Abstract
Background
Intracranial solitary fibrous tumors (SFTs), formerly hemangiopericytomas (HPCs), are rare, aggressive dural-based mesenchymal tumors. While adjuvant radiation therapy has been suggested to improve local tumor control (LTC), especially after subtotal resection, the role of postoperative stereotactic radiosurgery (SRS) and the optimal SRS dosing strategy remain poorly defined.
Methods
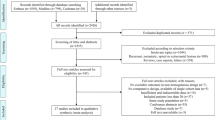
PubMed, EMBASE, and Web of Science were systematically searched according to PRISMA guidelines for studies describing postoperative SRS for intracranial SFTs. The search strategy was defined in the authors’ PROSPERO protocol (CRD42023454258).
Results
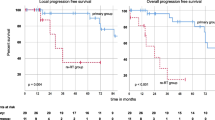
15 studies were included describing 293 patients harboring 476 intracranial residual or recurrent SFTs treated with postoperative SRS. At a mean follow-up of 21–77 months, LTC rate after SRS was 46.4–93% with a mean margin SRS dose of 13.5–21.7 Gy, mean maximum dose of 27-39.6 Gy, and mean isodose at the 42.5–77% line. In pooled analysis of individual tumor outcomes, 18.7% of SFTs demonstrated a complete SRS response, 31.7% had a partial response, 18.9% remained stable (overall LTC rate of 69.3%), and 30.7% progressed. When studies were stratified by margin dose, a mean margin dose > 15 Gy showed an improvement in LTC rate (74.7% versus 65.7%).
Conclusions
SRS is a safe and effective treatment for intracranial SFTs. In the setting of measurable disease, our pooled data suggests a potential dose response of improving LTC with increasing SRS margin dose. Our improved understanding of the aggressive biology of SFTs and the tolerated adjuvant SRS parameters supports potentially earlier use of SRS in the postoperative treatment paradigm for intracranial SFTs.


Similar content being viewed by others
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Board WCTE (2021) World Health Organization Classification of Tumours of the Central Nervous System. International Agency for Research on Cancer, Lyon
Chmielecki J, Crago AM, Rosenberg M, O’Connor R, Walker SR, Ambrogio L, Auclair D, McKenna A, Heinrich MC, Frank DA, Meyerson M (2013) Whole-exome sequencing identifies a recurrent NAB2-STAT6 fusion in solitary fibrous tumors. Nat Genet 45:131–132. https://doi.org/10.1038/ng.2522
Wu Y, Zhao T, Cai Y, Zheng M, Zhang Y, Qu Y, Cai Q (2023) Clinical outcomes of solitary fibrous tumors and hemangiopericytomas and risk factors related to recurrence and survival based on the 2021 WHO classification of central nervous system tumors. J Neurosurg 1–11. https://doi.org/10.3171/2023.4.JNS23147
Kinslow CJ, Bruce SS, Rae AI, Sheth SA, McKhann GM, Sisti MB, Bruce JN, Sonabend AM, Wang TJC (2018) Solitary-fibrous tumor/hemangiopericytoma of the central nervous system: a population-based study. J Neurooncol 138:173–182. https://doi.org/10.1007/s11060-018-2787-7
Rutkowski MJ, Sughrue ME, Kane AJ, Aranda D, Mills SA, Barani IJ, Parsa AT (2010) Predictors of mortality following treatment of intracranial hemangiopericytoma. J Neurosurg 113:333–339. https://doi.org/10.3171/2010.3.Jns091882
Fountas KN, Kapsalaki E, Kassam M, Feltes CH, Dimopoulos VG, Robinson JS, Smith JR (2006) Management of intracranial meningeal hemangiopericytomas: outcome and experience. Neurosurg Rev 29:145–153. https://doi.org/10.1007/s10143-005-0001-9
Melone AG, D’Elia A, Santoro F, Salvati M, Delfini R, Cantore G, Santoro A (2014) Intracranial hemangiopericytoma–our experience in 30 years: a series of 43 cases and review of the literature. World Neurosurg 81:556–562. https://doi.org/10.1016/j.wneu.2013.11.009
Jääskeläinen J, Servo A, Haltia M, Wahlström T, Valtonen S (1985) Intracranial hemangiopericytoma: radiology, Surgery, radiotherapy, and outcome in 21 patients. Surg Neurol 23:227–236. https://doi.org/10.1016/0090-3019(85)90087-4
Vuorinen V, Sallinen P, Haapasalo H, Visakorpi T, Kallio M, Jääskeläinen J (1996) Outcome of 31 intracranial haemangiopericytomas: poor predictive value of cell proliferation indices. Acta Neurochir (Wien) 138:1399–1408. https://doi.org/10.1007/bf01411118
Chacko G, Chacko AG, Rajshekhar V, Muliyil JP (2006) Intracranial hemangiopericytomas: correlation of topoisomerase IIalpha expression with biologic behavior. Surg Neurol 65:11–17. https://doi.org/10.1016/j.surneu.2005.08.013
Schiariti M, Goetz P, El-Maghraby H, Tailor J, Kitchen N (2011) Hemangiopericytoma: long-term outcome revisited. Clinical article. J Neurosurg 114:747–755. https://doi.org/10.3171/2010.6.Jns091660
Sonabend AM, Zacharia BE, Goldstein H, Bruce SS, Hershman D, Neugut AI, Bruce JN (2014) The role for adjuvant radiotherapy in the treatment of hemangiopericytoma: a Surveillance, Epidemiology, and end results analysis. J Neurosurg 120:300–308. https://doi.org/10.3171/2013.10.Jns13113
Dufour H, Métellus P, Fuentes S, Murracciole X, Régis J, Figarella-Branger D, Grisoli F (2001) Meningeal hemangiopericytoma: a retrospective study of 21 patients with special review of postoperative external radiotherapy. Neurosurgery 48:756–762 discussion 762. https://doi.org/10.1097/00006123-200104000-00011
Liu J, Wu S, Zhao K, Wang J, Shu K, Lei T (2022) Clinical features, management, and prognostic factors of Intracranial Solitary Fibrous Tumor. Front Oncol 12:915273. https://doi.org/10.3389/fonc.2022.915273
Ghia AJ, Chang EL, Allen PK, Mahajan A, Penas-Prado M, McCutcheon IE, Brown PD (2013) Intracranial hemangiopericytoma: patterns of failure and the role of radiation therapy. Neurosurgery 73:624–630 discussion 630. https://doi.org/10.1227/neu.0000000000000064
Ghose A, Guha G, Kundu R, Tew J, Chaudhary R (2017) CNS hemangiopericytoma: a systematic review of 523 patients. Am J Clin Oncol 40:223–227. https://doi.org/10.1097/coc.0000000000000146
Galanis E, Buckner JC, Scheithauer BW, Kimmel DW, Schomberg PJ, Piepgras DG (1998) Management of recurrent meningeal hemangiopericytoma. Cancer 82:1915–1920
Kondziolka D, Flickinger JC, Lunsford LD (2008) The principles of skull base radiosurgery. Neurosurg Focus 24:E11. https://doi.org/10.3171/foc/2008/24/5/e11
Coffey RJ, Cascino TL, Shaw EG (1993) Radiosurgical treatment of recurrent hemangiopericytomas of the meninges: preliminary results. J Neurosurg 78:903–908. https://doi.org/10.3171/jns.1993.78.6.0903
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Akl EA, Brennan SE, Chou R, Glanville J, Grimshaw JM, Hróbjartsson A, Lalu MM, Li T, Loder EW, Mayo-Wilson E, McDonald S, McGuinness LA, Stewart LA, Thomas J, Tricco AC, Welch VA, Whiting P, Moher D (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Int J Surg 88:105906. https://doi.org/10.1016/j.ijsu.2021.105906
Schardt C, Adams MB, Owens T, Keitz S, Fontelo P (2007) Utilization of the PICO framework to improve searching PubMed for clinical questions. BMC Med Inform Decis Mak 7:16. https://doi.org/10.1186/1472-6947-7-16
Munn Z, Barker TH, Moola S, Tufanaru C, Stern C, McArthur A, Stephenson M, Aromataris E (2020) Methodological quality of case series studies: an introduction to the JBI critical appraisal tool. JBI Evid Synth 18:2127–2133. https://doi.org/10.11124/jbisrir-d-19-00099
Wells GA SB, O’Connell D, Peterson J, Welch V, Losos M, Tugwell P (2011) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses
Chang SD, Sakamoto GT (2003) The role of radiosurgery for hemangiopericytomas. Neurosurg Focus 14:e14. https://doi.org/10.3171/foc.2003.14.5.15
Cohen-Inbar O, Lee CC, Mousavi SH, Kano H, Mathieu D, Meola A, Nakaji P, Honea N, Johnson M, Abbassy M, Mohammadi AM, Silva D, Yang HC, Grills I, Kondziolka D, Barnett GH, Lunsford LD, Sheehan J (2017) Stereotactic radiosurgery for intracranial hemangiopericytomas: a multicenter study. J Neurosurg 126:744–754. https://doi.org/10.3171/2016.1.Jns152860
Copeland WR, Link MJ, Stafford SL, Pollock BE (2014) Single-fraction stereotactic radiosurgery of meningeal hemangiopericytomas. J Neurooncol 120:95–102. https://doi.org/10.1007/s11060-014-1521-3
Ecker RD, Marsh WR, Pollock BE, Kurtkaya-Yapicier O, McClelland R, Scheithauer BW, Buckner JC (2003) Hemangiopericytoma in the central nervous system: treatment, pathological features, and long-term follow up in 38 patients. J Neurosurg 98:1182–1187. https://doi.org/10.3171/jns.2003.98.6.1182
Huang L, Bai J, Zhang Y, Cui Z, Zhang Z, Li J, Wang J, Yu X, Ling Z, Qu B, Pan L (2021) Treatment of residual, recurrent, or metastatic intracranial Hemangiopericytomas with Stereotactic Radiotherapy using CyberKnife. Front Oncol 11:577054. https://doi.org/10.3389/fonc.2021.577054
Iwai Y, Yamanaka K (2009) Gamma knife radiosurgery for other primary intra-axial tumors. Prog Neurol Surg 22:129–141. https://doi.org/10.1159/000163395
Kano H, Niranjan A, Kondziolka D, Flickinger JC, Lunsford LD (2008) Adjuvant stereotactic radiosurgery after resection of intracranial hemangiopericytomas. Int J Radiat Oncol Biol Phys 72:1333–1339. https://doi.org/10.1016/j.ijrobp.2008.03.024
Kim JW, Kim DG, Chung HT, Paek SH, Kim YH, Han JH, Park CK, Kim CY, Jung HW (2010) Gamma Knife stereotactic radiosurgery for intracranial hemangiopericytomas. J Neurooncol 99:115–122. https://doi.org/10.1007/s11060-010-0114-z
Kim BS, Kong DS, Seol HJ, Nam DH, Lee JI (2017) Gamma knife radiosurgery for residual or recurrent intracranial hemangiopericytomas. J Clin Neurosci 35:35–41. https://doi.org/10.1016/j.jocn.2016.10.002
Olson C, Yen CP, Schlesinger D, Sheehan J (2010) Radiosurgery for intracranial hemangiopericytomas: outcomes after initial and repeat Gamma Knife Surgery. J Neurosurg 112:133–139. https://doi.org/10.3171/2009.3.Jns0923
Sheehan J, Kondziolka D, Flickinger J, Lunsford LD (2002) Radiosurgery for treatment of recurrent intracranial hemangiopericytomas. Neurosurgery 51:905–910 discussion 910 – 901. https://doi.org/10.1097/00006123-200210000-00008
Sun S, Liu A, Wang C (2009) Gamma knife radiosurgery for recurrent and residual meningeal hemangiopericytomas. Stereotact Funct Neurosurg 87:114–119. https://doi.org/10.1159/000202978
Tsugawa T, Mori Y, Kobayashi T, Hashizume C, Shibamoto Y, Wakabayashi T (2014) Gamma knife stereotactic radiosurgery for intracranial hemangiopericytoma. J Radiosurg SBRT 3:29–35
Veeravagu A, Jiang B, Patil CG, Lee M, Soltys SG, Gibbs IC, Chang SD (2011) CyberKnife stereotactic radiosurgery for recurrent, metastatic, and residual hemangiopericytomas. J Hematol Oncol 4:26. https://doi.org/10.1186/1756-8722-4-26
Xiao J, Xu L, Ding Y, Wang W, Chen F, Zhou Y, Zhang F, Zhou Q, Wu X, Li J, Liang L, Jen YM (2021) Does post-operative radiotherapy improve the treatment outcomes of intracranial hemangiopericytoma? A retrospective study. BMC Cancer 21:915. https://doi.org/10.1186/s12885-021-08594-x
Sung KS, Moon JH, Kim EH, Kang SG, Kim SH, Suh CO, Kim SH, Lee KS, Chang WS, Chang JH (2018) Solitary fibrous tumor/hemangiopericytoma: treatment results based on the 2016 WHO classification. J Neurosurg 1–8. https://doi.org/10.3171/2017.9.Jns171057
Kim J (2017) The impact of postoperative radiation therapy on patterns of failure and survival improvement in patients with intracranial hemangiopericytoma. Neurooncology 19:iii117. https://doi.org/10.1093/neuonc/nox036
Stout AP, Murray MR (1942) HEMANGIOPERICYTOMA: A VASCULAR TUMOR FEATURING ZIMMERMANN’S PERICYTES. Ann Surg 116:26–33. https://doi.org/10.1097/00000658-194207000-00004
Louis DN, Perry A, Reifenberger G, von Deimling A, Figarella-Branger D, Cavenee WK, Ohgaki H, Wiestler OD, Kleihues P, Ellison DW (2016) The 2016 World Health Organization Classification of Tumors of the Central Nervous System: a summary. Acta Neuropathol 131:803–820. https://doi.org/10.1007/s00401-016-1545-1
Schweizer L, Koelsche C, Sahm F, Piro RM, Capper D, Reuss DE, Pusch S, Habel A, Meyer J, Göck T, Jones DT, Mawrin C, Schittenhelm J, Becker A, Heim S, Simon M, Herold-Mende C, Mechtersheimer G, Paulus W, König R, Wiestler OD, Pfister SM, von Deimling A (2013) Meningeal hemangiopericytoma and solitary fibrous tumors carry the NAB2-STAT6 fusion and can be diagnosed by nuclear expression of STAT6 protein. Acta Neuropathol 125:651–658. https://doi.org/10.1007/s00401-013-1117-6
Jo VY, Fletcher CD (2014) WHO classification of soft tissue tumours: an update based on the 2013 (4th) edition. Pathology 46:95–104. https://doi.org/10.1097/pat.0000000000000050
Trifiletti DM, Mehta GU, Grover S, Sheehan JP (2017) Clinical management and survival of patients with central nervous system hemangiopericytoma in the National Cancer Database. J Clin Neurosci 44:169–174. https://doi.org/10.1016/j.jocn.2017.06.036
Tobias S, Jahshan S, Grober Y, Soustiel JF (2022) Skull base hemangiopericytomas. Acta Neurol Belg 122:1537–1545. https://doi.org/10.1007/s13760-021-01812-0
Ramakrishna R, Rostomily R, Sekhar L, Rockhill J, Ferreira M (2014) Hemangiopericytoma: radical resection remains the cornerstone of therapy. J Clin Neurosci 21:612–615. https://doi.org/10.1016/j.jocn.2013.08.006
Kim BS, Kim Y, Kong DS, Nam DH, Lee JI, Suh YL, Seol HJ (2018) Clinical outcomes of intracranial solitary fibrous Tumor and hemangiopericytoma: analysis according to the 2016 WHO classification of central nervous system tumors. J Neurosurg 129:1384–1396. https://doi.org/10.3171/2017.7.Jns171226
Jha N, McNeese M, Barkley HT Jr., Kong J (1987) Does radiotherapy have a role in hemangiopericytoma management? Report of 14 new cases and a review of the literature. Int J Radiat Oncol Biol Phys 13:1399–1402. https://doi.org/10.1016/0360-3016(87)90236-7
Staples JJ, Robinson RA, Wen BC, Hussey DH (1990) Hemangiopericytoma–the role of radiotherapy. Int J Radiat Oncol Biol Phys 19:445–451. https://doi.org/10.1016/0360-3016(90)90556-y
Kwon SM, Na MK, Choi KS, Lim TH, Shin H, Lee J, Lee H, Kim W, Cho Y, Kim JG, Ahn C, Jang BH (2023) Impact of extent of resection and postoperative radiotherapy on survival outcomes in intracranial solitary fibrous tumors: a systematic review and meta-analysis. Neurosurg Rev 46:138. https://doi.org/10.1007/s10143-023-02046-9
Konar S, Jayan M, Shukla D, Bhat DI, Nishant S, Nandeesh BN, Devi BI (2021) The risks factor of recurrence after skull base hemangiopericytoma management: a retrospective case series and review of literature. Clin Neurol Neurosurg 208:106866. https://doi.org/10.1016/j.clineuro.2021.106866
Spina A, Boari N, Gagliardi F, Donofrio CA, Franzin A, Mortini P (2016) The current role of Gamma Knife radiosurgery in the management of intracranial haemangiopericytoma. Acta Neurochir (Wien) 158:635–642. https://doi.org/10.1007/s00701-016-2742-3
Lee A, Sidiqi B, Wang A, Safdieh J, Schreiber D (2018) Patterns of care and outcomes of postoperative radiation for intracranial hemangiopericytoma in United States hospitals. Clin Neurol Neurosurg 167:1–5. https://doi.org/10.1016/j.clineuro.2018.02.004
Guthrie BL, Ebersold MJ, Scheithauer BW, Shaw EG (1989) Meningeal hemangiopericytoma: histopathological features, treatment, and long-term follow-up of 44 cases. Neurosurgery 25:514–522
Nair R, Panettieri V, Chang JH, Dally M (2018) Post-operative stereotactic radiotherapy for the treatment of intracranial haemangiopericytoma: ‘A study of dose and outcome’. J Med Imaging Radiat Oncol 62:573–577. https://doi.org/10.1111/1754-9485.12745
Li Q, Deng W, Sun P (2022) Effect of different treatments for Intracranial Solitary Fibrous tumors: retrospective analysis of 31 patients. World Neurosurg 166:e60–e69. https://doi.org/10.1016/j.wneu.2022.06.089
Allen AJ, Labella DA, Richardson KM, Sheehan JP, Kersh CR (2022) Recurrent Solitary Fibrous Tumor (Intracranial Hemangiopericytoma) treated with a Novel Combined-Modality Radiosurgery technique: a Case Report and Review of the literature. Front Oncol 12:907324. https://doi.org/10.3389/fonc.2022.907324
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
Manuscript drafting (DG, JDB, HD, TW, PU); Figure and table design (DG, TW, PU, TGW, BC, MS, ARD); Manuscript editing and revision (DG, JDB, HD, TW, ETQ, BC, YZ, AG, SS, MS, ARD); Literature review (DG, JDB, HD, TW, TGW, ETQ, BC); Data Analysis (DG, JDB, HD, PU, TGW, ETQ, BC); Research team management and oversight (DG, ETQ, YZ, AG, SS, MS, ARD).
Corresponding author
Ethics declarations
Competing interests
The authors declare that this research was conducted in the absence of any commercial, financial, or other non-financial relationships that could be construed as a competing interest or a conflict of interest.
Ethics approval
No ethical approval was required for this systematic review of existing published literature.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Golub, D., McBriar, J.D., Donaldson, H. et al. Postoperative stereotactic radiosurgery for intracranial solitary fibrous tumors: systematic review and pooled quantitative analysis. J Neurooncol 165, 229–239 (2023). https://doi.org/10.1007/s11060-023-04499-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-023-04499-w