Abstract
Sexual minorities and immigrants face unique challenges to accessing health care in the United States. This study used data on nonelderly adults (n = 100,667) from the 2013–2016 National Health Interview Survey. Unadjusted prevalence estimates and multivariable logistic regression models (with and without interactions between immigration and sexual minority status) were used to compare health insurance coverage and access to care by immigration and sexual minority status. We did not find any differences in uninsurance, having a usual source of care, and a recent office visit by sexual orientation for US-born and foreign-born adults. However, compared to their heterosexual counterparts, US-born and foreign-born sexual minorities were more likely to have an emergency room visit in the prior year and report financial-related barriers to medical care, dental care, prescription medications, and mental health care. Foreign-born sexual minorities were more likely to have an emergency room visit and unmet mental health care needs due to cost compared to other subpopulations after controlling for sociodemographic characteristics. Broadening the knowledge and scope of research on sexual minority immigrants can inform targeted health policy approaches with the goal of achieving health equity for sexual minority immigrants.

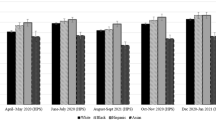
Source 2013–2016 National Health Interview Survey (NHIS), adults aged 18–64 years. All estimates used survey weights to adjust for the complex survey design of the NHIS and to generate nationally representative estimates
Similar content being viewed by others
References
Institute of Medicine. The health of lesbian, gay, bisexual, and transgender people: building a foundation for better understanding. Washington, DC: The National Academies Press; 2011.
Hatzenbuehler ML. How does sexual minority stigma “get under the skin”? A psychological mediation framework. Psychol Bull. 2009;135(5):707–30.
Hatzenbuehler ML, McLaughlin KA, Keyes KM, Hasin DS. The impact of institutional discrimination on psychiatric disorders in lesbian, gay, and bisexual populations: a prospective study. Am J Public Health. 2010;100(3):452–9.
Meyer IH. Prejudice, social stress, and mental health in lesbian, gay, and bisexual populations: conceptual issues and research evidence. Psychol Bull. 2003;129(5):674–97.
Gonzales G, Przedworski J, Henning-Smith C. Comparison of health and health risk factors between lesbian, gay, and bisexual adults and heterosexual adults in the United States. JAMA Intern Med. 2016;176(9):1344–51.
Fredriksen-Goldsen KI, Simoni JM, Kim H-J, et al. The health equity promotion model: reconceptualization of lesbian, gay, bisexual, and transgender (LGBT) health disparities. Am J Orthopsychiatry. 2014;84(6):653–63.
Almeida J, Biello KB, Pedraza F, Wintner S, Viruell-Fuentes E. The association between anti-immigrant policies and perceived discrimination among Latinos in the US: a multilevel analysis. SSM Popul Health. 2016;2(January):897–903.
Toomey RB, Umaña-Taylor AJ, Williams DR, Harvey-Mendoza E, Jahromi LB, Updegraff KA. Impact of Arizona’s SB 1070 immigration law on utilization of health care and public assistance among mexican-origin adolescent mothers and their mother figures. Am J Public Health. 2014;104(Supplement 1):28–34.
Rhodes SD, Mann L, Simán FM, et al. The impact of local immigration enforcement policies on the health of immigrant Hispanics/Latinos in the United States. Am J Public Health. 2015;105(2):329–37.
Hatzenbuehler ML, Prins SJ, Flake M, et al. Immigration policies and mental health morbidity among Latinos: a state-level analysis. Soc Sci Med. 2017;174:169–78.
Martinez O, Wu E, Sandfort T, et al. Evaluating the impact of immigration policies on health status among undocumented immigrants: a systematic review. J Immigr Minor Health. 2015;17(3):947–70.
Bowden WP, Rhodes SD, Wilkin AM, Carolina N. Sociocultural determinants of HIV/AIDS risk and service use among immigrant Latinos in North Carolina. Hisp J Behav Sci. 2006;28(4):546–62.
De Santis J. How do the sexual behaviors of foreign-born Hispanic men who have sex with men differ by relationship status? Am J Mens Health. 2012;6(1):6–17.
Gilbert P, Rhodes SD. HIV testing among immigrant sexual and gender minority Latinos in a US region with little historical Latino presence. AIDS Patient Care STDS. 2013;27(11):628–36.
Gilbert PA, Rhodes SD. Immigrant sexual minority Latino men in rural North Carolina: an exploration of social context, social behaviors, and sexual outcomes. J Homosex. 2014;61(8):1131–51.
Yoshikawa H, Wilson PA, Chae DH, Cheng J. Do family and friendship networks protect against the influence of discrimination on mental health and HIV risk among Asian and Pacific Islander gay men? AIDS Educ Prev. 2004;16(1):84–100.
Lewis NM. Urban encounters and sexual health among gay and bisexual immigrant men: perspectives from the settlement and AIDS service sectors. Geogr Rev. 2016;106(2):235–56.
Rhodes SD, Mccoy TP, Hergenrather KC, et al. Prevalence estimates of health risk behaviors of immigrant latino men who have sex with men. J Rural Health. 2012;28(1):73–83.
Rhodes SD, McCoy TP. Condom use among immigrant Latino sexual minorities: multilevel analysis after respondent-driven samples. AIDS Educ Prev. 2015;27(1):27–43.
Lewis NM, Wilson K. HIV risk behaviours among immigrant and ethnic minority gay and bisexual men in North America and Europe: a systematic review. Soc Sci Med. 2017;179:115–28.
Mizuno Y, Borkowf CB, Ayala G, Carballo-Diéguez A, Millett GA. Correlates of sexual risk for HIV among US-born and foreign-born Latino men who have sex with men (MSM): an analysis from the Brothers y Hermanos Study. J Immigr Minor Health. 2015;17(1):47–55.
Lessard D, Lebouché B, Engler K, Thomas R. An analysis of socio-demographic and behavioural factors among immigrant MSM in Montreal from an HIV-testing site sample. Can J Hum Sex. 2016;25(1):53–60.
Strömdahl S, Liljeros F, Thorson AE, Persson KI, Forsberg BC. HIV testing and prevention among foreign-born men who have sex with men: an online survey from Sweden. BMC Public Health. 2017;17(139):1–9.
Navaza B, Abarca B, Bisoffi F, Pool R, Roura M. Provider-initiated HIV testing for migrants in Spain: a qualitative study with health care workers and foreign-born sexual minorities. PLoS ONE. 2016;11(2):1–18.
Beymer MR, Weiss RE, Halkitis PN, et al. Disparities within the disparity-determining HIV risk factors among Latino gay and bisexual men attending a community-based clinic in Los Angeles, CA. J Acquir Immune Defic Syndr. 2016;73(2):237–44.
Gilbert PA, Perreira K, Eng E, Rhodes SD. Social stressors and alcohol use among immigrant sexual and gender minority Latinos in a non-traditional settlement state. Subst Use Misuse. 2014;49(11):1365–75.
Gray NN, Mendelsohn DM, Omoto AM. Community connectedness, challenges, and resilience among gay Latino immigrants. Am J Community Psychol. 2015;55:202–14.
Rhodes SD, Martinez O, Song E-Y, et al. Depressive symptoms among immigrant Latino sexual minorities. Am J Health Behav. 2014;6(244):1–16.
Tanner A, Reboussin B, Mann L, Song E, Alonzo J, Rhodes S. Factors influencing health care access perceptions and care-seeking behaviors of immigrant Latino sexual minority men and transgender individuals: baseline findings from the HOLA intervention study. J Health Care Poor Underserved. 2014;25(4):1679–97.
Gonzales G, Blewett LA. National and state-specific health insurance disparities for adults in same-sex relationships. Am J Public Health. 2014;104(2):e95–104.
Gonzales G, Moltz R, King M. Health insurance coverage for same-sex couples: disparities and trends under DOMA. In: Harvey VL, Housel TH, editors. Health care disparities and the LGBT population. Lanham: Lexington Books; 2014. pp. 87–106.
Heck JE, Sell RL, Gorin SS. Health care access among individuals involved in same-sex relationships. Am J Public Health. 2006;96(6):1111–8.
Buchmueller T, Carpenter CS. Disparities in health insurance coverage, access, and outcomes for individuals in same-sex versus different-sex relationships, 2000–2007. Am J Public Health. 2010;100(3):489–95.
Ash MA, Badgett MVL. Separate and unequal: the effect of unequal access to employment-based health insurance on same-sex and unmarried different-sex couples. Contemp Econ Policy. 2006;24(4):582–99.
Dahlhamer JM, Galinsky AM, Joestl SS, Ward BW. Barriers to health care among adults identifying as sexual minorities: A US national study. Am J Public Health. 2016;106(6):1116–22.
Clift JB, Kirby J. Health care access and perceptions of provider care among individuals in same-sex couples: findings from the Medical Expenditure Panel Survey (MEPS). J Homosex. 2012;59(6):839–50.
Karpman M, Skopec L, Long SK. QuickTake. Uninsurance Rate Nearly Halved for Lesbian, Gay, and Bisexual Adults since Mid-2013. Urban Institute Health Policy Center. http://hrms.urban.org/quicktakes/Uninsurance-Rate-Nearly-Halved-for-Lesbian-Gay-and-Bisexual-Adults-since-Mid-2013.html. Published 2015. Accessed 3 Mar 2016.
Skopec L, Long SK. Lesbian, gay, and bisexual adults making gains in health insurance and access to care. Health Aff. 2015;34(10):1769–73.
Tran LD. Moderate effects of same-sex legislation on dependent employer-based insurance coverage among sexual minorities. Med Care Res Rev. 2016;73(6):752–68.
Dawson L, Kates J, Damico A. The affordable care act and insurance coverage changes by sexual orientation. Menlo Park, CA; 2018.
Sabin JA, Riskind RG, Nosek BA. Health care providers’ implicit and explicit attitudes toward lesbian women and gay men. Am J Public Health. 2015;105(9):1831–41.
Mattocks KM, Sullivan JC, Bertrand C, Kinney RL, Sherman MD, Gustason C. Perceived stigma, discrimination, and disclosure of sexual orientation among a sample of lesbian veterans receiving care in the Department of Veterans Affairs. LGBT Health. 2015;2(2):147–53.
Kullgren JT. Restrictions on undocumented immigrants’ access to health services: the public health implications of welfare reform. Am J Public Health. 2003;93(10):1630–3.
Agrawal P, Venkatesh AK. Refugee resettlement patterns and state-level health care insurance access in the United States. Am J Public Health. 2016;106(4):662–3.
Timmins CL. The impact of language barriers on the health care of Latinos in the United States: a review of the literature and guidelines for practice. J Midwifery Womens Health. 2002;47(2):80–96.
Clough J, Lee S, Chae DH. Barriers to health care among Asian immigrants in the United States: a traditional review. J Health Care Poor Underserved. 2013;24(1):384–403.
National Center for Health Statistics. Health, United States, 2016: with chartbook on long-term trends in health. Hyattsville, MD; 2017.
Blewett LA, Drew JAR, Griffin R, King ML, Williams KCW. IPUMS Health Surveys: National Health Interview Survey, Version 6.2. Minneapolis; 2016.
Dey AN, Lucas JW. Physical and mental health characteristics of U.S.—and foreign-born adults: United States, 1998–2003. Adv Data. 2006;369:1–19.
Mehta NK, Elo IT, Ford ND, Siegel KR. Obesity among U.S.- and foreign-born Blacks by region of birth. Am J Prev Med. 2015;49(2):269–73.
Ward BW, Dahlhamer JM, Galinsky AM, Joestl SS. Sexual orientation and health among U.S. adults: National Health Interview Survey, 2013. Natl Health Stat Rep. 2014;July 15(77):1–12. 2(.
National Center for Health Statistics. National Health Interview Survey: Survey Description. Hyattsville, MD; 2016. ftp://ftp.cdc.gov/pub/Health_Statistics/NCHS/Dataset_Documentation/NHIS/2015/srvydesc.pdf.
Riosmena F, Kuhn R, Jochem WC. Explaining the immigrant health advantage: self-selection and protection in health-related factors among five major national-origin immigrant groups in the United States. Demography. 2017;54(1):175–200.
Riosmena F, Wong R, Palloni A. Migration selection, protection, and acculturation in health: a binational perspective on older adults. Demography. 2013;50(3):1039–64.
National Center for Health Statistics. A brief quality assessment of the NHIS sexual orientation data. Atlanta, GA; 2014.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gonzales, G., Dedania, R. & Driscoll, R. Health Insurance Coverage and Access to Care Among US-Born and Foreign-Born Sexual Minorities. J Immigrant Minority Health 21, 540–548 (2019). https://doi.org/10.1007/s10903-018-0774-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10903-018-0774-x