Abstract
Objective
This study aimed to investigate the association between each parameter of intermittent hypoxia in obstructive sleep apnea (OSA) and the cognitive profile, cortical thickness, and white matter integrity in middle-aged and older adults.
Methodology
Participants were newly diagnosed with moderate or severe OSA from the King Chulalongkorn Memorial Hospital, Bangkok, Thailand. Respiratory parameters from polysomnography were extracted. Each participant was tested on a battery of neuropsychological tests and underwent an MRI scan of the brain. Cortical thickness analysis and diffusion tensor imaging analysis were performed. Participants were classified as having either severe or mild hypoxia based on parameters of hypoxia, i.e., oxygen desaturation index, lowest oxygen saturation, and the percentage of total sleep time spent below 90% oxygen saturation.
Results
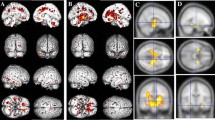
Of 17 patients with OSA, there were 8 men (47%). Median age was 57 years and median AHI was 60.6. Comparison of cortical thickness between the severe and the mild group of each hypoxic parameter revealed two clusters of cortical thinning at the right inferior frontal gyrus (p-value = 0.008) and right inferior parietal gyrus (p-value = 0.006) in the severe desaturation group and a cluster of cortical thinning at the superior parietal gyrus (p-value = 0.008) in the high oxygen desaturation index group. There was no difference in cognitive function or white matter integrity between groups.
Conclusions
The magnitude of the degree and frequency of desaturations in OSA are associated with a decrease in cortical thickness at the frontal and parietal regions.


Similar content being viewed by others
References
Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328(17):1230–1235. https://doi.org/10.1056/NEJM199304293281704
Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, Hla KM (2013) Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol 177(9):1006–1014
Bucks RS, Olaithe M, Rosenzweig I, Morrell MJ (2017) Reviewing the relationship between OSA and cognition: where do we go from here? Respirology 22(7):1253–1261. https://doi.org/10.1111/resp.13140
Beebe DW, Groesz L, Wells C, Nichols A, McGee K (2003) The neuropsychological effects of obstructive sleep apnea: a meta-analysis of norm-referenced and case-controlled data. Sleep 26(3):298–307
Jordan AS, McSharry DG, Malhotra A (2014) Adult obstructive sleep apnoea. Lancet 383(9918):736–747. https://doi.org/10.1016/S0140-6736(13)60734-5
Ferini-Strambi L, Baietto C, Di Gioia MR, Castaldi P, Castronovo C, Zucconi M, Cappa SF (2003) Cognitive dysfunction in patients with obstructive sleep apnea (OSA): partial reversibility after continuous positive airway pressure (CPAP). Brain Res Bull 61(1):87–92
Spira AP, Blackwell T, Stone KL, Redline S, Cauley JA, Ancoli-Israel S, Yaffe K (2008) Sleep-disordered breathing and cognition in older women. J Am Geriatr Soc 56(1):45–50. https://doi.org/10.1111/j.1532-5415.2007.01506.x
Ju G, Yoon IY, Lee SD, Kim TH, Choe JY, Kim KW (2012) Effects of sleep apnea syndrome on delayed memory and executive function in elderly adults. J Am Geriatr Soc 60(6):1099–1103. https://doi.org/10.1111/j.1532-5415.2012.03961.x
Joo EY, Jeon S, Kim ST, Lee JM, Hong SB (2013) Localized cortical thinning in patients with obstructive sleep apnea syndrome. Sleep 36(8):1153–1162. https://doi.org/10.5665/sleep.2876
Macey PM, Kumar R, Woo MA, Valladares EM, Yan-Go FL, Harper RM (2008) Brain structural changes in obstructive sleep apnea. Sleep 31(7):967–977
Kumar R, Chavez AS, Macey PM, Woo MA, Yan-Go FL, Harper RM (2012) Altered global and regional brain mean diffusivity in patients with obstructive sleep apnea. J Neurosci Res 90(10):2043–2052. https://doi.org/10.1002/jnr.23083
Delis DC KE, Kramer JH (2001) Delis-Kaplan Executive Function System: Technical Manual. Harcourt Assessment Company, San Antonio, TX
D W (2008) Wechsler Adult Intelligence Scale-Fourth Edition. Fourth Edition edn, Pearson, San Antonio, TX
D W (2009) Wechsler Memory Scale-Fourth Edition. Fourth Edition edn. Pearson, San Antonio, TX
Fischl B (2012) FreeSurfer. Neuroimage 62(2):774–781. https://doi.org/10.1016/j.neuroimage.2012.01.021
Jenkinson M, Beckmann CF, Behrens TE, Woolrich MW, Smith SM (2012) Fsl. Neuroimage 62(2):782–790. https://doi.org/10.1016/j.neuroimage.2011.09.015
Smith SM, Jenkinson M, Johansen-Berg H, Rueckert D, Nichols TE, Mackay CE, Watkins KE, Ciccarelli O, Cader MZ, Matthews PM, Behrens TE (2006) Tract-based spatial statistics: voxelwise analysis of multi-subject diffusion data. Neuroimage 31(4):1487–1505. https://doi.org/10.1016/j.neuroimage.2006.02.024
FreeSurfer Qdec. https://surfer.nmr.mgh.harvard.edu/fswiki/Qdec.
Cross NE, Memarian N, Duffy SL, Paquola C, LaMonica H, D'Rozario A, Lewis SJG, Hickie IB, Grunstein RR, Naismith SL (2018) Structural brain correlates of obstructive sleep apnoea in older adults at risk for dementia. Eur Respir J 52(1):1800740. https://doi.org/10.1183/13993003.00740-2018
Baril AA, Gagnon K, Brayet P, Montplaisir J, De Beaumont L, Carrier J, Lafond C, L'Heureux F, Gagnon JF, Gosselin N (2017) Gray matter hypertrophy and thickening with obstructive sleep apnea in middle-aged and older adults. Am J Respir Crit Care Med 195(11):1509–1518. https://doi.org/10.1164/rccm.201606-1271OC
Dewan NA, Nieto FJ, Somers VK (2015) Intermittent hypoxemia and OSA: implications for comorbidities. Chest 147(1):266–274. https://doi.org/10.1378/chest.14-0500
Harper RM, Kumar R, Macey PM, Woo MA, Ogren JA (2014) Affective brain areas and sleep-disordered breathing. Prog Brain Res 209:275–293. https://doi.org/10.1016/B978-0-444-63274-6.00014-X
Owen JE, BenediktsdOttir B, Gislason T, Robinson SR (2019) Neuropathological investigation of cell layer thickness and myelination in the hippocampus of people with obstructive sleep apnea. Sleep 42(1):1–13. https://doi.org/10.1093/sleep/zsy199
Park DC, Reuter-Lorenz P (2009) The adaptive brain: aging and neurocognitive scaffolding. Annu Rev Psychol 60:173–196. https://doi.org/10.1146/annurev.psych.59.103006.093656
Sharma H, Sharma SK, Kadhiravan T, Mehta M, Sreenivas V, Gulati V, Sinha S (2010) Pattern & correlates of neurocognitive dysfunction in Asian Indian adults with severe obstructive sleep apnoea. Indian J Med Res 132:409–414
Mathieu A, Mazza S, Decary A, Massicotte-Marquez J, Petit D, Gosselin N, Malo J, Montplaisir J (2008) Effects of obstructive sleep apnea on cognitive function: a comparison between younger and older OSAS patients. Sleep Med 9(2):112–120. https://doi.org/10.1016/j.sleep.2007.03.014
Hoth KF, Zimmerman ME, Meschede KA, Arnedt JT, Aloia MS (2013) Obstructive sleep apnea: impact of hypoxemia on memory. Sleep Breath 17(2):811–817. https://doi.org/10.1007/s11325-012-0769-0
Macey PM, Henderson LA, Macey KE, Alger JR, Frysinger RC, Woo MA, Harper RK, Yan-Go FL, Harper RM (2002) Brain morphology associated with obstructive sleep apnea. Am J Respir Crit Care Med 166(10):1382–1387. https://doi.org/10.1164/rccm.200201-050OC
Wang D, Thomas RJ, Yee BJ (1985) Grunstein RR (2016) Hypercapnia is more important than hypoxia in the neuro-outcomes of sleep-disordered breathing. J Appl Physiol 120(12):1484. https://doi.org/10.1152/japplphysiol.01008.2015
Kung SC, Shen YC, Chang ET, Hong YL, Wang LY (2018) Hypercapnia impaired cognitive and memory functions in obese patients with obstructive sleep apnoea. Sci Rep 8(1):17551. https://doi.org/10.1038/s41598-018-35797-3
Funding
This study was funded by Ratchadapisek Sompotch Endowment Fund, Faculty of Medicine, Chulalongkorn University, Grant No. RA 62/065.
Author information
Authors and Affiliations
Contributions
Conception and design of the study: A.C., N.C., Y.L., K.P.
Acquisition and analysis of the data: A.C., N.C., N.J., N.P., Y.S., C.C.
Drafting and revision of the manuscript: A.C., N.C., Y.L.
All authors reviewed and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they do not have any financial or non-financial potential conflicts of interest.
Ethics approval
All procedures performed in this study were in accordance with the ethical standards of the Faculty of Medicine, Chulalongkorn University Institutional Review Board, and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Data and code availability
Not applicable.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(PDF 580 kb)
Rights and permissions
About this article
Cite this article
Chokesuwattanaskul, A., Chirakalwasan, N., Jaimchariyatam, N. et al. Associations between hypoxia parameters in obstructive sleep apnea and cognition, cortical thickness, and white matter integrity in middle-aged and older adults. Sleep Breath 25, 1559–1570 (2021). https://doi.org/10.1007/s11325-020-02215-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-020-02215-w