Abstract
Purpose
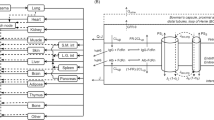
An in vitro dynamic pharmacokinetic (PK) cell culture system was developed to more precisely simulate physiologic nanoparticle/drug exposure.
Methods
A dynamic PK cell culture system was developed to more closely reflect physiologic nanoparticle/drug concentrations that are changing with time. Macrophages were cultured in standard static and PK cell culture systems with rifampin (RIF; 5 μg/ml) or β-glucan, chitosan coated, poly(lactic-co-glycolic) acid (GLU-CS-PLGA) nanoparticles (RIF equivalent 5 μg/ml) for 6 h. Intracellular RIF concentrations were measured by UPLC/MS. Antimicrobial activity against M. smegmatis was tested in both PK and static systems.
Results
The dynamic PK cell culture system mimics a one-compartment elimination pharmacokinetic profile to properly mimic in vivo extracellular exposure. GLU-CS-PLGA nanoparticles increased intracellular RIF concentration by 37% compared to free drug in the dynamic cell culture system. GLU-CS-PLGA nanoparticles decreased M. smegmatis colony forming units compared to free drug in the dynamic cell culture system.
Conclusions
The PK cell culture system developed herein enables more precise simulation of human PK exposure (i.e., drug dosing and drug elimination curves) based on previously obtained PK parameters.




Similar content being viewed by others
Abbreviations
- CFU :
-
Colony forming units
- CS:
-
Chitosan
- DAPI:
-
4′,6-diamidino-2-phenylindole
- DCM:
-
Dichloromethane
- DLS:
-
Dynamic light scattering
- GLU:
-
1,3 β-glucan
- HIV:
-
Human immunodeficiency virus
- PK:
-
Pharmacokinetic
- PLGA:
-
Poly(lactic-co-glycolic) acid
- PVA:
-
Poly(vinyl alcohol)
- RIF:
-
Rifampin
- RifP:
-
Rifapentine
- TB:
-
Tuberculosis
- TEM:
-
Transmission electron microscope
- UPLC-MS/MS :
-
Ultra performance liquid chromatography-tandem mass spectrometry
References
Ross KA, Brenza TM, Binnebose AM, Phanse Y, Kanthasamy AG, Gendelman HE, et al. Nano-enabled delivery of diverse payloads across complex biological barriers. J Control Release. 2015:S0168–3659.
Zahoor A, Sharma S, Khuller GK. Inhalable alginate nanoparticles as antitubercular drug carriers against experimental tuberculosis. Int J Antimicrob Agents. 2005;26(4):298–303.
Semete B, Booysen L, Kalombo L, Ramalapa B, Hayeshi R, Swai HS. Effects of protein binding on the biodistribution of PEGylated PLGA nanoparticles post oral administration. Int J Pharm. 2012;424(1–2):115–20.
Semete B, Booysen L, Lemmer Y, Kalombo L, Katata L, Verschoor J, et al. In vivo evaluation of the biodistribution and safety of PLGA nanoparticles as drug delivery systems. Nanomedicine. 2010;6(5):662–71.
Edagwa BJ, Guo D, Puligujja P, Chen H, McMillan J, Liu X, et al. Long-acting antituberculous therapeutic nanoparticles target macrophage endosomes. FASEB J. 2014;28(12):5071–82.
Kalluru R, Fenaroli F, Westmoreland D, Ulanova L, Maleki A, Roos N, et al. Poly(lactide-co-glycolide)-rifampicin nanoparticles efficiently clear Mycobacterium bovis BCG infection in macrophages and remain membrane-bound in phago-lysosomes. J Cell Sci. 2013;126(Pt 14):3043–54.
Dube A, Reynolds J, Law WC, Maponga CC, Prasad PN, Morse GD. Multimodal nanoparticles that provide immunomodulation and intracellular drug delivery for infectious diseases. Nanomedicine. 2014;10(4):831–8.
Parumasivam T, Leung S, Quan D, Triccas J, Britton W, Chan H. Rifapentine-loaded PLGA microparticles for tuberculosis inhaled therapy: preparation and in vitro aerosol characterization. Eur J Pharm Sci. 2016;88:1–11.
Sarkar S, Leo BF, Carranza C, Chen S, Rivas-Santiago C, Porter AE, et al. Modulation of human macrophage responses to Mycobacterium tuberculosis by silver nanoparticles of different size and surface modification. PLoS One. 2015;10(11):e0143077.
Jaryal N, Kaur H. Plumbago auriculata leaf extract-mediated AgNPs and its activities as antioxidant, anti-TB and dye degrading agents. J Biomater Sci Polym Ed. 2017:1–12.
Jafari A, Mosavari N, Movahedzadeh F, Nodooshan SJ, Safarkar R, Moro R, et al. Bactericidal impact of Ag, ZnO and mixed AgZnO colloidal nanoparticles on H37Rv Mycobacterium tuberculosis phagocytized by THP-1 cell lines. Microb Pathog. 2017;110:335–44.
Gopala Krishna P, Paduvarahalli Ananthaswamy P, Trivedi P, Chaturvedi V, Bhangi Mutta N, Sannaiah A, et al. Antitubercular activity of ZnO nanoparticles prepared by solution combustion synthesis using lemon juice as bio-fuel. Mater Sci Eng C Mater Biol Appl. 2017;75:1026–33.
Owens Iii DE, Peppas NA. Opsonization, biodistribution, and pharmacokinetics of polymeric nanoparticles. Int J Pharm. 2006;307(1):93–102.
Choi SR, Britigan BE, Moran DM, Narayanasamy P. Gallium nanoparticles facilitate phagosome maturation and inhibit growth of virulent Mycobacterium tuberculosis in macrophages. PLoS One. 2017;12(5):e0177987.
Rawal T, Kremer L, Halloum I, Butani S. Dry-powder inhaler formulation of rifampicin: an improved targeted delivery system for alveolar tuberculosis. J Aerosol Med Pulm Drug Deliv. 2017;30:388–98.
Rawal T, Parmar R, Tyagi RK, Butani S. Rifampicin loaded chitosan nanoparticle dry powder presents an improved therapeutic approach for alveolar tuberculosis. Colloids Surf B: Biointerfaces. 2017;154:321–30.
Gaspar DP, Faria V, Goncalves LM, Taboada P, Remunan-Lopez C, Almeida AJ. Rifabutin-loaded solid lipid nanoparticles for inhaled antitubercular therapy: physicochemical and in vitro studies. Int J Pharm. 2016;497(1–2):199–209.
Clemens DL, Lee BY, Xue M, Thomas CR, Meng H, Ferris D, et al. Targeted intracellular delivery of antituberculosis drugs to Mycobacterium tuberculosis-infected macrophages via functionalized mesoporous silica nanoparticles. Antimicrob Agents Chemother. 2012;56(5):2535–45.
Anisimova YV, Gelperina SI, Peloquin CA, Heifets LB. Nanoparticles as antituberculosis drugs carriers: effect on activity against Mycobacterium tuberculosis in human monocyte-derived macrophages. J Nanopart Res. 2000;2:165–71.
Zhou TLZ, Puligujja P, Palandri D, Hilaire J, Arainga M, Smith N, et al. Optimizing the preparation and stability of decorated antiretroviral drug nanocrystals. Nanomedicine. 2018;13(8):871–85.
Abolhasani MH, Safavi M, Goodarzi MT, Kassaee SM, Azin M. Identification and anti-cancer activity in 2D and 3D cell culture evaluation of an Iranian isolated marine microalgae Picochlorum sp. RCC486. Daru. 2018;26:105–16.
Bonnier F, Keating ME, Wrobel TP, Majzner K, Baranska M, Garcia-Munoz A, et al. Cell viability assessment using the Alamar blue assay: a comparison of 2D and 3D cell culture models. Toxicol in Vitro. 2015;29(1):124–31.
Hess MW, Pfaller K, Ebner HL, Beer B, Hekl D, Seppi T. 3D versus 2D cell culture implications for electron microscopy. Methods Cell Biol. 2010;96:649–70.
Database National Center for Biotechnology Information. Rifampicin [Available from: https://pubchem.ncbi.nlm.nih.gov/compound/Rifampicin]. Accessed 12/21/2018.
Horita Y, Alsultan A, Kwara A, Antwi S, Enimil A, Ortsin A, et al. Evaluation of the adequacy of WHO revised dosages of the first-line Antituberculosis drugs in children with tuberculosis using population pharmacokinetic modeling and simulations. Antimicrob Agents Chemother. 2018;62(9).
Prasad PN. Introduction to nanomedicine and nanobioengineering. New Jersey: Wiley; 2012.
Essaji Y, Yang Y, Albert CJ, Ford DA, Brown RJ. Hydrolysis products generated by lipoprotein lipase and endothelial lipase differentially impact THP-1 macrophage cell signalling pathways. Lipids. 2013;48(8):769–78.
Kim SHCS, Lim YJ, Choi JA, Lee J, Go D, Song CH. Phagocytosis influences the intracellular survival of Mycobacterium smegmatis via the endoplasmic reticulum stress response. Cell Biosci. 2018;8(52).
The Advantages of Hollow Fiber Bioreactors in Cell Culture [Available from: https://www.fibercellsystems.com/advantage/]. Accessed 12/21/2018.
Acknowledgments and Disclosures
Research reported in this publication was supported in part by 1R01AI129649-01A1 (NIAID) (JR); 1R56AI114298 (NIAID) (JR); University of Rochester Center for AIDS Research (CFAR) grant P30AI078498 (NIAID) (HK); and through a supplement to the University at Buffalo Pharmacology Specialty Laboratory, funded by UM1AI068634, UM1AI068636, and UM1AI106701 (NIAID)(GDM). HK was supported by Ruth L. Kirschstein National Research Service Award (NRSA) Institutional Research Training Grant 1T32GM099607 and UL1TR001412 (NCATS) (JR, HK). Research reported in this publication was supported in part by equipment donated by Waters Corporation. We acknowledge Dr. Martin Pavelka, University of Rochester, for the gernerous donation of M. Smegmatis. The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH.
Author information
Authors and Affiliations
Corresponding author
Additional information
Guest Editor: Admire Dube
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 1276 kb)
Rights and permissions
About this article
Cite this article
Kutscher, H.L., Morse, G.D., Prasad, P.N. et al. In vitro Pharmacokinetic Cell Culture System that Simulates Physiologic Drug and Nanoparticle Exposure to Macrophages. Pharm Res 36, 44 (2019). https://doi.org/10.1007/s11095-019-2576-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11095-019-2576-9