Abstract
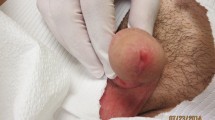
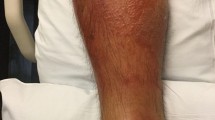
We present a case of cutaneous protothecosis caused by Prototheca wickerhamii infection. The patient was a 72-year-old man with hypoalbuminemia. He responded well to fluconazole treatment. We reviewed this case along with 17 other cases of cutaneous protothecosis reported from mainland China, Hong Kong, and Taiwan. Of the 18 cases, 7 each occurred in mainland China and Taiwan, and 4 occurred in Hong Kong. Thirteen cases were caused by P. wickerhamii (72.2%), and three were caused by P. zopfii (16.7%); in two cases, the species was not identified (11.1%). In all, 9 (50%) patients were immunocompromised, and 10 (55.5%) patients denied having a history of trauma. All patients presented with polymorphic skin lesions, and erythematous papules, plaques, or nodules was the most common presentation (15/18, 83.3%). Genotyping was performed in five cases, mostly by means of small subunit ribosomal DNA amplification (four cases). Susceptibility tests (6 patients) showed that P. wickerhamii was sensitive to amphotericin B and voriconazole but resistant to fluconazole or itraconazole. Treatment succeeded in 15 (83.3%) patients and failed in 3 (16.7%). Our data indicate that the number of cutaneous protothecosis cases is underestimated in China, and the skin lesions have some diagnostic value.


Similar content being viewed by others
References
Pore RS, Barnett EA, Barnes WC Jr, Walker JD. Prototheca ecology. Mycopathologia. 1983;81:49–62.
Roesler U, Möller A, Hensel A, Baumann D, Truyen U. Diversity within the current algal species Prototheca zopfii: a proposal for two Prototheca zopfii genotypes and description of a novel species, Prototheca blaschkeae sp. nov. Int J Syst Evol Microbiol. 2006;56:1419–25.
Satoh K, Ooe K, Nagayama H. MakimuraK. Prototheca cutis sp. nov., a newly discovered pathogen of protothecosis isolated from inflamed human skin. Int J Syst Evol Microbiol. 2010;60:1236–40.
Hirose N, Nishimura K, Inoue-Sakamoto M, Masuda M. Ribosomal internal transcribed spacer of Prototheca wickerhamii has characteristic structure useful for identification and genotyping. PLoS ONE. 2013;8:e81223.
Masuda M, Hirose N, Ishikawa T, Ikawa Y, Nishimura K. Prototheca miyajii sp. nov., isolated from a patient with systemic protothecosis. Int J Syst Evol Microbiol. 2016;66(3):1510–20.
Nagatsuka Y, Kiyuna T, Kigawa R, Sano C, Sugiyama J. Prototheca tumulicola sp. nov., a novel achlorophyllous, yeast-like microalga isolated from the stone chamber interior of the Takamatsuzuka Tumulus. Mycoscience. 2017;58(1):53–9.
Satoh K, Ooe K, Nagayama H, Makimura K. Prototheca cutis sp. nov., a newly discovered pathogen of protothecosis isolated from inflamed human skin. Int J Syst Evol Microbiol. 2010;60(Pt 5):1236–40.
Murugaiyan J, Ahrholdt J, Kowbel V, Roesler U. Establishment of a matrix-assisted laser desorption ionization time-of-flight mass spectrometry database for rapid identification of infectious achlorophyllous green micro-algae of the genus Prototheca. Clin Microbiol Infect. 2012;18(5):461–7.
Zaitz C, Godoy AM, Colucci FM, et al. Cutaneous protothecosis: report of a third Brazilian case. Int J Dermatol. 2006;45:124–6.
Mayorga J, Barba-Gómez JF, Verduzco-Martínez AP, Muñoz-Estrada VF, Welsh O. Protothecosis. Clin Dermatol. 2012;30:432–6.
Todd JR, King JW, Oberle A, et al. Protothecosis: report of a case with 20-year follow-up, and review of previously published cases. Med Mycol. 2012;50:673–89.
Inoue M, Miyashita A, Noguchi H, et al. Case report of cutaneous protothecosis caused by Prototheca wickerhamii designated as genotype 2 and current status of human protothecosis in Japan. J Dermatol. 2018;45:67–71.
Yip SY, Huang CT, Clark WH. Protothecosis, an infection by algae: report of a case from Hong Kong. J Dermatol. 1976;3:309–15.
Kuo TT, Hseuh S, Wu JL, Wang AM. Cutaneous protothecosis. A clinicopathologic study. Arch Pathol Lab Med. 1987;111:737–40.
Kuan YZ, Lee YC. Cutaneous protothecosis: first case in Taiwan. Taiwan Yi Xue Hui Za Zhi. 1989;88:747–51 (Article in Chinese).
Tang WY, Lo KK, Lam WY, Fung KS, Koehler A, Cheng AF. Cutaneous protothecosis: report of a case in Hong Kong. Br J Dermatol. 1995;133:479–82.
Chow KY. Cutaneous protothecosis. Hong Kong Dermatol Venereol Bull. 1999;7:184–6.
Ip FC, Tang WYM, Yau KC, Lo KK. Cutaneous protothecosis in Hong Kong. Hong Kong J Dermatol Venereol. 2007;15:170–7.
Shaoxi W, Guixia L, Yongnian S, Ningru G. The first case of Protothecosis zopfii in China. Chin Med Sci J. 2000;15:121–3.
Chao SC, Hsu MM, Lee JY. Cutaneous protothecosis: report of five cases. Br J Dermatol. 2002;146:688–93.
Zhao J, Liu W, Lv G, Shen Y, Wu S. Protothecosis successfully treated with amikacin combined with tetracyclines. Mycoses. 2004;47:156–8.
Lu S, Xi L, Qin W, Luo Y, Lu C, Li X. Cutaneous protothecosis: two new cases in China and literature review. Int J Dermatol. 2012;51:328–31.
Zhang QQ, Li L, Zhu LP, et al. Cutaneous protothecosis in patient with diabetes mellitus and review of published case reports. Mycopathologia. 2012;173:163–71.
Chou DW, Chung KM, Lee CT. Prototheca wickerhamii cutaneous and systemic infections. Am J Trop Med Hyg. 2014;91:664–5.
Zhang Q, Li L, Yuli K, Zhao Y, Zhu J, Zhu M. A case of cutaneous protothecosis mimics eczema. Mycopathologia. 2015;179:163–6.
Wang X, Fu YF, Wang RY, et al. Identification of clinically relevant fungi and prototheca species by rRNA gene sequencing and multilocus PCR coupled with electrospray ionization mass spectrometry. PLoS ONE. 2014;9:e98110.
Onozaki M, Makimura K, Satoh K, Hasegawa A. Detection and identification of genotypes of Prototheca zopfii in clinical samples by quantitative PCR analysis. Jpn J Infect Dis. 2013;66:383–90.
Dalmau J, Pimentel CL, Alegre M, et al. Treatment of protothecosis with voriconazole. J Am Acad Dermatol. 2006;55:S122–3.
Yun CH, Jeong JH, Ryu HR, et al. Cutaneous protothecosis responds rapidly to voriconazole. Int J Dermatol. 2016;55:1373–7.
Rex JH, Pfaller MA. Has antifungal susceptibility testing come of age? Clin Infect Dis. 2002;35:982–9.
Acknowledgements
We thank Meirong Li from the dermatology department of the Third Affiliated Hospital, Sun Yat-sen University, for the participation in the mycological tests for the presented patient. We also thank Wanzhen Yu from Taiwan Eden Social Welfare Foundation for her help in the literature search.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflicts of interest pertaining to this work.
Ethical Approval
The study was approved by the ethics committee of the First Affiliated Hospital of Sun Yat-sen University.
Informed Consent
Informed consent was obtained from the patient reported in the study.
Additional information
Handling editor: Patrick CY Woo.
Rights and permissions
About this article
Cite this article
Wang, F., Feng, P., Lin, Y. et al. Human Cutaneous Protothecosis: A Case Report and Review of Cases from Mainland China, Hong Kong, and Taiwan. Mycopathologia 183, 821–828 (2018). https://doi.org/10.1007/s11046-018-0292-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11046-018-0292-3