Abstract
Objectives
Cervical cancer is the most common malignancy among Nepalese women. Rational prevention measures are informed by epidemiological data on human papillomavirus (HPV) prevalence.
Methods
Cervical specimens were obtained from 932 married women aged 15–59 years from the general population of Bharatpur, Nepal, as well as from 61 locally diagnosed invasive cervical cancers (ICC). HPV was detected using a GP5+/6+ PCR-based assay.
Results
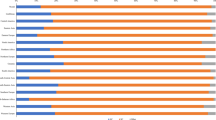
Among the general population, the overall prevalence of HPV was 8.6% (6.1% for high-risk types). Prevalence of abnormal Pap smears was 3.6%, including five high-grade squamous intraepithelial lesions. Residence in slum housing, lower education level, ≥3 sexual partners in a woman's lifetime, and husband’s extramarital affairs were significantly associated with HPV positivity. HPV prevalence was relatively constant across all age groups. HPV16 was the most common type, both among the general population (1.9%) and among 54 women with HPV-positive ICC (68.5%). HPV18 (22.2%) and 45 (5.6%) were also common in ICC.
Conclusions
Nepal has an intermediate burden of HPV infection, lower than many areas in India and China. Approximately 80% of cervical cancer in Nepal is theoretically preventable by HPV16/18 vaccines. In the meantime, screen-and-treat approaches should be encouraged to overcome difficulties that were encountered to recall women with screening-positive findings.

Similar content being viewed by others
Abbreviations
- CI:
-
Confidence interval
- HSIL:
-
High-grade squamous intraepithelial lesions
- HPV:
-
Human papillomavirus
- HPV16/18:
-
HPV16 and/or 18
- IARC:
-
International Agency for Research on Cancer
- ICC:
-
Invasive cervical cancer
- OR:
-
Odds ratio
References
United Nations Educational Scientific and Cultural Organization (2006) EFA Global Monitoring Report. Available from URL: http://gmr.uis.unesco.org/selectindicators.aspx
The World Bank Group (2006) 2006 World Development Indicators. Table 2.7: Poverty. Available from URL: http://devdata.worldbank.org/wdi2006/contents/Section2.htm
World Health Organization (2006) The world health report 2006: working together for health. World Health Organization, Geneva
B.P. Koirala Memorial Cancer Hospital (Nepal) (2004) Annual report 2003. B.P. Koirala Memorial Cancer Hospital, Chitawan
Maucort-Boulch D, Franceschi S, Plummer M (2008) International correlation between human papillomavirus prevalence and cervical cancer incidence. Cancer Epidemiol Biomarkers Prev 17:717–720
Kahn JA, Burk RD (2007) Papillomavirus vaccines in perspective. Lancet 369:2135–2137
Qiao YL, Sellors JW, Eder PS et al (2008) A new HPV-DNA test for cervical-cancer screening in developing regions: a cross-sectional study of clinical accuracy in rural China. Lancet Oncol 9:929–936
Sankaranarayanan R, Nene BM, Shastri SS et al (2009) HPV screening for cervical cancer in rural India. N Engl J Med 360:1385–1394
Clifford GM, Gallus S, Herrero R et al (2005) Worldwide distribution of human papillomavirus types in cytologically normal women in the International Agency for Research on Cancer HPV prevalence surveys: a pooled analysis. Lancet 366:991–998
Roda Husman AM, Snijders PJ, Stel HV, van den Brule AJ, Meijer CJ, Walboomers JM (1995) Processing of long-stored archival cervical smears for human papillomavirus detection by the polymerase chain reaction. Br J Cancer 72:412–417
Jacobs MV, Walboomers JM, Snijders PJ et al (2000) Distribution of 37 mucosotropic HPV types in women with cytologically normal cervical smears: the age-related patterns for high-risk and low-risk types. Int J Cancer 87:221–227
van den Brule AJ, Pol R, Fransen-Daalmeijer N, Schouls LM, Meijer CJ, Snijders PJ (2002) GP5+/6+ PCR followed by reverse line blot analysis enables rapid and high-throughput identification of human papillomavirus genotypes. J Clin Microbiol 40:779–787
Muñoz N, Bosch FX, de Sanjosé S et al (2003) Epidemiologic classification of human papillomavirus types associated with cervical cancer. N Engl J Med 348:518–527
Doll R, Payne P, Waterhouse J (1966) Cancer incidence in five continents: a technical report. Springer-Verlag (for UICC), Berlin
Franceschi S, Rajkumar R, Snijders PJF et al (2005) Papillomavirus infection in rural women in southern India. Br J Cancer 92:601–606
Dai M, Bao YP, Li N et al (2006) Human papillomavirus infection in Shanxi Province, People’s Republic of China: a population-based study. Br J Cancer 95:96–101
Li LK, Dai M, Clifford GM et al (2006) Human papillomavirus infection in Shenyang City, People’s Republic of China: a population-based study. Br J Cancer 95:1593–1597
Wu RF, Dai M, Qiao YL et al (2007) Human papillomavirus infection in women in Shenzhen City, People’s Republic of China, a population typical of recent Chinese urbanisation. Int J Cancer 121:1306–1311
Dondog B, Clifford GM, Vaccarella S et al (2008) Human papillomavirus infection in Ulaanbaatar, Mongolia: a population-based study. Cancer Epidemiol Biomarkers Prev 17:1731–1738
Keita N, Clifford GM, Koulibaly M et al (2009) HPV infection in women with and without cervical cancer in Conakry, Guinea. Br J Cancer 101:865–870
Anh PT, Hieu NT, Herrero R et al (2003) Human papillomavirus infection among women in South and North Vietnam. Int J Cancer 104:213–220
Sukvirach S, Smith JS, Tunsakul S et al (2003) Population-based human papillomavirus prevalence in Lampang and Songkla, Thailand. J Infect Dis 187:1246–1256
De Vuyst H, Clifford GM, Li N, Franceschi S (2009) HPV infection in Europe. Eur J Cancer 45:2632–2639
Thomas JO, Herrero R, Omigbodun AA et al (2004) Prevalence of papillomavirus infection in women in Ibadan, Nigeria: a population-based study. Br J Cancer 90:638–645
Franceschi S, Herrero R, Clifford GM et al (2006) Variations in the age-specific curves of human papillomavirus prevalence in women worldwide. Int J Cancer 119:2677–2684
Castle PE, Schiffman M, Herrero R et al (2005) A prospective study of age trends in cervical human papillomavirus acquisition and persistence in Guanacaste, Costa Rica. J Infect Dis 191:1808–1816
Khan MJ, Castle PE, Lorincz AT et al (2005) The elevated 10-year risk of cervical precancer and cancer in women with human papillomavirus (HPV) type 16 or 18 and the possible utility of type-specific HPV testing in clinical practice. J Natl Cancer Inst 97:1072–1079
Vaccarella S, Franceschi S, Herrero R et al (2006) Sexual behavior, condom use and HPV: pooled analysis of the International Agency for Research on Cancer HPV Prevalence Surveys. Cancer Epidemiol Biomarkers Prev 15:326–333
Bardin A, Vaccarella S, Clifford GM et al (2008) Human papillomavirus infection in women with and without cervical cancer in Warsaw, Poland. Eur J Cancer 44:557–564
Smith JS, Lindsay L, Hoots B et al (2007) Human papillomavirus type distribution in invasive cervical cancer and high-grade cervical lesions: a meta-analysis update. Int J Cancer 121:621–632
Agurto I, Arrossi S, White S et al (2005) Involving the community in cervical cancer prevention programs. Int J Gynaecol Obstet 89(Suppl 2):S38–S45
Murillo R, Almonte M, Pereira A et al (2008) Cervical cancer screening programs in Latin America and the Caribbean. Vaccine 26(Suppl 11):L37–L48
Garland SM, Cuzick J, Domingo EJ et al (2008) Recommendations for cervical cancer prevention in Asia Pacific. Vaccine 26(Suppl 12):M89–M98
Acknowledgments
The authors of the manuscript have no conflict of interest to declare. The authors thank Dr Johanne Sundby for valuable comments.
Financial support
This work was supported by the Bill & Melinda Gates Foundation (grant number 35537).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sherpa, A.T.L., Clifford, G.M., Vaccarella, S. et al. Human papillomavirus infection in women with and without cervical cancer in Nepal. Cancer Causes Control 21, 323–330 (2010). https://doi.org/10.1007/s10552-009-9467-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-009-9467-z