Abstract
Objective
There is no known preoperative marker that can effectively predict the risk of delayed neck metastasis (DNM), which is an important factor that determines the prognosis of early-stage oral cancer. In this study, we examined whether 18F-fluorodeoxyglucose positron emission tomography (18F-FDG-PET)/computed tomography (CT) uptake parameters of primary cancer can predict the risk of DNM in early-stage oral squamous cell carcinoma (OSCC).
Methods
Data from patients with stage I–II OSCC who underwent surgical resection of the primary tumor without elective neck dissection between January 2009 and December 2016 were retrospectively reviewed. Patient characteristics, histopathological factors, and PET/CT parameters (maximum standardized uptake value [SUVmax], metabolic tumor volume [MTV], and total lesion glycolysis [TLG]) were evaluated for their association with DNM. DNM rates were calculated, and the parameters that were statistically significant in the univariate analysis were used as explanatory variables. Independent factors associated with DNM were identified using multivariate analysis. For all statistical analyses, p-values < 0.05 were considered statistically significant.
Results
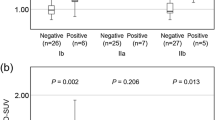
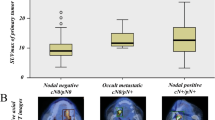
Data from 71 patients were analyzed in the study. The overall DNM rate among all patients was 21.8%. The univariate analysis showed that the T classification, depth of invasion, pattern of invasion, lymphovascular invasion, SUVmax, MTV, and TLG were significant predictors of DNM. However, the multivariate analysis revealed that only the depth of invasion, MTV, and TLG were independent predictors of DNM.
Conclusion
This study suggests that, in addition to conventional predictors, volume-based PET parameters are useful predictors of DNM in those with early-stage OSCC.







Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author on request. The data are not publicly available due to privacy or ethical restrictions.
References
Palme CE, Gullane PJ, Gilbert RW. Current treatment options in squamous cell carcinoma of the oral cavity. Surg Oncol Clin N Am. 2004;13:47–70. https://doi.org/10.1016/S1055-3207(03)00123-6.
Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, Jemal A. Global cancer statistics, 2012. CA Cancer J Clin. 2015;65:87–108. https://doi.org/10.3322/caac.21262.
Ferlay J, Shin HR, Bray F, Forman D, Mathers C, Parkin DM. Estimates of worldwide burden of cancer in 2008: Globocan 2008. Int J Cancer. 2010;127:2893–917. https://doi.org/10.1002/ijc.25516.
Fisch U. Lymphographic studies on the cervical lymphatic system. Fortschr Hals Nasen Ohrenheilkd. 1966;14:1–196.
da Silva SD, Hier M, Mlynarek A, Kowalski LP, Alaoui-Jamali MA. Recurrent oral cancer: current and emerging therapeutic approaches. Front Pharmacol. 2012;3:149. https://doi.org/10.3389/fphar.2012.00149.
Shah JP. Cervical lymph node metastases–diagnostic, therapeutic, and prognostic implications. Oncology (Williston Park). 1990;4:61–9.
D’Cruz AK, Vaish R, Kapre N, Dandekar M, Gupta S, Hawaldar R, et al. Elective versus therapeutic neck dissection in node-negative oral cancer. N Engl J Med. 2015;373:521–9. https://doi.org/10.1056/NEJMoa1506007.
Shah JP, Gil Z. Current concepts in management of oral cancer–surgery. Oral Oncol. 2009;45:394–401. https://doi.org/10.1016/j.oraloncology.2008.05.017.
Chaukar D, Dandekar M, Kane S, Arya S, Purandare N, Rangarajan V, et al. Relative value of ultrasound, computed tomography and positron emission tomography imaging in the clinically node-negative neck in oral cancer. Asia Pac J Clin Oncol. 2016;12:e332–8. https://doi.org/10.1111/ajco.12255.
Capote A, Escorial V, Muñoz-Guerra MF, Rodríguez-Campo FJ, Gamallo C, Naval L. Elective neck dissection in early-stage oral squamous cell carcinoma—does it influence recurrence and survival? Head Neck. 2007;29:3–11. https://doi.org/10.1002/hed.20482.
Dias FL, Kligerman J, Matos de Sá G, Arcuri RA, Freitas EQ, Farias T, et al. Elective neck dissection versus observation in stage I squamous cell carcinomas of the tongue and floor of the mouth. Otolaryngol Head Neck Surg. 2001;125:23–29, doi: https://doi.org/10.1067/mhn.2001.116188
Pimenta Amaral TMP, Da Silva Freire AR, Carvalho AL, Pinto CA, Kowalski LP. Predictive factors of occult metastasis and prognosis of clinical stages I and II squamous cell carcinoma of the tongue and floor of the mouth. Oral Oncol. 2004;40:780–6. https://doi.org/10.1016/j.oraloncology.2003.10.009.
Thiele OC, Seeberger R, Flechtenmacher C, Hofele C, Freier K. The role of elective supraomohyoidal neck dissection in the treatment of early, node-negative oral squamous cell carcinoma (OSCC): a retrospective analysis of 122 cases. J Craniomaxillofac Surg. 2012;40:67–70. https://doi.org/10.1016/j.jcms.2011.02.001.
Smith GI, O’Brien CJ, Clark J, Shannon KF, Clifford AR, McNeil EB, et al. Management of the neck in patients with T1 and T2 cancer in the mouth. Br J Oral Maxillofac Surg. 2004;42:494–500. https://doi.org/10.1016/j.bjoms.2004.06.013.
Andersen PE, Cambronero E, Shaha AR, Shah JP. The extent of neck disease after regional failure during observation of the N0 neck. Am J Surg. 1996;172:689–91. https://doi.org/10.1016/s0002-9610(96)00290-5.
Brandwein-Gensler M, Teixeira MS, Lewis CM, Lee B, Rolnitzky L, Hille JJ, et al. Oral squamous cell carcinoma: histologic risk assessment, but not margin status, is strongly predictive of local disease-free and overall survival. Am J Surg Pathol. 2005;29:167–78. https://doi.org/10.1097/01.pas.0000149687.90710.21.
Jakobsson PA, Eneroth CM, Killander D, Moberger G, Mårtensson B. Histologic classification and grading of malignancy in carcinoma of the larynx. Acta Radiol Ther Phys Biol. 1973;12:1–8. https://doi.org/10.3109/02841867309131085.
Anneroth G, Batsakis J, Luna M. Review of the literature and a recommended system of malignancy grading in oral squamous cell carcinomas. Scand J Dent Res. 1987;95:229–49. https://doi.org/10.1111/j.1600-0722.1987.tb01836.x.
Martínez-Gimeno C, Rodríguez EM, Vila CN, Varela CL. Squamous cell carcinoma of the oral cavity: a clinicopathologic scoring system for evaluating risk of cervical lymph node metastasis. Laryngoscope. 1995;105:728–33. https://doi.org/10.1288/00005537-199507000-00011.
Almangush A, Bello IO, Keski-Säntti H, Mäkinen LK, Kauppila JH, Pukkila M, et al. Depth of invasion, tumor budding, and worst pattern of invasion: prognostic indicators in early-stage oral tongue cancer. Head Neck. 2014;36:811–8. https://doi.org/10.1002/hed.23380.
Huang SH, Hwang D, Lockwood G, Goldstein DP, O’Sullivan B. Predictive value of tumor thickness for cervical lymph-node involvement in squamous cell carcinoma of the oral cavity: a meta-analysis of reported studies. Cancer. 2009;115:1489–97. https://doi.org/10.1002/cncr.24161.
Yamakawa N, Kirita T, Umeda M, Yanamoto S, Ota Y, Otsuru M, et al. Tumor budding and adjacent tissue at the invasive front correlate with delayed neck metastasis in clinical early-stage tongue squamous cell carcinoma. J Surg Oncol. 2019;119:370–8. https://doi.org/10.1002/jso.25334.
Kirita T, Yamakawa N, Ueda N, Yagyuu T. Tumor budding as a useful prognostic indicator in early oral squamous cell carcinoma. J Cancer Sci. 2018;10:162–7. https://doi.org/10.4172/1948-5956.1000536.
Phelps ME, Huang SC, Hoffman EJ, Selin C, Sokoloff L, Kuhl DE. Tomographic measurement of local cerebral glucose metabolic rate in humans with (F-18)2-fluoro-2-deoxy-D-glucose: validation of method. Ann Neurol. 1979;6:371–88. https://doi.org/10.1002/ana.410060502.
Kato H, Kuwano H, Nakajima M, Miyazaki T, Yoshikawa M, Ojima H, et al. Comparison between positron emission tomography and computed tomography in the use of the assessment of esophageal carcinoma. Cancer. 2002;94:921–8. https://doi.org/10.1002/cncr.10330.
Daisne JF, Duprez T, Weynand B, Lonneux M, Hamoir M, Reychler H, et al. Tumor volume in pharyngolaryngeal squamous cell carcinoma: comparison at CT, MR imaging, and FDG PET and validation with surgical specimen. Radiology. 2004;233:93–100. https://doi.org/10.1148/radiol.2331030660.
Ozawa Y, Hara M, Shibamoto Y, Tamaki T, Nishio M, Omi K. Utility of high-definition FDG-PET image reconstruction for lung cancer staging. Acta Radiol. 2013;54:916–20. https://doi.org/10.1177/0284185113488578.
Zhang H, Seikaly H, Biron VL, Jeffery CC. Utility of PET-CT in detecting nodal metastasis in cN0 early stage oral cavity squamous cell carcinoma. Oral Oncol. 2018;80:89–92. https://doi.org/10.1016/j.oraloncology.2018.04.003.
Sun R, Tang X, Yang Y, Zhang C. (18)FDG-PET/CT for the detection of regional nodal metastasis in patients with head and neck cancer: a meta-analysis. Oral Oncol. 2015;51:314–20. https://doi.org/10.1016/j.oraloncology.2015.01.004.
Allal AS, Dulguerov P, Allaoua M, Haenggeli CA, El-Ghazi EA, Lehmann W, et al. Standardized uptake value of 2-[(18)F] fluoro-2-deoxy-D-glucose in predicting outcome in head and neck carcinomas treated by radiotherapy with or without chemotherapy. J Clin Oncol. 2002;20:1398–404. https://doi.org/10.1200/JCO.2002.20.5.1398.
Wong RJ, Lin DT, Schöder H, Patel SG, Gonen M, Wolden S, et al. Diagnostic and prognostic value of [(18)F]fluorodeoxyglucose positron emission tomography for recurrent head and neck squamous cell carcinoma. J Clin Oncol. 2002;20:4199–208. https://doi.org/10.1200/JCO.2002.02.590.
Minn H, Lapela M, Klemi PJ, Grénman R, Leskinen S, Lindholm P, et al. Prediction of survival with fluorine-18-fluoro-deoxyglucose and PET in head and neck cancer. J Nucl Med. 1997;38:1907–11.
Shimomura H, Sasahira T, Yamanaka Y, Kurihara M, Imai Y, Tamaki S, et al. [18F]fluoro-2-deoxyglucose-positron emission tomography for the assessment of histopathological response after preoperative chemoradiotherapy in advanced oral squamous cell carcinoma. Int J Clin Oncol. 2015;20:308–16. https://doi.org/10.1007/s10147-014-0711-5.
Halfpenny W, Hain SF, Biassoni L, Maisey MN, Sherman JA, McGurk M. FDG-PET. A possible prognostic factor in head and neck cancer. Br J Cancer, 2002;86:512–516, doi: https://doi.org/10.1038/sj.bjc.6600114
Querellou S, Abgral R, Le Roux PY, Nowak E, Valette G, Potard G, et al. Prognostic value of fluorine-18 fluorodeoxyglucose positron-emission tomography imaging in patients with head and neck squamous cell carcinoma. Head Neck. 2012;34:462–8. https://doi.org/10.1002/hed.21765.
Paidpally V, Chirindel A, Lam S, Agrawal N, Quon H, Subramaniam RM. FDG-PET/CT imaging biomarkers in head and neck squamous cell carcinoma. Imaging Med. 2012;4:633–47. https://doi.org/10.2217/iim.12.60.
Abd El-Hafez YG, Moustafa HM, Khalil HF, Liao CT, Yen TC. Total lesion glycolysis: a possible new prognostic parameter in oral cavity squamous cell carcinoma. Oral Oncol. 2013;49:261–8. https://doi.org/10.1016/j.oraloncology.2012.09.005.
Lim R, Eaton A, Lee NY, Setton J, Ohri N, Rao S, et al. 18F-FDG PET/CT metabolic tumor volume and total lesion glycolysis predict outcome in oropharyngeal squamous cell carcinoma. J Nucl Med. 2012;53:1506–13. https://doi.org/10.2967/jnumed.111.101402.
Moon SH, Choi JY, Lee HJ, Son YI, Baek CH, Ahn YC, et al. Prognostic value of 18F-FDG PET/CT in patients with squamous cell carcinoma of the tonsil: comparisons of volume-based metabolic parameters. Head Neck. 2013;35:15–22. https://doi.org/10.1002/hed.22904.
Murphy JD, Chisholm KM, Daly ME, Wiegner EA, Truong D, Iagaru A, et al. Correlation between metabolic tumor volume and pathologic tumor volume in squamous cell carcinoma of the oral cavity. Radiother Oncol. 2011;101:356–61. https://doi.org/10.1016/j.radonc.2011.05.040.
Schinagl DA, Span PN, Oyen WJ, Kaanders JH. Can FDG PET predict radiation treatment outcome in head and neck cancer? Results of a prospective study. Eur J Nucl Med Mol Imaging. 2011;38:1449–58. https://doi.org/10.1007/s00259-011-1789-x.
Ryu IS, Kim JS, Roh JL, Cho KJ, Choi SH, Nam SY, et al. Prognostic significance of preoperative metabolic tumour volume and total lesion glycolysis measured by (18)F-FDG PET/CT in squamous cell carcinoma of the oral cavity. Eur J Nucl Med Mol Imaging. 2014;41:452–61. https://doi.org/10.1007/s00259-013-2571-z.
Hutchison IL, Ridout F, Cheung SMY, Shah N, Hardee P, Surwald C, et al. Nationwide randomised trial evaluating elective neck dissection for early stage oral cancer (SEND study) with meta-analysis and concurrent real-world cohort. Br J Cancer. 2019;121:827–36. https://doi.org/10.1038/s41416-019-0587-2.
Cao Y, Wang T, Yu C, Guo X, Li C, Li L. Elective neck dissection versus wait-and-watch policy for oral cavity squamous cell carcinoma in early stage: A systematic review and meta-analysis based on survival data. J Oral Maxillofac Surg. 2019;77:2154–67. https://doi.org/10.1016/j.joms.2019.03.015.
Bello IO, Soini Y, Salo T. Prognostic evaluation of oral tongue cancer: means, markers and perspectives (I). Oral Oncol. 2010;46:630–5. https://doi.org/10.1016/j.oraloncology.2010.06.006.
Regezi JA, Sciubba JJ, Jordan RCK. Oral pathology: clinical, pathologic correlations. 5th ed. St Louis (MO): Saunders Elsevier; 2008
Kim KH, Lee J, Chang JS, Lee CG, Yun M, Choi EC, et al. Prognostic value of FDG-PET volumetric parameters in patients with p16-positive oropharyngeal squamous cell carcinoma who received curative resection followed by postoperative radiotherapy or chemoradiotherapy. Head Neck. 2016;38:1515–24. https://doi.org/10.1002/hed.24465.
Schwartz DL, Harris J, Yao M, Rosenthal DI, Opanowski A, Levering A, et al. Metabolic tumor volume as a prognostic imaging-based biomarker for head-and-neck cancer: pilot results from Radiation Therapy Oncology Group protocol 0522. Int J Radiat Oncol Biol Phys. 2015;91:721–9. https://doi.org/10.1016/j.ijrobp.2014.12.023.
Abgral R, Valette G, Robin P, Rousset J, Keromnes N, Le Roux PY, et al. Prognostic evaluation of percentage variation of metabolic tumor burden calculated by dual-phase (18) FDG PET-CT imaging in patients with head and neck cancer. Head Neck. 2016;38(Suppl 1):E600–6. https://doi.org/10.1002/hed.24048.
Yamamoto E, Kohama G, Sunakawa H, Iwai M, Hiratsuka H. Mode of invasion, bleomycin sensitivity, and clinical course in squamous cell carcinoma of the oral cavity. Cancer. 1983;51:2175–80. https://doi.org/10.1002/1097-0142(19830615)51:12%3c2175::aid-cncr2820511205%3e3.0.co;2-m.
Kimura S, Nanbu U, Noguchi H, Harada Y, Kumamoto K, Sasaguri Y, et al. Macrophage CCL22 expression in the tumor microenvironment and implications for survival in patients with squamous cell carcinoma of the tongue. J Oral Pathol Med. 2019;48:677–85. https://doi.org/10.1111/jop.12885.
Kaihara T, Kusaka T, Kawamata H, Oda Y, Fujii S, Morita K, et al. Decreased expression of E-cadherin and Yamamoto-Kohama’s mode of invasion highly correlates with lymph node metastasis in esophageal squamous cell carcinoma. Pathobiology. 2001;69:172–8. https://doi.org/10.1159/000048772.
Weiss MH, Harrison LB, Isaacs RS. Use of decision analysis in planning a management strategy for the stage N0 neck. Arch Otolaryngol Head Neck Surg. 1994;120:699–702. https://doi.org/10.1001/archotol.1994.01880310005001.
Dünne AA, Müller HH, Eisele DW, Kessel K, Moll R, Werner JA. Meta-analysis of the prognostic significance of perinodal spread in head and neck squamous cell carcinomas (HNSCC) patients. Eur J Cancer. 2006;42:1863–8. https://doi.org/10.1016/j.ejca.2006.01.062.
da Silva SD, Morand GB, Alobaid FA, Hier MP, Mlynarek AM, Alaoui-Jamali MA, et al. Epithelial-mesenchymal transition (EMT) markers have prognostic impact in multiple primary oral squamous cell carcinoma. Clin Exp Metastasis. 2015;32:55–63. https://doi.org/10.1007/s10585-014-9690-1.
Huber GF, Fritzsche FR, Züllig L, Storz M, Graf N, Haerle SK, et al. Podoplanin expression correlates with sentinel lymph node metastasis in early squamous cell carcinomas of the oral cavity and oropharynx. Int J Cancer. 2011;129:1404–9. https://doi.org/10.1002/ijc.25795.
Huber GF, Züllig L, Soltermann A, Roessle M, Graf N, Haerle SK, et al. Down regulation of E-cadherin (ECAD) – a predictor for occult metastatic disease in sentinel node biopsy of early squamous cell carcinomas of the oral cavity and oropharynx. BMC Cancer. 2011;11(217):1–8. https://doi.org/10.1186/1471-2407-11-217.
Shinohara S, Kikuchi M, Suehiro A, Kishimoto I, Harada H. Is 18F-fluorodeoxyglucose positron emission tomography/computed tomography helpful in the decision-making process for neck dissection in patients with T1–T2 lingual cancer? Acta Otolaryngol. 2015;135:181–6. https://doi.org/10.3109/00016489.2014.975894.
Morand GB, Vital DG, Kudura K, Werner J, Stoeckli SJ, Huber GF, et al. Maximum Standardized Uptake Value (SUVmax) of primary tumor predicts occult neck metastasis in oral cancer. Sci Rep. 2018;8:11817. https://doi.org/10.1038/s41598-018-30111-7.
Brun E, Kjellén E, Tennvall J, Ohlsson T, Sandell A, Perfekt R, et al. FDG PET studies during treatment: prediction of therapy outcome in head and neck squamous cell carcinoma. Head Neck. 2002;24:127–35. https://doi.org/10.1002/hed.10037.
Machtay M, Natwa M, Andrel J, Hyslop T, Anne PR, Lavarino J, et al. Pretreatment FDG-PET standardized uptake value as a prognostic factor for outcome in head and neck cancer. Head Neck. 2009;31:195–201. https://doi.org/10.1002/hed.20942.
Kurokawa H, Yamashita Y, Takeda S, Zhang M, Fukuyama H, Takahashi T. Risk factors for late cervical lymph node metastases in patients with stage I or II carcinoma of the tongue. Head Neck. 2002;24:731–6. https://doi.org/10.1002/hed.10130.
Acknowledgements
We acknowledge the support of Dr. Yuu Tanaka from the Department of Rehabilitation, Faculty of Health Science, Wakayama Professional University of Rehabilitation for assistance with statistical analyses. We wish to thank Editage (http://www.editage.jp/) for English-language editing.
Funding
This study did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
Nobuhiro Yamakawa and Tadaaki Kirita contributed to the study conception and design. Material preparation and data collection were performed by Yohei Nakayama, Nobuhiro Ueda, and Takahiro Yagyuu. Analyses were performed by Nobuhiro Yamakawa and Shigehiro Tamaki. The first draft of the manuscript was written by Nobuhiro Yamakawa and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation and with the Helsinki Declaration of 1975, as revised in 2008. The study protocol was approved by the Ethics Committee of Nara Medical University (approval number: 2339).
Consent to participate
Informed consent was waived by the local Ethics Committee of Nara Medical University in view of the retrospective nature of the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yamakawa, N., Nakayama, Y., Ueda, N. et al. Volume-based 18F-fluorodeoxyglucose positron emission tomography/computed tomography parameters correlate with delayed neck metastasis in clinical early-stage oral squamous cell carcinoma. Oral Radiol 39, 668–682 (2023). https://doi.org/10.1007/s11282-023-00686-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11282-023-00686-7