Abstract
Kabuki Syndrome (KS) is a multisystemic genetic disorder. A portion of patients has immunological manifestations characterized by increased susceptibility to infections and autoimmunity. Aiming to describe the clinical and laboratory immunological aspects of KS, we conducted a retrospective multicenter observational study on patients with KS treated in centers affiliated to the Italian Primary Immunodeficiency Network.
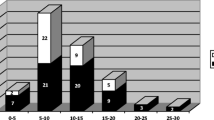
Thirty-nine patients were enrolled, with a median age at evaluation of 10 years (range: 3 m–21y). All individuals had organ malformations of variable severity. Congenital heart defect (CHD) was present in 19/39 patients (49%) and required surgical correction in 9/39 (23%), with associated thymectomy in 7/39 (18%). Autoimmune cytopenia occurred in 6/39 patients (15%) and was significantly correlated with thymectomy (p < 0.002), but not CHD. Individuals with cytopenia treated with mycophenolate as long-term immunomodulatory treatment (n = 4) showed complete response. Increased susceptibility to infections was observed in 22/32 patients (69%). IgG, IgA, and IgM were low in 13/29 (45%), 13/30 (43%) and 4/29 (14%) patients, respectively. Immunoglobulin substitution was required in three patients. Lymphocyte subsets were normal in all patients except for reduced naïve T-cells in 3/15 patients (20%) and reduced memory switched B-cells in 3/17 patients (18%). Elevated CD3 + TCRαβ + CD4-CD8-T-cells were present in 5/17 individuals (23%) and were correlated with hematological and overall autoimmunity (p < 0.05).
In conclusion, immunological manifestations of KS in our cohort include susceptibility to infections, antibody deficiency, and autoimmunity. Autoimmune cytopenia is correlated with thymectomy and elevated CD3 + TCRαβ + CD4-CD8-T-cells, and benefits from treatment with mycophenolate.


Similar content being viewed by others
Data Availability
The datasets generated and analysed during the current study are available from the corresponding author on reasonable request.
References
Margot H, Boursier G, Duflos C, Sanchez E, Amiel J, Andrau J-C et al. Immunopathological manifestations in Kabuki syndrome: a registry study of 177 individuals. Genet Med. 2019;0(0). Available from: http://www.nature.com/articles/s41436-019-0623-x.
Sobreira N, Brucato M, Zhang L, Ladd-Acosta C, Ongaco C, Romm J et al. Patients with a Kabuki syndrome phenotype demonstrate DNA methylation abnormalities. Eur J Hum Genet. 2017;25(12):1335–44. https://doi.org/10.1038/s41431-017-0023-0.
Makrythanasis P, van Bon BW, Steehouwer M, Rodríguez-Santiago B, Simpson M, Dias P, et al. MLL2 mutation detection in 86 patients with Kabuki syndrome: a genotype-phenotype study. Clin Genet. 2013;84(6):539–45.
Ng SB, Bigham AW, Buckingham KJ, Hannibal MC, McMillin MJ, Gildersleeve HI et al. Exome sequencing identifies MLL2 mutations as a cause of Kabuki syndrome. Nat Genet. 2010.
Lederer D, Grisart B, Digilio MC, Benoit V, Crespin M, Ghariani SC et al. Deletion of KDM6A, a histone demethylase interacting with MLL2, in three patients with Kabuki syndrome. Am J Hum Genet. 2012;90(1):119–24. Available from: http://www.ncbi.nlm.nih.gov/pubmed/22197486.
Bögershausen N, Tsai I-C, Pohl E, Kiper PÖS, Beleggia F, Percin EF, et al. RAP1-mediated MEK/ERK pathway defects in Kabuki syndrome. J Clin Invest. 2015;125(9):3585–99.
Niikawa N, Matsuura N, Fukushima Y, Ohsawa T, Kajii T. Kabuki make-up syndrome: a syndrome of mentalretardation, unusual facies, large and protruding ears, and postnatal growth deficiency. J Pediatr. 1981;99(4):565–9.
Kuroki Y, Suzuki Y, Chyo H, Hata A, Matsui I. A new malformation syndrome of long palpebralfissures, large ears, depressed nasal tip, and skeletal anomalies associated with postnatal dwarfism and mental retardation. J Pediatr. 1981;99(4):570–3.
Stagi S, Gulino AV, Lapi E, Rigante D. Epigenetic control of the immune system: a lesson from Kabuki syndrome. Immunol Res. 2016;64(2):345–59. Available from: http://www.ncbi.nlm.nih.gov/pubmed/26411453.
Merdler-Rabinowicz R, Pode-Shakked B, Vivante A, Lahav E, Kagan M, Chorin O et al. Kidney and urinary tract findings among patients with Kabuki (make-up) syndrome. Pediatr Nephrol. 2021;(0123456789):10–3. https://doi.org/10.1007/s00467-021-05216-3.
Picard C, Bobby Gaspar H, Al-Herz W, Bousfiha A, Casanova J-L, Chatila T, et al. International Union of Immunological Societies: 2017 primary immunodeficiency diseases Committee Report on Inborn errors of immunity. J Clin Immunol. 2018;38(1):96–128.
Tangye SG, Al-Herz W, Bousfiha A, Chatila T, Cunningham-Rundles C, Etzioni A et al. Human inborn errors of immunity: 2019 update on the classification from the International Union of Immunological Societies Expert Committee. J Clin Immunol. 2020.
Tangye SG, Al-Herz W, Bousfiha A, Cunningham-Rundles C, Franco JL, Holland SM et al. Human Inborn Errors of Immunity: 2022 Update on the Classification from the International Union of Immunological Societies Expert Committee. J Clin Immunol 2022. 2022 [cited 2022 Oct 4];1:1–35. Available from: https://link.springer.com/article/https://doi.org/10.1007/s10875-022-01289-3.
Bousfiha A, Jeddane L, Picard C, Al-Herz W, Ailal F, Chatila T, et al. Human inborn errors of immunity: 2019 update of the IUIS Phenotypical classification. J Clin Immunol. 2020;40(1):66–81.
Hoffman JD, Ciprero KL, Sullivan KE, Kaplan PB, McDonald-McGinn DM, Zackai EH, et al. Immune abnormalities are a frequent manifestation of Kabuki syndrome. Am J Med Genet. 2005;135 A(3):278–81.
Lin J, Lee W, Huang J, Chen PK, Chan K, Lo L, et al. Immunologic assessment and KMT2D mutation detection in Kabuki syndrome. Clin Genet. 2015;88(3):255–60.
Watanabe T, Miyakawa M, Satoh M, Abe T, Oda Y. Kabuki make-up syndrome associated with chronic idiopathic thrombocytopenic purpura. Acta Paediatr Jpn Overseas Ed. 1994;36(6):727–9. Available from: https://pubmed.ncbi.nlm.nih.gov/7871993/.
Fujishiro M, Ogihara T, Tsukuda K, Shojima N, Fukushima Y, Kimura S et al. A case showing an association between type 1 diabetes mellitus and Kabuki syndrome. Diabetes Res Clin Pract. 2003 ;60(1):25–31. Available from: https://pubmed.ncbi.nlm.nih.gov/12639762/.
Ming JE, Russell KL, McDonald-McGinn DM, Zackai EH. Autoimmune disorders in Kabuki syndrome. In: Am J Med Genet. 2005. p. 260–2.
Giordano P, Lassandro G, Sangerardi M, Faienza MF, Valente F, Martire B. Autoimmune haematological disorders in two Italian children with Kabuki syndrome. Ital J Pediatr. 2014;40(1). Available from: https://pubmed.ncbi.nlm.nih.gov/24460868/.
Cantoni S, Fattizzo B. Clinical course and management of adult-onset immune-mediated cytopenia associated with Kabuki syndrome. Eur J Intern Med. 2019;26(4):e10–1. https://doi.org/10.1016/j.ejim.2014.09.014.
Almécija AC, Pérez V, Baro M, Guerra-García P, Vivanco JL. Atypical Autoimmune Hematologic Disorders in a Patient With Kabuki Syndrome. J Pediatr Hematol Oncol. 2019;41(2):E114–5. Available from: https://pubmed.ncbi.nlm.nih.gov/29683950/.
Leonardi L, Testa A, Feleppa M, Paparella R, Conti F, Marzollo A et al. Immune dysregulation in Kabuki syndrome: a case report of Evans syndrome and hypogammaglobulinemia. Front Pediatr. 2023;11:1087002. Available from: https://www.frontiersin.org/articles/https://doi.org/10.3389/fped.2023.1087002/full.
Oto J, Mano A, Nakataki E, Yamaguchi H, Inui D, Imanaka H et al. An adult patient with Kabuki syndrome presenting with Henoch-Schönlein purpura complicated with pulmonary hemorrhage. J Anesth. 2008;22(4):460–3. Available from: https://pubmed.ncbi.nlm.nih.gov/19011790/.
Ho J, Fox D, Innes AM, McLeod R, Butzner D, Johnson N et al. Kabuki syndrome and Crohn disease in a child with familial hypocalciuric hypercalcemia. J Pediatr Endocrinol Metab. 2010;23(9):975–9. Available from: https://pubmed.ncbi.nlm.nih.gov/21175100/.
Nishizaki N, Fujinaga S, Hirano D, Murakami H, Kamei K, Ohtomo Y et al. Membranoproliferative glomerulonephritis Type 3 associated with Kabuki syndrome. Clin Nephrol. 2014;81(5):369–73. Available from: https://pubmed.ncbi.nlm.nih.gov/23149249/.
Arsov T, Sestan M, Cekada N, Frkovic M, Andrews D, He Y et al. Systemic lupus erythematosus: A new autoimmune disorder in Kabuki syndrome. Eur J Med Genet. 2019;62(6). Available from: https://pubmed.ncbi.nlm.nih.gov/30213761/.
Ferreras C, Aguiar F, Rodrigues M, Brito I. Kabuki syndrome with Sjögren Syndrome: First case reported. Reumatol Clínica (English Ed). 2021 https://doi.org/10.1016/j.reumae.2021.03.004.
Li S, Liu J, Yuan Y, Lu A, Liu F, Sun L et al. Case report: A study on the de novo KMT2D variant of Kabuki syndrome with Goodpasture’s syndrome by whole exome sequencing. Front Pediatr. 2022;10. Available from: https://pubmed.ncbi.nlm.nih.gov/36090579/.
Matsushima S, Kato K, Yoshimi A, Yoshiura K, Tsuchida M. Pernicious anemia associated with Kabuki syndrome. Pediatr Int. 2022;64(1). Available from: https://onlinelibrary.wiley.com/doi/https://doi.org/10.1111/ped.14960.
Tamura S, Kosako H, Furuya Y, Yamashita Y, Mushino T, Mishima H et al. A Patient with Kabuki Syndrome Mutation Presenting with Very Severe Aplastic Anemia. Acta Haematol. 2022;145(1):89–96. Available from: https://pubmed.ncbi.nlm.nih.gov/34515044/.
Marzollo A, Colavito D, Sartori S, Fanelli GN, Putti MC. Cerebral lymphoproliferation in a patient with Kabuki Syndrome. J Clin Immunol. 2018;38(4):475–7.
Deyà-Martínez A, Esteve-Solé A, Vélez-Tirado N, Celis V, Costa J, Cols M, et al. Sirolimus as an alternative treatment in patients with granulomatous-lymphocytic lung disease and humoral immunodeficiency with impaired regulatory T cells. Pediatr Allergy Immunol. 2018;29(4):425–32.
Mock JR, Kolb TM, Illei PB, Yang SC, Lederman HM, Merlo CA. Bronchus-associated lymphoid tissue in kabuki syndrome with associated hyper-IgM syndrome/common variable immunodeficiency. Am J Respir Crit Care Med [Internet]. 2016;194(4):514–5. Available from: https://doi.org/10.1164/rccm.201511-2305IM.
Chan AY, Torgerson TR. Primary immune regulatory disorders: a growing universe of immune dysregulation. Curr Opin Allergy Clin Immunol. 2020;20(6):582–90. Available from: https://pubmed.ncbi.nlm.nih.gov/32941318/.
Lindsley AW, Saal HM, Burrow TA, Hopkin RJ, Shchelochkov O, Khandelwal P, et al. Defects of B-cell terminal differentiation in patients with type-1 Kabuki syndrome. J Allergy Clin Immunol. 2016;137(1):179–187e10.
Gidwani P, Segal E, Shanske A, Driscoll C. Chorea associated with antiphospholipid antibodies in a patient with Kabuki syndrome. Am J Med Genet Part A. 2007;143A(12):1338–41.
Pilarowski GO, Cazares T, Zhang L, Benjamin JS, Ke Liu À, Jagannathan S, et al. Abnormal Peyer patch development and B-cell gut homing drive IgA deficiency in Kabuki syndrome. J Allergy Clin Immunol. 2020;145(3):982–92.
Di Candia F, Fontana P, Paglia P, Falco M, Rosano C, Piscopo C et al. Clinical heterogeneity of Kabuki syndrome in a cohort of Italian patients and review of the literature. Eur J Pediatr. 2022;181(1):171–87. Available from: https://pubmed.ncbi.nlm.nih.gov/34232366/.
Adam MP, Banka S, Bjornsson HT, Bodamer O, Chudley AE, Harris J, et al. Kabuki syndrome: International consensus diagnostic criteria. J Med Genet. 2019;56(2):89–95.
Provan D, Arnold DM, Bussel JB, Chong BH, Cooper N, Gernsheimer T et al. Updated international consensus report on the investigation and management of primary immune thrombocytopenia. Blood Adv. 2019;3(22):3780–817. Available from: https://ashpublications.org/bloodadvances/article/3/22/3780/428877/Updated-international-consensus-report-on-the.
Ladogana S, Maruzzi M, Samperi P, Perrotta S, Del Vecchio GC, Notarangelo LD, et al. Diagnosis and management of newly diagnosed childhood autoimmune haemolytic anaemia. Recommendations from the Red Cell Study Group of the Paediatric Haemato-Oncology Italian Association. Blood Transfus. 2017;15:259–67.
Fioredda F, Calvillo M, Bonanomi S, Coliva T, Tucci F, Farruggia P et al. Congenital and acquired neutropenia consensus guidelines on diagnosis from the Neutropenia Committee of the Marrow Failure Syndrome Group of the AIEOP (Associazione Italiana Emato-Oncologia Pediatrica). Pediatr Blood Cancer. 2011;57(1):10–7. Available from: https://pubmed.ncbi.nlm.nih.gov/21448998/.
Tosato F, Bucciol G, Pantano G, Putti MC, Sanzari MC, Basso G, et al. Lymphocytes subsets reference values in childhood. Cytom Part A. 2015;87(1):81–5.
Schatorjé EJH, Gemen EFA, Driessen GJA, Leuvenink J, van Hout RWNM et al. Age-matched reference values for B-lymphocyte subpopulations and CVID classifications in children. Scand J Immunol. 2011;74(5):502–10. Available from: https://pubmed.ncbi.nlm.nih.gov/21815909/.
Grunewald O, Lopez B, Brabant S, Rogeau S, Deschildre A, Phrommavanh V, et al. Immunoglobulin G (IgG) and IgG subclass reference intervals in children, using Optilite ® reagents. Clin Chem Lab Med. 2018;56(8):1319–27.
Philip P, N, Meinecke, David A, Dean J, Ayme S, Clark R, et al. Kabuki make-up (Niikawa-Kuroki) syndrome: a study of 16 non-japanese cases. Clin Dysmorphol. 1992;1:63–77.
Schrander-Stumpel C, Meinecke P, Wilson G, Gilleseen-Kaesbach G, Tinschert S, König R, et al. The Kabuki (Niikawa-Kuroki) syndrome: further delineation of the phenotype in 29 non-japanese patients. Eur J Pediatr. 1994;153(6):438–45.
Lin J, Lee W, Huang J, Chen PK, Chan K, Lo L et al. Immunologic assessment and KMT2D mutation detection in Kabuki syndrome. Clin Genet. 2015;88(3):255–60. Available from: http://www.ncbi.nlm.nih.gov/pubmed/25142838.
Lindsley AW, Saal HM, Burrow TA, Hopkin RJ, Shchelochkov O, Khandelwal P et al. Defects of B-cell terminal differentiation in patients with type-1 Kabuki syndrome. J Allergy Clin Immunol. 2016;137(1):179–187.e10. https://doi.org/10.1016/j.jaci.2015.06.002.
Choi HG, Min C, Lee CH, Kim SY. The relation of Sudden Sensorineural hearing loss in Pediatric patients with recurrent Otitis Media: a nested case-control study using a National Sample Cohort. Otol Neurotol. 2020;41(7):e836–41.
Krakau M, Dagöö BR, Hellström S, Granath A. Long-term hearing outcomes after recurrent acute otitis media during early childhood. Acta Otolaryngol. 2017;137(12):1238–43. https://doi.org/10.1080/00016489.2017.1362111.
Gidwani P, Segal E, Shanske A, Driscoll C. Chorea associated with antiphospholipid antibodies in a patient with Kabuki syndrome. Am J Med Genet Part A. 2007;143A(12):1338–41. https://doi.org/10.1002/ajmg.a.31774.
Tesch VK, Abolhassani H, Shadur B, Zobel J, Mareika Y, Sharapova S et al. Long-term outcome of LRBA deficiency in 76 patients after various treatment modalities as evaluated by the immune deficiency and dysregulation activity (IDDA) score. J Allergy Clin Immunol. 2020;145(5):1452–63. Available from: https://pubmed.ncbi.nlm.nih.gov/31887391/.
Leiding JW, Vogel TP, Santarlas VGJ, Mhaskar R, Smith MR, Carisey A et al. Monogenic early-onset lymphoproliferation and autoimmunity: Natural history of STAT3 gain-of-function syndrome. J Allergy Clin Immunol. 2022; Available from: https://pubmed.ncbi.nlm.nih.gov/36228738/.
Egg D, Rump IC, Mitsuiki N, Rojas-Restrepo J, Maccari ME, Schwab C et al. Therapeutic options for CTLA-4 insufficiency. J Allergy Clin Immunol. 2022;149(2):736–46. Available from: https://pubmed.ncbi.nlm.nih.gov/34111452/.
Liotti A, Ferrara AL, Loffredo S, Galdiero MR, Varricchi G, Di Rella F et al. Epigenetics: An opportunity to shape innate and adaptive immune responses. Immunology. 2022;167(4):451–70. Available from: https://onlinelibrary.wiley.com/doi/full/https://doi.org/10.1111/imm.13571.
Romano R, Cillo F, Moracas C, Pignata L, Nannola C, Toriello E et al. Epigenetic Alterations in Inborn Errors of Immunity. J Clin Med. 2022, Vol 11, Page 1261. 2022;11(5):1261. Available from: https://www.mdpi.com/2077-0383/11/5/1261/htm.
Passaretti F, Pignata L, Vitiello G, Alesi V, D’Elia G, Cecere F et al. Different Mechanisms Cause Hypomethylation of Both H19 and KCNQ1OT1 Imprinted Differentially Methylated Regions in Two Cases of Silver-Russell Syndrome Spectrum. Genes (Basel). 2022;13(10). Available from: https://pubmed.ncbi.nlm.nih.gov/36292759/.
Pignata L, Sparago A, Palumbo O, Andreucci E, Lapi E, Tenconi R et al. Mosaic Segmental and Whole-Chromosome Upd(11)mat in Silver-Russell Syndrome. Genes (Basel). 2021;12(4). Available from: https://pubmed.ncbi.nlm.nih.gov/33923683/.
Dutta A, Venkataganesh H, Love PE. New Insights into Epigenetic Regulation of T Cell Differentiation. Cells. 2021;10(12). Available from: https://pubmed.ncbi.nlm.nih.gov/34943965/.
Rodríguez-Cortez VC, Del Pino-Molina L, Rodríguez-Ubreva J, Ciudad L, Gómez-Cabrero D, Company C et al. Monozygotic twins discordant for common variable immunodeficiency reveal impaired DNA demethylation during naïve-to-memory B-cell transition. Nat Commun. 2015;6.
Zhang Z, Shi LH, Song L, Maurer K, Zhao X, Zackai EH et al. Chromatin Modifications in 22q11.2 Deletion Syndrome. J Clin Immunol. 2021;1853–64. https://doi.org/10.1007/s10875-021-01123-2.
Xin Z, Edmonson M, Wilkinson M, Patel A, Wu G, Liu Y et al. Exploring Genomic Alteration in Pediatric Cancer Using ProteinPaint. Nature Genetics. 2016;4–6. https://doi.org/10.1038/ng.3466.
Acknowledgements
We thank Fondazione Città della Speranza ONLUS (http://cittadellasperanza.org), Associazione di Promozione Sociale “Genitori in fuga” (https://www.genitoriinfuga.org) for their support to our scientific work. We would like to thank the patients, the patients’ families, and the nurses for their collaboration and efforts.
Author information
Authors and Affiliations
Contributions
AMar and MCP conceived and designed the study on behalf of the IPINet. SR, DMo, CA, EG, MT, FC, AP, FS, SN, EV, AMag, LB, SA, RC, LL, IDA, RR, DMe, SS, ECi, GG, AB, CP, AMar collected the data and treated the patients. Data analysis was performed by LR, AMar and ECa. The manuscript was written by AMar and LR with contributions from all authors. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics Approval
The study was approved from the local hospital Ethical Committee and was conducted in accordance with the Helsinki Declaration.
Consent to Participate
Informed consent was collected from all patients or their legal guardians.
Consent for Publication
Informed consent was collected from all patients or their legal guardians.
Conflict of Interest
The authors have no relevant financial or non-financial interests to disclose.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
On behalf of the Italian Primary Immunodeficiency Network (IPINet).
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Rossini, L., Ricci, S., Montin, D. et al. Immunological Aspects of Kabuki Syndrome: A Retrospective Multicenter Study of the Italian Primary Immunodeficiency Network (IPINet). J Clin Immunol 44, 105 (2024). https://doi.org/10.1007/s10875-024-01676-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10875-024-01676-y