Abstract
Introduction
The application of metabolomic analysis in the pediatric nephrology field may offer an innovative approach to profile analysis of renal diseases.
Objective
We aimed to analyze the salivary the major metabolites in the saliva of children and adolescents with chronic kidney disease (CKD) before and after hemodialysis.
Method
Thirty-six children diagnosed with CKD and forty healthy children were recruited for the study. 1H-NMR spectra were analyzed using multivariate and univariate approaches.
Results
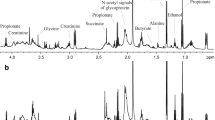
The CKD and the healthy control groups presented with similar numbers of dental caries (p > 0.05) as determined by the number of decayed, missing, or filled deciduous teeth (0.87 ± 2.2 and 0.67 ± 2.1, respectively) or permanent teeth (0.79 ± 1.30 and 0.90 ± 1.7, respectively). The amount of dental calculus was significantly higher in the CKD group than in the healthy control group (p < 0.001). Multivariate analyses using PLS-DA and O-PLS-DA demonstrated differences in the salivary metabolome of CKD patients before and after hemodialysis, as well as between post-dialysis CKD patients and healthy controls, suggesting that HD was not able to recover oral homeostasis. PLS-DA and OPLS-DA models showed satisfactory accuracy (ACC = 0.72) and prediction (0.64). On multivariate and univariate analyses, urea, acetate, ethanol, and fatty acid were significantly decreased in CKD saliva after hemodialysis. By contrast, saliva from the healthy controls had significantly higher levels of acetate and propionate and lower levels of ethanol, lactate, butyrate, phenylalanine, and creatinine than saliva from post-dialysis CKD patients.
Conclusion
Our results demonstrate that hemodialysis alters the expression of salivary metabolites; however, this alteration does not reestablish the healthy salivary metabolome, as the salivary metabolomic profile of healthy children is significantly different from that of children and adolescents with CKD, both before and after hemodialysis. The unique salivary characteristics of children with CKD may influence their oral health status.



Similar content being viewed by others
Abbreviations
- CKD:
-
Chronic kidney disease
- CRR:
-
Creatinine reduction rate
- CPMG:
-
Carr-Purcell-Meiboom-Gill
- dmft:
-
Decayed, missing, or filled deciduous teeth
- DMFT:
-
Decayed, missing, or filled permenant teeth
- HD:
-
Hemodialysis
- HD-A:
-
After hemodialysis
- HD-B:
-
Before hemodialysis
- NMR:
-
Nuclear magnetic resonance
- O-PLS-DA:
-
Orthogonal partial least squares discriminant analysis
- PLS-DA:
-
Partial least squares discriminant analysis
- TOCSY:
-
Total correlation spectroscopy
- URR:
-
Urea reduction rate
- VIP:
-
Variable importance in projection
References
Aimetti, M., Cacciatore, S., Graziano, A., & Tenori, L. (2012). Metabonomic analysis of saliva reveals generalized chronic periodontitis signature. Metabolomics, 8(3), 465–474.
Arregger, A. L., Cardoso, E. M., Tumilasci, O., & Contreras, L. N. (2008). Diagnostic value of salivary cortisol in end stage renal disease. Steroids, 73(1), 77–82.
Benmoussa, L., Renoux, M., & Radoi, L. (2015). Oral manifestations of chronic renal failure complicating a systemic genetic disease: Diagnostic dilemma. Case report and literature review. Journal of Oral and Maxillofacial Surgery. doi:10.1016/j.joms.2015.05.029
de Oliveira, L. R., Martins, C., Fidalgo, T. K., Freitas-Fernandes, L. B., de Oliveira Torres, R., Soares, A. L., Almeida, F. C., Valente, A. P., & de Souza, I. P. (2016). Salivary metabolite fingerprint of type 1 diabetes in young children. Journal of Proteome Research, 15(8), 2491–2499.
Desai, A. A., Nissenson, A., Chertow, G. M., Farid, M., Singh, I., Van Oijen, M. G., Esrailian, E., Solomon, M. D., & Spiegel, B. M. (2009). The relationship between laboratory-based outcome measures and mortality in end-stage renal disease: A systematic review. Hemodialysis International: International Symposium on Home Hemodialysis, 13(3), 347–359.
Driessens, F. C. M., Borggreven, J. M. P. M., Verbeeck, R. M. H., van Dijk, J. W. E., & Feagin, F. F. (1985). On the physicochemistry of plaque calcification and the phase composition of dental calculus. Journal Periodontal Research, 20, 329–336.
Epstein, S. R., Mandel, I., & Scopp, I. W. (1980). Salivary composition and calculus formation in patients undergoing hemodialysis. Journal of Periodontology, 51(6), 336–338.
Fidalgo, T. K. S., Freitas-Fernandes, L. B., Almeida, F. L., Valente, A. P., & Souza, I. P. R. (2015). Longitudinal evaluation of salivary profile from children with dental caries before and after treatment. Metabolomics, 11(3), 780–785.
Fidalgo, T. K. S., Freitas-Fernandes, L. B., Angeli, R., Muniz, A. M. S., Gonsalves, E., Santos, R., Almeida, F. L., Valente, A. P., & Souza, I. P. R. (2013). Salivary metabolite signatures of children with and without dental caries lesions. Metabolomics, 9(3), 657–666.
Fujiwara, M., Ando, I., Takeuchi, K., Oguma, S., Sato, H., Sekino, H., Sato, K., & Imai, Y. (2015). Metabolic responses during hemodialysis determined by quantitative (1)H NMR spectroscopy. Journal of Pharmaceutical and Biomedical Analysis, 111, 159–162.
Fujiwara, M., Kobayashi, T., Jomori, T., Maruyama, Y., Oka, Y., Sekino, H., Imai, Y., & Takeuchi, K. (2009). Pattern recognition analysis for 1H NMR spectra of plasma from hemodialysis patients. Analytical and Bioanalytical Chemistry, 394(6), 1655–1660.
Gray, L. R., Tompkins, S. C., & Taylor, E. B. (2014). Regulation of pyruvate metabolism and human disease. Cellular and Molecular Life Sciences: CMLS, 71(14), 2577–2604.
Gupta, M., Gupta, M., & Abhishek (2015). Oral conditions in renal disorders and treatment considerations: A review for pediatric dentist. Saudi Dental Journal, 27(3), 113–119.
Hocher, B., & Adamski, J. (2017). Metabolomics for clinical use and research in chronic kidney disease. Nature Reviews: Nephrology, 13(5), 269–284.
Huang, C. B., Alimova, Y., Myers, T. M., & Ebersole, J. L. (2011). Short- and medium-chain fatty acids exhibit antimicrobial activity for oral microorganisms. Archives of Oral Biology, 56(7), 650–654.
Jankowski, J., Hagemann, J., Yoon, M. S., van der Giet, M., Stephan, N., Zidek, W., Schluter, H., & Tepel, M. (2001). Increased vascular growth in hemodialysis patients induced by platelet-derived diadenosine polyphosphates. Kidney International, 59(3), 1134–1141.
Kaysen, G. A. (2007). Dialysis removes apolipoprotein c-i, improving very low-density lipoprotein clearance. Kidney International, 72(7), 779–781.
Klassen, J. T., & Krasko, B. M. (2002). The dental health status of dialysis patients. Journal of the Canadian Dental Association, 68(1), 34–38.
Lindon, J. C., Holmes, E., Bollard, M. E., Stanley, E. G., & Nicholson, J. K. (2004). Metabonomics technologies and their applications in physiological monitoring, drug safety assessment and disease diagnosis. Biomarkers: Biochemical Indicators of Exposure, Response, and Susceptibility to Chemicals, 9(1), 1–31.
Liu, J., & Duan, Y. (2012). Saliva: a potential media for disease diagnostics and monitoring. Oral Oncology, 48(7), 569–577.
Manhold, J. H., Volpe, A. R., Parker, L., & Adams, S. H. (1965). In vivo calculus assessment. Ii. A comparison of scoring techniques. Journal of Periodontology, 36, 299–304.
Martins, C., Siqueira, W. L., & Guimaraes Primo, L. S. (2008). Oral and salivary flow characteristics of a group of brazilian children and adolescents with chronic renal failure. Pediatric Nephrology, 23(4), 619–624.
Martins, C., Siqueira, W. L., Oliveira, E., Nicolau, J., & Primo, L. G. (2012). Dental calculus formation in children and adolescents undergoing hemodialysis. Pediatric nephrology, 27(10), 1961–1966.
Moco, S., Collino, S., Rezzi, S., & Martin, F. P. (2013). Metabolomics perspectives in pediatric research. Pediatric Research, 73(4 Pt 2), 570–576.
Nicholson, J. K., & Lindon, J. C. (2008). Systems biology: Metabonomics. Nature, 455(7216), 1054–1056.
Peterson, S., Woodhead, J., & Crall, J. (1985). Caries resistance in children with chronic renal failure: Plaque ph, salivary ph, and salivary composition. Pediatric Research, 19(8), 796–799.
Ramadan, Z., Jacobs, D., Grigorov, M., & Kochhar, S. (2006). Metabolic profiling using principal component analysis, discriminant partial least squares, and genetic algorithms. Talanta, 68(5), 1683–1691.
Seethalakshmi, C., Koteeswaran, D., & Chiranjeevi, V. (2014). Correlation of serum and salivary biochemical parameters in end stage renal disease patients undergoing hemodialysis in pre and post-dialysis state. Journal of Clinical Diagnostics Research, 8(12), CC12. doi:10.7860/JCDR/2014/10404.5306.
Silwood, C. J., Lynch, E., Claxson, A. W., & Grootveld, M. C. (2002). 1H and (13)C NMR spectroscopic analysis of human saliva. Journal of Dental Research, 81(6), 422–427.
Staples, A., & Wong, C. (2010). Risk factors for progression of chronic kidney disease. Current Opinion in Pediatrics, 22(2), 161–169.
Tomas, I., Marinho, J. S., Limeres, J., Santos, M. J., Araujo, L., & Diz, P. (2008). Changes in salivary composition in patients with renal failure. Archives of Oral Biology, 53(6), 528–532.
van Velzen, E. J., Westerhuis, J. A., van Duynhoven, J. P., van Dorsten, F. A., Hoefsloot, H. C., Jacobs, D. M., Smit, S., Draijer, R., Kroner, C. I., & Smilde, A. K. (2008). Multilevel data analysis of a crossover designed human nutritional intervention study. Journal of Proteome Research, 7(10), 4483–4491.
Walt, D. R., Blicharz, T. M., Hayman, R. B., Rissin, D. M., Bowden, M., Siqueira, W. L., Helmerhorst, E. J., Grand-Pierre, N., Oppenheim, F. G., Bhatia, J. S., et al. (2007). Microsensor arrays for saliva diagnostics. Annals of the New York Academy of Sciences, 1098, 389–400.
WHO. (1997). Oral health surveys: Basic methods, 4th edn. Geneva: WHO
Wishart, D. S., Tzur, D., Knox, C., Eisner, R., Guo, A. C., Young, N., Cheng, D., Jewell, K., Arndt, D., Sawhney, S., et al. (2007). Hmdb: The human metabolome database. Nucleic Acids Research, 35(Database issue), D521-D526.
Wong, C. J., Moxey-Mims, M., Jerry-Fluker, J., Warady, B. A., & Furth, S. L. (2012). Ckid (ckd in children) prospective cohort study: A review of current findings. American Journal of Kidney Diseases: The Official Journal of the National Kidney Foundation, 60(6), 1002–1011.
Wong, H., Mylrea, K., Feber, J., Drukker, A., & Filler, G. (2006). Prevalence of complications in children with chronic kidney disease according to kdoqi. Kidney International, 70(3), 585–590.
Xia, J., Sinelnikov, I. V., Han, B., & Wishart, D. S. (2015). Metaboanalyst 3.0–making metabolomics more meaningful. Nucleic Acids Research, 43(W1), W251-257.
Zhang, A., Sun, H., Wang, P., Han, Y., & Wang, X. (2012). Recent and potential developments of biofluid analyses in metabolomics. Journal of Proteomics, 75(4), 1079–1088.
Acknowledgements
The authors acknowledge the hemodialysis centers and the doctors Alberto Zagury and Gisella Pires Mello for their medical support.
Funding
This work was supported by Conselho Nacional de Desenvolvimento Científico e Tecnológico – CNPq (306214/2013; 303785/2014-4; 426265/2016-5), Fundação Carlos Chagas Filho de Amparo à Pesquisa do Estado do Rio de Janeiro – FAPERJ (201.278/2014; 620.012/2015; 202.902/2015), Centro Nacional de Ressonância Magnética Nuclear (CNRMN), and Instituto Nacional de Ciência and Tecnologia de Biologia Estrutural e Bioimagem (InBEB).
Author information
Authors and Affiliations
Contributions
All authors confirmed they have contributed to the intellectual content of this paper and have met the following 3 requirements: (a) significant contributions to the conception and design, acquisition of data, or analysis and interpretation of data; (b) drafting or revising the article for intellectual content; and (c) final approval of the published article.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical approval
This study analyzes collected data which involved human participants. This study was approved by the Local Ethical Committee (Comitê de Ética em Pesquisa do Hospital Federal de Bonsucesso - CEP-HFB 28/10).
Informed consent
Written informed consent was obtained from all participants or their respective legal representative.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Almeida, P.A., Fidalgo, T.K.S., Freitas-Fernandes, L.B. et al. Salivary metabolic profile of children and adolescents after hemodialysis. Metabolomics 13, 141 (2017). https://doi.org/10.1007/s11306-017-1283-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11306-017-1283-y