Abstract
Purpose
To date, limited data exist about the relationship between radiation dose–volume parameters and patient-reported quality of life (QOL) after thoracic radiotherapy (RT) for lung cancer. We conducted this prospective study to investigate which clinico-dosimetric factors have an impact on functional declines and symptom developments after thoracic RT for lung cancer.
Materials and methods
The study included 44 patients who had underwent thoracic three-dimensional conformal RT at our institution from 2016 to 2017. The health-related QOL was assessed using the EORTC QLQ-C30 and QLQ-LC13 questionnaires before RT (preRT), at the end of RT (endRT), and 3, 6, and 12 months after the completion of RT. RT dose–volume parameters of adjacent normal organs such as the lung, heart, and esophagus were retrieved and used for regression analysis.
Results
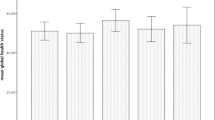
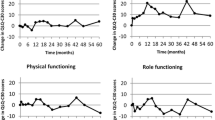
Thoracic RT induced a temporary deterioration of many of the functional statuses and symptoms, but most of those improved and recovered to baseline levels 3 months after RT. However, the role function (RF) decline persisted until 6 months after RT (p < 0.05). Dysphagia showed the most noticeable change at the endRT (p < 0.001). In the multiple regression analysis, the absolute volume of body received at least 50 Gy (p = 0.021) and a preRT RF score (p = 0.001) was significantly associated with the endRT RF scores. Dysphagia at the endRT was significantly associated with the V40 of the esophagus (p = 0.047), preRT emotional function (p = 0.029), and receipt of concurrent chemotherapy (p = 0.022).
Conclusions
Both the dosimetric parameters and preRT functional status have an impact on the weak aspect of patient-reported QOL, which may cause poor treatment compliance during and after thoracic RT. For patients with a low preRT QOL score or those having large tumor which may result in higher dose volumes, careful RT planning could prevent the deterioration of QOL after RT.


Similar content being viewed by others
References
Movsas B, Moughan J, Sarna L et al (2009) Quality of life supersedes the classic prognosticators for long-term survival in locally advanced non-small-cell lung cancer: an analysis of RTOG 9801. J Clin Oncol 27:5816–5822. https://doi.org/10.1200/JCO.2009.23.7420
Hallqvist A, Bergman B, Nyman J (2012) Health related quality of life in locally advanced NSCLC treated with high dose radiotherapy and concurrent chemotherapy or cetuximab–pooled results from two prospective clinical trials. Radiother Oncol 104:39–44. https://doi.org/10.1016/j.radonc.2012.05.006
Aaronson NK, Ahmedzai S, Bergman B et al (1993) The European Organization for Research and Treatment of Cancer QLQ-C30: a quality-of-life instrument for use in international clinical trials in oncology. J Natl Cancer Inst 85:365–376. https://doi.org/10.1093/jnci/85.5.365
Yun YH, Park YS, Lee ES et al (2004) Validation of the Korean version of the EORTC QLQ-C30. Qual Life Res 13:863–868. https://doi.org/10.1023/B:QURE.0000021692.81214.70
Bergman B, Aaronson NK, Ahmedzai S et al (1994) The EORTC QLQ-LC13: a modular supplement to the EORTC Core Quality of Life Questionnaire (QLQ-C30) for use in lung cancer clinical trials. EORTC Study Group on Quality of Life. Eur J Cancer 30A:635–642. https://doi.org/10.1016/0959-8049(94)90535-5
Gomez DR, Tang C, Zhang J et al (2019) Local consolidative therapy vs. maintenance therapy or observation for patients with oligometastatic non-small-cell lung cancer: long-term results of a multi-institutional, phase II, randomized study. J Clin Oncol. https://doi.org/10.1200/JCO.19.00201
Suh Y-G, Cho J (2019) Local ablative radiotherapy for oligometastatic non-small cell lung cancer. Radiat Oncol J 37:149–155. https://doi.org/10.3857/roj.2019.00514
Yun YH, Kim YA, Min YH et al (2012) Health-related quality of life in disease-free survivors of surgically treated lung cancer compared with the general population. Ann Surg 255:1000–1007. https://doi.org/10.1097/SLA.0b013e31824f1e9e
Pijls-Johannesma M, Houben R, Boersma L et al (2009) High-dose radiotherapy or concurrent chemo-radiation in lung cancer patients only induces a temporary, reversible decline in QoL. Radiother Oncol 91:443–448. https://doi.org/10.1016/j.radonc.2009.02.010
Vogel J, Wang X, Troxel AB et al (2019) Prospective assessment of demographic characteristics associated with worse health related quality of life measures following definitive chemoradiation in patients with locally advanced non-small cell lung cancer. Transl Lung Cancer Res 8:332–339. https://doi.org/10.21037/tlcr.2019.08.21
Fayers PM, Aaronson NK, Bjordal K, Groenvold M, Curran D, Bottomley A (2001) The EORTC QLQ-C30 Scoring Manual (3rd Edition). European Organisation for Research and Treatment of Cancer, Brussels
Wintner LM, Giesinger JM, Zabernigg A et al (2013) Quality of life during chemotherapy in lung cancer patients: results across different treatment lines. Br J Cancer 109:2301–2308. https://doi.org/10.1038/bjc.2013.585
Nguyen PAH, Vercauter P, Verbeke L et al (2019) Health outcomes for definite concurrent chemoradiation in locally advanced non-small cell lung cancer: a prospective study. Respir Int Rev Thorac Dis 97:310–318. https://doi.org/10.1159/000493984
Yucel B, Akkaş EA, Okur Y et al (2014) The impact of radiotherapy on quality of life for cancer patients: a longitudinal study. Support Care Cancer 22:2479–2487. https://doi.org/10.1007/s00520-014-2235-y
Eslick GD, Talley NJ (2008) Dysphagia: epidemiology, risk factors and impact on quality of life—a population-based study. Aliment Pharmacol Ther 27:971–979. https://doi.org/10.1111/j.1365-2036.2008.03664.x
Nguyen NP, Frank C, Moltz CC et al (2005) Impact of dysphagia on quality of life after treatment of head-and-neck cancer. Int J Radiat Oncol Biol Phys 61:772–778. https://doi.org/10.1016/j.ijrobp.2004.06.017
Mulugeta A, Zhou A, King C, Hyppönen E (2019) Association between major depressive disorder and multiple disease outcomes: a phenome-wide Mendelian randomisation study in the UK Biobank. Mol Psychiatry. https://doi.org/10.1038/s41380-019-0486-1
Nakamura Y, Momoki C, Okada G et al (2019) Preoperative depressive mood of patients with esophageal cancer might delay recovery from operation-related malnutrition. J Clin Med Res 11:188–195. https://doi.org/10.14740/jocmr3704
Baudry A-S, Anota A, Mariette C et al (2019) The role of trait emotional intelligence in quality of life, anxiety and depression symptoms after surgery for esophageal or gastric cancer: a French national database FREGAT. Psychooncology 28:799–806. https://doi.org/10.1002/pon.5023
Acknowledgements
The authors would like to thank Jisoo Shin for assistance in collecting the questionnaires answered by the patients.
Funding
The research for this manuscript was not financially supported and none of the authors had any relevant financial relationships.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that no actual or potential conflict of interest exists.
Informed consent
This study was approved by our Institutional Review Board (No. 16-2016-10), and all patients were well informed of the study protocol and had provided their written informed consent prior to treatment.
Research involving human participants and/or animals
This article does not contain any studies with animals performed by any of the authors.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the Institutional and/or National Research Committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kim, B.H., Kim, JS., Kim, K.H. et al. Clinical significance of radiation dose–volume parameters and functional status on the patient-reported quality of life changes after thoracic radiotherapy for lung cancer: a prospective study. Radiol med 126, 466–473 (2021). https://doi.org/10.1007/s11547-020-01273-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-020-01273-0