Abstract
Objectives
To analyze the survival and the associated factors affecting the prognosis of renal cell carcinoma (RCC) in China with a sufficiently large sample size.
Methods
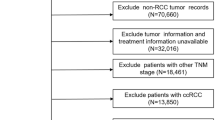
Clinical data with complete follow-up of 1326 RCC patients were successfully obtained. Progression-free survival (PFS) and cancer-specific survival (CSS) were calculated, survival analysis was performed by Kaplan–Meier analysis, and Cox proportional hazards regression models were served to estimate the prognostic significance of each variables.
Results
The median length of follow-up was 43.55 months (25–75 %, 25.47–68.75 months). During follow-up, 147 patients developed RCC-related progression, with a median PFS of 18.2 months (25–75 %, 7.50–47.27); 64 patients died from RCC-related progression, with a median CSS of 27.67 months (25–75 %, 14.10–58.53). For RCC patients in T1 stage, 3-, 5-, 8-, and 10-year CSS rates of patients receiving nephron-sparing nephrectomy were 99.33, 98.21, 97.40, and 97.40 %, respectively, which were significantly higher than radical nephrectomy patients (97.88, 96.28, 95.09, and 88.58 %, respectively). Cox proportional hazards regression model showed that tumor N stage, signs of lung metastasis (such as cough and hemoptysis), signs of bone metastasis (such as bone pain and fracture), pathological subtype of RCC, microscopic sarcomatoid change, and progression were prognosis factors for Chinese RCC patients.
Conclusions
Tumor stage, nephrectomy type, lung metastasis, bone metastasis, pathological subtype, sarcomatoid change, and type of progression were important risk factors for RCC. For T1 stage RCC patients, nephron-sparing nephrectomy showed better CSS than radical nephrectomy, which may guide the doctors and patients in their choices of surgical procedures.






Similar content being viewed by others
References
Ghoneim T, Ouzzane A, Leroy X et al (2012) Renal cell carcinoma of patients younger than 40 years old. Progres en urologie: journal de l’Association francaise d’urologie et de la Societe francaise d’urologie 22:93–99
Aron M, Nguyen MM, Stein RJ, Gill IS (2008) Impact of gender in renal cell carcinoma: an analysis of the SEER database. Eur Urol 54:133–140
Jeong IG, Yoo CH, Song K et al (2009) Age at diagnosis is an independent predictor of small renal cell carcinoma recurrence-free survival. J Urol 182:445–450
Taccoen X, Valeri A, Descotes JL et al (2007) Renal cell carcinoma in adults 40 years old or less: young age is an independent prognostic factor for cancer-specific survival. Eur Urol 51:980–987
Aziz A, May M, Zigeuner R et al (2014) Do young patients with renal cell carcinoma feature a distinct outcome after surgery? A comparative analysis of patient age based on the multinational CORONA database. J Urol 191:310–315
Steffens S, Junker K, Roos FC et al (2014) Small renal cell carcinomas—how dangerous are they really? Results of a large multicenter study. Eur J Cancer 50:739–745
Bianchi M, Becker A, Trinh QD et al (2013) An analysis of patients with T2 renal cell carcinoma (RCC) according to tumour size: a population-based analysis. BJU Int 111:1184–1190
Kopp RP, Mehrazin R, Palazzi KL et al (2014) Survival outcomes after radical and partial nephrectomy for clinical T2 renal tumours categorised by R.E.N.A.L. nephrometry score. BJU Int 114:708–718
Long CJ, Canter DJ, Kutikov A et al (2012) Partial nephrectomy for renal masses >/=7 cm: technical, oncological and functional outcomes. BJU Int 109:1450–1456
Becker F, Roos FC, Janssen M et al (2011) Short-term functional and oncologic outcomes of nephron-sparing surgery for renal tumours >/= 7 cm. Eur Urol 59:931–937
Laird A, Choy KC, Delaney H et al (2015) Matched pair analysis of laparoscopic versus open radical nephrectomy for the treatment of T3 renal cell carcinoma. World J Urol 33:25–32
Stewart GD, Ang WJ, Laird A, Tolley DA, Riddick AC, McNeill SA (2012) The operative safety and oncological outcomes of laparoscopic nephrectomy for T3 renal cell cancer. BJU Int 110:884–890
Lam JS, Klatte T, Patard JJ et al (2007) Prognostic relevance of tumour size in T3a renal cell carcinoma: a multicentre experience. Eur Urol 52:155–162
Patel HD, Kates M, Pierorazio PM et al (2014) Survival after diagnosis of localized T1a kidney cancer: current population-based practice of surgery and nonsurgical management. Urology 83:126–132
Meskawi M, Becker A, Bianchi M et al (2014) Partial and radical nephrectomy provide comparable long-term cancer control for T1b renal cell carcinoma. Int J Urol 21:122–128
Thompson RH, Siddiqui S, Lohse CM, Leibovich BC, Russo P, Blute ML (2009) Partial versus radical nephrectomy for 4 to 7 cm renal cortical tumors. J Urol 182:2601–2606
Thompson RH, Boorjian SA, Lohse CM et al (2008) Radical nephrectomy for pT1a renal masses may be associated with decreased overall survival compared with partial nephrectomy. J Urol 179:468–473
Patard JJ, Leray E, Cindolo L et al (2004) Multi-institutional validation of a symptom based classification for renal cell carcinoma. J Urol 172:858–862
Minardi D, Lucarini G, Filosa A et al (2008) Prognostic role of tumor necrosis, microvessel density, vascular endothelial growth factor and hypoxia inducible factor-1alpha in patients with clear cell renal carcinoma after radical nephrectomy in a long term follow-up. Int J Immunopathol Pharmacol 21:447–455
Minervini A, Di Cristofano C, Gacci M et al (2008) Prognostic role of histological necrosis for nonmetastatic clear cell renal cell carcinoma: correlation with pathological features and molecular markers. J Urol 180:1284–1289
Klatte T, Said JW, de Martino M et al (2009) Presence of tumor necrosis is not a significant predictor of survival in clear cell renal cell carcinoma: higher prognostic accuracy of extent based rather than presence/absence classification. J Urol 181:1558–1564
Teng J, Gao Y, Chen M et al (2014) Prognostic value of clinical and pathological factors for surgically treated localized clear cell renal cell carcinoma. Chin Med J (Engl) 127:1640–1644
Spiess PE, Kurian T, Lin HY et al (2012) Preoperative metastatic status, level of thrombus and body mass index predict overall survival in patients undergoing nephrectomy and inferior vena cava thrombectomy. BJU Int 110:E470–E474
Wagner B, Patard JJ, Mejean A et al (2009) Prognostic value of renal vein and inferior vena cava involvement in renal cell carcinoma. Eur Urol 55:452–459
Zugor V, Labanaris AP, Berthold L, Schott GE (2008) Inferior vena cava involvement in renal cell carcinoma: comparison of survival rates between patients with thrombus and infiltration. Scand J Urol Nephrol 42:35–39
Lee JH, Choi JW, Kim YS (2010) The value of histologic subtyping on outcomes of clear cell and papillary renal cell carcinomas: a meta-analysis. Urology 76:889–894
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
None.
Rights and permissions
About this article
Cite this article
Zhang, Y., Yu, H. & Li, H. Survival analysis of surgically treated renal cell carcinoma: a single Chinese medical center experience from 2002 to 2012. Int Urol Nephrol 47, 1327–1333 (2015). https://doi.org/10.1007/s11255-015-1046-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-015-1046-5