Abstract
Purpose
To evaluate the effect of single-dose intravenous dexamethasone on atrial fibrillation (AF) recurrence following radiofrequency catheter ablation.
Methods
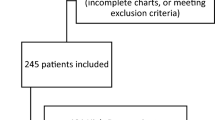
A cohort of 84 adult patients (> 18 years) underwent catheter ablation at Mayo Clinic Rochester from January to March 2019. Only first-time ablation patients were included, with all re-do ablations excluded to minimize heterogeneity. Administration of intraoperative dexamethasone 4 mg or 8 mg was determined by chart review from the procedure. At our institution, intraoperative intravenous steroids are administered for postoperative nausea and vomiting (PONV) prophylaxis at the discretion of the anesthesiologist. AF recurrence was determined by ECG or cardiac monitoring within 3 months or between 3 and 12 months post-ablation with an in-person follow-up visit.
Results
A total of 31 (36.9%) patients received intravenous dexamethasone compared to 54 (63.1%) who did not (approximating a 2:1 comparison group). The incidence of documented AF or atrial flutter, lasting greater than 30 s, within the first 3 months post-ablation was 29.0% in the dexamethasone group versus 24.5% in the non-dexamethasone group (p value 0.80). AF or atrial flutter recurrence at 3–12 months post-ablation was 3.2% in the dexamethasone group compared to 9.4% in the non-dexamethasone group (p value 0.41).
Conclusion
These data suggest that intraoperative intravenous dexamethasone administered during AF ablation for postoperative nausea and vomiting prophylaxis may not have a significant effect on AF recurrence rates.

Similar content being viewed by others
Availability of Data and Material
Not applicable.
Code Availability
Not applicable.
We the authors have disclosed all potential conflicts of interest. Our research does involve human participants who have consented to have their medical data used for research purposes. Our research does not involve animal subjects.
References
Lim HS, Schultz C, Dang J, et al. Time course of inflammation, myocardial injury, and prothrombotic response after radiofrequency catheter ablation for atrial fibrillation. Circ Arrhythm Electrophysiol. 2014;7(1):83–9.
McCabe JM, Smith LM, Tseng ZH, et al. Protracted CRP elevation after atrial fibrillation ablation. Pacing Clin Electrophysiol. 2008;31(9):1146–51.
Deftereos S, Giannopoulos G, Kossyvakis C, et al. Colchicine for prevention of early atrial fibrillation recurrence after pulmonary vein isolation: a randomized controlled study. J Am Coll Cardiol. 2012;60(18):1790–6.
Deftereos S, Giannopoulos G, Efremidis M, et al. Colchicine for prevention of atrial fibrillation recurrence after pulmonary vein isolation: mid-term efficacy and effect on quality of life. Heart Rhythm. 2014;11(4):620–8.
Kim YR, Nam GB, Han S, et al. Effect of short-term steroid therapy on early recurrence during the blanking period after catheter ablation of atrial fibrillation. Circ Arrhythm Electrophysiol. 2015;8(6):1366–72.
De Oliveira GS, Castro-Alves LJ, Ahmad S, Kendall MC, McCarthy RJ. Dexamethasone to prevent postoperative nausea and vomiting: an updated meta-analysis of randomized controlled trials. Anesth Analg. 2013;116(1):58–74.
Apfel CC, Korttila K, Abdalla M, et al. A factorial trial of six interventions for the prevention of postoperative nausea and vomiting. N Engl J Med. 2004;350(24):2441–51.
Weibel S, Rücker G, Eberhart LH et al (2020) Drugs for preventing postoperative nausea and vomiting in adults after general anaesthesia: a network meta-analysis. Cochrane Database Syst Rev. 10 19;10:CD012859
Won H, Kim JY, Shim J, et al. Effect of a single bolus injection of low-dose hydrocortisone for prevention of atrial fibrillation recurrence after radiofrequency catheter ablation. Circ J. 2013;77(1):53–9.
Kim DR, Won H, Uhm JS, et al. Comparison of two different doses of single bolus steroid injection to prevent atrial fibrillation recurrence after radiofrequency catheter ablation. Yonsei Med J. 2015;56(2):324–31.
Liu D, Ahmet A, Ward L, et al. A practical guide to the monitoring and management of the complications of systemic corticosteroid therapy. Allergy Asthma Clin Immunol. 2013;9(1):30.
Brunton LL, Knollmann BRC, Hilal-Dandan R (2018) Goodman & Gilman’s the pharmacological basis of therapeutics. Thirteenth edition. ed. McGraw Hill Medical; xiii, 1419 pages
Haines DE. The biophysics of radiofrequency catheter ablation in the heart: the importance of temperature monitoring. Pacing Clin Electrophysiol. 1993;16(3 Pt 2):586–91.
Nascimento T, Mota F, dos Santos LF, et al. Impact of prophylactic corticosteroids on systemic inflammation after extensive atrial ablation in pigs. Europace. 2012;14(1):138–45.
Lellouche N, Sacher F, Wright M, et al. Usefulness of C-reactive protein in predicting early and late recurrences after atrial fibrillation ablation. Europace. 2009;11(5):662–4.
Acknowledgements
All participating parties have been adequately acknowledged.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Drs. Kolade M. Agboola, Michael Dietrich, Roshan Karki, and Christopher V. DeSimone. The first draft of the manuscript was written by Dr. Kolade M. Agboola and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
Appropriate IRB approval was obtained for conducting this study.
Consent for Publication
Each patient provided generalized consent to participate in the research, which encompasses publication in an academic journal.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Agboola, K.M., Dietrich, M., Karki, R. et al. Single-Dose Intraprocedural Steroid Administration Does Not Impact Early Atrial Fibrillation Recurrence. Cardiovasc Drugs Ther 37, 151–157 (2023). https://doi.org/10.1007/s10557-021-07271-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10557-021-07271-2