Abstract
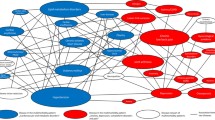
The detailed comorbidity patterns of community-dwelling older adults have not yet been explored. This study employed a network-based approach to investigate the comorbidity patterns of community-dwelling older adults living alone. The sample comprised a cross-sectional cohort of adults 65 or older living alone in a Korean city (n = 1041; mean age = 77.7 years, 77.6% women). A comorbidity network analysis that estimates networks aggregated from measures of significant co-occurrence between pairs of diseases was employed to investigate comorbid associations between 31 chronic conditions. A cluster detection algorithm was employed to identify specific clusters of comorbidities. The association strength was expressed as the observed-to-expected ratio (OER). As a result, fifteen diseases were interconnected within the network (OER > 1, p-value < .05). While hypertension had a high prevalence, osteoporosis was the most central disease, co-occurring with numerous other diseases. The strongest associations among comorbidities were found between thyroid disease and urinary incontinence, chronic otitis media and osteoporosis, gastric duodenal ulcer/gastritis and anemia, and depression and gastric duodenal ulcer/gastritis (OER > 1.85). Three distinct clusters were identified as follows: (a) cataracts, osteoporosis, chronic otitis media, osteoarthritis/rheumatism, low back pain/sciatica, urinary incontinence, post-accident sequelae, and thyroid diseases; (b) hyperlipidemia, diabetes mellitus, and hypertension; and (c) depression, skin disease, gastric duodenal ulcer/gastritis, and anemia. The results may prove valuable in guiding the early diagnosis, management, and treatment of comorbidities in older adults living alone.


Similar content being viewed by others
Data availability
The datasets used and analyzed during the current study are available from the corresponding author on reasonable request.
References
Nguyen H, Manolova G, Daskalopoulou C, Vitoratou S, Prince M, Prina AM. Prevalence of multimorbidity in community settings: a systematic review and meta-analysis of observational studies. J Comorbidity. 2019;9:2235042X19870934.
Gijsen R, Hoeymans N, Schellevis FG, Ruwaard D, Satariano WA, van den Bos GA. Causes and consequences of comorbidity: a review. J Clin Epidemiol. 2001;54(7):661–74.
Jindai K, Nielson CM, Vorderstrasse BA, Quiñones AR. Multimorbidity and functional limitations among adults 65 or older, NHANES 2005–2012. Prev Chronic Dis. 2016;13:E151.
Kim CH, Hwang I, Yoo WS. The common patterns of multimorbidity and its impact on healthcare cost in Korea. Health Policy Manag. 2014;24(3):219–27.
Picco L, Achilla E, Abdin E, Chong SA, Vaingankar JA, McCrone P, ... & Subramaniam M. Economic burden of multimorbidity among older adults: impact on healthcare and societal costs. BMC Health Serv Res. 2016;16:1–12.
Brunson JC, Agresta TP, Laubenbacher RC. Sensitivity of comorbidity network analysis. JAMIA Open. 2020;3(1):94–103.
Hidalgo CA, Blumm N, Barabási AL, Christakis NA. A dynamic network approach for the study of human phenotypes. PLoS Comput Biol. 2009;5(4):e1000353.
Fotouhi B, Momeni N, Riolo MA, Buckeridge DL. Statistical methods for constructing disease comorbidity networks from longitudinal inpatient data. Appl Netw Sci. 2018;3:1–34.
Borsboom D, Cramer AO. Network analysis: an integrative approach to the structure of psychopathology. Annu Rev Clin Psychol. 2013;9:91–121.
Guloksuz S, Pries LK, Van Os J. Application of network methods for understanding mental disorders: pitfalls and promise. Psychol Med. 2017;47(16):2743–52.
Capobianco E, Liò P. Comorbidity networks: beyond disease correlations. J Complex Netw. 2015;3(3):319–32.
Frank ES, Tripathi S, de Matos SR, Hawwa AF, Dehmer M. The human disease network. Syst Biomed. 2013;1(1):20–8.
Brunson JC, Laubenbacher RC. Applications of network analysis to routinely collected health care data: a systematic review. J Am Med Inform Assoc. 2018;25(2):210–21.
Qiu H, Wang L, Zeng X, Pan J. Comorbidity patterns in depression: a disease network analysis using regional hospital discharge records. J Affect Disord. 2022;296:418–27.
Zhou D, Wang L, Ding S, Shen M, Qiu H. Phenotypic disease network analysis to identify comorbidity patterns in hospitalized patients with ischemic heart disease using large-scale administrative data. Healthcare. 2022;10(1):80.
Ljubic B, Pavlovski M, Alshehri J, Roychoudhury S, Bajic V, Van Neste C, Obradovic Z. Comorbidity network analysis and genetics of colorectal cancer. Inform Med Unlocked. 2020;21:100492.
Ko H, Park YH, Cho B, Lim KC, Chang SJ, Yi YM, ... & Ryu SI. Gender differences in health status, quality of life, and community service needs of older adults living alone. Arch Gerontol Geriatr. 2019;83:239–45.
Statistics Korea. Statistics for the elderly. [Internet]. 2022. Available from: https://kostat.go.kr/portal/korea/kor_nw/1/1/index.board?bmode=read&aSeq=420896. Accessed 25 Sept 2023
Park B, Lee HA, Park H. Use of latent class analysis to identify multimorbidity patterns and associated factors in Korean adults aged 50 years and older. PLoS ONE. 2019;14(11):e0216259.
Shin J, Lee KS, Kim JH. Predicting old-age mortality using principal component analysis: results from a National Panel Survey in Korea. Medicina. 2020;56(7):360.
Cramer AO, Waldorp LJ, Van Der Maas HL, Borsboom D. Comorbidity: a network perspective. Behav Brain Sci. 2010;33(2–3):137–50.
Morris JN, Fries BE, Steel K, Ikegami N, Bernabei R, Carpenter GI, ... & Topinková E. Comprehensive clinical assessment in community setting: applicability of the MDS‐HC. J Am Geriatr Soc. 1997;45(8):1017–24.
Korea Institute for Health and Social Affairs. 2017 national survey of older Koreans. Sejong, South Korea: Author; 2017.
Park J, Lee DS, Christakis NA, Barabási AL. The impact of cellular networks on disease comorbidity. Mol Syst Biol. 2009;5(1):262.
Jeong E, Ko K, Oh S, Han HW. Network-based analysis of diagnosis progression patterns using claims data. Sci Rep. 2017;7(1):15561.
Hevey D. Network analysis: a brief overview and tutorial. Health Psychol Behav Med. 2018;6(1):301–28.
Wang TC, Lin CC, Lin CD, Chung HK, Wang CY, Tsai MH, Kao CH. Increased acquired cholesteatoma risk in patients with osteoporosis: a retrospective cohort study. PLoS ONE. 2015;10(7):e0132447.
Liao PS, Chiu CC, Fu YH, Hsia CC, Yang YC, Lee KF, ... & Kuo SJ. Incidence of hip fractures among patients with chronic otitis media: The Real-World Data. Medicina (Kaunas). 2022;58(8):1138.
Segade F, Daly KA, Allred D, Hicks PJ, Cox M, Brown M, ... & Bowden DW. Association of the FBXO11 gene with chronic otitis media with effusion and recurrent otitis media: the Minnesota COME/ROM Family Study. Arch Otolaryngol Head Neck Surg. 2006;132(7):729–33.
Rye MS, Wiertsema SP, Scaman ESH, Oommen J, Sun W, Francis RW, ... & Jamieson SE. FBXO11, a regulator of the TGFβ pathway, is associated with severe otitis media in Western Australian children. Genes Immun. 2011;12(5):352–59.
Wang X, Kua HY, Hu Y, Guo K, Zeng Q, Wu Q, ... & Li B. p53 functions as a negative regulator of osteoblastogenesis, osteoblast-dependent osteoclastogenesis, and bone remodeling. J Cell Biol. 2006;172(1):115–25.
Sran M, Mercier J, Wilson P, Lieblich P, Dumoulin C. Physical therapy for urinary incontinence in postmenopausal women with osteoporosis or low bone density: a randomized controlled trial. Menopause. 2016;23(3):286–93.
Berecki-Gisolf J, Spallek M, Hockey R, Dobson A. Height loss in elderly women is preceded by osteoporosis and is associated with digestive problems and urinary incontinence. Osteoporos Int. 2010;21(3):479–85.
Sran MM. Prevalence of urinary incontinence in women with osteoporosis. J Obstet Gynaecol Can. 2009;31(5):434–9.
Wei MC, Chou YH, Yang YS, Kornelius E, Wang YH, Huang CN. Osteoporosis and stress urinary incontinence in women: a National Health Insurance Database study. Int J Environ Res Public Health. 2020;17(12):4449.
Huang HK, Lin SM, Loh CH, Wang JH, Liang CC. Association between cataract and risks of osteoporosis and fracture: a nationwide cohort study. J Am Geriatr Soc. 2019;67(2):254–60.
Nemet AY, Hanhart J, Kaiserman I, Vinker S. Are cataracts associated with osteoporosis? Clin Ophthalmol. 2013;7:2079.
Chung SD, Chen YK, Chen YH, Lin HC. Hyperthyroidism and female urinary incontinence: a population-based cohort study. Clin Endocrinol. 2011;75(5):704–8.
Zargham M, Hajian MR, Alizadeh F, Eslami MJ, Khalili Boroujeni N, Gholipour F. Hypothyroidism is prevalent among adult women with chronic lower urinary tract symptoms. LUTS. 2022;14(4):248–54.
Cavalcoli F, Zilli A, Conte D, Massironi S. Micronutrient deficiencies in patients with chronic atrophic autoimmune gastritis: a review. World J Gastroenterol. 2017;23(4):563–72.
Brown ES, Varghese FP, McEwen BS. Association of depression with medical illness: does cortisol play a role? Biol Psychiatry. 2004;55(1):1–9.
Goodwin RD, Keyes KM, Stein MB, Talley NJ. Peptic ulcer and mental disorders among adults in the community: the role of nicotine and alcohol use disorders. Psychosom Med. 2009;71(4):463–8.
Stek ML, Vinkers DJ, Gussekloo J, Beekman AT, Van Der Mast RC, Westendorp RG. Is depression in old age fatal only when people feel lonely? Am J Psychiatry. 2005;162(1):178–80.
Scott KM, Alonso J, De Jonge P, Viana MC, Liu Z, O'Neill S, ... & Kessler RC. Associations between DSM-IV mental disorders and onset of self-reported peptic ulcer in the World Mental Health Surveys. J Psychosom Res. 2013;75(2):121–7.
Fang B, Liu H, Yang S, Xu R, Chen G. Impact of social isolation on subsequent peptic ulcer recurrence in older adults with mild cognitive impairment: the role of change in severity of depression. Psychosom Med. 2020;82(2):197–207.
Cho YJ, Jung TH, Jin HM, Kim JH, Kim DY, Kim SJ. Relationship between depression and endoscopic erosive gastritis in men and women aged over 40 years. Korean J Fam Pract. 2017;7(5):681–7.
Funding
This work was supported by a grant from the Korea Health Technology R&D Project through the Korea Health Industry Development Institute (KHDI), funded by the Ministry of Health & Welfare, Republic of Korea (grant number: HI18C1284).
Author information
Authors and Affiliations
Contributions
Conceptualization: CL, YHP; methodology: HAL, CL; formal analysis and investigation: CL; writing—original draft preparation: CL; writing—review and editing: YHP, BC, HAL; funding acquisition: BC, YHP; supervision: YHP, BC.
Corresponding author
Ethics declarations
Ethics approval
The original research project, “Development of a community-based integrated service model for older adults living alone,” was approved by the Seoul National University Hospital Institutional Review Board (approval no. H-1807–131–961). All participants gave written informed consent prior to enrollment to the study and were informed that they could withdraw their consent at any time during the study without any justification. For the present secondary data analysis, we obtained approval from the Seoul National University Institutional Review Board.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
About this article
Cite this article
Lee, C., Park, YH., Cho, B. et al. A network-based approach to explore comorbidity patterns among community-dwelling older adults living alone. GeroScience 46, 2253–2264 (2024). https://doi.org/10.1007/s11357-023-00987-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11357-023-00987-z