Abstract
Purpose
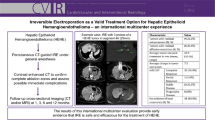
To compare the therapeutic effects of 125I versus non-125I combined with transcatheter arterial chemoembolization (TACE) for the treatment of unresectable hepatocellular carcinoma (HCC) with obstructive jaundice.
Methods
A retrospective analysis was conducted using the records of 54 consecutive patients who were initially diagnosed with HCC with obstructive jaundice between May 2009 and July 2016. Twenty-one cases (group A) were treated with percutaneous transhepatic biliary drainage (PTBD) followed by 125I radioactive seed strip implantation through the PTBD tube. After the total serum bilirubin level was reduced to normal and the liver function recovered to Child–Pugh class A or early B, TACE was conducted. In 33 cases (group B) PTBD was performed in combination with TACE without applying the 125I radioactive seeds. The duration of biliary patency and survival were analyzed.
Results
The technical success rate in both groups was 100%. The median biliary patency time was 6.000 ± 0.315 months (95% CI 5.382–6.618 months) in group A and 4.000 ± 0.572 months (95% CI 2.879–5.121 months) in group B; the two groups were significantly different (P = 0.001). The median survival was 11.000 ± 0.864 months (95% CI 9.306–12.694 months) in group A and 9.000 ± 0.528 months (95% CI 7.965–10.035 months) in group B; the two groups were significantly different (P = 0.022).
Conclusions
The combination of 125I with TACE was more effective than TACE without the radioactive seeds for treating patients with unresectable HCC with obstructive jaundice. Future prospective trials with larger samples will be required to validate these results.



Similar content being viewed by others
References
Mesci A, Gurer S, Guzel G, et al. Obstructive jaundice caused by hepatocellular carcinoma with bile duct tumor thrombi: a case report. Eurasian J Med. 2008;40:45–47.
Minami Y, Kudo M. Hepatocellular carcinoma with obstructive jaundice: endoscopic and percutaneous biliary drainage. Dig Dis. 2012;30:592–597.
Park S, Park JY, Chung MJ, et al. The efficacy of endoscopic palliation of obstructive jaundice in hepatocellular carcinoma. Yonsei Med J. 2014;55:1267–1272.
Choi J, Ryu JK, Lee SH, et al. Biliary drainage for obstructive jaundice caused by unresectable hepatocellular carcinoma: the endoscopic versus percutaneous approach. Hepatobiliary Pancreat Dis Int. 2012;11:636–642.
Shiu W, Dewar G, Leung N, et al. Hepatocellular carcinoma in Hong Kong: clinical study on 340 cases. Oncology. 1990;47:241–245.
Lau W, Leung K, Leung TW, et al. A logical approach to hepatocellular carcinoma presenting with jaundice. Ann Surg. 1997;225:281–285.
Cho HC, Lee JK, Lee KH, et al. Are endoscopic or percutaneous biliary drainage effective for obstructive jaundice caused by hepatocellular carcinoma? Eur J Gastroenterol Hepatol. 2011;23:224–231.
Suh YG, Kim DY, Han KH, et al. Effective biliary drainage and proper treatment improve outcomes of hepatocellular carcinoma with obstructive jaundice. Gut Liver. 2014;8:526–535.
Park HC, Park HB, Chung CY, et al. Acute obstructive cholangitis complicated by tumor migration after transarterial chemoembolization: a case report and literature review. Korean J Gastroenterol. 2014;63:171–175.
Garcea G, Ong SL, Dennison AR, Berry DP, Maddern GJ. Palliation of malignant obstructive jaundice. Dig Dis Sci. 2009;54:1184–1198. https://doi.org/10.1007/s10620-008-0479-4.
Peng SY, Wang JW, Liu YB, et al. Surgical Intervention for obstructive jaundice due to biliary tumor thrombus in hepatocellular carcinoma. World J Surg. 2004;28:43–46.
Ahmed S, de Souza NN, Qiao W, et al. Quality of life in hepatocellular carcinoma patients treated with transarterial chemoembolization. HPB Surg. 2016;2016:6120143. https://doi.org/10.1155/2016/6120143.
Park CK, Bae SH, Yang HJ, et al. Successful treatment of stereotactic body radiation therapy combined with transarterial chemolipiodolization for hepatocellular carcinoma with biliary obstruction. Korean J Intern Med. 2011;26:94–98.
Choi J, Ryu JK, Lee SH, et al. Palliative treatment of unresectable hepatocellular carcinoma with obstructive jaundice using biliary drainage with subsequent transarterial chemoembolization. J Palliat Med. 2013;16:1026–1033.
Chengwu T, Jian S, Wenming F, et al. Combination therapy of radiofrequency ablation and transarterial chemoembolization for unresectable hepatocellular carcinoma. Medicine (Baltimore) 2016; 95: e3754. Published online 2016 May 20. https://doi.org/10.1097/md.0000000000003754.
Jiao D, Xinwei H, Wang Y, et al. Y-configured metallic stent combined with 125I seed strands cavity brachytherapy for a patient with type IV Klatskin tumor. J Contemp Brachytherapy. 2016; 8: 356–360. https://doi.org/10.5114/jcb.2016.61704.
Wenhui LI, Zhenyu DAI, Lizheng YAO, et al. Chemoembolization and stenting combined with iodine-125 seed strands for the treatment of hepatocellular carcinoma with inferior vena cava obstruction. Exp Ther Med. 2015;10:973–977.
Kikuchi L, Oliveira A-S, et al. Hepatocellular carcinoma management in nonalcoholic fatty liver disease patients. Am J Clin Oncol. 2016;39:428–432.
Huang W-K, Yang S-F, You L-N, et al. Transcatheter arterial chemoembolisation (TACE) plus S-1 for the treatment of BCLC stage B hepatocellular carcinoma refractory to TACE. Contemp Oncol (Pozn). 2016;20:468–474.
Huang M, Lin Q, Wang H, et al. Survival benefit of chemoembolization plus Iodine125 seed implantation in unresectable hepatitis B-related hepatocellular carcinoma with PVTT: a retrospective matched cohort study. Eur Radiol. 2016;26:3428–3436.
Matsueda K, Yamamoto H, Umeoka F, et al. Effectiveness of endoscopic biliary drainage for unresectable hepatocellular carcinoma associated with obstructive jaundice. J Gastroenterol. 2001;36:173–180.
Lee JW, Han JK, Kim TK, et al. Obstructive jaundice in hepatocellular carcinoma: response after percutaneous transhepatic biliary drainage and prognostic factors. Cardiovasc Interv Radiol. 2002;25:176–179.
Zhang Y-F, Wei W, Wang J-H, et al. Transarterial chemoembolization combined with sorafenib for the treatment of hepatocellular carcinoma with hepatic vein tumor thrombus. Onco Targets Ther. 2016;9:4239–4246.
Qin L-X, Tang Z-Y. Hepatocellular carcinoma with obstructive jaundice: diagnosis, treatment and prognosis. World J Gastroenterol. 2003;9:385–391.
Bigot P, Buchanan GM, Hamy A, et al. Rupture of hepatocellular carcinoma into the biliary system with resulting bile duct thrombi: report of two cases. Case Rep Gastroenterol. 2007;1:123–129.
Paik EK, Kim M-S, Jang WI, et al. Benefits of stereotactic ablative radiotherapy combined with incomplete transcatheter arterial chemoembolization in hepatocellular carcinoma. Radiat Oncol. 2016: 22. Published online 2016 Feb 19. https://doi.org/10.1186/s13014-016-0597-7.
Ingold JA, Reed GB, Kaplan HS, Bagshaw MA. Radiation hepatitis. Am J Roentgenol Radium Ther Nucl Med. 1965;93:200–208.
Pan CC, Kavanagh BD, Dawson LA, et al. Radiation-associated liver injury. Int J Radiat Oncol Biol Phys. 2010;76:S94–S100. https://doi.org/10.1016/j.ijrobp.2009.06.092.
Marchal F, Elias D, Rauch P, et al. Prevention of biliary lesions that may occur during radiofrequency ablation of the liver. Ann Surg. 2006;243:82–88.
Schmidt A, Bloechinger M, Weber A, et al. Short-term effects and adverse events of endoscopically applied radiofrequency ablation appear to be comparable with photodynamic therapy in hilar cholangiocarcinoma. United European Gastroenterol J. 2016;4:570–579.
Yu X, Li J, Zhong X, et al. Combination of Iodine-125 brachytherapy and chemotherapy for locally recurrent stage III non-small cell lung cancer after concurrent chemoradiotherapy. BMC Cancer. 2015;15:656.
Sacco R, Mismas V, Marceglia S, et al. Transarterial radioembolization for hepatocellular carcinoma: an update and perspectives. World J Gastroenterol. 2015;21:6518–6525.
Kennedy AS, Coldwell D, Nutting C, et al. Resin 90Y-microsphere brachytherapy for unresectable colorectal liver metastases: modern USA experience. Int J Radiat Oncol Biol Phys. 2006;65:412–425.
Zhou ZG, Chen JB, Qiu HB, et al. Parecoxib prevents complications in hepatocellular carcinoma patients receiving hepatic transarterial chemoembolization: a prospective score-matched cohort study. Oncotarget. 2016;7:27938–27945.
Siriwardana RC, Niriella MA, Dassanayake AS, et al. Factors affecting post-embolization fever and liver failure after trans-arterial chemo-embolization in a cohort without background infective hepatitis—a prospective analysis. BMC Gastroenterol. 2015; 96. Published online 2015 Aug 4. https://doi.org/10.1186/s12876-015-0329-8.
Wigmore SJ, Redhead DN, Thomson BN, et al. Postchemoembolisation syndrome–tumour necrosis or hepatocyte injury? Br J Cancer. 2003;89:1423–1427.
Khan KN, Nakata K, Kusumoto Y, et al. Evaluation of nontumorous tissue damage by transcatheter arterial embolization for hepatocellular carcinoma. Cancer Res. 1991;51:5667–5671.
Kecheng Xu, Niu Lizhi, Feng Mu, et al. Cryosurgery in combination with brachytherapy of iodine-125 seeds for pancreatic cancer. Gland Surg. 2013;2:91–99.
Chuan-Xing L, Xu H, Bao-Shan H, et al. Efficacy of therapy for hepatocellular carcinoma with portal vein tumor thrombus: Chemoembolization and stent combined with iodine-125 seed. Cancer Biol Ther. 2011;10:865–871. https://doi.org/10.4161/cbt.12.10.17676.
Gao J, Zhang Q, Zhang J, et al. Radiofrequency ablation of the main lesion of hepatocellular carcinoma and bile duct tumor thrombus as a radical therapeutic alternative. Med (Baltimore). 2015;94:e1122. https://doi.org/10.1002/1097-0142(19940301)73:5<1335:AID-CNCR2820730505>3.0.CO;2-M.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have declared that no conflict of interest exists.
Rights and permissions
About this article
Cite this article
Li, S., He, X., Dang, L. et al. Efficacy of 125I Versus Non-125I Combined with Transcatheter Arterial Chemoembolization for the Treatment of Unresectable Hepatocellular Carcinoma with Obstructive Jaundice. Dig Dis Sci 63, 321–328 (2018). https://doi.org/10.1007/s10620-017-4899-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-017-4899-x