Abstract
Background
Stroke is a global public health challenge. Frailty models can detect and consider the effects of the unknown factors influencing survival along with other known factors. This study aims to evaluate health care providers’ effect, along with the demographic and clinical factors, on the stroke patients’ survival by using the shared frailty survival models.
Methods
In the 2-year follow-up, a total of 1036 patients with first-ever stroke were recruited from 2013 up to 2015 with census sampling method from two hospitals of Iran, as the health care providers. For model selection, we fitted parametric and semiparametric survival models with parametric shared frailty and used the goodness of fit criteria to compare the models.
Result
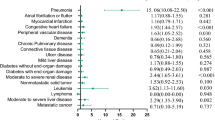
The median follow-up was 730 days. The rate of mortality was 38% during the follow-up period. The Weibull model with gamma frailty had a better fit than the other survival models. The significant variables from the Weibull model were NIHSS score as the stroke severity (score < 5: reference category; scores 5–19: HR = 2.99, p value < 0.001; score ≥ 20: HR = 5.66, p value < 0.001) and age (HR = 1.03, p value < 0.001). Even with the incorporation of the demographic and clinical factors in the survival model, the effect of health care providers as the shared frailty effect was significant (p < 0.001).
Conclusions
Despite considering the known demographic and clinical prognostic factors, health care providers’ effect on the patients’ survival after stroke was still significant. This may be due to the existing difference between two hospitals in facilities, management, coordination, and efficiency of treatment.

Similar content being viewed by others
Data availability
The data of this study were collected from two hospitals, under the supervision of Tabriz University of Medical Sciences. The dataset analyses during the current study are available from the corresponding author on reasonable request.
Code availability
Statistical analysis was done by Stata version 16 (College Station, TX: Stata Corp LLC; 2019). The ethics code of the study is IR.TBZMED.REC.1398.1203.
Abbreviations
- NIHSS:
-
Modified National Institutes of Health Stroke Scale
- BIC:
-
Bayesian information criterion
- AIC:
-
Akaike information criterion
- Ref:
-
Reference category
- BMI:
-
Body mass index
- HTN:
-
Hypertension
- SE:
-
Standard error
- HR:
-
Hazard ratio
References
Béjot Y, Daubail B, Giroud M (2016) Epidemiology of stroke and transient ischemic attacks: current knowledge and perspectives. J Rev Neurol (Paris) 172(1):59–68
Feigin VL, Stark BA, Johnson CO, Roth GA, Bisignano C, Abady GG et al (2021) Global, regional, and national burden of stroke and its risk factors, 1990–2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet Neurol 20(10):795–820
Che B, Shen S, Zhu Z, Wang A, Xu T, Peng Y et al (2020) Education level and long-term mortality, recurrent stroke, and cardiovascular events in patients with ischemic stroke. J Am Heart Assoc 9(16):e016671
Markaki I, Nilsson U, Kostulas K, Sjöstrand C (2014) High cholesterol levels are associated with improved long-term survival after acute ischemic stroke. J Stroke Cerebrovasc Dis 23(1):e47–e53
Rivera-Caravaca JM, Roldán V, Esteve-Pastor MA, Valdés M, Vicente V, Lip GY et al (2017) Cessation of oral anticoagulation is an important risk factor for stroke and mortality in atrial fibrillation patients. Thromb Haemost 117(07):1448–1454
Carlsson M, Wilsgaard T, Johnsen SH, Johnsen L-H, Løchen M-L, Njølstad I et al (2021) Long-term survival, causes of death, and trends in 5-year mortality after intracerebral hemorrhage: the Tromsø Study. Stroke 52(12):3883–3890
Kirkevold M (2010) The role of nursing in the rehabilitation of stroke survivors: an extended theoretical account. J ANS Adv Nurs Sci 33(1):E27–E40
Desvina Della, Helda (2020) Short-term survival of stroke patients according to hemorrhagic and ischemic stroke type in National Brain Center Hospital Jakarta. Ind J Public Health Res Dev 11(3):1474–8
Donkor ES (2018) Stroke in the century: a snapshot of the burden, epidemiology, and quality of life. Stroke Res Treat 2018
Du H-S, Ma J-J, Li M (2016) High-quality health information provision for stroke patients. Chin Med J 129(17):2115
Cruz-Cruz C, Moreno-Macías H, del Socorro Parra-Cabrera M, Hernández-Girón C, Calleja-Castillo JM (2019) Survival after ischemic and hemorrhagic stroke: a 4-year follow-up at a Mexican hospital. J Stroke Cerebrovasc Dis 28(8):2109–14
Meyer BC, Lyden PD (2009) The modified National Institutes of Health Stroke Scale: its time has come. Int J Stroke 4(4):267–73
Kasner SE, Cucchiara BL, McGarvey ML, Luciano JM, Liebeskind DS, Chalela JA (2003) Modified National Institutes of Health Stroke Scale can be estimated from medical records. Stroke 34(2):568–70
Kernan WN, Ovbiagele B, Black HR, Bravata DM, Chimowitz MI, Ezekowitz MD et al (2014) Guidelines for the prevention of stroke in patients with stroke and transient ischemic attack: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 45(7):2160–236
Jellinger PS, Handelsman Y, Rosenblit PD, Bloomgarden ZT, Fonseca VA, Garber AJ et al (2017) American Association of Clinical Endocrinologists and American College of Endocrinology guidelines for management of dyslipidemia and prevention of cardiovascular disease. Endocr Pract 23(s2):1–87
Monaco JV, Gorfine M, Hsu L (2018) General semiparametric shared frailty model: estimation and simulation with frailtySurv. J Stat Softw 86(4):1–42
Kim BJ, Lee S-H, Jung K-H, Yu K-H, Lee B-C, Roh J-K (2012) Dynamics of obesity paradox after stroke, related to time from onset, age, and causes of death. Neurology 79(9):856–63
Vemmos K, Ntaios G, Spengos K, Savvari P, Vemmou A, Pappa T et al (2011) Association between obesity and mortality after acute first-ever stroke: the obesity–stroke paradox. Stroke 42(1):30–6
Towfighi A, Ovbiagele BJS (2009) The impact of body mass index on mortality after stroke. Stroke 40(8):2704–8
Skolarus LE, Sanchez BN, Levine DA, Baek J, Kerber KA, Morgenstern LB et al (2014) Association of body mass index and mortality after acute ischemic stroke. Circ Cardiovasc Qual Outcomes 7(1):64–9
Forlivesi S, Cappellari M, Bonetti B (2021) Obesity paradox and stroke: a narrative review. Eat Weight Disord 26(2):417–23
Yeramaneni S, Kleindorfer DO, Sucharew H, Alwell K, Moomaw CJ, Flaherty ML et al (2017) Hyperlipidemia is associated with lower risk of poststroke mortality independent of statin use: a population-based study. Int J Stroke 12(2):152–160
Eriksson S-E, Olsson J-E (2001) Survival and recurrent strokes in patients with different subtypes of stroke: a fourteen-year follow-up study. Cerebrovasc Dis 12(3):171–80
Liu X, Xu G, Wu W, Zhang R, Yin Q, Zhu W (2006) Subtypes and one-year survival of first-ever stroke in Chinese patients: the Nanjing Stroke Registry. Cerebrovasc Dis 22(2–3):130–6
Oksala N, Oksala A, Pohjasvaara T, Vataja R, Kaste M, Karhunen P et al (2009) Age related white matter changes predict stroke death in long term follow-up. J Neurol Neurosurg Psychiatry 80(7):762–6
Rønning OM (2013) Very long-term mortality after ischemic stroke: predictors of cardiovascular death. Acta Neurol Scand Suppl 127:69–72
Arboix A, García-Eroles L, Oliveres M, Targa C, Balcells M, Massons J (2010) Pretreatment with statins improves early outcome in patients with first-ever ischaemic stroke: a pleiotropic effect of statins or a beneficial effect of hypercholesterolemia? BMC Neurol 10(1):47
Fernandes TG, Goulart AC, Santos-Junior WR, Alencar AP, Benseñor IM, Lotufo PA (2012) Educational levels and the functional dependence of ischemic stroke survivors. Cad Saude Publica 28:1581–90
Che B, Shen S, Zhu Z, Wang A, Xu T, Peng Y et al (2020) Education level and long-term mortality, recurrent stroke, and cardiovascular events in patients with ischemic stroke. J Am Heart Assoc 9(16):e016671
Elfassy T, Grasset L, Glymour MM, Swift S, Zhang L, Howard G et al (2019) Sociodemographic disparities in long-term mortality among stroke survivors in the United States: The REGARDS Study. Stroke 50(4):805–812
Novbakht H, Shamshirgaran SM, Sarbakhsh P, Savadi-Oskouei D, Yazdchi MM, Ghorbani Z (2020) Predictors of long-term mortality after first-ever stroke. J Educ Health Promot 9:45
Bryndziar T, Matyskova D, Sedova P, Belaskova S, Zvolsky M, Bednarik J et al (2021) Predictors of short-and long-term mortality in ischemic stroke: a community-based study in Brno, Czech Republic. Cerebrovasc Dis 17:1–8. https://doi.org/10.1159/000519937
Adoukonou T, Agbétou M, Bangbotché R, Kossi O, Mefo PF, Magne J et al (2020) Long-term mortality of stroke survivors in Parakou: 5-year follow-up. J Stroke Cerebrovasc Dis 29(6):104785
Balan TA, Putter H (2019) frailtyEM: An R package for estimating semiparametric shared frailty models. J Stat Softw 90(7):1–29
Munda M, Rotolo F, Legrand C (2012. parfm: Parametric Frailty Models in R. Journal of Statistical Software 51(11):1–20. https://doi.org/10.18637/jss.v051.i11
Tesema GA, Worku MG, Teshale AB (2021) Duration of birth interval and its predictors among reproductive-age women in Ethiopia: Gompertz gamma shared frailty modeling. Plos one 16(2):e0247091
Cho KH, Nam CM, Lee SG, Kim TH, Lee S-H, Park E-C (2019) Measuring of quality of care in patients with stroke and acute myocardial infarction: an application of algebra effectiveness model. Medicine (Baltimore) 98(20):e15353
Ingeman A, Pedersen L, Hundborg HH, Petersen P, Zielke S, Mainz J et al (2008) Quality of care and mortality among patients with stroke: a nationwide follow-up study. Med Care 46:63–9
Okere AN, Sanogo V, Balkrishnan R, Diaby V (2020) A quantitative analysis of the effect of continuity of care on 30-day readmission and in-hospital mortality among patients with acute ischemic stroke. J Stroke Cerebrovasc Dis 29(9):105053
Acknowledgements
This study has been extracted from a master’s thesis (in progress, with code IR.TBZMED.REC.1398.1203). We thank Tabriz University of Medical Sciences for financial support.
Funding
Tabriz University of Medical Sciences supported our study in data collection and analysis of data.
Author information
Authors and Affiliations
Contributions
Navideh Nikmohammadi performed the analyses, interpreted the results, and prepared the manuscript. Neda Gilani contributed to comment on the manuscript. Morteza Shamshirgaran was involved in data collection. Parvin Sarbakhsh contributed to the interpretation and clarification of the data and commented on the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval
The ethical aspects of this study were approved by the institutional ethics committee of Tabriz University of Medical Sciences, with code IR.TBZMED.REC.1398.1203.
Consent to participate
We confirm that informed consent has been taken from all participants.
Consent for publication
The manuscript is extracted from MSc dissertation in Tabriz University of Medical Sciences. All authors consented publication of manuscript.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nikmohammadi, N., Gilani, N., Shamshirgaran, S.M. et al. Health care providers’ effect on long-term mortality after the first-ever stroke: application of shared frailty survival models. Neurol Sci 43, 4307–4313 (2022). https://doi.org/10.1007/s10072-022-05983-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-022-05983-3