Abstract
Purpose
Although there is research establishing that physical pain is a risk factor for suicidal ideation, there is limited understanding of how physical pain confers risk.
Methods
The current study uses ecological momentary assessment to explore hopelessness as a potential mechanism of physical pain’s effect on suicidal ideation in two distinct samples: an undergraduate population reporting elevated levels of suicidal ideation and an outpatient population with borderline personality disorder receiving comprehensive dialectical behavior therapy.
Results
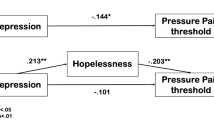
Our results demonstrated that hopelessness significantly mediated the relationship between physical pain and suicidal ideation in both samples. This implies that physical pain might increase hopelessness, which may in turn increase suicidal ideation.
Conclusions
Our study adds to a growing body of research of risk factors for suicide, and future research should explore this relationship between physical pain and hopelessness with suicidal behavior.

Similar content being viewed by others
References
Al-Dajani, N., Uliaszek, A. A., & Hamdullahpur, K. (2019). It’s the thought that counts: Belief in suicide as an escape moderates the relationship between emotion dysregulation and suicidal ideation cross-sectionally and longitudinally. Borderline Personality Disorder and Emotion Dysregulation, 6(1), 16. https://doi.org/10.1186/s40479-019-0112-5.
Al-Obaidi, S. M., Nelson, R. M., Al-Awadhi, S., & Al-Shuwaie, N. (2000). The role of anticipation and fear of pain in the persistence of avoidance behavior in patients with chronic low back pain. Spine, 25(9), 1126–1131. https://doi.org/10.1097/00007632-200005010-00014.
Aldrich, S., Eccleston, C., & Crombez, G. (2000). Worrying about chronic pain: Vigilance to threat and misdirected problem solving. Behaviour Research and Therapy, 38(5), 457–470. https://doi.org/10.1016/s0005-7967(99)00062-5.
Arntz, A., van Eck, M., de Jong, P., & van den Hout, M. A. (1990). The relationship between underpredicted pain and escape. Behaviour Research and Therapy, 28(1), 87–90. https://doi.org/10.1016/0005-7967(90)90059-r.
Asparouhov, T., & Muthén, B. (2019). Latent variable centering of predictors and mediators in Multilevel and Time-Series models. Structural Equation Modeling: A Multidisciplinary Journal, 26(1), 119–142. https://doi.org/10.1080/10705511.2018.1511375.
Basten-Günther, J., Peters, M., & Lautenbacher, S. (2019). Optimism and the experience of Pain: A systematic review. Behavioral Medicine (Washington D C), 45(4), 323–339. https://doi.org/10.1080/08964289.2018.1517242.
Baumeister, R. F. (1990). Suicide as escape from self. Psychological Review, 97(1), 90–113. https://doi.org/10.1037/0033-295x.97.1.90.
Beck, A. T., Kovacs, M., & Weissman, A. (1975). Hopelessness and suicidal behavior: An overview. Journal of the American Medical Association, 234(11), 1146–1149. https://doi.org/10.1001/jama.1975.03260240050026.
Beck, A. T., Brown, G., & Steer, R. A. (1989). Prediction of eventual suicide in psychiatric inpatients by clinical ratings of hopelessness. Journal of Consulting and Clinical Psychology, 57, 309–310. https://doi.org/10.1037/0022-006X.57.2.309.
Beck, A. T., Brown, G., Berchick, R. J., Stewart, B. L., & Steer, R. A. (1990). Relationship between hopelessness and ultimate suicide: A replication with psychiatric outpatients. The American Journal of Psychiatry, 147(2), 190–195. https://doi.org/10.1176/ajp.147.2.190.
Beck, A. T., Steer, R. A., Beck, J. S., & Newman, C. F. (1993). Hopelessness, Depression, suicidal ideation, and clinical diagnosis of Depression. Suicide and Life-Threatening Behavior, 23(2), 139–145. https://doi.org/10.1111/j.1943-278X.1993.tb00378.x.
Burr, E. M., Rahm-Knigge, R. L., & Conner, B. T. (2018). The differentiating role of state and trait hopelessness in suicidal ideation and suicide attempt. Archives of Suicide Research: Official Journal of the International Academy for Suicide Research, 22(3), 510–517. https://doi.org/10.1080/13811118.2017.1366960.
Cáceda, R., Kordsmeier, N. C., Golden, E., Gibbs, H. M., & Delgado, P. L. (2017). Differential Processing of Physical and Psychological Pain during Acute Suicidality. Psychotherapy and Psychosomatics, 86(2), 116–118. https://doi.org/10.1159/000450713.
Cáceda, R., Kim, D. J., Carbajal, J. M., & Hou, W. (2022). The experience of Pain is strongly Associated with Poor Sleep Quality and increased risk for suicide. Archives of Suicide Research: Official Journal of the International Academy for Suicide Research, 26(3), 1572–1586. https://doi.org/10.1080/13811118.2021.1939208.
Calati, R., Laglaoui Bakhiyi, C., Artero, S., Ilgen, M., & Courtet, P. (2015). The impact of physical pain on suicidal thoughts and behaviors: Meta-analyses. Journal of Psychiatric Research, 71, 16–32. https://doi.org/10.1016/j.jpsychires.2015.09.004.
Chatard, A., & Selimbegović, L. (2011). When self-destructive thoughts flash through the mind: Failure to meet standards affects the accessibility of suicide-related thoughts. Journal of Personality and Social Psychology, 100, 587–605. https://doi.org/10.1037/a0022461.
Chochinov, H. M., Wilson, K. G., Enns, M., & Lander, S. (1998). Depression, hopelessness, and suicidal ideation in the terminally ill. Psychosomatics, 39(4), 366–370. https://doi.org/10.1016/S0033-3182(98)71325-8.
Conversano, C., Rotondo, A., Lensi, E., Della Vista, O., Arpone, F., & Reda, M. A. (2010). Optimism and its impact on Mental and Physical Well-Being. Clinical Practice and Epidemiology in Mental Health: CP & EMH, 6, 25–29. https://doi.org/10.2174/1745017901006010025.
Corbett, M., Foster, N. E., & Ong, B. N. (2007). Living with low back pain—stories of hope and despair. Social Science & Medicine, 65(8), 1584–1594. https://doi.org/10.1016/j.socscimed.2007.06.008.
Czyz, E. K., Horwitz, A. G., Arango, A., & King, C. A. (2019). Short-term change and prediction of suicidal ideation among adolescents: A daily diary study following psychiatric hospitalization. Journal of Child Psychology and Psychiatry and Allied Disciplines, 60(7), 732–741. https://doi.org/10.1111/jcpp.12974.
Durant, T., Mercy, J., Kresnow, M., Simon, T., Potter, L., & Hammond, W. (2006). Racial differences in hopelessness as a risk factor for a nearly Lethal suicide attempt. Journal of Black Psychology - J BLACK PSYCHOL, 32, 285–302. https://doi.org/10.1177/0095798406290468.
Eccleston, C., & Crombez, G. (1999). Pain demands attention: A cognitive-affective model of the interruptive function of pain. Psychological Bulletin, 125(3), 356–366. https://doi.org/10.1037/0033-2909.125.3.356.
Edwards, R. R., Smith, M. T., Kudel, I., & Haythornthwaite, J. (2006). Pain-related catastrophizing as a risk factor for suicidal ideation in chronic pain. Pain, 126(1–3), 272–279. https://doi.org/10.1016/j.pain.2006.07.004.
Facts About Suicide | Suicide | CDC. (2023, May 17). https://www.cdc.gov/suicide/facts/index.html.
Franklin, J. C., Hessel, E. T., & Prinstein, M. J. (2011). Clarifying the role of pain tolerance in suicidal capability. Psychiatry Research, 189(3), 362–367. https://doi.org/10.1016/j.psychres.2011.08.001.
Groholt, B., Ekeberg, Ø., & Haldorsen, T. (2006). Adolescent suicide attempters: What predicts future suicidal acts? Suicide & Life-Threatening Behavior, 36(6), 638–650. https://doi.org/10.1521/suli.2006.36.6.638.
Hall, R. C., Platt, D. E., & Hall, R. C. (1999). Suicide risk assessment: A review of risk factors for suicide in 100 patients who made severe suicide attempts. Evaluation of suicide risk in a time of managed care. Psychosomatics, 40(1), 18–27. https://doi.org/10.1016/S0033-3182(99)71267-3.
Hanssen, M. M., Peters, M. L., Vlaeyen, J. W. S., Meevissen, Y. M. C., & Vancleef, L. M. G. (2013). Optimism lowers pain: Evidence of the causal status and underlying mechanisms. Pain, 154(1), 53–58. https://doi.org/10.1016/j.pain.2012.08.006.
Juurlink, D. N., Herrmann, N., Szalai, J. P., Kopp, A., & Redelmeier, D. A. (2004). Medical illness and the risk of suicide in the elderly. Archives of Internal Medicine, 164(11), 1179–1184. https://doi.org/10.1001/archinte.164.11.1179.
Kim, S. H. (2016). Suicidal ideation and suicide attempts in older adults: Influences of chronic illness, functional limitations, and pain. Geriatric Nursing (New York, N.Y.), 37(1), 9–12. https://doi.org/10.1016/j.gerinurse.2015.07.006.
Kim, D. J., Job, A., Gokarakonda, S., Huang, C., Chekuri, L., Carbajal, J. M., & Cáceda, R. (2022). Synergistic effect of chronic pain and nonsuicidal self-harm on pain sensitivity. European Archives of Psychiatry and Clinical Neuroscience, 272(3), 371–380. https://doi.org/10.1007/s00406-021-01283-7.
Kirtley, O. J., Rodham, K., & Crane, C. (2020). Understanding suicidal ideation and behaviour in individuals with chronic pain: A review of the role of novel transdiagnostic psychological factors. The Lancet Psychiatry, 7(3), 282–290. https://doi.org/10.1016/S2215-0366(19)30288-3.
Kleiman, E. M., Turner, B. J., Fedor, S., Beale, E. E., Huffman, J. C., & Nock, M. K. (2017). Examination of real-time fluctuations in suicidal ideation and its risk factors: Results from two ecological momentary assessment studies. Journal of Abnormal Psychology, 126, 726–738. https://doi.org/10.1037/abn0000273.
Kleiman, E. M., Yeager, A. L., Grove, J. L., Kellerman, J. K., & Kim, J. S. (2020). Real-time Mental Health Impact of the COVID-19 pandemic on College students: Ecological momentary Assessment Study. JMIR Mental Health, 7(12), e24815. https://doi.org/10.2196/24815.
Klonsky, E. D., & May, A. M. (2015). The three-step theory (3ST): A new theory of suicide rooted in the ideation-to-action framework. International Journal of Cognitive Therapy, 8(2), 114–129. https://doi.org/10.1521/ijct.2015.8.2.114.
Kraemer, H. C., Gullion, C. M., Rush, A. J., Frank, E., & Kupfer, D. J. (1994). Can state and trait variables be disentangled? A methodological framework for psychiatric disorders. Psychiatry Research, 52(1), 55–69. https://doi.org/10.1016/0165-1781(94)90120-1.
Leeuw, M., Goossens, M., Linton, S., Crombez, G., Boersma, K., & Vlaeyen, J. (2007). The fear-avoidance model of Musculoskeletal Pain: Current state of scientific evidence. Journal of Behavioral Medicine, 30, 77–94. https://doi.org/10.1007/s10865-006-9085-0.
Lew, B., Huen, J., Yu, P., Yuan, L., Wang, D. F., Ping, F., Talib, M. A., Lester, D., & Jia, C. X. (2019). Associations between depression, anxiety, stress, hopelessness, subjective well-being, coping styles and suicide in Chinese university students. PLOS ONE, 14(7), e0217372. https://doi.org/10.1371/journal.pone.0217372.
O’Connor, R. C., & Cassidy, C. (2007). Predicting hopelessness: The interaction between optimism/pessimism and specific future expectancies. Cognition and Emotion, 21, 596–613. https://doi.org/10.1080/02699930600813422.
Orbach, I., Stein, D., Palgi, Y., Asherov, J., Har-Even, D., & Elizur, A. (1996). Perception of physical pain in accident and suicide attempt patients: Self-preservation vs self-destruction. Journal of Psychiatric Research, 30(4), 307–320. https://doi.org/10.1016/0022-3956(96)00008-8.
Orbach, I., Palgi, Y., Stein, D., Har-even, D., Lotem-peleg, M., Asherov, J., & Elizur, A. (1996a). Tolerance for physical pain in suicidal subjects. Death Studies, 20(4), 327–341. https://doi.org/10.1080/07481189608252786.
Qiu, T., Klonsky, E. D., & Klein, D. N. (2017). Hopelessness predicts suicide ideation but not attempts: A 10-Year longitudinal study. Suicide and Life-Threatening Behavior, 47(6), 718–722. https://doi.org/10.1111/sltb.12328.
Racine, M. (2018). Chronic pain and suicide risk: A comprehensive review. Progress in Neuro-Psychopharmacology & Biological Psychiatry, 87(Pt B), 269–280. https://doi.org/10.1016/j.pnpbp.2017.08.020.
Rizvi, S. L., Hughes, C. D., Hittman, A. D., & Vieira Oliveira, P. (2017). Can trainees effectively deliver Dialectical Behavior Therapy for individuals with Borderline personality disorder? Outcomes from a training clinic. Journal of Clinical Psychology, 73(12), 1599–1611. https://doi.org/10.1002/jclp.22467.
Rosseel, Y. (2012). Lavaan: An R Package for Structural equation modeling. Journal of Statistical Software, 48, 1–36. https://doi.org/10.18637/jss.v048.i02.
Santos, J., Martins, S., Azevedo, L. F., & Fernandes, L. (2020). Pain as a risk factor for suicidal behavior in older adults: A systematic review. Archives of Gerontology and Geriatrics, 87, 104000. https://doi.org/10.1016/j.archger.2019.104000.
Smith, J. M., Alloy, L. B., & Abramson, L. Y. (2006). Cognitive vulnerability to depression, rumination, hopelessness, and suicidal ideation: Multiple pathways to self-injurious thinking. Suicide & Life-Threatening Behavior, 36(4), 443–454. https://doi.org/10.1521/suli.2006.36.4.443.
Stewart, S. M., Kennard, B. D., Lee, P. W. H., Mayes, T., Hughes, C., & Emslie, G. (2005). Hopelessness and suicidal ideation among adolescents in two cultures. Journal of Child Psychology and Psychiatry and Allied Disciplines, 46(4), 364–372. https://doi.org/10.1111/j.1469-7610.2004.00364.x.
Tang, N. K. Y., & Crane, C. (2006). Suicidality in chronic pain: A review of the prevalence, risk factors and psychological links. Psychological Medicine, 36(5), 575–586. https://doi.org/10.1017/S0033291705006859.
Treede, R. D., Rief, W., Barke, A., Aziz, Q., Bennett, M. I., Benoliel, R., Cohen, M., Evers, S., Finnerup, N. B., First, M. B., Giamberardino, M. A., Kaasa, S., Kosek, E., Lavand’homme, P., Nicholas, M., Perrot, S., Scholz, J., Schug, S., Smith, B. H., & Wang, S. J. (2015). A classification of chronic pain for ICD-11. Pain, 156(6), 1003–1007. https://doi.org/10.1097/j.pain.0000000000000160.
Wang, Y., Jiang, N., Cheung, E. F. C., Sun, H., & Chan, R. C. K. (2015). Role of depression severity and impulsivity in the relationship between hopelessness and suicidal ideation in patients with major depressive disorder. Journal of Affective Disorders, 183, 83–89. https://doi.org/10.1016/j.jad.2015.05.001.
Wetzel, R. D. (1976). Hopelessness, depression, and suicide intent. Archives of General Psychiatry, 33(9), 1069–1073. https://doi.org/10.1001/archpsyc.1976.01770090059005.
Zhang, L., Cai, H., Bai, W., Zou, S. Y., Feng, K. X., Li, Y. C., Liu, H. Z., Du, X., Zeng, Z. T., Lu, C. M., Zhang, L., Mi, W. F., Ding, Y. H., Yang, J. J., Jackson, T., Cheung, T., Su, Z., An, F. R., & Xiang, Y. T. (2022). Prevalence of suicidality in clinically stable patients with major depressive disorder during the COVID-19 pandemic. Journal of Affective Disorders, 307, 142–148. https://doi.org/10.1016/j.jad.2022.03.042.
Funding
This work was supported by the Busch Biomedical Award awarded to Shireen Rizvi and Evan Kleiman.
Author information
Authors and Affiliations
Contributions
Hannah R. Krall. Conceptualization, Methodology, Writing original draft, Writing review & editing. Allison K. Ruork. Methodology, Writing Review & Editing. Shireen L. Rizvi. Conceptualization, Methodology, Writing review & editing, Supervision. Evan M. Kleiman. Conceptualization, Methodology, Writing review & editing, Supervision.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declared that there were no conflicts of interest with respect to the authorship or the publication of this article.
Animal Rights
No animal studies were carried out by the authors for this article.
Consent to Participate
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Krall, H.R., Ruork, A.K., Rizvi, S.L. et al. Hopelessness as a Mechanism of the Relationship between Physical Pain and Thoughts of Suicide: Results from Two Smartphone-Based Real-Time Monitoring Samples. Cogn Ther Res (2024). https://doi.org/10.1007/s10608-024-10472-2
Accepted:
Published:
DOI: https://doi.org/10.1007/s10608-024-10472-2