Abstract
Purpose
Therapeutic intervention at glioblastoma (GBM) progression, as defined by current assessment criteria, is arguably too late as second-line therapies fail to extend survival. Still, most GBM trials target recurrent disease. We propose integration of a novel imaging biomarker to more confidently and promptly define progression and propose a critical timepoint for earlier intervention to extend therapeutic exposure.
Methods
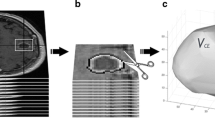
A retrospective review of 609 GBM patients between 2006 and 2019 yielded 135 meeting resection, clinical, and imaging inclusion criteria. We qualitatively and quantitatively analyzed 2000+ sequential brain MRIs (initial diagnosis to first progression) for development of T2 FLAIR signal intensity (SI) within the resection cavity (RC) compared to the ventricles (V) for quantitative inter-image normalization. PFS and OS were evaluated using Kaplan–Meier curves stratified by SI. Specificity and sensitivity were determined using a 2 × 2 table and pathology confirmation at progression. Multivariate analysis evaluated SI effect on the hazard rate for death after adjusting for established prognostic covariates. Recursive partitioning determined successive quantifiers and cutoffs associated with outcomes. Neurological deficits correlated with SI.
Results
Seventy-five percent of patients developed SI on average 3.4 months before RANO-assessed progression with 84% sensitivity. SI-positivity portended neurological decline and significantly poorer outcomes for PFS (median, 10 vs. 15 months) and OS (median, 20 vs. 29 months) compared to SI-negative. RC/V ratio ≥ 4 was the most significant prognostic indicator of death.
Conclusion
Implications of these data are far-reaching, potentially shifting paradigms for glioma treatment response assessment, altering timepoints for salvage therapeutic intervention, and reshaping glioma clinical trial design.





Similar content being viewed by others
Data availability
All data supporting the findings presented in this manuscript are available upon reasonable request directly to the corresponding author, NG. These data are not part of public domain or database as they are of the patient protected medical record and doing so would compromise the privacy of the research participants.
References
Stupp R, Mason WP, van den Bent MJ et al (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med 352(10):987–996
Gilbert MR, Wang M, Aldape KD et al (2013) Dose-dense temozolomide for newly diagnosed glioblastoma: a randomized phase III clinical trial. J Clin Oncol 31(32):4085–4091
Gorlia T, Stupp R, Brandes AA et al (2012) New prognostic factors and calculators for outcome prediction in patients with recurrent glioblastoma: a pooled analysis of EORTC brain tumor group phase I and II clinical trials. Eur J Cancer 48(8):1176–1184
Ortega A, Sarmiento JM, Ly D et al (2016) Multiple resections and survival of recurrent glioblastoma patients in the temozolomide era. J Clin Neurosci 24:105–111
Wann A, Tully PA, Barnes EH et al (2018) Outcomes after second surgery for recurrent glioblastoma: a retrospective case–control study. J Neuro-Oncol 137(2):409–415
Wong ET, Hess KR, Gleason MJ et al (1999) Outcomes and prognostic factors in recurrent glioma patients enrolled onto phase II clinical trials. J Clin Oncol 17(8):2572–2578
Kamiya-Matsuoka C, Gilbert MR (2015) Treating recurrent glioblastoma: an update. CNS Oncol 4(2):91–104
Tipping M, Eickhoff J, Robins HI (2017) Clinical outcomes in recurrent glioblastoma with bevacizumab therapy: an analysis of the literature. J Clin Neurosci 44:101–106
Weller M, van den Bent M, Hopkins K et al (2014) EANO guideline for the diagnosis and treatment of anaplastic gliomas and glioblastoma. Lancet Oncol 15(9):e395–403
Nayak L, DeAngelis LM, Brandes AA et al (2017) The neurologic assessment in neuro-oncology (NANO) scale: a tool to assess neurologic function for integration into the response assessment in neuro-oncology (RANO) criteria. Neuro-Oncology 19(5):625–635
Marcucci F, Corti A (2012) How to improve exposure of tumor cells to drugs: promoter drugs increase tumor uptake and penetration of effector drugs. Adv Drug Deliv Rev 64(1):53–68
Reardon DA, Rich JN, Friedman HS, Bigner DD (2006) Recent advances in the treatment of malignant astrocytoma. J Clin Oncol 24(8):1253–1265
Wen PY, Kesari S (2008) Malignant gliomas in adults. N Engl J Med 359(5):492–507
de Souza CF, Sabedot TS, Malta TM et al (2018) A distinct DNA methylation shift in a subset of glioma CpG island methylator phenotypes during tumor recurrence. Cell Rep 23(2):637–651
Choi S, Yu Y, Grimmer MR, Wahl M, Chang SM, Costello JF (2018) Temozolomide-associated hypermutation in gliomas. Neuro Oncol 20(10):1300–1309
Kim EL, Sorokin M, Kantelhardt SR et al (2020) Intratumoral heterogeneity and longitudinal changes in gene expression predict differential drug sensitivity in newly diagnosed and recurrent glioblastoma. Cancers 12(2):E520
Jakola AS, Myrmel KS, Kloster R et al (2012) Comparison of a strategy favoring early surgical resection vs a strategy favoring watchful waiting in low-grade gliomas. JAMA 308(18):1881–1888
Chan TS, Hsu CC, Pai VC et al (2016) Metronomic chemotherapy prevents therapy-induced stromal activation and induction of tumor-initiating cells. J Exp Med 213(13):2967–2988
James K, Eisenhauer E, Christian M et al (1999) Measuring response in solid tumors: unidimensional versus bidimensional measurement. J Natl Cancer Inst 91(6):523–528
Macdonald DR, Cascino TL, Schold SC Jr, Cairncross JG (1990) Response criteria for phase II studies of supratentorial malignant glioma. J Clin Oncol 8(7):1277–1280
Wen PY, Macdonald DR, Reardon DA et al (2010) Updated response assessment criteria for high-grade gliomas: response assessment in neuro-oncology working group. J Clin Oncol 28(11):1963–1972
Galanis E, Buckner JC, Maurer MJ et al (2006) Validation of neuroradiologic response assessment in gliomas: measurement by RECIST, two-dimensional, computer-assisted tumor area, and computer-assisted tumor volume methods. Neuro-oncology 8(2):156–165
Therasse P, Arbuck SG, Eisenhauer EA et al (2000) New guidelines to evaluate the response to treatment in solid tumors: European Organization for Research and Treatment of Cancer, National Cancer Institute of the United States, National Cancer Institute of Canada. J Natl Cancer Inst 92(3):205–216
Ellingson BM, Bendszus M, Boxerman J et al (2015) Consensus recommendations for a standardized Brain Tumor Imaging Protocol in clinical trials. Neuro-oncology 17(9):1188–1198
Hamilton JD, Lin J, Ison C et al (2015) Dynamic contrast-enhanced perfusion processing for neuroradiologists: model-dependent analysis may not be necessary for determining recurrent high-grade glioma versus treatment effect. AJNR Am J Neuroradiol 36(4):686–693
O'Brien BJ, Colen RR (2014) Post-treatment imaging changes in primary brain tumors. Curr Oncol Rep 16(8):397
Gallego Perez-Larraya J, Lahutte M, Petrirena G et al (2012) Response assessment in recurrent glioblastoma treated with irinotecan-bevacizumab: comparative analysis of the Macdonald, RECIST, RANO, and RECIST + F criteria. Neuro-oncology 14(5):667–673
Winterstein M, Munter MW, Burkholder I, Essig M, Kauczor HU, Weber MA (2010) Partially resected gliomas: diagnostic performance of fluid-attenuated inversion recovery MR imaging for detection of progression. Radiology 254(3):907–916
Ito-Yamashita T, Nakasu Y, Mitsuya K, Mizokami Y, Namba H (2013) Detection of tumor progression by signal intensity increase on fluid-attenuated inversion recovery magnetic resonance images in the resection cavity of high-grade gliomas. Neurol Med Chir 53(7):496–500
Sarbu N, Oleaga L, Valduvieco I, Pujol T, Berenguer J (2016) Increased signal intensity in FLAIR sequences in the resection cavity can predict progression and progression-free survival in gliomas. Neurocirugia 27(6):269–276
Bette S, Gempt J, Huber T et al (2017) FLAIR signal increase of the fluid within the resection cavity after glioma surgery: generally valid as early recurrence marker? J Neurosurg 127:417–425
Sharma M, Juthani RG, Vogelbaum MA (2017) Updated response assessment criteria for high-grade glioma: beyond the MacDonald criteria. Chin Clin Oncol 6(4):37
Louis DN, Ohgaki H, Wiestler OD et al (2007) The 2007 WHO classification of tumours of the central nervous system. Acta Neuropathol 114(2):97–109
Louis DN, Perry A, Reifenberger G et al (2016) The 2016 world health organization classification of tumors of the central nervous system: a summary. Acta Neuropathol 131:803–820
Cihoric N, Tsikkinis A, Minniti G et al (2017) Current status and perspectives of interventional clinical trials for glioblastoma: analysis of ClinicalTrials.gov. Radiat Oncol 12:1
Reardon DA, Ballman KV, Buckner JC, Chang SM, Ellingson BM (2014) Impact of imaging measurements on response assessment in glioblastoma clinical trials. Neuro-Oncology 16:724–735
Henson JW, Ulmer S, Harris GJ (2008) Brain tumor imaging in clinical trials. AJNR Am J Neuroradiol 29:419–424
Chukwueke UN, Wen PY (2019) Use of the response assessment in neuro-oncology (RANO) criteria in clinical trials and clinical practice. CNS Oncol 8(1):28
Essig M, Metzner R, Bonsanto M et al (2001) Postoperative fluid-attenuated inversion recovery MR imaging of cerebral gliomas: initial results. Eur Radiol 11:2004–2010
Das S, Marsden PA (2013) Angiogenesis in glioblastoma. N Engl J Med 369(16):1561–1563
Gerson SL (2004) MGMT: its role in cancer aetiology and cancer therapeutics. Nat Rev Cancer 4(4):296–307
Sharma S, Salehi F, Scheithauer BW, Rotondo F, Syro LV, Kovacs K (2009) Role of MGMT in tumor development, progression, diagnosis, treatment and prognosis. Anticancer Res 29(10):3759–3768
Bell EH, Zhang P, Fisher BJ et al (2018) Association of MGMT promoter methylation status with survival outcomes in patients with high-risk glioma treated with radiotherapy and temozolomide: an analysis from the NRG Oncology/RTOG 0424 trial. JAMA Oncol 4(10):1405–1409
Sun M, Oh T, Ivan ME (2015) Survival impact of time to initiation of chemoradiotherapy after resection of newly diagnosed glioblastoma. J Neurosurg 122:1144–1150
Warren KT, Liu L, Liu Y, Milano MT, Walter KA (2019) The impact of timing of concurrent chemoradiation in patients with high-grade glioma in the era of the Stupp protocol. Front Oncol 9:18
Perry JR, Bélanger K, Mason WP et al (2010) Phase II trial of continuous dose-intense temozolomide in recurrent malignant glioma: RESCUE study. J Clin Oncol 28(12):2051–2057
Omuro A, Chan TA, Abrey LE et al (2013) Phase II trial of continuous low-dose temozolomide for patients with recurrent malignant glioma. Neuro-Oncology 15(2):242–250
Lee J, Park SH, Kim YZ (2018) Prognostic evaluation of neurological assessment of the neuro-oncology scale in glioblastoma patients. Brain Tumor Res Treat 6(1):22–30
Armstrong TS, Mendoza T, Gning I et al (2006) Validation of the MD anderson symptom inventory brain tumor module (MDASi-BT). J Neurooncol 80(1):27–35
Acknowledgements
We acknowledge Dr. Susan Chang, Director of the UCSF Division of Neuro-Oncology and Director of the 2019 Society for Neuro-Oncology Clinical Trials Course, Dr. Mark Gilbert, Chief of the Neuro-Oncology Branch (NOB) at the National Institutes of Health, Dr. Priya Kumthekar of Northwestern University Feinberg School of Medicine, and to Dr. Prakash Chinnaiyan, Professor, Oakland University William Beaumont School of Medicine for dedicating their time and critical review of the research. The members of the NRG Brain Tumor & Neurosurgery Committees, and the NCI Brain Malignancies Steering Committee for their involvement in critical assessment of this work. To Geisinger Research Institute leadership, Dr. David Ledbetter, and Department Chair, Dr. Neil Holland, for allowing the dedicated research time. Finally, thanks to my donors: Mr. Jeff Erdly, Mr. Jerry Sandel, The Lowe Family, and The Comp Family.
Funding
Geisinger Foundation, [01100000000000, Account #341020–752025] Philanthropic donations from Mr. Jeff Erdly, Mr. Jerry Sandel, Lowe Family, and Comp Family.
Author information
Authors and Affiliations
Contributions
NG, VP, MM, TC—Concept development as well as the below listed contributions. SB, YO, YH—Substantial involvement in the development of the draft manuscript, contributed important intellectual content, data interpretation as well as the below listed contributions. LL, JM, GM, SK, AC, ML, AM, JV, LN—Data interpretations and development of figures, critical revisions and discussions around important intellectual content. Final approval of the planned version for publication. All authors agreed to be accountable for all aspects of the work for accuracy and are committed to the integrity of the final product.
Corresponding author
Ethics declarations
Conflicts of interest
M. Mehta: Consulting for Karyopharm, Tocagen, Astra-Zeneca, Blue Earth Diagnostics, Celgene, Abbvie. Board of Directors: Oncoceutics. N. Gatson: Advisory Board for Novocure. Y. Odia: Advisory Board for Novocure and Abbvie and Trial Support: Novocure and BMS. All remaining authors declare that they have no conflicts of interest.
Ethics approval
As a retrospective study all treatments were part of routine care and thereby ethical approval was waived by the Geisinger Health Ethics Committee.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Gatson, N.T.N., Bross, S.P., Odia, Y. et al. Early imaging marker of progressing glioblastoma: a window of opportunity. J Neurooncol 148, 629–640 (2020). https://doi.org/10.1007/s11060-020-03565-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-020-03565-x