Abstract
Purpose
Peri-implantitis is a biofilm-induced pathological condition, and different approaches have been proposed to manage this condition. This study introduces a surgical technique in accordance with the concept of guided bone regeneration for implants with extensive peri-implant defects.
Methods
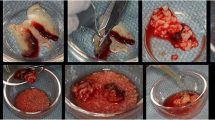
This pilot study was conducted on 7 patients with 11 implants (4 females and 3 males; 32 to 61 years). In this technique, we used a titanium mesh, a combination of autogenous bone, allogenic graft material, and acellular dermal matrix to reconstruct the peri-implant defects. All implants were placed submerged, and the second-stage surgery was conducted after 8 months. Soft tissue augmentation and vestibuloplasty were performed in the second-stage surgery, if required.
Results
The mean function time of implants was 60.5 ± 29.4 months. The mean baseline probing pocket depth was 5.7 ± 1.4 mm, and soft tissue recession was observed at two sites (18%). The mean recession and keratinized tissue width (KTW) values were 0.4 ± 0.8 mm and 3 ± 1.6 mm, respectively. The mean marginal bone loss and bone gain were 4.4 ± 1.2 mm and 2.9 ± 0.9 mm, respectively, which showed a significant improvement.
Conclusion
Our preliminary evaluations showed favorable results in terms of radiographic defect fill and soft tissue condition. It appears that this technique may lead to promising outcomes in cautiously selected patients seeking to retain their failing implants. However, long-term results following functional loading are required before recommending this technique for daily practice.



Similar content being viewed by others
References
Hasturk H, Kantarci A (2015) Activation and resolution of periodontal inflammation and its systemic impact. Periodontol 2000 69(1):255–273. https://doi.org/10.1111/prd.12105
Teles R, Teles F, Frias-Lopez J, Paster B, Haffajee A (2013) Lessons learned and unlearned in periodontal microbiology. Periodontol 2000 62(1):95–162. https://doi.org/10.1111/prd.12010
Derks J, Schaller D, Hakansson J, Wennstrom JL, Tomasi C, Berglundh T (2016) Peri-implantitis - onset and pattern of progression. J Clin Periodontol 43(4):383–388. https://doi.org/10.1111/jcpe.12535
Fransson C, Tomasi C, Pikner SS, Gröndahl K, Wennström JL, Leyland AH et al (2010) Severity and pattern of peri-implantitis-associated bone loss. J Clin Periodontol 37(5):442–448. https://doi.org/10.1111/j.1600-051X.2010.01537.x
Schwarz F, Derks J, Monje A, Wang H-L (2018) Peri-implantitis. J Clin Periodontol 45(Suppl 20):S246–S266. https://doi.org/10.1111/jcpe.12954
Staubli N, Walter C, Schmidt JC, Weiger R, Zitzmann NU (2017) Excess cement and the risk of peri-implant disease - a systematic review. Clin Oral Implants Res 28(10):1278–1290. https://doi.org/10.1111/clr.12954
Monje A, Insua A, Wang HL (2019) Understanding peri-implantitis as a plaque-associated and site-specific entity: on the local predisposing factors. J Clin Med 8(2). https://doi.org/10.3390/jcm8020279.
Schwarz F, Hegewald A, Becker J (2014) Impact of implant-abutment connection and positioning of the machined collar/microgap on crestal bone level changes: a systematic review. Clin Oral Implants Res 25(4):417–425. https://doi.org/10.1111/clr.12215
John G, Becker J, Schmucker A, Schwarz F (2017) Non-surgical treatment of peri-implant mucositis and peri-implantitis at two-piece zirconium implants: A clinical follow-up observation after up to 3 years. J Clin Periodontol 44(7):756–761. https://doi.org/10.1111/jcpe.12738
Carcuac O, Abrahamsson I, Charalampakis G, Berglundh T (2015) The effect of the local use of chlorhexidine in surgical treatment of experimental peri-implantitis in dogs. J Clin Periodontol 42(2):196–203. https://doi.org/10.1111/jcpe.12332
Berglundh T, Wennstrom JL, Lindhe J (2018) Long-term outcome of surgical treatment of peri-implantitis. A 2–11-year retrospective study. Clin Oral Implants Res 29(4):404–410. https://doi.org/10.1111/clr.13138
Renvert S, Polyzois I, Maguire R (2009) Re-osseointegration on previously contaminated surfaces: a systematic review. Clin Oral Implants Res 20(Suppl 4):216–227. https://doi.org/10.1111/j.1600-0501.2009.01786.x
Esposito M, Ardebili Y, Worthington HV (2014) Interventions for replacing missing teeth: different types of dental implants. Cochrane Database Syst Rev 2014(7):CD003815-CD. https://doi.org/10.1002/14651858.CD003815.pub4
Atieh MA, Alsabeeha NH, Faggion CM Jr, Duncan WJ (2013) The frequency of peri-implant diseases: a systematic review and meta-analysis. J Periodontol 84(11):1586–1598. https://doi.org/10.1902/jop.2012.120592
Halperin-Sternfeld M, Zigdon-Giladi H, Machtei EE (2016) The association between shallow vestibular depth and peri-implant parameters: a retrospective 6 years longitudinal study. J Clin Periodontol 43(3):305–310
Kadkhodazadeh M, Amid R (2012) Evaluation of peri-implant tissue health using a scoring system. JIACD 4:51–57
De Bruyn H, Vandeweghe S, Ruyffelaert C, Cosyn J, Sennerby L (2013) Radiographic evaluation of modern oral implants with emphasis on crestal bone level and relevance to peri-implant health. Periodontol 2000 62(1):256–70. https://doi.org/10.1111/prd.12004
Aghazadeh A, Rutger Persson G, Renvert S (2012) A single-centre randomized controlled clinical trial on the adjunct treatment of intra-bony defects with autogenous bone or a xenograft: results after 12 months. J Clin Periodontol 39(7):666–673. https://doi.org/10.1111/j.1600-051X.2012.01880.x
Khoury F, Buchmann R (2001) Surgical therapy of peri-implant disease: a 3-year follow-up study of cases treated with 3 different techniques of bone regeneration. J Periodontol 72(11):1498–1508. https://doi.org/10.1902/jop.2001.72.11.1498
Roos-Jansåker A-M, Renvert H, Lindahl C, Renvert S (2007) Surgical treatment of peri-implantitis using a bone substitute with or without a resorbable membrane: a prospective cohort study. J Clin Periodontol 34(7):625–632. https://doi.org/10.1111/j.1600-051X.2007.01102.x
Schwarz F, Sahm N, Bieling K, Becker J (2009) Surgical regenerative treatment of peri-implantitis lesions using a nanocrystalline hydroxyapatite or a natural bone mineral in combination with a collagen membrane: a four-year clinical follow-up report. J Clin Periodontol 36(9):807–814. https://doi.org/10.1111/j.1600-051X.2009.01443.x
Tomasi C, Regidor E, Ortiz-Vigón A, Derks J (2019) Efficacy of reconstructive surgical therapy at peri-implantitis-related bone defects. A systematic review and meta-analysis. J Clin Periodontol 46 Suppl 21:340–356. https://doi.org/10.1111/jcpe.13070
Schwarz F, Herten M, Sager M, Bieling K, Sculean A, Becker J (2007) Comparison of naturally occurring and ligature-induced peri-implantitis bone defects in humans and dogs. Clin Oral Implants Res 18(2):161–170. https://doi.org/10.1111/j.1600-0501.2006.01320.x
Aghazadeh A, Persson RG, Renvert S (2020) Impact of bone defect morphology on the outcome of reconstructive treatment of peri-implantitis. Int J Implant Dent 6(1):33. https://doi.org/10.1186/s40729-020-00219-5
Schwarz F, Sahm N, Schwarz K, Becker J (2010) Impact of defect configuration on the clinical outcome following surgical regenerative therapy of peri-implantitis. J Clin Periodontol 37(5):449–455. https://doi.org/10.1111/j.1600-051X.2010.01540.x
Heitz-Mayfield LJA, Salvi GE, Mombelli A, Faddy M, Lang NP (2012) Anti-infective surgical therapy of peri-implantitis. A 12-month prospective clinical study. Clin Oral Implants Res 23(2):205–210. https://doi.org/10.1111/j.1600-0501.2011.02276.x
Thabit AK, Fatani DF, Bamakhrama MS, Barnawi OA, Basudan LO, Alhejaili SF (2019) Antibiotic penetration into bone and joints: An updated review. Int J Infect Dis 81:128–136. https://doi.org/10.1016/j.ijid.2019.02.005
Vigano P, Alccayhuaman KAA, Sakuma Sh, Amari Y, Franco B, Botticelli D (2019) Use of TiBrush for surface decontamination at peri-implantitis sites in dogs: Radiographic and histological outcomes. J Investig Clin Dent 10(1):e12378. https://doi.org/10.1111/jicd.12378
Aljohani M, Yong SL, Bin RA (2020) The effect of surgical regenerative treatment for peri-implantitis: A systematic review. Saudi Dent J 32(3):109–119. https://doi.org/10.1016/j.sdentj.2019.10.006
Froum SJ, Froum SH, Rosen PS (2012) Successful management of peri-implantitis with a regenerative approach: a consecutive series of 51 treated implants with 3- to 7.5-year follow-up. Int J Periodontics Restorative Dent. 32(1):11–20
Roccuzzo M, Pittoni D, Roccuzzo A, Charrier L, Dalmasso P (2017) Surgical treatment of peri-implantitis intrabony lesions by means of deproteinized bovine bone mineral with 10% collagen: 7-year-results. Clin Oral Implants Res 28(12):1577–1583. https://doi.org/10.1111/clr.13028
Schwarz F, John G, Mainusch S, Sahm N, Becker J (2012) Combined surgical therapy of peri-implantitis evaluating two methods of surface debridement and decontamination. A two-year clinical follow up report. J Clin Periodontol 39(8):789–797. https://doi.org/10.1111/j.1600-051X.2012.01867.x
Wiltfang J, Zernial O, Behrens E, Schlegel A, Warnke PH, Becker ST (2012) Regenerative treatment of peri-implantitis bone defects with a combination of autologous bone and a demineralized xenogenic bone graft: a series of 36 defects. Clin Implant Dent Relat Res 14(3):421–427. https://doi.org/10.1111/j.1708-8208.2009.00264.x
Morelli F, Apaza Alccayhuaman KA, Vigano P, Bengazi F, Urbizo J, Cesaretti G, Botticelli D (2019) Peri-implantitis at implants with diffetent diameters: a pilot study in dogs. Int J Implant Dent 5(1):21. https://doi.org/10.1186/s40729-019-0177-3
Dalago HR, Schuldt Filho G, Rodrigues MA, Renvert S, Bianchini MA (2017) Risk indicators for Peri-implantitis. A cross-sectional study with 916 implants. Clin Oral Implants Res 28(2);144–50. https://doi.org/10.1111/clr.12772
Zandim-Barcelos DL, Carvalho GG, Sapata VM, Villar CC, Hammerle C, Romito GA (2019) Implant-based factor as possible risk for peri-implantitis. Braz Oral Res 33(suppl 1):e067
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of Shahid Beheshti University of Medical Sciences.
Consent to participate
Written informed consent was obtained from all participants prior to their enrollment.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kadkhodazadeh, M., Amid, R. & Moscowchi, A. Management of extensive peri-implant defects with titanium meshes. Oral Maxillofac Surg 25, 561–568 (2021). https://doi.org/10.1007/s10006-021-00955-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10006-021-00955-x