Abstract
Purpose
To compare changes in asphericity of anterior and posterior corneal surfaces for different myopia patients after corneal topography-guided femtosecond-assisted laser in situ keratomileuses (FS-LASIK), and to analyze correlations between asphericity of corneal surfaces and preoperative spherical equivalence (SEQ).
Methods
In this prospective study, 59 patients who underwent corneal topography-guided FS-LASIK surgery were enrolled and divided into the mild–moderate myopia group (67 eyes) and the high myopia group (44 eyes). Postoperative follow-ups were performed at 1, 3, and 6 months. Postoperative changes in aspherical coefficient (Q values), corneal higher-order aberrations (HOAs), and spherical aberrations (Z40) were compared between the two groups. Relevance between Q value changes and SEQ, HOAs, and Z40 as well as between SEQ and changes of HOAs and Z40 was analyzed.
Results
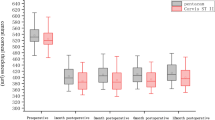
There was a significant increase in Q values of the anterior (each diameter) and posterior (6–8 mm) corneal surface in both groups than before surgery (P < 0.001). Q values of corneal anterior (each diameter) and posterior (7–9 mm) surface in the high group were considerably larger than the mild–moderate group (P < 0.05). Corneal anterior surface HOAs and Z40 values in the high group largely exceeded those of the mild–moderate group (P < 0.001). The preoperative SEQ was linearly correlated with postoperative anterior Q change (ΔQ), HOAs change (ΔHOAs), and spherical aberration change (ΔZ40).
Conclusion
The changes of corneal asphericity in patients with high myopia were greater than mild–moderate myopia, with more corneal HOAs and Z40 introduced when corneal topography-guided FS-LASIK was conducted.






Similar content being viewed by others
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on request.
References
Ahn JM, Choi BJ, Kim EK, Sgrignoli B (2013) Three different aspheric treatment algorithms of laser-assisted sub-epithelial keratectomy in patients with high myopia. Jpn J Ophthalmol 57:191–198. https://doi.org/10.1007/s10384-012-0218-4
Villa C, Gutierrez R, Jimenez JR, Gonzalez-Meijome JM (2007) Night vision disturbances after successful LASIK surgery. Br J Ophthalmol 91:1031–1037. https://doi.org/10.1136/bjo.2006.110874
El Awady HE, Ghanem AA, Saleh SM (2011) Wavefront-optimized ablation versus topography-guided customized ablation in myopic LASIK: comparative study of higher order aberrations. Ophthalmic Surg Lasers Imaging Retina 42:314–320. https://doi.org/10.3928/15428877-20110421-01
Jain AK, Malhotra C, Pasari A, Kumar P, Moshirfar M (2016) Outcomes of topography-guided versus wavefront-optimized laser in situ keratomileusis for myopia in virgin eyes. J Cataract Refract Surg 42:1302–1311. https://doi.org/10.1016/j.jcrs.2016.06.035
Kim J, Choi S-H, Lim DH, Yang CM, Yoon G-J, Chung T-Y (2019) Topography-guided versus wavefront-optimized laser in situ keratomileusis for myopia: surgical outcomes. J Cataract Refract Surg 45:959–965. https://doi.org/10.1016/j.jcrs.2019.01.031
Holland S, Lin DT, Tan JC (2013) Topography-guided laser refractive surgery. Curr Opin Ophthalmol 24:302–309. https://doi.org/10.1097/ICU.0b013e3283622a59
Tan J, Simon D, Mrochen M, Por YM (2012) Clinical results of topography-based customized ablations for myopia and myopic astigmatism. J Refract Surg 28:S829–S836. https://doi.org/10.3928/1081597x-20121005-04
Zhang Y-L, Xu X-H, Cao L-J, Liu L (2020) Corneal curvature, asphericity, and aberrations after transepithelial photorefractive keratectomy and femtosecond laser-assisted in situ keratomileusis for myopia: a prospective comparative study. Indian J Ophthalmol 68:2945. https://doi.org/10.4103/ijo.IJO_1106_20
Bao F, Cao S, Wang J, Wang Y, Huang W, Zhu R, Zheng X, Huang J, Chen S, Li Y (2019) Regional changes in corneal shape over a 6-month follow-up after femtosecond-assisted LASIK. J Cataract Refract Surg 45:766–777. https://doi.org/10.1016/j.jcrs.2018.12.017
Patel SV, Erie JC, McLaren JW, Bourne WM (2007) Confocal microscopy changes in epithelial and stromal thickness up to 7 years after LASIK and photorefractive keratectomy for myopia. J Refract Surg 23:385–392. https://doi.org/10.3928/1081-597X-20070401-11
Ganesh S, Patel U, Brar S (2015) Posterior corneal curvature changes following refractive small incision lenticule extraction. Clin Ophthalmol 9:1359. https://doi.org/10.2147/OPTH.S84354
Yamaguchi T, Ohnuma K, Tomida D, Konomi K, Satake Y, Negishi K, Tsubota K, Shimazaki J (2011) The contribution of the posterior surface to the corneal aberrations in eyes after keratoplasty. Investig Ophthalmol Vis Sci 52:6222–6229. https://doi.org/10.1167/iovs.11-7647
Vetter JM, Holtz C, Vossmerbaeumer U, Pfeiffer N (2012) Irregularity of the posterior corneal surface during applanation using a curved femtosecond laser interface and microkeratome cutting head. J Refract Surg 28:209–214. https://doi.org/10.3928/1081597X-20120208-02
Wu W, Wang Y (2016) Corneal higher-order aberrations of the anterior surface, posterior surface, and total cornea after SMILE, FS-LASIK, and FLEx surgeries. Eye Contact Lens 42:358–365. https://doi.org/10.1097/ICL.0000000000000225
Jin H-Y, Wan T, Yu X-N, Wu F, Yao K (2018) Corneal higher-order aberrations of the anterior surface, posterior surface, and total cornea after small incision lenticule extraction (SMILE): high myopia versus mild to moderate myopia. BMC Ophthalmol 18:1–9. https://doi.org/10.1186/s12886-018-0965-1
Gyldenkerne A, Ivarsen A, Hjortdal JØ (2015) Comparison of corneal shape changes and aberrations induced by FS-LASIK and SMILE for myopia. J Refract Surg 31:223–229. https://doi.org/10.3928/1081597X-20150303-01
Xi L (2020) Wavefront properties of the anterior and posterior corneal surface after transepithelial photorefractive keratectomy in myopia. Exp Ther Med 19:1183–1188. https://doi.org/10.3892/etm.2019.8338
Juhasz E, Kranitz K, Sandor GL, Gyenes A, Toth G, Nagy ZZ (2014) Wavefront properties of the anterior and posterior corneal surface after photorefractive keratectomy. Cornea 33:172–176. https://doi.org/10.1097/ICO.0000000000000035
Chen X, Wang Y, Zhang J, Yang S-N, Li X, Zhang L (2017) Comparison of ocular higher-order aberrations after SMILE and Wavefront-guided Femtosecond LASIK for myopia. BMC Ophthalmol 17:1–8. https://doi.org/10.1186/s12886-017-0431-5
Davis WR, Raasch TW, Mitchell GL, Mutti DO, Zadnik K (2005) Corneal asphericity and apical curvature in children: a cross-sectional and longitudinal evaluation. Investig Ophthalmol Vis Sci 46:1899–1906. https://doi.org/10.1167/iovs.04-0558
Huang H, Yang J, Bao H, Chen S, Xia B, Zou J (2012) Retrospective analysis of changes in the anterior corneal surface after Q value guided LASIK and LASEK in high myopic astigmatism for 3 years. BMC Ophthalmol 12:1–6. https://doi.org/10.1186/1471-2415-12-15
Funding
This work is supported by the Tianjin Key Clinical Disciplines (Specialties) Construction Project (TJLCZDXKM013).
Author information
Authors and Affiliations
Contributions
YW and SSS have equal first authors. Study design (WY, HY, WSH); data collecting (WY, LZL, WGQ); data and statistical analysis (SSS, WY); writing the manuscript (SSS, WY); revision of the manuscript (HY, ZSZ, WRH).
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing financial interest.
Ethical approval
This study was performed in full compliance with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of Tianjin Medical University (No. ChiCTR2100045632).
Informed consent
Full and informed consent was given by each subject for these experiments.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wu, Y., Sun, S., Liu, Z. et al. Changes in asphericity of anterior and posterior corneal surfaces for mild–moderate and high myopia after topography-guided FS-LASIK. Int Ophthalmol 42, 3555–3565 (2022). https://doi.org/10.1007/s10792-022-02356-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-022-02356-9