Abstract
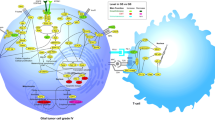
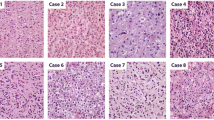
This study aims to establish a simplified molecular classification of glioblastomas (GBMs) based on molecular genetic alterations. GBM cases (n-114) were evaluated for IDH-1 and TP53 mutation by Sanger sequencing, PDGFRA and EGFR amplification by FISH, NF1 and YKL40 expression by qRT-PCR. Subsequently they were classified into four subgroups: classical like (CL), proneural like (PN), mesenchymal like (MES) and neural like (NEU). CL subtype was most frequent (39 %), followed by PN (32 %) and MES (20 %) subtypes. PN subtype had significantly younger age at presentation and longest survival (median PFS—82.5 weeks; 1 and 2 years OS—90.6 and 71.3 %). Other three subgroups had equally poor prognosis and hence, clubbed together as non-proneural (Non-PN) (median PFS—39 weeks; 1 and 2 years OS—66 and 0 %). Hence, we recommended this relatively easy method of subclassifying GBMs into PN and Non-PN which are statistically different in prognosis (both OS and PFS on uni and multivariate analysis). Although evaluation of six molecular alterations for identifying these two subgroups is still cumbersome, we propose segregation of PN subtype alone based on assessment of IDH1, TP53 and PDGFRA status, which is relatively easy and may be amenable to routine practice.


Similar content being viewed by others
References
Dolecek TA, Propp JM, Stroup NE, Kruchko C (2009) CBTRUS statistical report: primary brain and central nervous system tumors diagnosed in the United States in 2005–2009. Neuro Oncol 14:1–49
Stupp R, Hegi ME, Mason WP et al (2009) Effects of radiotherapy with concomitant and adjuvant temozolomide versus radiotherapy alone on survival in glioblastoma in a randomised phase III study: 5-year analysis of the EORTC-NCIC trial. Lancet Oncol 10:459–466
Louis DN, Ohgaki H, Wiestler OD, Cavenee WK (2007) WHO classification of tumours of the central nervous system. In: Bosman FT, Jaffe ES, Lakhani SR, Ohgaki H (eds) International Agency for Research on Cancer (IARC), Lyon
Phillips HS, Kharbanda S, Chen R et al (2006) Molecular subclasses of high-grade glioma predict prognosis, delineate a pattern of disease progression, and resemble stages in neurogenesis. Cancer Cell 9:157–173
Verhaak RG, Hoadley KA, Purdom E et al (2010) Integrated genomic analysis identifies clinically relevant subtypes of glioblastoma characterized by abnormalities in PDGFRA, IDH1, EGFR, and NF1. Cancer Cell 17:98–110
Brennan C, Momota H, Hambardzumyan D et al (2009) Glioblastoma subclasses can be defined by activity among signal transduction pathways and associated genomic alterations. PLoS One 4:e7752
Jalali R, Datta D (2008) Prospective analysis of incidence of central nervous tumors presenting in a tertiary cancer hospital from India. J Neurooncol 87:111–114
Jha P, Suri V, Singh G et al (2011) Characterization of molecular genetic alterations in GBMs highlights a distinctive molecular profile in young adults. Diagn Mol Pathol 20:225–232
Ohgaki H, Kleihues P (2007) Genetic pathways to primary and secondary glioblastoma. Am J Pathol 170:1445–1453
Brennan CW, Verhaak RG, McKenna A et al (2013) The somatic genomic landscape of glioblastoma. Cell 155:462–477
Purkait S, Jha P, Sharma MC et al (2013) CDKN2A deletion in pediatric versus adult glioblastomas and predictive value of p16 immunohistochemistry. Neuropathology 33:405–412
Lee Y, Scheck AC, Cloughesy TF et al (2008) Gene expression analysis of glioblastomas identifies the major molecular basis for the prognostic benefit of younger age. BMC Med Genomics 1:52
Popova SN, Bergqvist M, Dimberg A et al (2014) Subtyping of gliomas of various WHO grades by the application of immunohistochemistry. Histopathology 64:365–379
Le Mercier M, Hastir D, Moles Lopez X et al (2012) A simplified approach for the molecular classification of glioblastomas. PLoS One 7:e45475
Guillaudeau A, Durand K, Pommepuy I et al (2009) Determination of EGFR status in gliomas: usefulness of immunohistochemistry and fluorescent in situ hybridization. Appl Immunohistochem Mol Morphol 17:220–226
Marquez A, Wu R, Zhao J et al (2004) Evaluation of epidermal growth factor receptor (EGFR) by chromogenic in situ hybridization (CISH) and immunohistochemistry (IHC) in archival gliomas using bright-field microscopy. Diagn Mol Pathol 13:1–8
Martinho O, Longatto-Filho A, Lambros MB et al (2009) Expression, mutation and copy number analysis of platelet-derived growth factor receptor A (PDGFRA) and its ligand PDGFA in gliomas. Br J Cancer 101:973–982
Pollack IF, Hamilton RL, Finkelstein SD et al (1997) The relationship between TP53 mutations and overexpression of p53 and prognosis in malignant gliomas of childhood. Cancer Res 57:304–309
Yoon KS, Lee MC, Kang SS et al (2001) p53 mutation and epidermal growth factor receptor overexpression in glioblastoma. J Korean Med Sci 16:481–488
Calzolari A, Chiarelli I, Bianchi S et al (1997) Immunohistochemical vs molecular biology methods. Complementary techniques for effective screening of p53 alterations in head and neck cancer. Am J Clin Pathol 107:7–11
Noushmehr H, Weisenberger DJ, Diefes K et al (2010) Identification of a CpG island methylator phenotype that defines a distinct subgroup of glioma. Cancer Cell 17:510–522
Jha P, Pia Patric IR, Shukla S et al (2014) Genome-wide methylation profiling identifies an essential role of reactive oxygen species in pediatric glioblastoma multiforme and validates a methylome specific for H3 histone family 3A with absence of G-CIMP/isocitrate dehydrogenase 1 mutation. Neuro Oncol 16:1607–1617
Hartmann C, Meyer J, Balss J et al (2009) Type and frequency of IDH1 and IDH2 mutations are related to astrocytic and oligodendroglial differentiation and age: a study of 1,010 diffuse gliomas. Acta Neuropathol 118:469–474
Sonoda Y, Kumabe T, Nakamura T et al (2009) Analysis of IDH1 and IDH2 mutations in Japanese glioma patients. Cancer Sci 100:1996–1998
Yan H, Parsons DW, Jin G et al (2009) IDH1 and IDH2 mutations in gliomas. N Engl J Med 360:765–773
Agarwal S, Sharma MC, Jha P et al (2013) Comparative study of IDH1 mutations in gliomas by immunohistochemistry and DNA sequencing. Neuro Oncol 15:718–726
Acknowledgments
The authors are thankful to Indian Council of Medical Research (ICMR) and Neuro Sciences Centre for funding; all consultants from the Departments of Pathology and Neurosurgery, AIIMS; all technical staff from the Neuropathology laboratory, AIIMS and Department of Biostatistics, AIIMS.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Purkait, S., Mallick, S., Sharma, V. et al. A simplified approach for molecular classification of glioblastomas (GBMs): experience from a tertiary care center in India. Brain Tumor Pathol 33, 183–190 (2016). https://doi.org/10.1007/s10014-016-0251-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10014-016-0251-y