Abstract
Background
The Postpartum-Specific Anxiety Scale (PSAS) is an international measure designed to evaluate anxiety experienced by mothers in the postpartum period from one day to six months; the scale was translated into Arabic and validated within Palestinian context to test postpartum anxiety among Palestinian women.
Aims
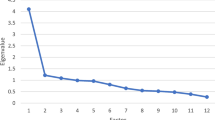
The current study aimed to test the psychometric properties and the factorial structure within the Arabic language in a Palestinian context using confirmatory factor analysis (CFA). The sample of this study consisted of 475 Palestinian women recruited from health centers in the West Banks of Palestine using a convenience sample. 61% were of ages 20–30 years and 39% percent ages 31–40 years.
Findings
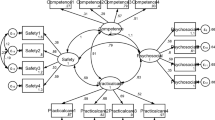
The PSAS showed good validity and reliability indicators in assessing postpartum anxiety within Palestinian context. Results of CFA showed a stable construct of a four-factor structure in assessing postpartum anxiety among Palestinian mothers: (1) competence and attachment anxieties, (2) infant safety and welfare anxieties, (3) practical baby care anxieties and (4) psychosocial adjustment to motherhood, which is consisting with the original four-factor structure of the scale.
Conclusions
The PSAS showed good validity indicators within Palestinian context. Therefore, it is recommended to conduct similar studies with clinical and non-clinical groups in the Palestinian society. The PSAS can be a useful measure to assess anxiety levels among women during the postpartum months; which will enable mental health providers to provide psychological interventions for mothers whose anxiety levels are high.
Significance
During the postpartum period, mothers are particularly vulnerable to a number of distinct changes that are generally perceived as distressing and stressful. Although such stressors are common, some mothers may experience significant anxiety as a result of these stressors. Validating international tools to evaluate postpartum anxiety among Palestinian women is crucial, as women living in this context experience several stressors and life challenges due to the political conflict. The PSAS can be a useful measure to assess anxiety level among mothers during the postpartum months; which enable mental health providers to provide psychological interventions for mothers whose anxiety levels are high.

Similar content being viewed by others
Data Availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- PSAS:
-
Postpartum-Specific Anxiety Scale
- EFA:
-
Exploratory factor analysis
- CFA:
-
Confirmatory factor analysis
- STAI:
-
State Trait Anxiety Inventory
- GAD:
-
Generalized Anxiety Disorder
- EPDS:
-
The Edinburgh Postnatal Depression Scale
- BDI-II:
-
The Beck Depression Inventory-II
- IRB:
-
Institutional Review Board
References
Al-Mandhari, A., Samhouri, D., Abubakar, A., & Brennan, R. (2020). Coronavirus Disease 2019 outbreak: Preparedness and readiness of countries in the Eastern Mediterranean Region. Eastern Mediterranean Health Journal, 26(2), 136–137. https://doi.org/10.26719/2020.26.2.136.
Ali, E. (2018). Women’s experiences with postpartum anxiety disorders: A narrative literature review. International journal of women’s health, 10, 237–249. https://doi.org/10.2147/IJWH.S158621.
Barnett, B., Schaafsma, M., Gusman, A., & Parker, G. Maternal anxiety: A 5-year intervention study. (1991). J Child Psychol 32(3),423–438.
Bayri Bingol, F., Bal, M. D., Aydin Ozkan, S., & Zengin, O. (2021). The adaptation of the postpartum-specific anxiety scale into the Turkish language. Journal of Reproductive and Infant Psychology, 39(1), 86–99. https://doi.org/10.1080/02646838.2019.1705265.
Beck, A. T., Steer, R. A., & Garbin, M. G. (1988). Psychometric properties of the Beck depression inventory: Twenty-five years of evaluation. Clinical Psychology Review, 8, 77–100. https://doi.org/10.1016/0272-7358(88)90050-5.
Brockington, I., Macdonald, E., & Wainscott, G. (2006). Anxiety, obsessions and morbid preoccupations in pregnancy and the puerperium. Arch Womens Ment Health, 9(5), 253–263. https://doi.org/10.1007/s00737-006-0134-z.
Brummelte, S., & Galea, L. A. (2016). Postpartum depression: Etiology, treatment and consequences for maternal care. Hormones and behavior, 77, 153–166. https://doi.org/10.1016/j.yhbeh.2015.08.008.
Bydlowski, S. (2015). Les troubles psychiques du post-partum: dépistage et prévention après la naissance : Recommandations. Journal de Gynécologie Obstétrique. Biologie de La Reproduction, 44(10), 1152–1156. https://doi.org/10.1016/j.jgyn.2015.09.016.
Byrnes, L. (2019). Perinatal mood and anxiety disorders: Findings from focus groups of at risk women. Archives Of Psychiatric Nursing, 33(6), 149–153. https://doi.org/10.1016/j.apnu.2019.08.014.
Cohen, R. J., & Swerdlik, M. E. (2005). Psychological Testing and Assessment: An Introduction to Tests and Measurement (6th ed.). New York: McGraw-Hill.
Cox, J. L., Holden, J. M., & Sagovsky, R. (1987). Detection of postnatal depression: Development of the 10-item Edinburgh Postnatal Depression Scale. The British Journal of Psychiatry, 150(6), 782–786. https://doi.org/10.1192/bjp.150.6.782.
Davies, S. M., Christiansen, P., Harrold, J. A., et al. (2021). Creation and validation of the Postpartum specific anxiety Scale Research Short-Form (PSAS-RSF). Arch Womens Ment Health, 24, 957–969. https://doi.org/10.1007/s00737-021-01114-7.
Dennis, C. (2006). Identifying predictors of breastfeeding self-efficacy in the immediate postpartum period. Research In Nursing & Health, 29(4),256–268.
Dennis, C. L., Coghlan, M., & Vigod, S. (2013). Can we identify mothers at-risk for postpartum anxiety in the immediate postpartum period using the state-trait anxiety inventory? Journal of Affective Disorders, 150(3), 1217–1220. https://doi.org/10.1016/j.jad.2013.05.049.
Dipietro, J. A., Costigan, K. A., & Sipsma, H. L. (2008). Continuity in self-report measures of maternal anxiety, stress, and depressive symptoms from pregnancy through two years postpartum. Journal of Psychosomatic Obstetrics & Gynecology, 29(2), 115–124. https://doi.org/10.1080/01674820701701546.
Duran, S. (2020). Postpartum specific anxiety scale (PSAS): Reliability and validity of the turkish version. Perspectives in Psychiatric Care, 56(1), 95–101. https://doi.org/10.1111/ppc.12385.
Fairbrother, N., Young, A. H., Janssen, P., Antony, M. M., & Tucker, E. (2015). Depression and anxiety during the perinatal period. BMC psychiatry, 15, 206. https://doi.org/10.1186/s12888-015-0526-6.
Fallon, V., Halford, J. C. G., Bennett, K. M., & Harrold, J. A. (2016). The Postpartum specific anxiety scale: Development and preliminary validation. Archives of Women’s Mental Health, 19(6), 1079–1090. https://doi.org/10.1007/s00737-016-0658-9.
Farr, S. L., Dietz, P. M., O’Hara, M. W., Burley, K., & Ko, J. Y. (2014). Postpartum anxiety and comorbid depression in a population-based sample of women. Journal of Women’s Health, 23(2), 120–128. https://doi.org/10.1089/jwh.2013.4438.
Figueiredo, B., & Conde, A. (2011). Anxiety and depression symptoms in women and men from early pregnancy to 3-months postpartum: Parity differences and effects. Journal of Affective Disorders, 132(1–2), 146–157. https://doi.org/10.1016/j.jad.2011.02.007.
Galland, B. C., Taylor, B. J., Elder, D. E., & Herbison, P. (2012). Normal sleep patterns in infants and children: A systematic review of observational studies. Sleep Medicine Reviews, 16(3), 213–222. https://doi.org/10.1016/j.smrv.2011.06.001.
Grekin, R., & O’Hara, M. W. (2014). Prevalence and risk factors of postpartum posttraumatic stress disorder: A meta-analysis. Clinical Psychology Review, 34(5), 389–401. https://doi.org/10.1016/j.cpr.2014.05.003.
Hasanzadeh, R., Jafarabadi, M. A., & Hasanpour, S. (2021). Psychometric evaluation of the postpartum specific anxiety scale in an Iranian population (PSAS-IR). BMC Pregnancy Childbirth 21, 597 (2021). https://doi.org/10.1186/s12884-021-04085-w.
Hung, C. H. (2005). Women’s postpartum stress, social support, and health status. Western Journal of Nursing Research, 27(2), 148–159. https://doi.org/10.1177/0193945904270913.
Kingston, D., Tough, S., & Whitfield, H. (2012). Prenatal and postpartum psychological distress and infant development: A systematic review. Child Psychiatry And Human Development, 43(5), 683–714.
Mahamid, F. A. (2020). Collective trauma, quality of life and resilience in narratives of third generation Palestinian refugee children. Child Indicators Research, 13, 2181–2204. https://doi.org/10.1007/s12187-020-09739-3.
Mahamid, F. A., Bdier, D. (2021). The association between positive religious coping, perceived stress, and depressive symptoms during the spread of coronavirus (COVID-19) among a sample of adults in Palestine: Across sectional study. Journal of Religion and Health, 60, 34–49. https://doi.org/10.1007/s10943-020-01121-5.
Milgrom, J., Martin, P. D., & Negri, L. M. (2000). Treating postnatal depression. A Psychological Approach for Health Care Practitioners.
Murtaja, E. F., & Thabet, A. A. (2017). Anxiety and depression among pregnant women in the Gaza Strip. Psychology and Cognitive Sceinces, 3(4), 137–144. https://doi.org/10.17140/PCSOJ-3-136.
National Collaborating Centre for Mental Health. (2014). Antenatal and postnatal mental health: Clinical management and service guidance (updated ed). National Institute for Health and Care Excellence (commissioners), National Clinical Guideline Number 192. London: The British Psychological Society and The Royal College of Psychiatrists.
Nayak, M. B., & Milner, J. S. (1998). Neuropsychological functioning: Comparison of mothers at high- and low-risk for child physical abuse. Child Abuse & Neglect, 22(7), 687–703. https://doi.org/10.1016/s0145-2134(98)00052-0.
Oyetunji, A., & Chandra, P. (2020). Postpartum stress and infant outcome: A review of current literature. Psychiatry research, 284, 112769. https://doi.org/10.1016/j.psychres.2020.112769.
Petersen, I., Peltola, T., Kaski, S., Walters, K. R., & Hardoon, S. (2018). Depression, depressive symptoms and treatments in women who have recently given birth: UK cohort study. British Medical Journal Open, 8(10), e022152. https://doi.org/10.1136/bmjopen-2018-022152.
Phillips, J., Sharpe, L., Matthey, S., & Charles, M. (2009). Maternally focused worry. Archives of Women’s Mental Health, 12(6), 409–418. https://doi.org/10.1007/s00737-009-0091-4.
Polachek, I. S., Harari, L. H., Baum, M., & Strous, R. D. (2014). Postpartum anxiety in a cohort of women from the general population: Risk factors and association with depression during last week of pregnancy, postpartum depression and postpartum PTSD. Israel Journal of Psychiatry, 51(2), 128–134.
Qandil, S., Jabr, S., Wagler, S., & Collin, S. M. (2016). Postpartum depression in the occupied palestinian territory: A longitudinal study in Bethlehem. BMC pregnancy and childbirth, 16(1), 375. https://doi.org/10.1186/s12884-016-1155-x.
Remes, O., Brayne, C., van der Linde, R., & Lafortune, L. (2016). A systematic review of reviews on the prevalence of anxiety disorders in adult populations. Brain and behavior, 6(7), e00497. https://doi.org/10.1002/brb3.497.
Salah, M., Breaka, R., & Alkasseh, A. (2018). Prevalence of anxiety and depression among mothers of newborns admitted to neonatal intensive care units in Gaza Strip. Edelweiss: Psychiatry Open Access, 2, 2–1. https://doi.org/10.33805/2638-8073.109.
Salari, P., Nazari, S., Mazlom, S., Ghanbari, R., & Abadi, H. B, A (2014). Comparing Postpartum Stressors and Social Support Level in Primiparous and Multiparous Women. Journal of Midwifery and Reproductive Health, 2(1), 71–76.
Shaheen, M. A., & Iemayah, J. I. (2015). Postpartum Depression among palestinian women in the directorate of Bethlehem. Journal of Al-Quds Open University for Educational & Psychological Research & Studies, 3(10), 13–45. https://digitalcommons.aaru.edu.jo/jaqou_edpsych/vol3/iss10/1.
Spitzer, R. L., Kroenke, K., Williams, J. B. W., & Löwe, B. (2006). A brief measure for assessing generalized anxiety disorder. Archives of Internal Medicine, 166(10), 1092. https://doi.org/10.1001/archinte.166.10.1092.
Stewart, D. E., & Vigod, S. (2016). Postpartum depression. New England Journal of Medicine, 375(22), 2177–2186. https://doi.org/10.1056/NEJMcp011542.
Teissedre, F., & Chabol, H. (2003). Postnatal depression: A study of the predictive effects of postnatal anxiety. Irish Journal of Psychological Medicine, 20(4), 111–114. https://doi.org/10.1017/S0790966700007898.
Turk, D. C., Dworkin, R. H., Burke, L. B., Gershon, R., Rothman, M., Scott, J., & Wyrwich, K. W. (2006). Developing patient-reported outcome measures for pain clinical trials: IMMPACT recommendations. Pain, 125(3), 208–215. https://doi.org/10.1016/j.pain.2006.09.028.
Wenzel, A., Stuart, S., & Collaborator. (2011). Anxiety in childbearing women: Diagnosis and treatment. American Psychological Association. https://doi.org/10.1037/12302-000.
Zappas, P. M., Becker, K., & Walton-Moss, B. (2021). Postpartum anxiety. Journal for Nurse Practitioners, 17(1), 60–64. https://doi.org/10.1016/j.nurpra.2020.08.017.
Acknowledgements
Not applicable.
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Contributions
All authors contributed equally to this work. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical Approval
All procedures performed in this study involving human participants were in accordance with the ethical standards of An- Najah University’s Research Ethics Board, the American Psychological Association (APA, 2010) and with the 2013 Helsinki Declaration.
Conflict of interest
The authors declare that they have no conflict of interest. All authors agreeing for submitting the manuscript to the Infant Mental Health Journal.
Informed Consent
Informed consent was obtained from all participants.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mahamid, F., Chou, P., Sarhan, A. et al. Psychometric Properties and Factorial Structure of Postpartum-Specific Anxiety Scale (PSAS) Within Arabic Language in a Palestinian Context. Matern Child Health J 27, 1589–1598 (2023). https://doi.org/10.1007/s10995-023-03747-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-023-03747-9