Abstract
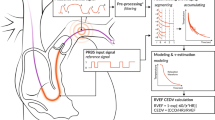
Peroral endoscopic myotomy (POEM) is natural orifice transluminal endoscopic surgery to treat esophageal achalasia. During POEM, cardiovascular dynamics can be impaired by capnoperitoneum, capnomediastinum, and systemic carbon dioxide accumulation. We systematically investigated changes in cardiovascular dynamics during POEM. We included 31 patients having POEM in this single-center prospective observational study. Before and every 5 min during POEM we measured mean arterial pressure (MAP), heart rate (HR), cardiac index (CI), stroke volume index (SVI), and systemic vascular resistance index (SVRI) using non-invasive finger cuff-derived pulse wave analysis. During POEM, the median MAP was higher than the median baseline MAP of 77 (67;86) mmHg. HR (median at baseline: 67 (60;72) bpm), CI (2.8 (2.5;3.2) L/min/m2), SVI (42 (34;51) mL/m2), and SVRI (1994 (1652; 2559) dyn × s × cm−5 × m−2) remained stable during POEM. Mixed model-derived 95% confidence limits of hemodynamic variables during POEM were 72 to 106 mmHg for MAP, 65 to 79 bpm for HR, 2.7 to 3.3 L/min/m2 for CI, 37 and 46 mL/m2 for SVI, and 1856 and 2954 dyn × s × cm−5 × m−2 for SVRI. POEM is a safe procedure with regard to cardiovascular dynamics as it does not markedly impair MAP, HR, CI, SVI, or SVRI.



Similar content being viewed by others
Data availability
Data are available from the authors upon reasonable request.
References
Pandolfino JE, Gawron AJ. Achalasia: a systematic review. JAMA. 2015;313:1841–52. https://doi.org/10.1001/jama.2015.2996.
Inoue H, Minami H, Kobayashi Y, Sato Y, Kaga M, Suzuki M, et al. Peroral endoscopic myotomy (POEM) for esophageal achalasia. Endoscopy. 2010;42:265–71. https://doi.org/10.1055/s-0029-1244080.
Stavropoulos SN, Desilets DJ, Fuchs KH, Gostout CJ, Haber G, Inoue H, et al. Per-oral endoscopic myotomy white paper summary. Gastrointest Endosc. 2014;80:1–15. https://doi.org/10.1016/j.gie.2014.04.014.
Von Renteln D, Fuchs KH, Fockens P, Bauerfeind P, Vassiliou MC, Werner YB, et al. Peroral endoscopic myotomy for the treatment of achalasia: an international prospective multicenter study. Gastroenterology. 2013;145:309–11. https://doi.org/10.1053/j.gastro.2013.04.057.
von Renteln D, Inoue H, Minami H, Werner YB, Pace A, Kersten JF, et al. Peroral endoscopic myotomy for the treatment of achalasia: a prospective single center study. Am J Gastroenterol. 2012;107:411–7. https://doi.org/10.1038/ajg.2011.388.
Ponds FA, Fockens P, Lei A, Neuhaus H, Beyna T, Kandler J, et al. Effect of peroral endoscopic myotomy vs pneumatic dilation on symptom severity and treatment outcomes among treatment-naive patients with achalasia: a randomized clinical trial. JAMA. 2019;322:134–44. https://doi.org/10.1001/jama.2019.8859.
Werner YB, Hakanson B, Martinek J, Repici A, von Rahden BHA, Bredenoord AJ, et al. Endoscopic or surgical myotomy in patients with idiopathic achalasia. N Engl J Med. 2019;381:2219–29. https://doi.org/10.1056/NEJMoa1905380.
Löser B, Werner YB, Löser A, Rösch T, Petzoldt M. Anesthesia in gastrointestinal endoscopy: peroral endoscopic myotomy. Anaesthesist. 2019;68:607–14. https://doi.org/10.1007/s00101-019-00655-y.
Löser B, Recio Ariza O, Saugel B, Reuter DA, Zöllner C, Werner YB, et al. Anesthesia for patients undergoing peroral endoscopic myotomy procedures: a review of the literature. Anesth Analg. 2019. https://doi.org/10.1213/ANE.0000000000004420.
Löser B, Werner YB, Punke MA, Saugel B, Haas S, Reuter DA, et al. Anesthetic considerations for patients with esophageal achalasia undergoing peroral endoscopic myotomy: a retrospective case series review. Can J Anaesth. 2017;64:480–8. https://doi.org/10.1007/s12630-017-0820-5.
Meidert AS, Saugel B. Techniques for non-invasive monitoring of arterial blood pressure. Front Med. 2017;4:231. https://doi.org/10.3389/fmed.2017.00231.
Saugel B, Cecconi M, Hajjar LA. Noninvasive cardiac output monitoring in cardiothoracic surgery patients: available methods and future directions. J Cardiothorac Vasc Anesth. 2019;33:1742–52. https://doi.org/10.1053/j.jvca.2018.06.012.
Saugel B, Vincent J-L. Cardiac output monitoring: how to choose the optimal method for the individual patient. Curr Opin Crit Care. 2018;24:165–72. https://doi.org/10.1097/MCC.0000000000000492.
Teboul J-L, Saugel B, Cecconi M, De Backer D, Hofer CK, Monnet X, et al. Less invasive hemodynamic monitoring in critically ill patients. Intensive Care Med. 2016;42:1350–9. https://doi.org/10.1007/s00134-016-4375-7.
Wagner JY, Saugel B. When should we adopt continuous noninvasive hemodynamic monitoring technologies into clinical routine? J Clin Monit Comput. 2015;29:1–3. https://doi.org/10.1007/s10877-014-9619-x.
Wagner JY, Körner A, Schulte-Uentrop L, Kubik M, Reichenspurner H, Kluge S, et al. A comparison of volume clamp method-based continuous noninvasive cardiac output (CNCO) measurement versus intermittent pulmonary artery thermodilution in postoperative cardiothoracic surgery patients. J Clin Monit Comput. 2018;32:235–44. https://doi.org/10.1007/s10877-017-0027-x.
Wagner JY, Grond J, Fortin J, Negulescu I, Schöfthaler M, Saugel B. Continuous noninvasive cardiac output determination using the CNAP system: evaluation of a cardiac output algorithm for the analysis of volume clamp method-derived pulse contour. J Clin Monit Comput. 2016;30:487–93. https://doi.org/10.1007/s10877-015-9744-1.
Wagner JY, Negulescu I, Schöfthaler M, Hapfelmeier A, Meidert AS, Huber W, et al. Continuous noninvasive arterial pressure measurement using the volume clamp method: an evaluation of the CNAP device in intensive care unit patients. J Clin Monit Comput. 2015;29:807–13. https://doi.org/10.1007/s10877-015-9670-2.
Jeleazcov C, Krajinovic L, Münster T, Birkholz T, Fried R, Schüttler J, et al. Precision and accuracy of a new device (CNAPTM) for continuous non-invasive arterial pressure monitoring: assessment during general anaesthesia. Br J Anaesth. 2010;105:264–72. https://doi.org/10.1093/bja/aeq143.
Smolle K-H, Schmid M, Prettenthaler H, Weger C. The accuracy of the CNAP® device compared with invasive radial artery measurements for providing continuous noninvasive arterial blood pressure readings at a medical intensive care unit: a method-comparison study. Anesth Analg. 2015;121:1508–16. https://doi.org/10.1213/ANE.0000000000000965.
Ho HS, Saunders C, Gunther RA, Wolfe BM. Effector of hemodynamics during laparoscopy: CO2 absorption or intra-abdominal pressure? J Surg Res. 1995;59:497–503. https://doi.org/10.1006/jsre.1995.1198.
Koivusalo AM, Kellokumpu I, Scheinin M, Tikkanen I, Mäkisalo H, Lindgren L. A comparison of gasless mechanical and conventional carbon dioxide pneumoperitoneum methods for laparoscopic cholecystectomy. Anesth Analg. 1998;86:153–8. https://doi.org/10.1097/00000539-199801000-00031.
Hirvonen EA, Poikolainen EO, Pääkkönen ME, Nuutinen LS. The adverse hemodynamic effects of anesthesia, head-up tilt, and carbon dioxide pneumoperitoneum during laparoscopic cholecystectomy. Surg Endosc. 2000;14:272–7. https://doi.org/10.1007/s004640000038.
Walder AD, Aitkenhead AR. Role of vasopressin in the haemodynamic response to laparoscopic cholecystectomy. Br J Anaesth. 1997;78:264–6. https://doi.org/10.1093/bja/78.3.264.
Myre K, Rostrup M, Buanes T, Stokland O. Plasma catecholamines and haemodynamic changes during pneumoperitoneum. Acta Anaesthesiol Scand. 1998;14:343–7. https://doi.org/10.1111/j.1399-6576.1998.tb04927.x.
Atkinson TM, Giraud GD, Togioka BM, Jones DB, Cigarroa JE. Cardiovascular and ventilatory consequences of laparoscopic surgery. Circulation. 2017;135:700–10. https://doi.org/10.1161/CIRCULATIONAHA.116.023262.
Hömme R. Anesthesia for laparoscopic interventions. Anaesthesist. 2011;60:175–87. https://doi.org/10.1007/s00101-011-1856-5.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
BS: This author conceived and designed the study, was responsible for data analysis and interpretation, drafted the manuscript, and supervised the study. CV: This author collected the data, was responsible for data analysis and interpretation, and drafted the manuscript. HOP: This author was responsible for data analysis and interpretation, performed the statistical analyses, and critically revised the manuscript for important intellectual content. TR: This author was responsible for data analysis and interpretation and critically revised the manuscript for important intellectual content. MP: This author was responsible for data analysis and interpretation and critically revised the manuscript for important intellectual content. BL: This author conceived and designed the study, was responsible for data analysis and interpretation, and drafted the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
BS has received institutional restricted research grants, honoraria for giving lectures, and refunds of travel expenses from CNSystems Medizintechnik GmbH (Graz, Austria). For all other authors there is no conflict of interest to disclose.
Ethics approval
Ethical approval for this study (PV5540) was provided by the Ethics Committee of the Medical Board of Hamburg, Germany (Prof M. Carstensen) on 22 August 2017.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Glossary
- POEM
-
Peroral endoscopic myotomy
- ASA
-
American Society of Anesthesiologists
- MAP
-
Mean arterial pressure
- HR
-
Heart rate
- CI
-
Cardiac index
- SVI
-
Stroke volume index
- SVRI
-
Systemic vascular resistance index
- CO2
-
Carbon dioxide
- etCO2
-
End-tidal carbon dioxide
- MV
-
Minute ventilation
- TV
-
Tidal volume
- RR
-
Respiratory rate
- PEAK
-
Peak inspiratory pressure
- PEEP
-
Positive end-expiratory pressure
Rights and permissions
About this article
Cite this article
Saugel, B., Vokuhl, C., Pinnschmidt, H.O. et al. Cardiovascular dynamics during peroral endoscopic myotomy for esophageal achalasia: a prospective observational study using non-invasive finger cuff-derived pulse wave analysis. J Clin Monit Comput 35, 827–834 (2021). https://doi.org/10.1007/s10877-020-00541-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-020-00541-8