Abstract
Objectives
This study aimed to assess the morphological differences in the articular disc (AD) between hemophilic patients and healthy individuals of the control group for further association with signs and symptoms.
Methods
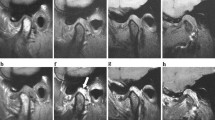
Fourteen severe hemophilic patients had their AD evaluated by magnetic resonance imaging (MRI). The morphological findings were compared to those of a control group consisting of 14 healthy individuals. MRI was used to evaluate all the components of the temporomandibular (TMJ), including the AD, resulting in sequential T1-weighted parasagittal images. All the images were acquired with teeth in maximum intercuspation position.
Results
Morphological alterations showed significant statistical differences (P-value = 0.0068), whereas no statistical differences were found in the other variables, including TMJ pain, headache, bruxism and mouth opening limitation. In the group of non-hemophilic individuals, only two (14.29%) presented AD with non-biconcave features, whereas in the group of hemophilic patients, nine (64.29%) presented AD with a morphology other than biconcave.
Conclusions
In patients with severe hemophilia, there seems to be a pattern of morphological alterations in the articular disc over time. The standard biconcave morphology of AD tends to change into other ones, particularly biplanar, hemiconvex and folded.



Similar content being viewed by others
Data availability
The data used to support the findings of this study are available to interested readers upon reasonable request.
References
Coppola A, Di Capua M, Di Minno MN, et al. Treatment of hemophilia: a review of current advances and ongoing issues. J Blood Med. 2010;1:183–95. https://doi.org/10.2147/JBM.S6885.
Sharma V, Khalid A, Cohen AJ. Management of pregnancy in a patient with severe hemophilia type a. AJP Rep. 2013;3(1):29–32. https://doi.org/10.1055/s-0032-1331376.
Ferreira AA, Leite IC, Bustamante-Teixeira MT, et al. Hemophilia A in Brazil—epidemiology and treatment developments. J Blood Med. 2014;5:175–84. https://doi.org/10.2147/JBM.S68234.
Khokhrin DV, Gileva OS, Khaliavina IN, et al. TMJ pathology in hemophilia patients. Stomatologiia (Mosk). 2012;91(2):46–8.
Lyons LP, Weinberg JB, Wittstein JR, et al. Blood in the joint: effects of hemarthrosis on meniscus health and repair techniques. Osteoarthr Cartil. 2021;29(4):471–9. https://doi.org/10.1016/j.joca.2020.11.008.
Hardaker WT Jr, Garrett WE Jr, Bassett FH 3rd. Evaluation of acute traumatic hemarthrosis of the knee joint. South Med J. 1990;83(6):640–4. https://doi.org/10.1097/00007611-199006000-00011.
Heard BJ, Barton KI, Agbojo OM, et al. Molecular response of rabbit menisci to surgically induced hemarthrosis and a single intra-articular dexamethasone treatment. J Orthop Res. 2019;37(9):2043–52. https://doi.org/10.1002/jor.24346.
Kaneda T, Nagayama M, Ohmori M, et al. Hemarthrosis of the temporomandibular joint in a patient with hemophilia B: report of case. J Oral Surg. 1979;37(7):513–4.
Nishioka GJ, Van Sickels JE, Tilson HB. Hemophilic arthropathy of the temporomandibular joint: review of the literature, a case report, and discussion. Oral Surg Oral Med Oral Pathol. 1988;65(2):145–50. https://doi.org/10.1016/0030-4220(88)90155-7.
Costa AL, Yasuda CL, Appenzeller S, et al. Comparison of conventional MRI and 3D reconstruction model for evaluation of temporomandibular joint. Surg Radiol Anat. 2008;30(8):663–7. https://doi.org/10.1007/s00276-008-0400-z.
Detamore MS, Athanasiou KA. Structure and function of the temporomandibular joint disc: implications for tissue engineering. J Oral Maxillofac Surg. 2003;61(4):494–506. https://doi.org/10.1053/joms.2003.50096.
Alomar X, Medrano J, Cabratosa J, et al. Anatomy of the temporomandibular joint. Semin Ultrasound CT MR. 2007;28(3):170–83.
Bag AK, Gaddikeri S, Singhal A, et al. Imaging of the temporomandibular joint: an update. World J Radiol. 2014;6(8):567–82. https://doi.org/10.4329/wjr.v6.i8.567.
Franchini M. The modern treatment of haemophilia: a narrative review. Blood Transfus. 2013;11(2):178–82. https://doi.org/10.2450/2012.0166-11.
Dworkin SF, LeResche L. Research diagnostic criteria for temporomandibular disorders: review, criteria, examinations and specifications, critique. J Craniomandib Disord. 1992;6(4):301–55.
Alonso MB, Gamba TO, Lopes SL, Cruz AD, Freitas DQ, Haiter-Neto F. Magnetic resonance imaging of the temporomandibular joint acquired using different parameters. J Morphol Sci. 2014;31(2):103–9. https://doi.org/10.4322/jms.062913.
de Farias JF, Melo SL, Bento PM, et al. Correlation between temporomandibular joint morphology and disc displacement by MRI. Dentomaxillofac Radiol. 2015;44(7):20150023. https://doi.org/10.1259/dmfr.20150023.
Guimarães TB, Ferreira-Cabrini MB, Quaglio CL, et al. Temporomandibular disorder: prevalence among hemophiliac patients. Int J Odontostomatol. 2015;9:295–300.
Yenel S, Cankal DA, Kayali SK, et al. Temporomandibular disorders in patients with inherited coagulation disorders: a clinical study. J Stomatol Oral Maxillofac Surg. 2022;123(4):473–7. https://doi.org/10.1016/j.jormas.2021.10.005.
Bennett GL, Leeson MC, Michael A. Extensive hemosiderin deposition in the medial meniscus of a knee. Its possible relationship to degenerative joint disease. Clin Orthop Relat Res. 1988;230:182–5.
Murphy MK, MacBarb RF, Wong ME, et al. Temporomandibular disorders: a review of etiology, clinical management, and tissue engineering strategies. Int J Oral Maxillofac Implants. 2013;28(6):e393-414. https://doi.org/10.11607/jomi.te20.
Kondrat W, Sierpinska T, Radke J. Assessment of the temporomandibular joint function in young adults without complaints from the masticatory system. Int J Med Sci. 2018;15(2):161–9. https://doi.org/10.7150/ijms.21665.
Shaffer SM, Brismee JM, Sizer PS, et al. Temporomandibular disorders. Part 1: anatomy and examination/diagnosis. J Man Manip Ther. 2014;22(1):2–12. https://doi.org/10.1179/2042618613Y.0000000060.
Nascimento Falcao I, Cal Alonso MBC, da Silva LH, et al. 3D morphology analysis of TMJ articular eminence in magnetic resonance imaging. Int J Dent. 2017;2017:5130241. https://doi.org/10.1155/2017/5130241.
Funding
This study was supported by FAPESP (São Paulo Research Foundation) Grants: 13/10999-5.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was approved by the Institutional Review Board of UNICAMP, according to protocol number 24113913.3.0000.5404. All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008. Informed consent was obtained from all patients for being included in the study.
Informed consent
Written informed consent was obtained from all subjects for being included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
de Oliveira, L.A.P., Gomes, J.P.P., Pimentel-Silva, L.R. et al. Magnetic resonance imaging evaluation of the disc morphology of temporomandibular joint in patients with severe hemophilia. Oral Radiol 39, 759–765 (2023). https://doi.org/10.1007/s11282-023-00697-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11282-023-00697-4