Abstract
Background
Prior to volar locked plating and early motion protocols, ligamentous injuries incidentally associated with distal radius fractures may have been indirectly treated with immobilization. Our goal was to determine the prevalence of scapholunate instability in our population, while identifying those who may have had progression of instability.
Methods
We retrospectively reviewed 221 distal radius fractures treated with a volar locking plate during a 6-year period. Average patient age was 59 years. Standard posteroanterior and lateral radiographs from the first and last postoperative visits were analyzed for scapholunate instability, using the criteria of scapholunate gap ≥3 mm and scapholunate angle ≥60°.
Results
Six patients (3 %) met neither or only one criterion for instability at the first postoperative visit and did not have ligament repair and then went on to meet both criteria at the last postoperative visit after an early motion protocol. Seven patients (3 %) met both criteria at the first and last postoperative visits and did not have ligament repair. Five patients (2 %) underwent primary scapholunate ligament repair at the time of distal radius fixation.
Conclusions
In our representative population, scapholunate instability was uncommon, either from initial injury or possible progression of occult ligament injury, despite early motion without operative treatment of the ligament. Thus, we did not find strong evidence for routinely delaying motion or pursuing further workup. When early radiographs clearly demonstrate acute scapholunate instability, more aggressive treatment may be appropriate for selected patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Scapholunate ligament injuries are reportedly common with distal radius fractures, based on arthroscopic studies of relatively young patients with higher energy injuries [5, 8, 14]. While current treatment of distal radius fractures is generally routine and reliable, treatment of scapholunate instability is neither [4], and little evidence exists to guide treatment of this combination of injuries. With the trend towards volar locked plating and early motion protocols, speculation has been raised that we may begin to see progression of occult ligament injuries (i.e., not seen on initial radiographs) that were previously treated indirectly by immobilization [5].
In our practice, we routinely begin active range of motion at 1–2 weeks after volar locked plating of distal radius fractures, which takes advantage of rigid fixation. Our practice also includes patients more typical of this injury, generally older than in the aforementioned studies of ligament injuries. Our goal was to determine the prevalence of scapholunate instability in our patients, while distinguishing those who may have had progression of instability from those who already had instability upon presentation. Our hypothesis was that we would find few cases of instability overall, and even fewer with apparent progression of instability after early motion, thus supporting our current protocol.
Materials and Methods
All distal radius fractures treated with the Acumed (Hillsboro, OR) Acu-Loc first-generation volar locking plate at our institution during a 6-year period were, retrospectively, reviewed. Cases with fewer than 3 months of follow-up were excluded (17 fractures), leaving 221 fractures in the study group. Average patient age was 59 years (range 18–96). Seventy-seven percent of patients were female, and 53 % of fractures were left-sided. By the AO classification of fractures, there were 38 % type A, 7 % type B, and 55 % type C.
Standard posteroanterior (PA) and lateral radiographs were analyzed at the first and last postoperative visits. Initial injury films were not used due to frequent poor quality (e.g., obscured by plaster or metal splint material) and nonstandard views (e.g., varying degrees of obliquity). Scapholunate angle was measured on the lateral radiograph, using the line tangent to the volar aspects of the proximal and distal scaphoid poles and the line perpendicular to tangent of the lunate poles [12]. Scapholunate gap was measured on the PA radiograph, using the midpoints of the opposing scaphoid and lunate surfaces [18]. The criteria for scapholunate instability were scapholunate gap ≥3 mm and scapholunate angle ≥60°. Clenched-fist view, fluoroscopy, arthrography, arthroscopy, and magnetic resonance imaging (MRI) were not routinely obtained.
Approval was obtained from the institutional review board regarding procedures to ensure protection of human rights and informed consent.
Surgical Technique
All procedures were performed by three fellowship-trained hand surgeons. Regional anesthesia was used for the majority of cases. Standard technique involved the flexor carpi radialis approach, elevation of the pronator quadratus, fracture reduction and fixation assisted by fluoroscopy, and repair of the pronator quadratus. A volar plaster splint was applied for 1–2 weeks postoperatively, at which time sutures were removed and a Velcro wrist splint was provided. Therapy including active range of motion was then initiated with a certified hand therapist.
If ligament repair was performed, direct reapproximation was achieved with Mitek (Raynham, MA) Mini QuickAnchor suture anchors and supported with Blatt capsulodesis and temporary pinning. A volar plaster splint was applied for 1–2 weeks postoperatively, at which time sutures were removed and a short-arm thumb spica cast was placed. The cast and pins were removed at 6 to 8 weeks postoperatively. Therapy including active range of motion was then initiated with a certified hand therapist.
Results
Average follow-up was 6.2 months (range 3–45). Eighteen cases (8 %) met radiographic criteria for scapholunate instability (scapholunate gap ≥3 mm, scapholunate angle ≥60°) at first and/or last postoperative visit, or had ligament repair at the time of distal radius fixation. These included:
-
Group I:
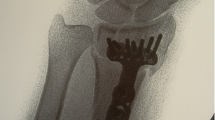
Six patients (3 %) met neither criteria (four patients) or only one criterion (two patients) for instability at the first postoperative visit and did not have ligament repair and then went on to meet both criteria at the last postoperative visit. Average age of these patients was 71 years (range 58–90). Four were female. Two were left-sided. There were one type A, one type B, and four type C fractures. A representative radiograph from this group is shown (Fig. 1).
-
Group II:
Seven patients (3 %) met both criteria for instability at the first and last postoperative visits and did not have ligament repair. Average age of these patients was 64 years (range 41–74). Five were female. Three were left-sided. There were three type A and four type C fractures. A representative radiograph from this group is shown (Fig. 2).
-
Group III:
Five patients (2 %) underwent primary scapholunate ligament repair with suture anchors, Blatt capsulodesis, and temporary pinning at the time of volar locked plating of the distal radius fracture. Average age of these patients was 48 years (range 21–62). Three were female. Four were left-sided. There were two type B and three type C fractures.
None of the excluded patients met radiographic criteria for instability during their follow-up of less than 3 months.
Discussion
Scapholunate instability as determined by established radiographic parameters appears to be uncommon despite early motion after volar locked plating of distal radius fractures. Overall, only 8 % of our patients had radiographic evidence of instability at any time, and only 3 % (group I) had apparent progression during the follow-up period which might be attributed to early motion. Thus, we did not find strong support for routinely delaying motion or investigating for possible occult scapholunate ligament injuries, such as with MRI or arthroscopy, especially considering the higher age and low demand in these six patients (group I, average age 71 years).
Even when apparent at injury, instability may result not from the acute trauma, but from chronic or accumulated trauma, generalized laxity, crystalline arthropathy, or other age-related changes accompanying osteoarthritis [1, 3, 17, 19, 21, 25]. Indeed, four of the seven cases in group II demonstrated evidence of pre-existing wrist pathology, including chondrocalcinosis and/or arthritic changes (sclerosis and narrowing) of the radioscaphoid, capitolunate, or scaphotrapeziotrapezoid articulations. Whether or not instability is related to such pre-existing pathology, relatively higher age and lower demand may still favor non-operative treatment of the ligament in some cases (as in our group II, average age 64 years).
In this regard, our series is clinically relevant as our demographics are more typical of distal radius fractures in the general population (i.e., older patients, predominantly female, lower energy injuries) compared to prior studies of distal radius fracture with ligament injuries [5, 8, 14]. Those studies involved patients with average ages of 32, 39, and 41, with more males in total, and found a 14–20 % prevalence of arthroscopically confirmed grade 3 or 4 scapholunate ligament tear. Younger patients are also more prone to acute scapholunate ligament injuries in general [16]. We found few cases of instability, at any time point, in our older population.
Ligament Repair
In younger or more active patients, surgeons may recommend more aggressive treatment for scapholunate ligament injury (as in our group III, average age 48 years). Repair or reconstruction is generally considered advisable to avoid scapholunate advanced collapse (SLAC) wrist and is therefore commonly accepted practice [4, 22]. More aggressive workup for occult injuries might thus be warranted in these cases. The aforementioned study of younger patients (average 41 years) by Forward et al. found that distal radius fractures with untreated arthroscopically diagnosed grade 3 scapholunate ligament injuries were associated with greater pain on Watson’s shift test at 1 year, compared to untreated lower grade ligament injuries [5]. In spite of this, grip strength, range of motion, and overall Gartland and Werley scores were not significantly different. Furthermore, subjective Gartland and Werley scores were surprisingly significantly better among the untreated grade 3 ligament injuries, prompting speculation that untreated high-grade ligament injuries allow the carpus to better conform to the altered distal radius after fracture, thus perhaps making ligament repair inadvisable in some cases [24].
If primary scapholunate ligament repair is pursued, improved techniques may be needed and continue to be investigated. For isolated tears, primary repair augmented with Blatt capsulodesis (as in our group III) has shown disappointing results at long term (average 5.5 years), with 15 of 17 patients rated fair or poor [18]. Two studies have shown better results, although at shorter term (average 19 and 33 months) [2, 13]. When primary repair is not possible, various types of capsulodesis and tenodesis have been utilized [4]. Dorsal intercarpal ligament capsulodesis has shown favorable clinical results at long term (average 7 years), although eight of 16 patients developed radiographic arthritis [6]. “Three-ligament tenodesis” has shown favorable clinical results at medium term (average 46 months), although nine of 38 patients developed radiographic arthritis [7]. Based on the literature, current surgical techniques can be recommended, although may not consistently prevent, delay, or mitigate the natural history of SLAC wrist [4, 6, 7, 10, 18].
The most relevant published study on combined surgery for distal radius fracture and scapholunate ligament tear found that fracture fixation with ligament repair or pinning demonstrated outcomes equivalent to historical controls without ligament instability (ruled out by fluoroscopic observation of scaphoid stability with wrist manipulation under anesthesia) [10]. However, that study had several limitations: 39 of 57 eligible patients did not participate, ligament treatment was heterogeneous (nine had direct repair, nine had pinning only), there were no untreated confirmed ligament tears for comparison, follow-up was relatively brief (minimum 12 months), and QuickDASH scores were suboptimal in both groups (27 with ligament procedure, 22 without) compared to prior studies of volar plating (average scores 4 or 5) [20, 23]. Thus, the authors assert, “we cannot state definitively that recognizing and treating scapholunate instability improves motion, grip, and comfort, or limits the potential for future arthrosis.” [10] However, they concluded that such treatment is “worthwhile in active patients,” which is compatible with the consensus supporting ligament surgery, as mentioned earlier.
Outcomes
Although the numbers of our groups I, II, and III are too small for meaningful analysis, we found general support for our treatments. At an average of 5 months postoperatively, QuickDASH scores were favorable and comparable in groups I and II, and none of these patients had further surgery. Both representative cases (Figs. 1 and 2) were doing well and had returned to baseline level of activity at the time of their respective radiographs. Of the five patients who underwent ligament repair (group III), four had long-term follow-up at an average of 5 years. Outcomes were good, including average QuickDASH score of 5 and average pain VAS of 1. None had further surgery. However, we noted worsening scapholunate gap (average 4.8 mm) and scapholunate angle (average 68°), suggesting that the ligament repair was not durable over time.
Limitations
A limitation of our study is the lack of a more definitive reference standard for evaluating occult ligament injuries, such as by arthrography, arthroscopy, or MRI. However, in support of our methods, one study found that arthroscopic grade 3 and 4 lesions, which are most relevant with regard to the potential need for repair, corresponded with radiographic gaps of 3–5 and 5–6 mm, respectively, and thus would be detected by our study protocol [8]. Similarly, a recent multicenter study of interobserver reliability using standard PA and lateral radiographs to detect scapholunate dissociation, with CT arthrography and operative confirmation as the reference standard, found a negative predictive value of 98 %, and thus concluded that radiographs were reliable for ruling out dissociation [9]. Another option may have been stress radiographs or fluoroscopy to assess for dynamic instability. However, clenched-fist radiographs are likely not tolerated or unreliable in the early period, and the intraoperative fluoroscopic “carpal stretch test” has been described as having only 78 % sensitivity for detecting grade 3 or 4 scapholunate ligament injuries [11]. Lastly, although occult injuries were undetected in our protocol (by definition), one study showed that the vast majority of such lesions (found to be radiographically normal, arthroscopically grade 1 or 2), without distal radius fracture, did not progress to worsening scapholunate gap, angle, or arthritis even at long term (average 7 years) [15].
Limited duration of follow-up may be a weakness with regard to group I, as progression of scapholunate instability may occur over a longer period than our average 6.2 months of follow-up. However, as just mentioned above, progression of an occult ligament injury to SLAC wrist is not inevitable even at long term [15]. Furthermore, studies have shown that a complete ligament tear may still be amenable to primary repair as late as 9 months (average 6 months) [18] or even 84 months (average 17 months) [13]; thus, surgical options would remain open after fracture repair. As outcomes of distal radius volar plating are nearly optimal by 3 to 6 months postoperatively [20, 23], future investigations might examine a staged approach, including immediate volar plating (with early motion), followed by delayed ligament repair or reconstruction (with requisite immobilization), long before SLAC wrist develops.
While the retrospective nature of our study allowed for selection bias regarding which patients were advised to have ligament repair (i.e., generally younger), this did not affect our conclusion that instability is uncommon, as all patients with or without ligament repair were counted. Contralateral wrist radiographs might have been helpful in suggesting generalized laxity, as a recent study of 124 contralateral asymptomatic wrists found a scapholunate gap ≥5 mm in 52 % and scapholunate angle ≥60° in 70 %, in accordance with prior studies [17]. Similarly, workup for gout or pseudogout might suggest etiology for scapholunate instability other than the acute injury, as discussed earlier [1, 3].
In summary, in our more representative population of distal radius fracture patients treated with volar locked plating, radiographic scapholunate instability appears to be uncommon, either from initial injury or after possible progression of occult ligament injury, despite early motion without operative treatment of the ligament. Thus, we did not find strong evidence for routinely delaying motion or pursuing further workup. When early radiographs clearly demonstrate scapholunate instability, and other causes are ruled out (e.g., generalized, senescent, crystalline-induced), surgical repair or reconstruction may be appropriate, particularly for selected patients (e.g., active, laborers, younger, larger gaps). Further investigations of natural history, surgical techniques, and long-term results are warranted.
References
Beck JD, Deegan JH, Riehl JT, Klena JC. Incidence of scapholunate ligament dissociation in patients with aspiration-confirmed gout. J Hand Surg [Am]. 2010;35(12):1938–42.
Bickert B, Sauerbier M, Germann G. Scapholunate ligament repair using the Mitek bone anchor. J Hand Surg (Br). 2000;25(2):188–92.
Chen C, Chandnani VP, Kang HS, Resnick D, Sartoris DJ, Haller J. Scapholunate advanced collapse: a common wrist abnormality in calcium pyrophosphate dihydrate crystal deposition disease. Radiology. 1990;177(2):459–61.
Chennagiri RJ, Lindau TR. Assessment of scapholunate instability and review of evidence for management in the absence of arthritis. J Hand Surg Eur Vol. 2013;38(7):727–38.
Forward DP, Lindau TR, Melsom DS. Intercarpal ligament injuries associated with fractures of the distal part of the radius. J Bone Joint Surg Am. 2007;89(11):2334–40.
Gajendran VK, Peterson B, Slater Jr RR, Szabo RM. Long-term outcomes of dorsal intercarpal ligament capsulodesis for chronic scapholunate dissociation. J Hand Surg [Am]. 2007;32(9):1323–33.
Garcia-Elias M, Lluch AL, Stanley JK. Three-ligament tenodesis for the treatment of scapholunate dissociation: indications and surgical technique. J Hand Surg [Am]. 2006;31(1):125–34.
Geissler WB, Freeland AE, Savoie FH, McIntyre LW, Whipple TL. Intracarpal soft-tissue lesions associated with an intra-articular fracture of the distal end of the radius. J Bone Joint Surg Am. 1996;78(3):357–65.
Gradl G, Neuhaus V, Fuchsberger T, Guitton TG, Prommersberger KJ, Ring D, et al. Radiographic diagnosis of scapholunate dissociation among intra-articular fractures of the distal radius: interobserver reliability. J Hand Surg [Am]. 2013;38(9):1685–90.
Gradl G, Pillukat T, Fuchsberger T, Knobe M, Ring D, Prommersberger KJ. The functional outcome of acute scapholunate ligament repair in patients with intra-articular distal radius fractures treated by internal fixation. Arch Orthop Trauma Surg. 2013;133(9):1281–7.
Kwon BC, Choi SJ, Song SY, Baek SH, Baek GH. Modified carpal stretch test as a screening test for detection of scapholunate interosseous ligament injuries associated with distal radial fractures. J Bone Joint Surg Am. 2011;93(9):855–62.
Larsen CF, Stigsby B, Lindequist S, Bellstrøm T, Mathiesen FK, Ipsen T. Observer variability in measurements of carpal bone angles on lateral wrist radiographs. J Hand Surg [Am]. 1991;16(5):893–8.
Lavernia CJ, Cohen MS, Taleisnik J. Treatment of scapholunate dissociation by ligamentous repair and capsulodesis. J Hand Surg [Am]. 1992;17(2):354–9.
Lindau T, Arner M, Hagberg L. Intra-articular lesions in distal fractures of the radius in young adults. A descriptive arthroscopic study in 50 patients. J Hand Surg (Br). 1997;22(5):638–43.
O’Meeghan CJ, Stuart W, Mamo V, Stanley JK, Trail IA. The natural history of an untreated isolated scapholunate interosseus ligament injury. J Hand Surg (Br). 2003;28(4):307–10.
Pappou IP, Basel J, Deal DN. Scapholunate ligament injuries: a review of current concepts. Hand. 2013;8(2):146–56.
Picha BM, Konstantakos EK, Gordon DA. Incidence of bilateral scapholunate dissociation in symptomatic and asymptomatic wrists. J Hand Surg [Am]. 2012;37(6):1130–5.
Pomerance J. Outcome after repair of the scapholunate interosseous ligament and dorsal capsulodesis for dynamic scapholunate instability due to trauma. J Hand Surg [Am]. 2006;31(8):1380–6.
Rosenthal DI, Schwartz M, Phillips WC, Jupiter J. Fracture of the radius with instability of the wrist. Am J Roentgenol. 1983;141(1):113–6.
Rozental TD, Blazar PE, Franko OI, Chacko AT, Earp BE, Day CS. Functional outcomes for unstable distal radial fractures treated with open reduction and internal fixation or closed reduction and percutaneous fixation. A prospective randomized trial. J Bone Joint Surg Am. 2009;91(8):1837–46.
Wadhwani A, Carey J, Propeck T, Hentzen P, Eustace S. Isolated scaphotrapeziotrapezoid osteoarthritis: a possible radiographic marker of chronic scapholunate ligament disruption. Clin Radiol. 1998;53(5):376–8.
Watson HK, Ballet FL. The SLAC wrist: scapholunate advanced collapse pattern of degenerative arthritis. J Hand Surg [Am]. 1984;9(3):358–65.
Wei DH, Raizman NM, Bottino CJ, Jobin CM, Strauch RJ, Rosenwasser MP. Unstable distal radial fractures treated with external fixation, a radial column plate, or a volar plate. A prospective randomized trial. J Bone Joint Surg Am. 2009;91(7):1568–77.
Weiss CB. Editorial reply: intercarpal ligament injuries associated with fractures of the distal part of the radius. J Bone Joint Surg Am. 2008;90A:1169–70.
Wright TW, Del Charco M, Wheeler D. Incidence of ligament lesions and associated degenerative changes in the elderly wrist. J Hand Surg [Am]. 1994;19(2):313–8.
Conflict of Interest
Virginia M. Jones declares that she has no conflict of interest.
Nathan G. Everding declares that he has no conflict of interest.
Jason M. Desmarais declares that he has no conflict of interest.
Maximillian C. Soong declares that he has no conflict of interest.
Statement of Human and Animal Rights
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008.
Statement of Informed Consent
Approval was obtained from the institutional review board regarding procedures to ensure protection of human rights and informed consent.
Author information
Authors and Affiliations
Corresponding author
Additional information
Investigation performed at: Lahey Clinic
About this article
Cite this article
Jones, V.M., Everding, N.G., Desmarais, J.M. et al. Scapholunate instability after distal radius volar plating. HAND 10, 678–682 (2015). https://doi.org/10.1007/s11552-015-9779-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11552-015-9779-2