Abstract
Purpose
To perform a comprehensive psychometric analysis of the Boston Carpal Tunnel Syndrome Questionnaire (BCTQ) by means of factor and Rasch analyses in subjects with neurophysiologic confirmation of carpal tunnel syndrome (CTS). Relationship between clinical severity assessed with the log-linear version of the BCTQ and neurophysiologic severity assessed with nerve conduction studies was further examined.
Methods
Five hundred and twenty-eight individuals completed the questionnaire. Confirmatory and exploratory factor analyses were used to determine the latent structure of the BCTQ. Through Rasch methodology, a log-linear version was proposed given the latent structure of the questionnaire. Linear relationship between the proposed questionnaire and neurophysiologic findings was established.
Results
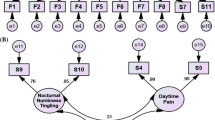
The BCTQ underlying structure comprises, at least, three factors that may be represented by Functionality, Paresthesia and Pain domains. Two log-linear subscales may be proposed: subscale 1 comprised of the Functionality factor and subscale 2 which incorporates the Paresthesia and Pain factors under a bifactor solution. Neurophysiologic and clinical severity classification system displays a very weak linear correlation.
Conclusion
A log-linear version of the BCTQ, useful as an outcome tool in clinical and trial settings, is proposed. Neurophysiological data lack the ability to resemble changes in clinical status of individuals with CTS.

Similar content being viewed by others
References
Wipperman, J., & Goerl, K. (2016). Carpal Tunnel Syndrome: Diagnosis and management. American Family Physician, 94(12), 993–999
Levine, D. W., Simmons, B. P., Koris, M. J., Daltroy, L. H., Hohl, G. G., Fossel, A. H., et al. (1993). A self-administered questionnaire for the assessment of severity of symptoms and functional status in carpal tunnel syndrome. Journal of Bone and Joint Surgery American, 75(11), 1585–1592
Patrick, D. L., Burke, L. B., Powers, J. H., Scott, J. A., Rock, E. P., Dawisha, S., et al. (2007). Patient-reported outcomes to support medical product labeling claims: FDA perspective. Value Health., 10(Suppl 2), S125–S137
MacDermid, J. C. (2014). Patient-reported outcomes: state-of-the-art hand surgery and future applications. Hand Clinics, 30(3), 293–304
Bravini, E., Franchignoni, F., Giordano, A., Sartorio, F., Ferriero, G., Vercelli, S., et al. (2015). Classical test theory and Rasch analysis validation of the Upper Limb Functional Index in subjects with upper limb musculoskeletal disorders. Archives of Physical Medicine and Rehabilitation, 96(1), 98–104
Amadio, P. C., Silverstein, M. D., Ilstrup, D. M., Schleck, C. D., & Jensen, L. M. (1996). Outcome assessment for carpal tunnel surgery: The relative responsiveness of generic, arthritis-specific, disease-specific, and physical examination measures. J Hand Surg Am., 21(3), 338–346
Atroshi I, Johnsson R, Sprinchorn A. (1998). Self-administered outcome instrument in carpal tunnel syndrome. Reliability validity and responsiveness evaluated in 102 patients. Acta Orthopaedica Scandinavica, 69(1), 82–88.
Bessette, L., Sangha, O., Kuntz, K. M., Keller, R. B., Lew, R. A., Fossel, A. H., et al. (1998). Comparative responsiveness of generic versus disease-specific and weighted versus unweighted health status measures in carpal tunnel syndrome. Medical Care, 36(4), 491–502
Gay, R. E., Amadio, P. C., & Johnson, J. C. (2003). Comparative responsiveness of the disabilities of the arm, shoulder, and hand, the carpal tunnel questionnaire, and the SF-36 to clinical change after carpal tunnel release. Journal of Hand Surgery America, 28(2), 250–254
Greenslade, J. R., Mehta, R. L., Belward, P., & Warwick, D. J. (2004). Dash and Boston questionnaire assessment of carpal tunnel syndrome outcome: What is the responsiveness of an outcome questionnaire? Journal of Hand Surgery British, 29(2), 159–164
Rosales RS, Delgado EB, de la Lastra-Bosch ID. Evaluation of the Spanish version of the DASH and carpal tunnel syndrome health-related quality-of-life instruments: cross-cultural adaptation process and reliability. Journal of Hand Surgery America. 2002;27(2):334–43.
Atroshi, I., Lyren, P. E., & Gummesson, C. (2009). The 6-item CTS symptoms scale: A brief outcomes measure for carpal tunnel syndrome. Quality of Life Research, 18(3), 347–358
De Kleermaeker, F., Levels, M., Verhagen, W. I. M., & Meulstee, J. (2019). Validation of the Dutch version of the Boston Carpal Tunnel Questionnaire. Frontiers in Neurology, 10, 1154
Lue, Y. J., Wu, Y. Y., Liu, Y. F., Lin, G. T., & Lu, Y. M. (2015). Confirmatory factor analysis of the Boston Carpal Tunnel Questionnaire. Journal of Occupational Rehabilitation, 25(4), 717–724
de Campos, C. C., Manzano, G. M., de Andrade, L. B., Castelo Filho, A., & Nobrega, J. A. (2003). Translation and validation of an instrument for evaluation of severity of symptoms and the functional status in carpal tunnel syndrome. Arquivos de Neuro-Psiquiatria, 61(1), 51–55
Imaeda, T., Uchiyama, S., Toh, S., Wada, T., Okinaga, S., Sawaizumi, T., et al. (2007). Validation of the Japanese Society for Surgery of the Hand version of the Carpal Tunnel Syndrome Instrument. Journal of Orthopaedic Science, 12(1), 14–21
Ortiz-Corredor, F., Calambas, N., Mendoza-Pulido, C., Galeano, J., Diaz-Ruiz, J., & Delgado, O. (2011). Factor analysis of carpal tunnel syndrome questionnaire in relation to nerve conduction studies. Clinical Neurophysiology, 122(10), 2067–2070
Conrad, K. J., & Smith, E. V., Jr. (2004). International conference on objective measurement: Applications of Rasch analysis in health care. Medical Care, 42(1 Suppl), I1-6
Tennant, A., & Conaghan, P. G. (2007). The Rasch measurement model in rheumatology: What is it and why use it? When should it be applied, and what should one look for in a Rasch paper? Arthritis and Rheumatism, 57(8), 1358–1362
Tesio, L. (2007). Functional assessment in rehabilitative medicine: Principles and methods. Europa Medicophysica, 43(4), 515–523
Wade, D. T. (1999). Outcome measurement and rehabilitation. Clinical Rehabilitation, 13(2), 93–95
Forrest, M., & Andersen, B. (1986). Ordinal scale and statistics in medical research. British Medical Journal (Clinical Research Edition), 292(6519), 537–538
Wright, B. D., & Linacre, J. M. (1989). Observations are always ordinal; measurements, however, must be interval. Archives of Physical Medicine and Rehabilitation, 70(12), 857–860
Nielsen, T., & Dammeyer, J. (2019). Measuring higher education students’ perceived stress: An IRT-based construct validity study of the PSS-10. Studies in Educational Evaluation., 63, 17–25
Hong, I., & Bonilha, H. S. (2017). Psychometric properties of upper extremity outcome measures validated by Rasch analysis: A systematic review. International Journal of Rehabilitation Research, 40(1), 1–10
Franchignoni, F., Giordano, A., Sartorio, F., Vercelli, S., Pascariello, B., & Ferriero, G. (2010). Suggestions for refinement of the Disabilities of the Arm, Shoulder and Hand Outcome Measure (DASH): a factor analysis and Rasch validation study. Archives of Physical Medicine and Rehabilitation, 91(9), 1370–1377
Jablecki, C. K., Andary, M. T., So, Y. T., Wilkins, D. E., & Williams, F. H. (1993). Literature review of the usefulness of nerve conduction studies and electromyography for the evaluation of patients with carpal tunnel syndrome. AAEM Quality Assurance Committee. Muscle Nerve., 16(12), 1392–1414
Mondelli, M., Reale, F., Sicurelli, F., & Padua, L. (2000). Relationship between the self-administered Boston questionnaire and electrophysiological findings in follow-up of surgically-treated carpal tunnel syndrome. J Hand Surg Br., 25(2), 128–134
Padua, L., Padua, R., Lo Monaco, M., Aprile, I., & Tonali, P. (1999). Multiperspective assessment of carpal tunnel syndrome: a multicenter study. Italian CTS Study Group. Neurology, 53(8), 1654–1659
Ortiz-Corredor, F., & Lopez-Monsalve, A. (2009). Using neurophysiological reference values as an approach to carpal tunnel syndrome diagnosis. Revista de Salud Pública (Bogotá, Colombia), 11(5), 794–801
Padua, L., LoMonaco, M., Gregori, B., Valente, E. M., Padua, R., & Tonali, P. (1997). Neurophysiological classification and sensitivity in 500 carpal tunnel syndrome hands. Acta Neurologica Scandinavica, 96(4), 211–217
Team RC. (2013). R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. http://www.R-project.org/.
Revelle W. (2016). psych: Procedures for Personality and Psychological Research. Northwestern University, Evanston, Illinois, USA: https://CRAN.R-project.org/package=psych Version = 1.6.9
Rosseel, Y. (2012). lavaan: An R package for structural equation modeling. Journal of Statistical Software., 48(2), 1–36
Andrich, D., Sheridan, B., & Luo, G. (2010). Rasch models for measurement: RUMM2030. RUMM Laboratory Pty Ltd.
Fabrigar, L. R., Wegener, D. T., MacCallum, R. C., & Strahan, E. J. (1999). Evaluating the use of exploratory factor analysis in psychological research. Psychological Methods, 4(3), 272–299
Hayton, J. C., Allen, D. G., & Scarpello, V. (2004). Factor retention decisions in exploratory factor analysis: A tutorial on parallel analysis. Organizational Research Methods., 7(2), 191–205
Timmerman, M. E., & Lorenzo-Seva, U. (2011). Dimensionality assessment of ordered polytomous items with parallel analysis. Psychological Methods, 16(2), 209–220
Revelle, W., & Rocklin, T. (1979). Very simple structure: an alternative procedure for estimating the optimal number of interpretable factors. Multivariate Behaviour Research, 14(4), 403–414
Velicer, W. F. (1976). Determining the number of components from the matrix of partial correlations. Psychometrika, 24(2), 321–327
Goldberg, L. R., & Velicer, W. F. (2006). Principles of exploratory factor analysis. In S. Strack (Ed.), Differentiating normal and abnormal personality. (pp. 209–237). Springer Publishing Co.
Lee, C. T., Zhang, G., & Edwards, M. C. (2012). Ordinary least squares estimation of parameters in exploratory factor analysis with ordinal data. Multivariate Behaviour Research, 47(2), 314–339
Schmitt, T. A. (2011). Current methodological considerations in exploratory and confirmatory factor analysis. Journal of Psychoeducational Assessment, 29(4), 304–321
Krijnen, W. P. (1996). Algorithms for unweighted least-squares factor analysis. Computational Statistics & Data Analysis, 21(2), 133–147
Guadagnoli, E., & Velicer, W. F. (1988). Relation of sample size to the stability of component patterns. Psychological Bulletin, 103(2), 265–275
Christensen, K. B., Makransky, G., & Horton, M. (2017). Critical values for Yen’s Q3: identification of local dependence in the Rasch model using residual correlations. Applied Psychological Measurement, 41(3), 178–194
Pomeroy, I. M., Tennat, A., Mills, R. J., & Young, C. A. (2020). The WHOQOL-BREF: A modern psychometric evaluation of its internal construct validity in people with multiple sclerosis. Quality of Life Research, 29(7), 1961–1972
Rodriguez, A., Reise, S. P., & Haviland, M. G. (2016). Evaluating bifactor models: Calculating and interpreting statistical indices. Psychological Methods, 21(2), 137–150
Andrich, D. (2016). Components of variance of scales with a bifactor subscale structure from Twwo calculations of α. Educational Measurement: Issues and Practice., 35(4), 24–30
Leite, J. C., Jerosch-Herold, C., & Song, F. (2006). A systematic review of the psychometric properties of the Boston Carpal Tunnel Questionnaire. BMC Musculoskeletal Disorders, 7, 78
Maeda, Y., Kettner, N., Kim, J., Kim, H., Cina, S., Malatesta, C., et al. (2016). Primary somatosensory/motor cortical thickness distinguishes paresthesia-dominant from pain-dominant carpal tunnel syndrome. Pain, 157(5), 1085–1093
You, H., Simmons, Z., Freivalds, A., Kothari, M. J., & Naidu, S. H. (1999). Relationships between clinical symptom severity scales and nerve conduction measures in carpal tunnel syndrome. Muscle and Nerve, 22(4), 497–501
Nora, D. B., Becker, J., Ehlers, J. A., & Gomes, I. (2005). What symptoms are truly caused by median nerve compression in carpal tunnel syndrome? Clinical Neurophysiology, 116(2), 275–283
Nora, D. B., Becker, J., Ehlers, J. A., & Gomes, I. (2004). Clinical features of 1039 patients with neurophysiological diagnosis of carpal tunnel syndrome. Clinical Neurology and Neurosurgery, 107(1), 64–69
Alfonso, C., Jann, S., Massa, R., & Torreggiani, A. (2010). Diagnosis, treatment and follow-up of the carpal tunnel syndrome: a review. Neurological Sciences, 31(3), 243–252
Peters, S., Johnston, V., Hines, S., Ross, M., & Coppieters, M. (2016). Prognostic factors for return-to-work following surgery for carpal tunnel syndrome: a systematic review. JBI Database of Systematic Reviews and Implementation Reports, 14(9), 135–216
Luckhaupt, S. E., Dahlhamer, J. M., Ward, B. W., Sweeney, M. H., Sestito, J. P., & Calvert, G. M. (2013). Prevalence and work-relatedness of carpal tunnel syndrome in the working population, United States, 2010 National Health Interview Survey. American Journal of Industrial Medicine, 56(6), 615–624
Dimberg, E. L. (2011). The office evaluation of weakness. Seminars in Neurology, 31(1), 115–130
Stone, J., & Aybek, S. (2016). Functional limb weakness and paralysis. Handbook of Clinical Neurology, 139, 213–228
Multanen, J., Ylinen, J., Karjalainen, T., Ikonen, J., Häkkinen, A., & Repo, J. P. (2020). Structural validity of th Boston Carpal Tunnel Questionnaire and its short version, the 6-Item CTS symptoms scale: A Rasch analysis one year after surgery. BMC Musculoskeletal Disorders, 21(1), 609
Acknowledgements
Authors would like to thank Alvaro J. Ruiz-Morales, Martin Rondon-Sepulveda and Ivan Alfredo Mendoza for their advice on methodology
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors of this manuscript declare that they have no conflict of interest.
Ethical approval
No animal subjects were involved in the research. All subjects attend to authors’ institution sign anonymity and confidentiality forms. This project was approved by authors’ institution Committee on Medical Ethics and Research (Number 2018-90).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Mendoza-Pulido, C., Ortiz-Corredor, F. Measurement properties of the Boston Carpal Tunnel Questionnaire in subjects with neurophysiological confirmation of carpal tunnel syndrome: a Rasch analysis perspective. Qual Life Res 30, 2697–2710 (2021). https://doi.org/10.1007/s11136-021-02860-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-021-02860-y