Abstract
Purpose
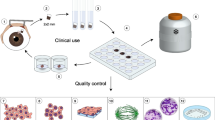
Ethanol and mitomycin C (MMC) are clinically used to treat corneal diseases such as LASEK and LASIK surgery. In this study, we investigated the effects of time-dependent alcohol and MMC in cultured rat limbal stem cells (LSCs) to determine the appropriate time for the use of this compound in the clinical setting.
Methods
LSCs (N = 10 eyes) isolated from male Wistar rats were cultured and characterized; then, isolates were divided into three groups. One group was exposed to a 20% concentration of ethanol for 5, 10, 15, 20, 25, and 30 s, and cell viability was assessed one, three, and five days following ethanol exposure using an MTT assay. To investigate the effect of MMC, cells in the second group were treated with 0.02% MMC in various periods (i.e., 15 s, 30 s, 60 s, 90 s, and 120 s) and time-dependent responses of cultured LSCs were recorded. Cells in the third group were co-treated with ethanol and MMC; then, dose and time dependency was evaluated.
Results
In comparison with the viable cells in the control group, ethanol markedly decreased the viability of cells in a time-dependent manner in days one and three. On day five, the viability of LSCs was improved significantly (p < 0.05) in comparison with day one. The number of viable progenitor cells was significantly decreased after MMC treatment in a time-dependent manner, as determined by the MTT assay (p < 0.001). The use of mitomycin, along with alcohol, decreased cell viability in all groups treated with ethanol + MMC compared to the control on days one, three, and five (p < 0.0001).
Conclusions
Our findings suggest that ethanol and MMC reduced cell viability in cultured LSCs in a time-dependent manner. In addition, when LSCs were exposed to alcohol alone, they had a better recovery process within 5 days in comparison to when exposed to mitomycin alone or mitomycin + alcohol.







Similar content being viewed by others
References
Sacchetti M, Rama P, Bruscolini A, Lambiase A (2018) Limbal stem cell transplantation: clinical results, limits, and perspectives. Stem Cells Int. https://doi.org/10.1155/2018/8086269
Dua HS, Saini JS, Azuara-Blanco A, Gupta P (2000) Limbal stem cell deficiency: concept, aetiology, clinical presentation, diagnosis and management. Indian J Ophthalmol 48:83
Dziasko MA, Armer HE, Levis HJ, Shortt AJ, Tuft S, Daniels JT (2014) Localisation of epithelial cells capable of holoclone formation in vitro and direct interaction with stromal cells in the native human limbal crypt. PLoS ONE 9:e94283
Karimi S, Arabi A, Shahraki T (2021) Alcohol and the eye. J Ophthalmic Vis Res 16:260
Antonios R, Fattah MA, Mosquera SA, Abiad BH, Sleiman K, Awwad ST (2017) Single-step transepithelial versus alcohol-assisted photorefractive keratectomy in the treatment of high myopia: a comparative evaluation over 12 months. Br J Ophthalmol 101:1106–1112
Lucena MA, Alves de ED, Krause HB, Alves de MM, Aquino do RPL (2021) : Treatment of persistent epithelial ingrowth after Lasik with mechanical debridement, use of 20% alcohol and fibrin glue. Rev. Bras. Oftalmol. 80
Altinbay D, Taskin I (2022) The effectiveness of corneal epithelial debridement performed with an alcohol-impregnated sponge. Klin Monbl Augenheilkd 239:185–190
Dua HS, Deshmukh R, Ting DSJ, Wilde C, Nubile M, Mastropasqua L, Said DG (2021) Topical use of alcohol in ophthalmology-diagnostic and therapeutic indications. Ocul Surf 21:1–15
Zhang P, Liu M, Liao R (2012) Toxic effect of using twenty percent alcohol on corneal epithelial tight junctions during LASEK. Mol Med Rep 6:33–38
Mahar PS Use of mitomycin C in ocular surgery; a narrative review. Pakistan J Ophthalmol, 35 (2019)
Geggel HS, Friend J, Thoft RA (1985) Collagen gel for ocular surface. Invest Ophthalmol Vis Sci 26:901–905
Fagerholm P, Lagali NS, Merrett K, Jackson WB, Munger R, Liu Y, Polarek JW, Söderqvist M, Griffith M (2010) A biosynthetic alternative to human donor tissue for inducing corneal regeneration: 24-month follow-up of a phase 1 clinical study. Sci Transl Med 2:4661–4661
Cohen JI, Nagy LE (2011) Pathogenesis of alcoholic liver disease: interactions between parenchymal and non-parenchymal cells. J Dig Dis 12:3–9
Luo J (2012) Mechanisms of ethanol-induced death of cerebellar granule cells. Cerebellum 11:145–154
Cherian PP, Schenker S, Henderson GI (2008) Ethanol-mediated DNA damage and PARP-1 apoptotic responses in cultured fetal cortical neurons. Alcohol Clin Exp Res 32:1884–1892
Oh JY, Yu JM, Ko JH (2013) Analysis of ethanol effects on corneal epithelium. Invest Ophthalmol Vis Sci 54:3852–3856
Sia RK, Ryan DS, Stutzman RD, Psolka M, Mines MJ, Wagner ME, Weber ED, Wroblewski KJ, Bower KS (2012) Alcohol versus brush PRK: visual outcomes and adverse effects. Lasers Surg Med 44:475–481
Tsumi E, Levy J, Pitchkhadze A, Baidousi A, Lifshitz T (2012) New approach for pterygium removal using 20% ethanol. Int Ophthalmol 32:443–448
Luger MHA, Ewering T, Arba-Mosquera S (2012) Consecutive myopia correction with transepithelial versus alcohol-assisted photorefractive keratectomy in contralateral eyes: one-year results. J Cataract Refract Surg 38:1414–1423
Moss SE, Klein R, Klein BEK (2000) Prevalence of and risk factors for dry eye syndrome. Arch Ophthalmol 118:1264–1268
de Oliveira RC, Wilson SE (2020) Biological effects of mitomycin C on late corneal haze stromal fibrosis following PRK. Exp Eye Res 200:108218
Xu H, Liu S, Xia X, Huang P, Wang P, Wu X (2001) Mitomycin C reduces haze formation in rabbits after excimer laser photorefractive keratectomy. J Refract Surg 17(3):342–349
Awwad ST, Chacra LM, Helwe C, Dhaini AR, Telvizian T, Torbey J, Abdul Fattah M, Torres-Netto EA, Hafezi F, Shetty R (2021) Mitomycin C application after corneal cross-linking for keratoconus increases stromal haze. J Refract Surg 37:83–90
Tchah H, Cho EH, Kook MS (2004) Evaluation for safety of cultured corneal fibroblasts with cotreatment of alcohol and mitomycin C. Invest Ophthalmol Vis Sci 45:86–92
Nassiri N, Farahangiz S, Rahnavardi M, Rahmani L, Nassiri N (2008) Corneal endothelial cell injury induced by mitomycin-C in photorefractive keratectomy: nonrandomized controlled trial. J Cataract Refract Surg 34:902–908
Acknowledgements
This work was done in small animal's transplantation ward, cellular and molecular research center, Medical Basic Sciences Institute, Ahvaz Jundishapur University of Medical Sciences, Ahvaz, Iran.
Funding
This work was funded by Ahvaz Jundishapur University of Medical Sciences..
Author information
Authors and Affiliations
Contributions
Ava Nasrolahi and Fereshteh Nejaddehbashi wrote the main manuscript text, Mitra Zamani isolated limbal stem cells, Vahid Bayati performed immunocytochemistry. All authors reviewed the manuscript."
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Conflict of interest
The authors have not disclosed any competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bayati, V., Nasrolahi, A., Zamani, M. et al. Evaluation of the effects of ethanol and mitomycin on survival of rat limbal stem cells: an in vitro study. Int Ophthalmol 43, 2503–2512 (2023). https://doi.org/10.1007/s10792-023-02650-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-023-02650-0