Abstract
Background
Fast glomerular filtration rate (GFR) decline is associated with adverse outcomes, but the associated risk factors among patients without chronic kidney disease (CKD) are not well defined.
Methods
From a primary care registry of 37,796, we identified 2219 (6%) adults with at least three estimated (e)GFR values and a baseline eGFR between 60 and 119 ml/min/1.73 m2 during an observation period of 8 years. We defined fast GFR decline as > 5 ml/min/1.73 m2 per year. The outcome measure was incident CKD (eGFR < 60 ml/min/1.73 m2). Clinical and demographic characteristics were compared using Chi-square and independent-samples t tests.
Results
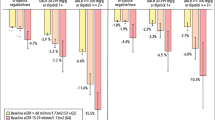
Older age, African-American race, unmarried status, hypertension and type 2 diabetes were more common in both fast decliners and those who developed incident CKD (p < 0.0001 to < 0.05). Lower neighborhood socioeconomic status, current smoking and baseline eGFR 90–119 ml/min/1.73 m2 were associated with fast decline (p < 0.01), while baseline eGFR 60–74 ml/min/1.73 m2 with incident CKD (p < 0.05). In multivariate regression models, among fast decliners with mildly reduced baseline eGFR (60–89 ml/min/1.73 m2), older age was significantly associated with incident CKD [odds ratio (OR) 1.04; 95% CI 1.01–1.08], and among those with normal baseline eGFR (≥ 90–119 ml/min/1.73 m2), type 2 diabetes was significantly associated with incident CKD (OR 3.83; 95% CI 1.35–10.89).
Conclusions
Among primary care patients without CKD, GFR is checked infrequently. We have identified patients at high risk of progressive CKD, in whom we suggest a closer monitoring of renal function.
Similar content being viewed by others
References
Muntner P, He J, Hamm L, Loria C, Whelton PK (2002) Renal insufficiency and subsequent death resulting from cardiovascular disease in the United States. J Am Soc Nephrol 13(3):745–753
Natali A, Boldrini B, Baldi S, Rossi M, Landi P, Severi S, Solini A, Ferrannini E (2014) Impact of mild to moderate reductions of glomerular filtration rate on coronary artery disease severity. Nutr Metab Cardiovasc Dis 24(6):681–688
Mohandas R, Segal M, Srinivas TR, Johnson BD, Wen X, Handberg EM, Petersen JW, Sopko G, Merz CN, Pepine CJ (2015) Mild renal dysfunction and long-term adverse outcomes in women with chest pain: results from the National Heart, Lung, and Blood Institute-sponsored Women’s Ischemia Syndrome Evaluation (WISE). Am Heart J 169(3):412–418
Lambers Heerspink HJ, Tighiouart H, Sang Y, Ballew S, Mondal H, Matsushita K, Coresh J, Levey AS, Inker LA (2014) GFR decline and subsequent risk of established kidney outcomes: a meta-analysis of 37 randomized controlled trials. Am J Kidney Dis 64(6):860–866
Inker LA, Lambers Heerspink HJ, Mondal H, Schmid CH, Tighiouart H, Noubary F, Coresh J, Greene T, Levey AS (2014) GFR decline as an alternative end point to kidney failure in clinical trials: a meta-analysis of treatment effects from 37 randomized trials. Am J Kidney Dis 64(6):848–859
El-Ghoul B, Elie C, Sqalli T, Jungers P, Daudon M, Grunfeld JP, Lesavre P, Joly D (2009) Nonprogressive kidney dysfunction and outcomes in older adults with chronic kidney disease. J Am Geriatr Soc 57(12):2217–2223
Perkins RM, Bucaloiu ID, Kirchner HL, Ashouian N, Hartle JE, Yahya T (2011) GFR decline and mortality risk among patients with chronic kidney disease. Clin J Am Soc Nephrol CJASN 6(8):1879–1886
Collister D, Ferguson T, Komenda P, Tangri N (2016) The patterns, risk factors, and prediction of progression in chronic kidney disease: a narrative review. Semin Nephrol 36(4):273–282
Hsu CY, Lin F, Vittinghoff E, Shlipak MG (2003) Racial differences in the progression from chronic renal insufficiency to end-stage renal disease in the United States. J Am Soc Nephrol 14(11):2902–2907
Al-Aly Z, Zeringue A, Fu J, Rauchman MI, McDonald JR, El-Achkar TM, Balasubramanian S, Nurutdinova D, Xian H, Stroupe K et al (2010) Rate of kidney function decline associates with mortality. J Am Soc Nephrol 21(11):1961–1969
Tsai WC, Wu HY, Peng YS, Ko MJ, Wu MS, Hung KY, Wu KD, Chu TS, Chien KL (2016) Risk factors for development and progression of chronic kidney disease: a systematic review and exploratory meta-analysis. Medicine 95(11):e3013
Zoppini G, Targher G, Chonchol M, Ortalda V, Negri C, Stoico V, Bonora E (2012) Predictors of estimated GFR decline in patients with type 2 diabetes and preserved kidney function. Clin J Am Soc Nephrol CJASN 7(3):401–408
Sumida K, Molnar MZ, Potukuchi PK, George K, Thomas F, Lu JL, Yamagata K, Kalantar-Zadeh K, Kovesdy CP (2017) Changes in albuminuria and subsequent risk of incident kidney disease. Clin J Am Soc Nephrol, CJASN
Tonelli M, Klarenbach SW, Lloyd AM, James MT, Bello AK, Manns BJ, Hemmelgarn BR (2011) Higher estimated glomerular filtration rates may be associated with increased risk of adverse outcomes, especially with concomitant proteinuria. Kidney Int 80(12):1306–1314
Manard WT, Syberg K, Behera A, Salas J, Schneider FD, Armbrecht E, Hooks-Anderson D, Crannage E, Scherrer J (2016) Higher referrals for diabetes education in a medical home model of care. J Am Board Fam Med JABFM 29(3):377–384
Hooks-Anderson DR, Crannage EF, Salas J, Scherrer JF (2015) Race and referral to diabetes education in primary care patients with prediabetes and diabetes. Diabetes Educ 41(3):281–289
Brieler JA, Scherrer JF, Salas J (2015) Differences in prescribing patterns for anxiety and depression between general internal medicine and family medicine. J Affect Disord 172:153–158
Scherrer JF, Salas J, Brieler JA, Miller BJ, Meyer D, Schneider FD (2015) Depression leads to incident vascular disease: evidence for the relevance to primary care. Fam Pract 32(2):147–151
Koraishy FM, Hooks-Anderson D, Salas J, Scherrer JF (2017) Rate of renal function decline, race and referral to nephrology in a large cohort of primary care patients. Fam Pract 34(4):416–422
Hsu TW, Kuo KL, Hung SC, Huang PH, Chen JW, Tarng DC (2013) Progression of kidney disease in non-diabetic patients with coronary artery disease: predictive role of circulating matrix metalloproteinase-2, -3, and -9. PLoS ONE 8(7):e70132
Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF 3rd, Feldman HI, Kusek JW, Eggers P, Van Lente F, Greene T et al (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150(9):604–612
Matsushita K, Mahmoodi BK, Woodward M, Emberson JR, Jafar TH, Jee SH, Polkinghorne KR, Shankar A, Smith DH, Tonelli M et al (2012) Comparison of risk prediction using the CKD-EPI equation and the MDRD study equation for estimated glomerular filtration rate. JAMA 307(18):1941–1951
Coresh J, Turin TC, Matsushita K, Sang Y, Ballew SH, Appel LJ, Arima H, Chadban SJ, Cirillo M, Djurdjev O et al (2014) Decline in estimated glomerular filtration rate and subsequent risk of end-stage renal disease and mortality. JAMA 311(24):2518–2531
Inker LA, Astor BC, Fox CH, Isakova T, Lash JP, Peralta CA, Kurella Tamura M, Feldman HI (2014) KDOQI US commentary on the 2012 KDIGO clinical practice guideline for the evaluation and management of CKD. Am J Kidney Dis 63(5):713–735
Upadhyay A, Earley A, Haynes SM, Uhlig K (2011) Systematic review: blood pressure target in chronic kidney disease and proteinuria as an effect modifier. Ann Intern Med 154(8):541–548
Davis E, Campbell K, Gobe G, Hawley C, Isbel N, Johnson DW (2016) Association of anthropometric measures with kidney disease progression and mortality: a retrospective cohort study of pre-dialysis chronic kidney disease patients referred to a specialist renal service. BMC Nephrol 17(1):74
Tonelli M, Wiebe N, Guthrie B, James MT, Quan H, Fortin M, Klarenbach SW, Sargious P, Straus S, Lewanczuk R et al (2015) Comorbidity as a driver of adverse outcomes in people with chronic kidney disease. Kidney Int 88(4):859–866
Staplin N, Haynes R, Herrington WG, Reith C, Cass A, Fellstrom B, Jiang L, Kasiske BL, Krane V, Levin A et al (2016) Smoking and adverse outcomes in patients with CKD: the study of heart and renal protection (SHARP). Am J Kidney Dis 68(3):371–380
Roblin DW (2013) Validation of a neighborhood SES index in a managed care organization. Med Care 51(1):e1–e8
Patzer RE, McClellan WM (2012) Influence of race, ethnicity and socioeconomic status on kidney disease. Nat Rev Nephrol 8(9):533–541
Frayne SM, Miller DR, Sharkansky EJ, Jackson VW, Wang F, Halanych JH, Berlowitz DR, Kader B, Rosen CS, Keane TM (2010) Using administrative data to identify mental illness: what approach is best? Am J Med Qual 25(1):42–50
Herget-Rosenthal S, Dehnen D, Kribben A, Quellmann T (2013) Progressive chronic kidney disease in primary care: modifiable risk factors and predictive model. Prev Med 57(4):357–362
Tohidi M, Hasheminia M, Mohebi R, Khalili D, Hosseinpanah F, Yazdani B, Nasiri AA, Azizi F, Hadaegh F (2012) Incidence of chronic kidney disease and its risk factors, results of over 10 year follow up in an Iranian cohort. PLoS ONE 7(9):e45304
O’Seaghdha CM, Lyass A, Massaro JM, Meigs JB, Coresh J, D’Agostino RB Sr, Astor BC, Fox CS (2012) A risk score for chronic kidney disease in the general population. Am J Med 125(3):270–277
Chien KL, Lin HJ, Lee BC, Hsu HC, Lee YT, Chen MF (2010) A prediction model for the risk of incident chronic kidney disease. Am J Med 123(9):836–846
Hall YN, Himmelfarb J (2017) The CKD classification system in the precision medicine era. Clin J Am Soc Nephrol CJASN 12(2):346–348
Rosansky SJ (2012) Renal function trajectory is more important than chronic kidney disease stage for managing patients with chronic kidney disease. Am J Nephrol 36(1):1–10
Methven S, MacGregor MS, Traynor JP, Hair M, O’Reilly DS, Deighan CJ (2011) Comparison of urinary albumin and urinary total protein as predictors of patient outcomes in CKD. Am J Kidney Dis 57(1):21–28
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Informed consent
The creation of this retrospective cohort and its use for primary care research were approved by the SLU Institutional Review Board. Informed consent was waived due to the observational nature of the study, and no PHI was used.
Rights and permissions
About this article
Cite this article
Koraishy, F.M., Hooks-Anderson, D., Salas, J. et al. Fast GFR decline and progression to CKD among primary care patients with preserved GFR. Int Urol Nephrol 50, 501–508 (2018). https://doi.org/10.1007/s11255-018-1805-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-018-1805-1