Abstract
Background
Obstructive sleep apnea (OSA) is known to be associated with metabolic dysregulation and incident cardiovascular diseases. However, its association with end-stage renal disease (ESRD) has not been clarified. This study aimed to evaluate longitudinally whether OSA is an independent risk factor for ESRD.
Methods
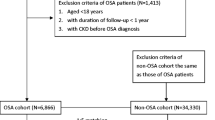
This retrospective nationwide population-based cohort study included data on 67,359 patients with OSA and 336,795 age-, sex- and years of the enrollment-matched controls without OSA obtained from the Korean National Health Insurance Service database from 2009 to 2014. The study population was followed up from baseline to the date of ESRD diagnosis or until 2016. A Cox proportional-hazards model with multivariable adjustment was used to evaluate the association between OSA and incident ESRD.
Results
A significantly higher incident ESRD risk (adjusted hazard ratio: 1.29, 95% confidence interval 1.02–1.62) was observed for patients older than 40 years with OSA than for matched controls, when adjusted for age, sex, income status, smoking, alcohol consumption, body mass index, diabetes, hypertension, dyslipidemia, estimated glomerular filtration rate, and proteinuria. The OSA group remained predictive of higher risk of ESRD incidence in subgroups of age ≥ 65 years, female sex, hypertension, dyslipidemia, proteinuria, and chronic kidney disease.
Conclusion
OSA was associated with a higher risk of incident ESRD. Understanding the association between OSA and ESRD might provide further insights to establish national health care policy.


Similar content being viewed by others
References
Lin CH, Perger E, Lyons OD. Obstructive sleep apnea and chronic kidney disease. Curr Opin Pulmon Med. 2018;24(6):549–54. https://doi.org/10.1097/MCP.0000000000000525.
Mohsenin V. Obstructive sleep apnea and hypertension: a critical review. Curr Hypertens Rep. 2014;16(10):482. https://doi.org/10.1007/s11906-014-0482-4.
Jordan AS, McSharry DG, Malhotra A. Adult obstructive sleep apnoea. Lancet. 2014;383(9918):736–47. https://doi.org/10.1016/S0140-6736(13)60734-5.
Pien GW, Schwab RJ. Sleep disorders during pregnancy. Sleep. 2004;27(7):1405–17.
Leung RS, Bradley TD. Sleep apnea and cardiovascular disease. Am J Respir Crit Care Med. 2001;164(12):2147–65. https://doi.org/10.1164/ajrccm.164.12.2107045.
Budhiraja R, Siddiqi TA, Quan SF. Sleep disorders in chronic obstructive pulmonary disease: etiology, impact, and management. J Clin Sleep Med. 2015;11(3):259–70. https://doi.org/10.5664/jcsm.4540.
Yaggi HK, Concato J, Kernan WN, Lichtman JH, Brass LM, Mohsenin V. Obstructive sleep apnea as a risk factor for stroke and death. N Engl J Med. 2005;353(19):2034–41. https://doi.org/10.1056/NEJMoa043104.
Nicholl DDM, Ahmed SB, Loewen AHS, Hemmelgarn BR, Sola DY, Beecroft JM, et al. Declining kidney function increases the prevalence of sleep apnea and nocturnal hypoxia. Chest. 2012;141(6):1422–30. https://doi.org/10.1378/chest.11-1809.
Lee YC, Hung SY, Wang HK, Lin CW, Wang HH, Chen SW, et al. Sleep apnea and the risk of chronic kidney disease: a nationwide population-based cohort study. Sleep. 2015;38(2):213–21. https://doi.org/10.5665/sleep.4400.
Kato K, Takata Y, Usui Y, Shiina K, Asano K, Hashimura Y, et al. Severe obstructive sleep apnea increases cystatin C in clinically latent renal dysfunction. Respir Med. 2011;105(4):643–9. https://doi.org/10.1016/j.rmed.2010.11.024.
Sakaguchi Y, Shoji T, Kawabata H, Niihata K, Suzuki A, Kaneko T, et al. High prevalence of obstructive sleep apnea and its association with renal function among nondialysis chronic kidney disease patients in Japan: a cross-sectional study. Clin J Am Soc Nephrol. 2011;6(5):995–1000. https://doi.org/10.2215/CJN.08670910.
Markou N, Kanakaki M, Myrianthefs P, Hadjiyanakos D, Vlassopoulos D, Damianos A, et al. Sleep-disordered breathing in nondialyzed patients with chronic renal failure. Lung. 2006;184(1):43–9. https://doi.org/10.1007/s00408-005-2563-2.
Drager LF, McEvoy RD, Barbe F, Lorenzi-Filho G, Redline S, Initiative I. Sleep apnea and cardiovascular disease: lessons from recent trials and need for team science. Circulation. 2017;136(19):1840–50. https://doi.org/10.1161/CIRCULATIONAHA.117.029400.
Song SO, Jung CH, Song YD, Park CY, Kwon HS, Cha BS, et al. Background and data configuration process of a nationwide population-based study using the Korean national health insurance system. Diabetes Metabol J. 2014;38(5):395–403. https://doi.org/10.4093/dmj.2014.38.5.395.
Lee SR, Choi EK, Rhee TM, Lee HJ, Lim WH, Kang SH, et al. Evaluation of the association between diabetic retinopathy and the incidence of atrial fibrillation: a nationwide population-based study. Int J Cardiol. 2016;223:953–7. https://doi.org/10.1016/j.ijcard.2016.08.296.
Yang HK, Han K, Kwon HS, Park YM, Cho JH, Yoon KH, et al. Obesity, metabolic health, and mortality in adults: a nationwide population-based study in Korea. Sci Rep. 2016;6:30329. https://doi.org/10.1038/srep30329.
Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF 3rd, Feldman HI, et al. A new equation to estimate glomerular filtration rate. Ann Internal Med. 2009;150(9):604–12.
Marshall NS, Wong KK, Phillips CL, Liu PY, Knuiman MW, Grunstein RR. Is sleep apnea an independent risk factor for prevalent and incident diabetes in the Busselton Health Study? J Clin Sleep Med. 2009;5(1):15–20.
Drager LF, Li J, Reinke C, Bevans-Fonti S, Jun JC, Polotsky VY. Intermittent hypoxia exacerbates metabolic effects of diet-induced obesity. Obesity (Silver Spring). 2011;19(11):2167–74. https://doi.org/10.1038/oby.2011.240.
Polotsky VY, Li J, Punjabi NM, Rubin AE, Smith PL, Schwartz AR, et al. Intermittent hypoxia increases insulin resistance in genetically obese mice. J Physiol. 2003;552(Pt 1):253–64. https://doi.org/10.1113/jphysiol.2003.048173.
Louis M, Punjabi NM. Effects of acute intermittent hypoxia on glucose metabolism in awake healthy volunteers. J Appl Physiol (1985). 2009;106(5):1538–44. https://doi.org/10.1152/japplphysiol.91523.2008.
Dong R, Dong Z, Liu H, Shi F, Du J. Prevalence, Risk Factors, Outcomes, and treatment of obstructive sleep apnea in patients with cerebrovascular disease: a systematic review. J Stroke Cerebrovasc Dis. 2018. https://doi.org/10.1016/j.jstrokecerebrovasdis.2017.12.048.
Ahmed SB, Ronksley PE, Hemmelgarn BR, Tsai WH, Manns BJ, Tonelli M, et al. Nocturnal hypoxia and loss of kidney function. PLoS ONE. 2011;6(4):e19029. https://doi.org/10.1371/journal.pone.0019029.
Sakaguchi Y, Hatta T, Hayashi T, Shoji T, Suzuki A, Tomida K, et al. Association of nocturnal hypoxemia with progression of CKD. Clin J Am Soc Nephrol. 2013;8(9):1502–7. https://doi.org/10.2215/CJN.11931112.
Canales MT, Hagen EW, Barnet JH, Peppard PE, Derose SF. Sleep apnea and kidney function trajectory: results from a 20-year longitudinal study of healthy middle-aged adults. Sleep. 2018. https://doi.org/10.1093/sleep/zsx181.
Dempsey JA, Veasey SC, Morgan BJ, O'Donnell CP. Pathophysiology of sleep apnea. Physiol Rev. 2010;90(1):47–112. https://doi.org/10.1152/physrev.00043.2008.
Eckert DJ, Malhotra A. Pathophysiology of adult obstructive sleep apnea. Proc Am Thorac Soc. 2008;5(2):144–53. https://doi.org/10.1513/pats.200707-114MG.
Zalucky AA, Nicholl DD, Hanly PJ, Poulin MJ, Turin TC, Walji S, et al. Nocturnal hypoxemia severity and renin-angiotensin system activity in obstructive sleep apnea. Am J Respir Crit Care Med. 2015;192(7):873–80. https://doi.org/10.1164/rccm.201502-0383OC.
Nicholl DD, Hanly PJ, Poulin MJ, Handley GB, Hemmelgarn BR, Sola DY, et al. Evaluation of continuous positive airway pressure therapy on renin-angiotensin system activity in obstructive sleep apnea. Am J Respir Crit Care Med. 2014;190(5):572–80. https://doi.org/10.1164/rccm.201403-0526OC.
Punjabi NM, Shahar E, Redline S, Gottlieb DJ, Givelber R, Resnick HE, et al. Sleep-disordered breathing, glucose intolerance, and insulin resistance: the Sleep Heart Health Study. Am J Epidemiol. 2004;160(6):521–30. https://doi.org/10.1093/aje/kwh261.
Acknowledgements
This study was supported by the Bio & Medical Technology Development Program of the NRF funded by the Korean government, MSIT (NRF-2017M3A9E8023016, NRF-2017M3A9E8023001); Grant (BCRI18024) of Chonnam National University Hospital Biomedical Research Institute; and Grant (CRI18015-1) of Chonnam National University Hospital Biomedical Research Institute.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare no competing financial interests.
Ethical approval
Ethical approval was waived in this study by the Institutional Review Board (IRB) of Chonnam National University Hospital (#IRB no. CNUH-EXP-2018-019).
Informed consent
Informed consent was not obtained because patient records and information were anonymized and de-identified prior to analysis.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Choi, H.S., Kim, H.Y., Han, KD. et al. Obstructive sleep apnea as a risk factor for incident end stage renal disease: a nationwide population-based cohort study from Korea. Clin Exp Nephrol 23, 1391–1397 (2019). https://doi.org/10.1007/s10157-019-01779-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-019-01779-6