Abstract
Background
Oncology settings increasingly use patient experience data to evaluate clinical performance. Given that older patients with hematologic malignancies are a high-risk population, this study examined factors associated with patient-reported health care experiences during the first year of their cancer diagnosis.
Methods
Cross-sectional study using the 2000–2015 SEER-CAHPS® data to examine patient experiences of Medicare enrollees with a primary diagnosis of leukemia or lymphoma. The primary outcomes were three CAHPS assessments: overall care, personal doctor, and health plan overall. We estimated case-mix adjusted and fully adjusted associations between factors (i.e., clinical and sociodemographic) and the CAHPS outcomes using bivariate statistical tests and multiple linear regression.
Results
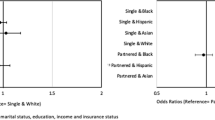
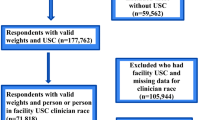
The final sample included 1,151 patients, with 431 diagnosed with leukemia and 720 diagnosed with lymphoma (median time from diagnosis to survey 6 months). Patients who completed the survey further apart from the diagnosis date reported significantly higher adjusted ratings of care overall (β .39, p = .008) than those closer to diagnosis. American Indian/Alaska Native, Asian, and Pacific Islander patients had lower adjusted ratings of care overall (β − .73, p = .003) than Non-Hispanic white patients. Multimorbidity was significantly associated with higher adjusted personal doctor ratings (β .26, p = .003).
Conclusions
Unfavorable patient experiences among older adults diagnosed with hematologic malignancies warrant targeted efforts to measure and improve care quality. Future measurement of experiences of cancer care soon after diagnosis, coupled with careful sampling of high-priority populations, will inform oncology leaders and clinicians on strategies to improve care for high-risk, high-cost populations.


Similar content being viewed by others
References
Leukemia and Lymphoma Society (2019) Facts and statistics, general blood cancers. https://www.lls.org/facts-and-statistics/facts-and-statistics-overview/facts-and-statistics. Accessed 1 Feb 2020
Rathnasabapathy R, Lancet JE (2003) Management of acute myelogenous leukemia in the elderly. Cancer Control 10(6):469–477. https://doi.org/10.1177/107327480301000605
Habermann TM, Weller EA, Morrison VA et al (2006) Rituximab-CHOP versus CHOP alone or with maintenance rituximab in older patients with diffuse large B-cell lymphoma. J Clin Oncol 24(19):3121–3127. https://doi.org/10.1200/JCO.2005.05.1003
American Cancer Society (2017) External beam radiation therapy. https://www.cancer.org/treatment/treatments-and-side-effects/treatment-types/radiation/external-beam-radiation-therapy.html. Accessed 25 Mar 2019
Wagner EH, Aiello Bowles EJ, Greene SM et al (2010) The quality of cancer patient experience: perspectives of patients, family members, providers and experts. BMJ Qual Saf 19(6):484–489. https://doi.org/10.1136/qshc.2010.042374
Crawford R, Sully K, Conroy R et al (2020) Patient-centered insights on treatment decision making and living with acute myeloid leukemia and other hematologic cancers. Patient 13(1):83–102. https://doi.org/10.1007/s40271-019-00384-9
Abel GA, Klepin HD (2018) Frailty and the management of hematologic malignancies. Blood 131(5):515–524. https://doi.org/10.1182/blood-2017-09-746420
Mollica MA (2017) Patient experiences of cancer care: scoping review, future directions, and introduction of a new data resource: surveillance epidemiology and end results-consumer assessment of healthcare providers and systems (SEER-CAHPS). Patient Exp J 4(1):103–121
Agarwal AK, Hahn L, Merchant RM, Rosin R (2019) Handcrafting the patient experience. NEJM Catal. https://doi.org/10.1056/CAT.19.0618
Blayney DW, Simon MK, Podtschaske B et al (2018) Critical lessons from high-value oncology practices. JAMA Oncol 4(2):164. https://doi.org/10.1001/jamaoncol.2017.3803
Howell DA, Smith AG, Jack A et al (2013) Time-to-diagnosis and symptoms of myeloma, lymphomas and leukaemias: a report from the haematological malignancy research network. BMC Hematol 13(1):9. https://doi.org/10.1186/2052-1839-13-9
Howell DA, Hart RI, Smith AG, Macleod U, Patmore R, Roman E (2019) Disease-related factors affecting timely lymphoma diagnosis: a qualitative study exploring patient experiences. Br J Gen Pract 69(679):e134–e145. https://doi.org/10.3399/bjgp19X701009
Gee GC, Ford CL (2011) Structural racism and health inequities. Du Bois Rev 8(1):115–132. https://doi.org/10.1017/S1742058X11000130
Boyd R, Lindo E, Weeks L, McLemore M (2020) On racism: a new standard for publishing on racial health inequities. Health Aff Blog. https://doi.org/10.1377/hblog20200630.939347
Hardeman RR, Karbeah J (2020) Examining racism in health services research: a disciplinary self-critique. Health Serv Res 55(S2):777–780. https://doi.org/10.1111/1475-6773.13558
Chawla N, Urato M, Ambs A et al (2015) Unveiling SEER-CAHPS®: a new data resource for quality of care research. J Gen Intern Med 30(5):641–650. https://doi.org/10.1007/s11606-014-3162-9
National Cancer Institute (2020) About the SEER program. SEER. https://seer.cancer.gov/about/overview.html. Accessed 20 Jan 2020
Andersen RM (1995) Revisiting the behavioral model and access to medical care: does it matter? J Health Soc Behav 36(1):1. https://doi.org/10.2307/2137284
Centers for Medicare & Medicaid Services. (2019) Consumer assessment of healthcare providers & systems (CAHPS). https://www.cms.gov/Research-Statistics-Data-and-Systems/Research/CAHPS. Accessed 30 Jan 2020
SEER-CAHPS® (2018) National Cancer Institute. https://healthcaredelivery.cancer.gov/seer-cahps/overview/description.html. Accessed 11 Dec 2018
Morales LS, Elliott MN, Weech-Maldonado R, Hays RD (2001) Differences in CAHPS® adult survey reports and ratings by race and ethnicity: an analysis of the national CAHPS® benchmarking data 1.0. Health Serv Res 36(3):595–617
Paddison CAM, Elliott MN, Haviland AM et al (2013) Experiences of care among medicare beneficiaries with ESRD: medicare consumer assessment of healthcare providers and systems (CAHPS) survey results. Am J Kidney Dis 61(3):440–449. https://doi.org/10.1053/j.ajkd.2012.10.009
Quigley DD, Elliott MN, Setodji CM, Hays RD (2018) Quantifying magnitude of group-level differences in patient experiences with health care. Health Serv Res 53:3027–3051. https://doi.org/10.1111/1475-6773.12828
Ayanian JZ, Zaslavsky AM, Arora NK et al (2010) Patients’ experiences with care for lung cancer and colorectal cancer: findings from the cancer care outcomes research and surveillance consortium. J Clin Oncol 28(27):4154–4161. https://doi.org/10.1200/JCO.2009.27.3268
Survey Instruments and Specifications (2020) Medicare advantage and prescription drug plan CAHPS survey. https://ma-pdpcahps.org/en/survey-instruments-and-specifications/. Accessed 22 Apr 2020
National Cancer Institute (2019) Site recode ICD-O-3. Surveillance, epidemiology, and end results program. https://seer.cancer.gov/siterecode/index.html. Accessed 25 Feb 2019
Sterne JAC, White IR, Carlin JB et al (2009) Multiple imputation for missing data in epidemiological and clinical research: potential and pitfalls. BMJ 338:b2393–b2393. https://doi.org/10.1136/bmj.b2393
Saunders CL, Abel GA, Lyratzopoulos G (2015) Inequalities in reported cancer patient experience by socio-demographic characteristic and cancer site: evidence from respondents to the English Cancer Patient Experience Survey. Eur J Cancer Care (Engl) 24(1):85–98. https://doi.org/10.1111/ecc.12267
National Cancer Institute (2020) Case-mix adjustment guidance for SEER-CAHPS analyses. https://healthcaredelivery.cancer.gov/seer-cahps/researchers/adjustment_guidance.html. Accessed 20 Jan 2020
Elliott MN, Haviland AM, Orr N, Hambarsoomian K, Cleary PD (2011) How do the experiences of medicare beneficiary subgroups differ between managed care and original medicare?: Experiences of medicare beneficiary subgroups. Health Serv Res 46(4):1039–1058. https://doi.org/10.1111/j.1475-6773.2011.01245.x
Lines LM, Cohen J, Halpern MT, Smith AW, Kent EE (2019) Care experiences among dually enrolled older adults with cancer: SEER-CAHPS, 2005–2013. Cancer Causes Control 30(10):1137–1144. https://doi.org/10.1007/s10552-019-01218-7
Anhang Price R, Elliott MN, Zaslavsky AM et al (2014) Examining the role of patient experience surveys in measuring health care quality. Med Care Res Rev 71(5):522–554. https://doi.org/10.1177/1077558714541480
Systemic Therapy (2018) Cancer Treatments, Moffit Cancer Center. https://www.moffitt.org/treatments/systemic-therapy/. Accessed 30 Nov 2018
Almeida AM, Ramos F (2016) Acute myeloid leukemia in the older adults. Leuk Res Rep 6:1–7. https://doi.org/10.1016/j.lrr.2016.06.001
Gobbi PG, Broglia C, Di Giulio G et al (2004) The clinical value of tumor burden at diagnosis in Hodgkin lymphoma. Cancer 101(8):1824–1834. https://doi.org/10.1002/cncr.20568
Abel GA, Saunders CL, Lyratzopoulos G (2016) Post-sampling mortality and non-response patterns in the English Cancer Patient Experience Survey: Implications for epidemiological studies based on surveys of cancer patients. Cancer Epidemiol 41:34–41. https://doi.org/10.1016/j.canep.2015.12.010
Nabulsi NA, Alobaidi A, Talon B et al (2020) Self-reported health and survival in older patients diagnosed with multiple myeloma. Cancer Causes Control 31(7):641–650. https://doi.org/10.1007/s10552-020-01305-0
Mollica MA, Weaver KE, McNeel TS, Kent EE (2018) Examining urban and rural differences in perceived timeliness of care among cancer patients: A SEER-CAHPS study: patient experiences: urban vs rural. Cancer 124(15):3257–3265. https://doi.org/10.1002/cncr.31541
Abel GA, Friese CR, Magazu LS et al (2008) Delays in referral and diagnosis for chronic hematologic malignancies: a literature review. Leuk Lymphoma 49(7):1352–1359. https://doi.org/10.1080/10428190802124281
Friese CR, Abel GA, Magazu LS, Neville BA, Richardson LC, Earle CC (2009) Diagnostic delay and complications for older adults with multiple myeloma. Leuk Lymphoma 50(3):392–400. https://doi.org/10.1080/10428190902741471
Mohile SG, Dale W, Somerfield MR et al (2018) Practical assessment and management of vulnerabilities in older patients receiving chemotherapy: ASCO guideline for geriatric oncology. JCO 36(22):2326–2347. https://doi.org/10.1200/JCO.2018.78.8687
Aldoss I, Forman SJ, Pullarkat V (2019) Acute lymphoblastic leukemia in the older adult. JOP 15(2):67–75. https://doi.org/10.1200/JOP.18.00271
Elliott MN, Edwards C, Angeles J, Hambarsoomians K, Hays RD (2005) Patterns of unit and item nonresponse in the CAHPS® hospital survey: unit and item nonresponse. Health Serv Res 40(6p2):2096–2119. https://doi.org/10.1111/j.1475-6773.2005.00476.x
Elliott MN, Haviland AM, Kanouse DE, Hambarsoomian K, Hays RD (2009) Adjusting for subgroup differences in extreme response tendency in ratings of health care: impact on disparity estimates. Health Serv Res 44(2p1):542–561. https://doi.org/10.1111/j.1475-6773.2008.00922.x
Halpern MT, Urato MP, Kent EE (2017) The health care experience of patients with cancer during the last year of life: analysis of the SEER-CAHPS data set: health care ratings in last year of Life. Cancer 123(2):336–344. https://doi.org/10.1002/cncr.30319
Farias AJ, Ochoa CY, Toledo G, Bang S-I, Hamilton AS, Du XL (2020) Racial/ethnic differences in patient experiences with health care in association with earlier stage at breast cancer diagnosis: findings from the SEER-CAHPS data. Cancer Causes Control 31(1):13–23. https://doi.org/10.1007/s10552-019-01254-3
Moorley C, Darbyshire P, Serrant L, Mohamed J, Ali P, Souza RD (2020) Dismantling structural racism: nursing must not be caught on the wrong side of history. J Adv Nurs 76(10):2450–2453. https://doi.org/10.1111/jan.14469
Evans MK, Rosenbaum L, Malina D, Morrissey S, Rubin EJ (2020) Diagnosing and treating systemic racism. N Engl J Med 383(3):274–276. https://doi.org/10.1056/NEJMe2021693
Simonds VW, Wallerstein N, Duran B, Villegas M (2013) Community-based participatory research: its role in future cancer research and public health practice. Prev Chronic Dis. https://doi.org/10.5888/pcd10.120205
Sacks GD, Lawson EH, Dawes AJ et al (2015) Relationship between hospital performance on a patient satisfaction survey and surgical quality. JAMA Surg 150(9):858. https://doi.org/10.1001/jamasurg.2015.1108
Evensen CT, Yost KJ, Keller S et al (2019) Development and testing of the CAHPS cancer care survey. JOP. https://doi.org/10.1200/JOP.19.00039
CAHPS Surveys and Guidance (2018) agency for healthcare research and quality, Rockville, MD. https://www.ahrq.gov/cahps/surveys-guidance/index.html. Accessed 30 Nov 2018
Pew Research Center (2019) Collecting survey data. Pew research center methods. https://www.pewresearch.org/methods/u-s-survey-research/collecting-survey-data/. Accessed 27 Mar 2019
Acknowledgments
The content was solely the responsibility of the authors and does not represent the official views of the American Cancer Society or the United States Department of Health and Human Services. We are grateful for Dr. Michelle Mollica and team at the SEER-CAHPS program at the National Cancer Institute.
Funding
Supported in part by the American Cancer Society Doctoral Degree Scholarship in Cancer Nursing (33507-DSCN-19-048-01-SCN), Hillman Scholars Program in Nursing Innovation, and the Jonas Nurse Scholars Program. Dr. Friese is supported by The University of Michigan Rogel Cancer Center (P30-CA-046592).
Author information
Authors and Affiliations
Contributions
AF and CRF performed conceptualization, funding acquisition, data curation, supervision, validation, and visualization. All authors involved in formal analysis, investigation, methodology, project administration, resources, software, writing of the original draft, review, and editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fauer, A., Choi, S.W., Wallner, L.P. et al. Understanding quality and equity: patient experiences with care in older adults diagnosed with hematologic malignancies. Cancer Causes Control 32, 379–389 (2021). https://doi.org/10.1007/s10552-021-01395-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-021-01395-4