO, et al. The effect of the shock index and scoring systems for predicting mortality among geriatric patients with upper gastrointestinal bleeding: a prospective cohort study. Sao Paulo Med J, 2022,140(4):531–539
Chen L, Zheng H, Wang S. Prediction model of emergency mortality risk in patients with acute upper gastrointestinal bleeding: a retrospective study. PeerJ, 2021,9:e11656
Jiang GJ, Gao RK, Wang M, et al. A Nomogram Model for Predicting Type-2 Myocardial Infarction Induced by Acute Upper Gastrointestinal Bleeding. Curr Med Sci, 2022,42(2):317–326
Zhou YJ, Zheng JN, Zhou YF, et al. Development of a prognostic nomogram for cirrhotic patients with upper gastrointestinal bleeding. Eur J Gastroenterol Hepatol, 2017,29(10):1166–1173
Lai Y, Xu Y, Zhu Z, et al. Development and validation of a model to predict rebleeding within three days after endoscopic hemostasis for high-risk peptic ulcer bleeding. BMC Gastroenterol, 2022,22(1):64
Riley RD, Ensor J, Snell KIE, et al. Calculating the sample size required for developing a clinical prediction model. BMJ, 2020,368:m441
Al Duhailib Z, Dionne JC, Alhazzani W. Management of severe upper gastrointestinal bleeding in the ICU. Curr Opin Crit Care, 2020,26(2):212–218
Zhang Z, Zhao X, Li Z, et al. Development of a nomogram model to predict survival outcomes in patients with primary hepatic neuroendocrine tumors based on SEER database. BMC Cancer, 2021,21(1):567
Fu M, Huang Y, Peng X, et al. Development of Tumor Mutation Burden-Related Prognostic Model and Novel Biomarker Identification in Stomach Adenocarcinoma. Front Cell Dev Biol, 2022,10:790920
Laine L, Laursen SB, Zakko L, et al. Severity and Outcomes of Upper Gastrointestinal Bleeding With Bloody Vs. Coffee-Grounds Hematemesis. Am J Gastroenterol, 2018,113(3):358–366
Al-Naamani K, Alzadjali N, Barkun AN, et al. Does blood urea nitrogen level predict severity and high-risk endoscopic lesions in patients with nonvariceal upper gastrointestinal bleeding? Can J Gastroenterol, 2008,22(4):399–403
Tomizawa M, Shinozaki F, Hasegawa R, et al. Patient characteristics with high or low blood urea nitrogen in upper gastrointestinal bleeding. World J Gastroenterol, 2015,21(24):7500–7505
Chopra D, Rosenberg M, Moayyedi P, et al. Is Blood Urea Concentration an Independent Predictor of Positive Endoscopic Findings in Presumed Upper Gastrointestinal Bleeding? Dig Dis, 2020,38(1):77–84
Chen L, Chen L, Zheng H, et al. The association of blood urea nitrogen levels upon emergency admission with mortality in acute exacerbation of chronic obstructive pulmonary disease. Chron Respir Dis, 2021,18:14799731211060051
Kaya E, Karaca MA, Aldemir D, et al. Predictors of poor outcome in gastrointestinal bleeding in emergency department. World J Gastroenterol, 2016,22(16):4219–4225
Cúrdia Gonçalves T, Barbosa M, Xavier S, et al. AIMS65 score: a new prognostic tool to predict mortality in variceal bleeding. Scand J Gastroenterol, 2017,52(4):469–470
Monteiro S, Gonçalves TC, Magalhães J, et al. Upper gastrointestinal bleeding risk scores: Who, when and why? World J Gastrointest Pathophysiol, 2016,7(1):86–96
Kim MS, Choi J, Shin WC. AIMS65 scoring system is comparable to Glasgow-Blatchford score or Rockall score for prediction of clinical outcomes for non-variceal upper gastrointestinal bleeding. BMC Gastroenterol, 2019,19(1):136
Sengupta N, Tapper EB, Patwardhan VR, et al. High Glasgow Blatchford Score at admission is associated with recurrent bleeding after discharge for patients hospitalized with upper gastrointestinal bleeding. Endoscopy, 2016,48(1):9–15
Carlsen NV, De Muckadell OBS, Laursen SB. Risk scoring systems for assessment of patients with upper gastrointestinal bleeding. Ugeskr Laeger (Danish), 2021,183(12):V11200856
Uysal Y, Babus SB, Kose A, et al. The prognostic significance of the risk scores at upper gastrointestinal bleeding. Niger J Clin Pract, 2019,22(8):1099–1108
Tham J, Stanley A. Clinical utility of pre-endoscopy risk scores in upper gastrointestinal bleeding. Expert Rev Gastroenterol Hepatol, 2019,13(12):1161–1167
Lu X, Zhang X, Chen H. Comparison of the AIMS65 score with the Glasgow-Blatchford and Rockall scoring systems for the prediction of the risk of in-hospital death among patients with upper gastrointestinal bleeding. Rev Esp Enferm Dig, 2020,112(6):467–473
Acknowledgements
We thank Li-long ZHANG and Li HUANG for their help in revision of this manuscript.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
All authors declare no conflict of interest in this research.
Additional information
This work was supported by Wuhan Scientific Research Project (No. EX20B05) and National Nature Science Foundation of China (No. 82000521).
Rights and permissions
About this article
Cite this article
Liu, Z., Zhang, L., Li, G. et al. A Nomogram Model for Prediction of Mortality Risk of Patients with Dangerous Upper Gastrointestinal Bleeding: A Two-center Retrospective Study. CURR MED SCI 43, 723–732 (2023). https://doi.org/10.1007/s11596-023-2748-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-023-2748-z