Abstract
Purpose
To compare the sonographic findings between pediatric patients with/without mediastinitis after cardiovascular surgery.
Methods
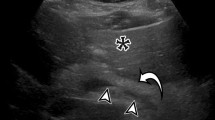
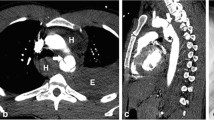
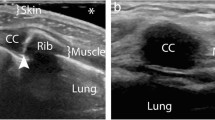
We included 18 pediatric patients with suspected mediastinitis after cardiovascular surgery who underwent ultrasound. They were divided into two groups according to the presence of mediastinitis, confirmed by positive bacterial culture from the mediastinum (number with/without mediastinitis = 5/13). The following sonographic findings were compared between the groups: (1) increased parasternal fat echogenicity and (2) retrosternal mediastinal fluid collection. Additionally, sex, age, and the interval between surgery and ultrasound examination were also compared. Fisher’s exact and Mann–Whitney U tests were used for statistical comparisons.
Results
A significant difference was observed between patients with and without mediastinitis in the presence of increased fat echogenicity around the sternum (present/absent with mediastinitis vs. present/absent without mediastinitis: 5/0 vs. 3/10, respectively; P = 0.007) and retrosternal mediastinal fluid collection (5/0 vs. 2/11, respectively; P = 0.002). There was no significant difference in sex (male/female; 3/2 vs. 6/7; P > 0.999); age (months; 12.6 ± 9.4 (range, 1–22) vs. 6.9 ± 5.4 (range, 1–21); P = 0.336); and interval between surgery and ultrasound examination (days; 12.8 ± 7.2 (range, 6–20) vs. 19.1 ± 14.9 (range, 1–45); P = 0.443).
Conclusion
Although our cohort was small, none of the patients without increased parasternal fat echogenicity or mediastinal fluid collection was diagnosed with mediastinitis. These sonographic findings may help identify the possible presence of mediastinitis. Ultrasound may be the modality of first choice to evaluate pediatric patients for mediastinitis after cardiovascular surgery.





Similar content being viewed by others
References
Long CB, Shah SS, Lautenbach E, et al. Postoperative mediastinitis in children: epidemiology, microbiology and risk factors for Gram-negative pathogens. Pediatr Infect Dis J. 2005;24:315–9.
Kagen J, Lautenbach E, Bilker WB, et al. Risk factors for mediastinitis following median sternotomy in children. Pediatr Infect Dis J. 2007;26:613–8.
Abu-Omar Y, Kocher GJ, Bosco P, et al. European Association for Cardio-Thoracic Surgery expert consensus statement on the prevention and management of mediastinitis. Eur J Cardiothorac Surg. 2017;51:10–29.
Nateghian A, Taylor G, Robinson JL. Risk factors for surgical site infections following open-heart surgery in a Canadian pediatric population. Am J Infect Control. 2004;32:397–401.
Jolles H, Henry DA, Roberson JP, et al. Mediastinitis following median sternotomy: CT findings. Radiology. 1996;201:463–6.
Yamashiro T, Kamiya H, Murayama S, et al. Infectious mediastinitis after cardiovascular surgery: role of computed tomography. Radiat Med. 2008;26:343–7.
Carrol CL, Jeffrey RB Jr, Federle MP, et al. CT evaluation of mediastinal infections. J Comput Assist Tomogr. 1987;11:449–54.
Yamaguchi H, Yamauchi H, Yamada T, et al. Diagnostic validity of computed tomography for mediastinitis after cardiac surgery. Ann Thorac Cardiovasc Surg. 2001;7:94–8.
Tortoriello TA, Friedman JD, McKenzie ED, et al. Mediastinitis after pediatric cardiac surgery: a 15-year experience at a single institution. Ann Thorac Surg. 2003;76:1655–60.
Laussen PC. Neonates with congenital heart disease. Curr Opin Pediatr. 2001;13:220–6.
Reddy VM. Low birth weight and very low birth weight neonates with congenital heart disease: timing of surgery, reasons for delaying or not delaying surgery. Semin Thorac Cardiovasc Surg Pediatr Card Surg Annu. 2013;16:13–20.
Wernovsky G, Ghanayem N, Ohye RG, et al. Hypoplastic left heart syndrome: consensus and controversies in 2007. Cardiol Young. 2007;17(Suppl 2):75–86.
Pena E, Fontan L, Blanco M. Superior vena cava syndrome and collateral circulation in the abdominal wall by a fibrosing mediastinitis. Med Clin (Barc). 2012;139:e9.
Foldyna B, Mueller M, Etz CD, et al. Computed tomography improves the differentiation of infectious mediastinitis from normal postoperative changes after sternotomy in cardiac surgery. Eur Radiol. 2019;29:2949–57.
Exarhos DN, Malagari K, Tsatalou EG, et al. Acute mediastinitis: spectrum of computed tomography findings. Eur Radiol. 2005;15:1569–74.
Maddern IR, Goodman LR, Almassi GH, et al. CT after reconstructive repair of the sternum and chest wall. Radiology. 1993;186:665–70.
Helenon O, Folinais D, Cornud F, et al. X-ray computed tomography in the course of mediastinitis after sternostomy for heart surgery. J Radiol. 1987;68:237–45.
Jump C, Anupindi S, Peranteau W, et al. Extensive thoracic injury from button battery ingestion. J Pediatr Gastroenterol Nutr. 2016;62:e24.
David RA, Weiner MA, Rakow JI. Chronic active mediastinitis in a 7-year-old boy: MRI findings. Pediatr Radiol. 1996;26:669–71.
Hosokawa T, Yamada Y, Hsokawa M, et al. Ultrasound imaging of the anorectal malformation during the neonatal period: a comprehensive review. Jpn J Radiol. 2018;36:581–91.
Hosokawa T, Yamada Y, Takahashi H, et al. Postnatal ultrasound to determine the surgical strategy for congenital diaphragmatic hernia. J Ultrasound Med. 2019;38:2347–58.
Hosokawa T, Suzuki S, Tanami Y, et al. Ultrasound evaluation of complications after cardiovascular surgery in pediatric patients: a case series. Med Ultrason. 2020;22:108–13.
Hosokawa T, Yamada Y, Tanami Y, et al. Associations between sonographic findings and operative time of transumbilical laparoscopic-assisted appendectomy for acute appendicitis in children. AJR Am J Roentgenol. 2019;11:1–9.
Lee MW, Kim YJ, Jeon HJ, et al. Sonography of acute right lower quadrant pain: importance of increased intraabdominal fat echo. Am J Roentgenol. 2009;192:174–9.
Hosokawa T, Yamada Y, Tanami Y, et al. Computed tomography findings of mediastinitis after cardiovascular surgery. Pediatr Int. 2020;62:206–13.
Shkolnik B, Judson MA, Austin A, et al. Diagnostic accuracy of thoracic ultrasonography to differentiate transudative from exudative pleural effusion. Chest. 2020. https://doi.org/10.1016/j.chest.2020.02.051.
Hosokawa T, Hosokawa M, Tanami Y, et al. Use of ultrasound findings to predict bowel ischemic changes in pediatric patients with intestinal volvulus. J Ultrasound Med. 2020;39:683–92.
Ouedraogo S, Kambire JL, Ouedraogo S, et al. Surgical site infection after digestive surgery: diagnosis and treatment in a context of limited resources. Surg Infect (Larchmt). 2020. https://doi.org/10.1089/sur.2019.007.
Kay HR, Goodman LR, Teplick SK, et al. Use of computed tomography to assess mediastinal complications after median sternotomy. Ann Thorac Surg. 1983;36:706–14.
Goodman LR, Kay HR, Teplick SK, et al. Complications of median sternotomy: computed tomographic evaluation. Am J Roentgenol. 1983;141:225–30.
Hehrlein FW, Herrmann H, Kraus J. Complications of median sternotomy in cardiovascular surgery. J Cardiovasc Surg (Torino). 1972;13:390–3.
Chiu TC, Chou YH, Tiu CM, et al. Right-sided colonic diverticulitis: clinical features, sonographic appearances, and management. J Med Ultrasound. 2017;25:33–9.
Tan MZ, Whitgift J, Warren H. Mediastinitis, pseudo-aneurysm formation, aortic bleed, and death from endoscopic botulinum toxin injection. Endoscopy. 2016;48(Suppl 1):E186–E187187.
Hosokawa T, Tanami Y, Sato Y, et al. Comparison of imaging findings between acute focal bacterial nephritis (acute lobar nephronia) and acute pyelonephritis: a preliminary evaluation of the sufficiency of ultrasound for the diagnosis of acute focal bacterial nephritis. Emerg Radiol. 2020. https://doi.org/10.1007/s10140-020-01771-8.
Tewarie L, Moza AK, Khattab MA, et al. Effective combination of different surgical strategies for deep sternal wound infection and mediastinitis. Ann Thorac Cardiovasc Surg. 2019;25:102–10.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
TH, YT, YS, YK, KN, and EO declare that they have no financial or personal relationships that could lead to a conflict of interest.
Research involving human subjects
This research was performed in accordance with the tenets of the Declaration of Helsinki.
Informed consent
This retrospective study was approved by the ethics committee of our institution, and informed consent was waived.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Hosokawa, T., Tanami, Y., Sato, Y. et al. Comparison of sonographic findings between pediatric patients with mediastinitis and without mediastinitis after cardiovascular surgery. J Med Ultrasonics 47, 625–633 (2020). https://doi.org/10.1007/s10396-020-01029-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10396-020-01029-3