Abstract
Background
The mandible of the rabbit is considered a reliable model to be used to study bone regeneration in defects. The aim of the present study was to evaluate the formation of new bone around implants installed in defects of either 5 or 10 mm in the mandible of rabbits.
Materials and methods
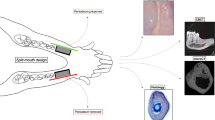
In 12 rabbits, 3 mm deep circumferential defect, either 5 or 10 mm in diameter, were prepared bilaterally and an implant was placed in the center. A collagen membrane was placed to close the entrance. After 10 weeks, biopsies were taken, histological slides were prepared, and different regions of the defects were analyzed.
Results
Similar amounts of new bone were found in both defects. However, most of the 5 mm defects were filled with new bone. New bone was observed closing the entrance of the defect and laid onto the implant surface. Only in a few cases the healing was incomplete. Despite a similar percentage of new bone found within the 10 mm defects, the healing was incomplete in most of the cases, presenting a low rate of bone formation onto the implant surface within the defect. Only one case presented the closure of the entrance.
Conclusions
The dimensions of the defect strongly influenced the healing so that a circumferential marginal defect of 10 mm around an implant in the mandible body should be considered a critical-sized defect. The presence of the implant and of residues of teeth might have strongly influenced the healing.








Similar content being viewed by others
Data availability
No datasets were generated or analysed during the current study.
References
Guo J, Meng Z, Chen G, Xie D, Chen Y, Wang H, Tang W, Liu L, Jing W, Long J, Guo W, Tian W (2012) Restoration of critical-size defects in the rabbit mandible using porous nanohydroxyapatite-polyamide scaffolds. Tissue Eng Part A 18(11–12):1239–1252. https://doi.org/10.1089/ten.TEA.2011.0503Epub 2012 Mar 19. PMID: 22320360
Bos GD, Goldberg VM, Powell AE, Heiple KG, Zika JM (1983) The effect of histocompatibility matching on canine frozen bone allografts. J Bone Joint Surg 65:89–96
Hollinger JO, Kleinschmidt JC (1990) The critical size defect as an experimental model to test bone repair materials. J Craniofac Surg. ;1(1):60 – 8. https://doi.org/10.1097/00001665-199001000-00011. PMID: 1965154
Schmitz JP, Hollinger JO (1996) The critical size defect as an experimental model for craniomandibulofacial non-unions. Clin Orthop Relat Res 205:299–308
Cooper GM, Mooney MP, Gosain AK, Campbell PG, Losee JE, Huard J (2010) Testing the critical size in calvarial bone defects: revisiting the concept of a critical-size defect. Plast Reconstr Surg 125(6):1685–1692. https://doi.org/10.1097/PRS.0b013e3181cb63a3PMID: 20517092; PMCID: PMC2946111
Monir A, Mukaibo T, Abd El-Aal ABM, Nodai T, Munemasa T, Kondo Y, Masaki C, El-Shair MA, Matsuo K, Hosokawa R (2021) Local administration of HMGB-1 promotes bone regeneration on the critical-sized mandibular defects in rabbits. Sci Rep 11(1):8950. https://doi.org/10.1038/s41598-021-88195-7PMID: 33903607; PMCID: PMC8076241
Awadeen MA, Al-Belasy FA, Ameen LE, Helal ME, Grawish ME (2020) Early therapeutic effect of platelet-rich fibrin combined with allogeneic bone marrow-derived stem cells on rats’ critical-sized mandibular defects. World J Stem Cells 12(1):55–69. https://doi.org/10.4252/wjsc.v12.i1.55PMID: 32110275; PMCID: PMC7031757
Trejo-Iriarte CG, Serrano-Bello J, Gutiérrez-Escalona R, Mercado-Marques C, García-Honduvilla N, Buján-Varela J, Me-dina LA (2019) Evaluation of bone regeneration in a critical size cortical bone defect in rat mandible using microCT and his-tological analysis. Arch Oral Biol. ;101:165–171. doi: 10.1016/j.archoralbio.2019.01.010. Epub 2019 Feb 5. PMID: 30951954
Frame JW (1980) A convenient animal model for testing bone substitute materials. J Oral Surg 38(3):176–180 PMID: 6928181
Gilsanz V, Roe TF, Gibbens DT, Schulz EE, Carlson ME, Gonzalez O, Boechat MI (1988) Effect of sex steroids on peak bone density of growing rabbits. Am J Physiology-Endocrinology Metabolism 255:416–421
Pearce AI, Richards RG, Milz S, Schneider E, Pearce SG (2007) Animal models for implant biomaterial research in bone: a review. Eur Cell Mater. ;13:1–10. https://doi.org/10.22203/ecm.v013a01. PMID: 17334975
Newman E, Turner AS, Wark JD (1995) The potential of sheep for the study of osteopenia: current status and comparison with other animal models. Bone 16:277–284
Castaneda S, Largo R, Calvo E, Rodriguez-Salvanes F, Marcos ME, Diaz-Curiel M, Herrero-Beaumont G (2006) Bone mineral measurements of subchondral and trabecular bone in healthy and osteoporotic rabbits. Skeletal Radiol 35:34–41
Cheng G, Li Z, Wan Q, Lv K, Li D, Xing X, Li Z (2015) A novel animal model treated with tooth extraction to repair the full-thickness defects in the mandible of rabbits. J Surg Res 194(2):706–716 Epub 2014 Nov 14. PMID: 25491176
Jianqi H, Hong H, Lieping S, Genghua G (2002) Comparison of calcium alginate film with collagen membrane for guided bone regeneration in mandibular defects in rabbits. J Oral Maxillofac Surg. ;60(12):1449-54. https://doi.org/10.1053/joms.2002.36108. PMID: 12465009
Kazakos K, Lyras DN, Thomaidis V, Agrogiannis G, Botaitis S, Drosos G, Kokka A, Verettas D (2011) Application of PRP gel alone or in combination with guided bone regeneration does not enhance bone healing process: an experimental study in rabbits. J Craniomaxillofac Surg 39(1):49–53 Epub 2010 Apr 24. PMID: 20456969
Wang Y, Zhang X, Mei S, Li Y, Khan AA, Guan S, Li X (2023) Determination of critical-sized defect of mandible in a rabbit model: micro-computed tomography, and histological evaluation. Heliyon 9(7):e18047. https://doi.org/10.1016/j.heliyon.2023.e18047PMID: 37539284; PMCID: PMC10393617
Sakaguchi R, Xavier SP, Morinaga K, Botticelli D, Silva ER, Nakajima Y, Baba S (2023) Histological comparison of Collagenated Cancellous equine bone blocks used as inlay or onlay for lateral bone augmentation in rabbits. Mater (Basel) 16(20):6742. https://doi.org/10.3390/ma16206742PMID: 37895725; PMCID: PMC10608602Xxxxxxx
Asano A, Xavier SP, Ricardo Silva E, Morinaga K, Botticelli D, Nakajima Y, Baba S Critical-sized marginal defects around implants treated with xenografts in rabbits. Accepted for publication in Oral Maxillofac Surg
Botticelli D, Berglundh T, Lindhe J (2004) Resolution of bone defects of varying dimension and configuration in the marginal portion of the peri-implant bone. An experimental study in the dog. J Clin Periodontol. ;31(4):309 – 17. https://doi.org/10.1111/j.1600-051X.2004.00502.x. PMID: 15016260
Faul F, Erdfelder E, Buchner A, Lang AG (2009) Statistical power analyses using G*Power 3.1: tests for correlation and regression analyses. Behav Res Methods. ;41(4):1149-60. https://doi.org/10.3758/BRM.41.4.1149. PMID: 19897823
Faul F, Erdfelder E, Lang AG, Buchner A (2007) G*Power 3: a flexible statistical power analysis program for the social, be-havioral, and biomedical sciences. Behav Res Methods. ;39(2):175 – 91. https://doi.org/10.3758/bf03193146. PMID: 17695343
Kotagudda Ranganath S, Schlund M, Delattre J, Ferri J, Chai F (2022) Bilateral double site (calvarial and mandibular) critical-size bone defect model in rabbits for evaluation of a craniofacial tissue engineering constructs. Mater Today Bio 14:100267. https://doi.org/10.1016/j.mtbio.2022.100267
Wang Y, Zhang X, Mei S, Li Y, Khan AA, Guan S, Li X (2023) Determination of critical-sized defect of mandible in a rabbit model: micro-computed tomography, and histological evaluation. Heliyon 9(7):e18047. https://doi.org/10.1016/j.heliyon.2023.e18047
Carmagnola D, Berglundh T, Lindhe J (2002) The effect of a fibrin glue on the integration of Bio-Oss with bone tissue. A ex-perimental study in labrador dogs. J Clin Periodontol. ;29(5):377 – 83. https://doi.org/10.1034/j.1600-051x.2002.290501.x. PMID: 12060419
Cardaropoli G, Araújo M, Hayacibara R, Sukekava F, Lindhe J (2005) Healing of extraction sockets and surgically produced - augmented and non-augmented - defects in the alveolar ridge. An experimental study in the dog. J Clin Periodontol. ;32(5):435 – 40. https://doi.org/10.1111/j.1600-051X.2005.00692.x. PMID: 15842256
Botticelli D, Berglundh T, Buser D, Lindhe J (2003) Appositional bone formation in marginal defects at implants. Clin Oral Implants Res. ;14(1):1–9. https://doi.org/10.1034/j.1600-0501.2003.140101.x. PMID: 12562359
Botticelli D, Berglundh T, Buser D, Lindhe J (2003) The jumping distance revisited: An experimental study in the dog. Clin Oral Implants Res. ;14(1):35–42. https://doi.org/10.1034/j.1600-0501.2003.140105.x. PMID: 12562363
Cardaropoli G, Araújo M, Lindhe J (2003) Dynamics of bone tissue formation in tooth extraction sites. An experimental study in dogs. J Clin Periodontol. ;30(9):809 – 18. https://doi.org/10.1034/j.1600-051x.2003.00366.x. PMID: 12956657
Araújo MG, Lindhe J (2005) Dimensional ridge alterations following tooth extraction. An experimental study in the dog. J Clin Periodontol. ;32(2):212-8. https://doi.org/10.1111/j.1600-051X.2005.00642.x. PMID: 15691354
Scala A, Lang NP, Schweikert MT, de Oliveira JA, Rangel-Garcia I Jr, Botticelli D (2014) Sequential healing of open extraction sockets. An experimental study in monkeys. Clin Oral Implants Res. ;25(3):288–295. https://doi.org/10.1111/clr.12148. Epub 2013 Apr 1. PMID: 23551527
Akimoto K, Becker W, Persson R, Baker DA, Rohrer MD, O’Neal RB (1999 May-Jun) Evaluation of titanium implants placed into simulated extraction sockets: a study in dogs. Int J Oral Maxillofac Implants 14(3):351–360 PMID: 10379108
Botticelli D, Berglundh T, Persson LG, Lindhe J (2005) Bone regeneration at implants with turned or rough surfaces in self-contained defects. An experimental study in the dog. J Clin Periodontol. ;32(5):448 – 55. https://doi.org/10.1111/j.1600-051X.2005.00693.x. PMID: 15842258
Li J, Zheng Y, Yu Z, Kankala RK, Lin Q, Shi J, Chen C, Luo K, Chen A, Zhong Q (2023) Surface-modified titanium and titanium-based alloys for improved osteogenesis: a critical review. Heliyon 10(1):e23779 PMID: 38223705; PMCID: PMC10784177
Liang J, Lu X, Zheng X, Li YR, Geng X, Sun K, Cai H, Jia Q, Jiang HB, Liu K (2023) Modification of titanium orthopedic implants with bioactive glass: a systematic review of in vivo and in vitro studies. Front Bioeng Biotechnol 11:1269223. https://doi.org/10.3389/fbioe.2023.1269223PMID: 38033819; PMCID: PMC10686101
Yang S, Jiang W, Ma X, Wang Z, Sah RL, Wang J, Sun Y (2023) Nanoscale morphologies on the surface of 3D-Printed Titanium implants for Improved Osseointegration: a systematic review of the literature. Int J Nanomed 18:4171–4191 PMID: 37525692; PMCID: PMC10387278
Scarano A, Orsini T, Di Carlo F, Valbonetti L, Lorusso F (2021) Graphene-Doped Poly (Methyl-Methacrylate) (Pmma) implants: a Micro-CT and histomorphometrical study in rabbits. Int J Mol Sci 22(3):1441. https://doi.org/10.3390/ijms22031441PMID: 33535482; PMCID: PMC7867091
Rahmani R, Lyubartsev AP (2023) Biomolecular Adsorprion at ZnS nanomaterials: a Molecular Dynamics Simulation Study of the Adsorption preferences, effects of the Surface curvature and coating. Nanomaterials (Basel) 13(15):2239. https://doi.org/10.3390/nano13152239PMID: 37570556; PMCID: PMC10421200
Araújo MG, Sonohara M, Hayacibara R, Cardaropoli G, Lindhe J (2002) Lateral ridge augmentation by the use of grafts comprised of autologous bone or a biomaterial. An experiment in the dog. J Clin Periodontol. ;29(12):1122-31. https://doi.org/10.1034/j.1600-051x.2002.291213.x. PMID: 12492915
Santis E, Lang NP, Favero G, Beolchini M, Morelli F, Botticelli D (2015) Healing at mandibular block-grafted sites. An experimental study in dogs. Clin Oral Implants Res 26(5):516–522. https://doi.org/10.1111/clr.12434Epub 2014 Jun 12. PMID: 24921198
Kanayama M, Botticelli D, Apaza Alccayhuaman KA, Yonezawa D, Silva ER, Xavier SP (2021) Jul-Aug;36(4):703–714 The Impact on the Healing of Bioactivation with Argon Plasma of a Xenogeneic Graft with Adequate Fixation but Poor Adaptation to the Recipient Site: An Experimental Study in Rabbits. Int J Oral Maxillofac Implants. https://doi.org/10.11607/jomi.8695. PMID: 34411209
Herford AS, Boyne PJ (2008) Reconstruction of mandibular continuity defects with bone morphogenetic protein-2 (rhBMP-2). J Oral Maxillofac Surg 66:616–624
Chim H, Gosain AK (2009) Biomaterials in craniofacial surgery: experimental studies and clinical application. J Craniofac Surg 20:29–33
Misch CE, Qu Z, Bidez MW (1999) Mechanical properties of trabecular bone in the human mandible: implications for dental implant treatment planning and surgical placement. J Oral Maxillofac Surg 57:700–706 discussion 706-8
Acknowledgements
We thank Dr. Vitor Ferreira Balan for the surgical procedures and Mr. Sebas-tiao Blanco (University of São Paulo, Faculty of Dentistry of Ribeirão Preto) for processing the histological slides. The scientific contribution in the histological assessment by Dr. Alí Karol Apaza Alccayhuaman (Department of Oral Biology, Medical University of Vienna, 1090 Vienna, Austria) was greatly appreciated. The implants were donated by Leader Medica, Padua, Italy.
Funding
The study was economically supported by ARDEC Academy, Italy.
Author information
Authors and Affiliations
Contributions
A.M. contributed in the conceptualization, methodology, formal analysis, data curation, writing the original draft and reviewing the final version of the article.S.P.X. reviewing the final version of the article in the conceptualization, methodology, and investigation.E.R.S. in investigation.K.M. contributed contributed in conceptualization and reviewing and editing the article.D.B. contributed contributed in conceptualization, methodology, formal analysis, data curation, writing the original draft and reviewing and editing the article, project administration and funding acquisition.Y.N. contributed in methodology, project administration and funding acquisition.S.B. contributed in conceptualization, supervision of the project, reviewing and editing the article.All authors have read and approved the article before submission for publication.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Morimoto, A., Porfirio Xavier, S., Ricardo Silva, E. et al. Critical-sized marginal defects around implants in the rabbit mandible. Oral Maxillofac Surg (2024). https://doi.org/10.1007/s10006-024-01233-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10006-024-01233-2