Abstract
The present study aimed to examine the association between the presence, number, and type of positive psychotic symptoms (PPS) and clinical severity in adolescent patients. Five hundred-six patients aged 11–17 years were assigned to either the noPPS (n = 341), the delusional beliefs only (del; n = 32), the hallucinations only (hall; n = 80), or the delusional beliefs and hallucinations (del&hall; n = 53) group. Generalized Structural Equation Modeling was applied to identify the best-fitting model representing clinical severity indicated by psychiatric diagnoses, depressivity, personality pathology, non-suicidal self-injury, suicide attempts, perceived stress, and psychosocial impairments, assessed by interviews and questionnaires. The groups were compared concerning the final model’s factors. The final model consisted of three factors representing psychopathology and functional impairments, self-harming behavior, and perceived stress (BIC difference to reference model: 103.99). Participants with any PPS scored higher on all factors than the noPPS group (differences in SD: 0.49–1.48). Additionally, the del&hall group scored 1.31 SD higher on psychopathology and functional impairments than the hall group, and 1.16 SD higher on self-harming behavior compared to the del group. Finally, the hall group scored 0.84 SD higher on self-harming behavior than the del group, with no group differences in the other factors. In adolescent patients, the presence of PPS may represent a marker for a more severe form of mental disorder, with hallucinations being indicative of self-harming behavior. Early transdiagnostic assessment of PPS seems indicated as it may inform treatment in the context of clinical staging.
Similar content being viewed by others
Introduction
Psychotic symptoms exist as a continuum in terms of severity, associated distress, and their effects on functioning and help-seeking behavior [1,2,3,4]. While psychotic experiences (PEs) occur across the lifespan, they are particularly prevalent in young people, with a median prevalence of 7.5% [5,6,7,8,9]. Adolescents with PEs are nearly three times more likely to be diagnosed with a non-psychotic disorder and four times more likely to be diagnosed with a psychotic disorder [10,11,12]. In addition, PEs in adolescence have been found to be associated with a greater number of co-occurring psychiatric diagnoses [6, 10], higher levels of depressive symptoms [13, 14], greater personality pathology [15], higher levels of subjectively perceived stress [16], and poorer social and global functioning [17,18,19]. A strong link with PEs has also been found with self-harming behavior [20,21,22,23,24], with individuals with PEs having shown threefold increased odds for non-suicidal self-injury (NSSI) and suicide attempts [25, 26], and fourfold increased odds of suicide death [27]. When the relationship between different PEs subtypes (e.g., visual and auditory hallucinations, mind reading, referential ideas, and persecutory delusions) and self-harming behavior was examined, only auditory and visual hallucinatory experiences remained significant predictors after controlling for confounding factors, such as depression [21, 28]. Overall, PEs during adolescence are seen as a non-pathognomic risk maker for negative long-term outcomes, including mental health problems and functional impairments [12, 29, 30]. Accordingly, identifying those young people with such markers or early signs of mental disorder is a crucial precondition for indicated prevention and early intervention efforts in order to prevent negative long-term outcomes. A key shortcoming of the current empirical evidence on the clinical significance of PEs in adolescents is that it is mainly community-based, relying on potentially inflated self-reports [31]. Consequently, it is still unclear whether psychotic symptoms are also an indicator of greater clinical severity in help-seeking youth, where they could inform treatment selection and planning in the context of a clinical staging approach [32]. Given the rising demand and decreasing resources for youth mental health services, understanding the maximum intensity of treatment needed for each individual is crucial. To close this gap, the current study aimed at examining the link between the presence, the number of, and the type of positive psychotic symptoms (PPS; delusional beliefs and hallucinations) and clinical severity in a help-seeking, transdiagnostic sample of adolescents. We applied an explorative latent modeling approach that allowed us to consider multiple indicators of clinical severity (e.g., number of psychiatric diagnoses, psychosocial impairments, self-harming behavior, etc.) simultaneously in a single statistical model and to explore the impact of psychotic symptoms on the factor structure that represents clinical severity. Based on previous research, we hypothesized that (1) individuals with hallucinations and/or delusional beliefs would show greater clinical severity than individuals without PPS [10,11,12,13,14,15,16,17,18,19], (2) that individuals with both hallucinations and delusional beliefs would show greater clinical severity than individuals with only hallucinations or delusional beliefs [6], and (3) that individuals who experience hallucinations only would particularly show more self-harming behavior than individuals who experience delusional beliefs only [21, 28].
Methods
Participants and procedures
The sample of this study (N = 506) stems from two cohort studies conducted at the University Hospital of Child and Adolescent Psychiatry and Psychotherapy, University of Bern, Switzerland. Participants were consecutively recruited from general psychiatric inpatient and day-care services (“Bernese Basic Documentation” [BeBaDoc] sample), and a specialized outpatient clinic for risk-taking behavior and self-harm (“Ambulanz für Risikoverhalten und Selbstschädigung” [AtR!Sk]) sample). Inclusion criteria were: 11–18 years of age (BeBaDoc sample), 12–17 years of age (AtR!Sk sample), self-harming or risk-taking behavior (AtR!Sk sample), and sufficient fluency in German language skills. Exclusion criteria were patients lacking capacity to understand the study details or provide informed consent. Written informed consent was obtained from all participants, as well as from a parent or legal guardian for those under the age of 14 years. Assessments were conducted by trained clinicians (AtR!Sk) or trained doctoral and psychology students (BeBaDoc). In the AtR!Sk study, assessments formed part of the routine diagnostic assessment procedure at entry to the clinic and therefore participants were not reimbursed. BeBaDoc participants received the equivalent of 20CHF worth of vouchers. Both studies were approved by the local ethics committee (BeBaDoc Ethics ID: 2018–01339; and AtR!Sk Ethics ID: 2018–00942).
Measures
Demographic data
Information was collected using a standardized set of interview questions to assess age, sex, and school type.
Assessment of psychiatric diagnoses and positive psychotic symptoms (PPS)
The Mini International Neuropsychiatric Interview for Children and Adolescents (MINI-KID; [33]) was used to rate current psychiatric disorders. Diagnosis was included in the analyses as a categorical variable with three levels: no diagnosis, one diagnosis, and two or more diagnoses. In addition, specific items from the section on assessment of psychotic disorders and affective disorders with psychotic features were used to assess delusional beliefs (present at the time of the interview) and hallucinations (occurrence in the past month; a full list of items is provided in the Supplementary Material [SM]). A group variable for the occurrence of PPS with the following mutually exclusive categories was created: no occurrence of PPS (noPPS), delusional beliefs only (del), hallucinations only (hall), and co-occurring delusional beliefs and hallucinations (del&hall). Borderline personality disorder (BPD) was assessed using the corresponding section of the Structured Clinical Interview for DSM-IV Axis II (SCID-II) [34, 35].
Personality functioning
The Semi-structured Interview for DSM-5 Personality Functioning (STiP-5.1; [36]) assesses impairment in self- and interpersonal functioning according to the alternative DSM-5 model for personality disorders (AMPD; [37]). The interviewer scores the degree of impairment in each facet on the Personality Functioning Scale (LPFS; [38]), ranging from 0 (no impairment) to 4 (extreme impairment). For the analyses, the mean score of the two domain scores (self- and interpersonal functioning) was used, which in turn were composed of the mean of their underlying three facets each.
Depression severity
The Children’s Depression Rating Scale (CDRS; [39]), a 16-item semi-structured interview, was used to determine the severity of depression. Items were rated on a scale of 1 (no particular problems) to 7 (severe, clinically significant problems), respectively 1 to 5 for the items on sleep, appetite, and speech rate. The sum score was used for analyses.
Psychosocial functioning
The Social and Occupational Functioning Assessment Scale (SOFAS; [40]) was used in the AtR!Sk sample and the Children’s Global Assessment Scale (CGAS; [41]) in the BeBaDoc sample. Both are clinician-rated measures of global functional capacity, with scores ranging from 0 (minimum functional capacity) to 100 (maximum functional capacity). For the analyses, scores were standardized.
Perceived stress
The Perceived Stress Scale (PSS; [42]) was used to assess non-specific stress. Items were rated on a score from 0 (never) to 4 (very often). The sum score ranging range from 0 to 40 was used for analyses.
NSSI and suicide attempts
According to the DSM-5, NSSI is the intentional damage of body tissue without suicidal intention for socially unsanctioned purposes; and a suicide attempt is a self-initiated sequence of behaviors by an individual who, at the time of initiation, expects that the set of actions would lead to his or her own death [37]. The Self-Injurious Thoughts and Behaviors Interview (SITBI) was used to assess the number of days with NSSI incidents and the frequency of suicide attempts in the last year [43]. NSSI incidents in the last year were included in the analyses as a categorical variable with three levels according to criterion A of the DSM-5 diagnosis of Non-suicidal Self-Injury (i.e., no incidents, NSSI on one to 4 days [subthreshold], NSSI on 5 or more days [criterion A fulfilled]; [37]). Suicide attempts in the last year were operationalized with a three-level categorical variable (i.e., no attempts, one attempt, two or more attempts).
Statistical analyses
Missing value analyses revealed less than 5% missing values in all variables. We performed available-case analyses. To examine clinical severity at the latent level, we first fitted a structural equation model (SEM) with one single factor overarching all indicators (i.e., depressivity, psychosocial functioning, perceived stress, personality functioning, suicide attempts, NSSI incidents, number of diagnoses) as a baseline model. Its global model fit was evaluated using the Comparative Fit Index (CFI), the Standardized Root Mean Square Residuals (SRMR), and the Root Mean Square Error of Approximation (RMSEA) [44]. The SEM was then compared to a Generalized Structural Equation Model (GSEM) with the same model structure, as it is better suited for ordinal data present in three of the indicators (i.e., number of diagnoses, NSSI incidents, and suicide attempts; [45]). Finally, a GSEM, including the PPS group variable and covariates (i.e., sex, age, sample [AtR!Sk, BeBaDok]) loading as predictors on the factor, was fitted and compared with the simple GSEM, using the Likelihood-Ratio Test. To determine if a more complex factor structure could more accurately explain the data, we tested every possible 2- and 3-factor GSEM model structure with the seven designated indicators (n = 560). Analyses were performed with 1000 iterations for each model structure with covariates and the dummy coded PPS group variable loading on every latent factor. Given seven indicators, we limited our analysis to models with no more than three factors to maintain analytical parsimony. The error terms of the factors were allowed to correlate because a common measurement error was expected. The best-fitting model of all possible factor combinations, selected for its lowest Bayesian Information Criterion (BIC), provided the factor composition that was contrasted between the groups to answer our research questions. To test the hypotheses, differences in the latent factor(s) of the best-fitting model between the PPS groups were examined using contrasts (hypothesis 1 [presence]: noPSS versus PPS [i.e., del, hall, del&hall]; hypothesis 2 [number]: del&hall vs. del, del&hall vs. hall; hypothesis 3 [type]: del vs. hall). Group differences in standard deviation (DSD) with confidence intervals were calculated as effect size measures [46], with a DSD of at least 0.5 being considered as clinically relevant [47]. To assess if psychotic disorders influenced the effects, we recalculated the best-fitting model and contrasts after excluding patients with a psychotic disorder (ICD-10 F2 diagnosis; sensitivity analysis). Analyses were performed in Stata 17 [48] and Mplus (Version 8.10; [49]). An alpha level of 0.05 was applied.
Results
Sample characteristics
Of 643 patients who were eligible (BeBaDoc: n = 344, 53, 5%; AtR!Sk: n = 299, 46.5%), 75 (11.7%) did either not give informed consent or dropped out after consent (BeBaDoc: n = 42, 6.5%; AtR!Sk: n = 33, 5.1%). In addition, 42 (6.5%) participants were excluded because of duplicate measurements or participation in both studies (BeBaDoc: n = 22, 3.4%; AtR!Sk: n = 20, 3.1%). Of the 526 remaining participants, 20 (3.1%) were excluded due to missing data on the PPS group variable, leaving a total of N = 506 (78.7%) for analyses. Sociodemographic and clinical characteristics are reported in Table 1.
Latent representation of clinical severity
The 1-factor SEM performed acceptable (RMSEA = 0.074; 90% confidence interval [CI]: 0.053, 0.096) to excellent (CFI = 0.961; SRMR = 0.041; [50, 51]). The GSEM, better suited for ordinal data [45], showed similar results to the SEM (see Table 2). Finally, the likelihood ratio test comparing the 1-factor GSEM with and without predictors was significant, indicating that the inclusion of the predictors significantly improved the model fit (χ2 [6] = 116.20, p < 0.001).
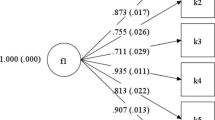
The exploratory analyses of all possible 2- and 3-factor models given the seven selected indicators showed that using the BIC as criterion for good model fit, a 3-factor model appeared to fit the data best (BIC: 7183.84). This best-fitting 3-factor model showed a difference of more than ten relative to the 1-factor GSEM (BIC: 7287.83) and the next best convergent multifactorial model (BIC: 7222.34), indicating very strong evidence for better model fit [52, 53]. The factor structure we derived through this model selection process can be seen in Fig. 1, where we labeled the three factors based on their indicators as psychopathology and functional impairments, self-harming behavior, and perceived stress. The factors’ error terms were moderately to strongly correlated with each other. See SM for the complete results for the 1-factor and the best-fitting 3-factor GSEM. As Stata’s GSEM module did not allow the necessary parameter restriction of the Stress factor to estimate its error variance in an interpretable way (setting error variance of manifest indicator to zero or including manifest indicator instead of factor not possible), we fitted an equivalent model in Mplus, where Stress was included as a manifest variable. This model showed the same loglikelihood (H0 value = − 3461.17; see SM for complete results), confirming the validity of the final model.
The best-fitting multifactorial model (GSEM) with three factors. N = 506. Coefficients are unstandardized unless otherwise stated. Path coefficients of the control variables Sex, Age, and Sample have been omitted for presentation reasons. Covariances of the latent factors are standardized. Complete results can be found in SM. aCoefficients of the three dummy-coded variables representing the PPS group variable have been omitted from this figure for simplicity, as they do not allow any meaningful interpretation. bStandardized coefficients. cCoefficient in unstandardized log odds calculated using ordered logistic regression. Odds ratio in parentheses. *** indicates p < .001, ** indicates p < .01
Hypotheses testing
When testing hypothesis 1, adolescents with PPS (del, hall, or del and hall) scored significantly higher on psychopathology and functional impairments (DSD = −1.48, 95% CI − 1.99, −0.98), self-harming behavior (DSD = − 0.49, 95% CI − 0.84, − 0.14), and perceived stress (DSD = − 0.53, 95% CI − 0.70, − 0.35) compared with adolescents without PPS (see Table 3 for contrasts and SM for a graphical representation of their magnitude). Additional exploratory post-hoc analyses revealed that adolescents with hallucinations only had significantly higher scores on all three factors (psychopathology and functional impairments: DSD = − 0.79, 95% CI − 1.31, − 0.27; self-harming behavior: DSD = − 0.66, 95% CI − 1.10, − 0.23; perceived stress: DSD = − 0.44, 95% CI − 0.66, − 0.22), while those with delusional beliefs only showed higher scores on psychopathology and functional impairments (DSD = -1.56, 95% CI −2.38, − 0.75) and perceived distress (DSD = − 0.54, 95% CI − 0.87, -0.21) but not self-harming behavior when compared with those without PPS.
Testing hypothesis 2 revealed that adolescents with both delusional beliefs and hallucinations demonstrated comparable scores of psychopathology and functional impairments and perceived stress, but greater scores of self-harming behavior (DSD = − 1.16, 95% CI − 1.95, − 0.36), compared with adolescents with delusional beliefs only. In contrast, when compared to adolescents with hallucinations only, adolescents with both delusional beliefs and hallucinations scored higher on psychopathology and functional impairments (DSD = − 1.31, 95% CI − 2.06, − 0.56), with comparable scores for self-harming behavior and perceived stress. Finally, the examination of hypothesis 3 showed that adolescents with hallucinations only had a higher self-harming behavior score than adolescents reporting delusional beliefs only (DSD = − 0.84, 95% CI − 1.50, 0.18). In contrast, no group differences were found for psychopathology and functional impairments, and perceived stress. To better understand the group difference in self-harming behavior, we additionally explored whether participants with delusional beliefs only and those with hallucinations only differed in NSSI and suicide attempts, respectively, using two separate ordered logistic regressions. Adolescents experiencing hallucinations only were 4.29 (95% CI 1.61, 11.45) times more likely to report more frequent NSSI than individuals with delusional beliefs only (Model: Chi2 [6] = 148.03, p < 0.001, n = 499; see SM for complete results). No significant group difference was found for suicide attempts (OR = 2.12, p = 0.108; Model: Chi2 [6] = 31.86, p < 0.001, n = 500; see SM for complete results). The sensitivity analysis revealed no differences in results when participants with a psychotic disorder were excluded.
Discussion
This study examined PPS as a marker of clinical severity in a help-seeking, transdiagnostic sample of adolescents using a latent modeling approach. Four main findings emerged: First, clinical severity was best represented by three latent factors; psychopathology and functional impairments overarching general indices of psychopathology (i.e., depressivity, personality functioning, and number of psychiatric diagnoses) and impairments in psychosocial functioning, self-harming behavior represented by NSSI and suicide attempts, and perceived stress. The factor psychopathology and functional impairments is consistent with the p factor; a latent dimension that represents covariation among all forms of psychopathology [54]. Recent studies suggest that the p factor may also be relevant for the understanding of psychopathology in children and adolescents [55,56,57], and that personality pathology can be meaningfully included alongside general psychopathology in a joint personality-psychopathology framework in youth [58]. The differentiation of the self-harming behavior from the psychopathology and functional impairments factor is in line with evidence indicating that self-harm occurs across a variety of internalizing and externalizing psychopathology and personality pathology, and may thus represent a transdiagnostic marker of greater clinical severity [59]. Moreover, the two components of this factor, NSSI and suicide attempts, show shared etiological factors, biological correlates, and genetic overlap [60]. The identification of a perceived stress factor may reflect that the experience of general subjective distress is different from the other psychopathology- and risk-based indices of clinical severity. Another reason could be stress being the only construct measured through self-report [61]. Second, in comparison to adolescents without PPS, those with at least one PPS showed higher scores on all factors (except for the delusions only group, which did not differ in self-harming behavior compared to the no PPS group). Third, adolescents with two PPS scored higher on psychopathology and functional impairments when compared to those with hallucinations only, and higher on self-harming behavior when compared to those with delusional beliefs only. Fourth, adolescents with hallucinations or delusional beliefs only differed from each other only regarding self-harming behavior, with higher scores for the former group. Post-hoc analyses revealed that this group difference was mainly based on more frequent NSSI in the stand-alone hallucinations group, with no group difference in the frequency of suicide attempts. The effect sizes for the group differences were at or above the threshold of 0.5 SD, supporting the clinical relevance of the findings. Taken together, these findings extend previous community-based research that found PE during adolescence to be a risk maker for negative long-term outcomes (e.g., mental health problems and functional impairments) by demonstrating that in help-seeking adolescents the presence of PPS indicates a more severe form of mental disorder, with hallucinations being particularly indicative of an increased risk for self-harming behavior such as NSSI. The fact that the results remained stable when adolescents with psychotic disorders were removed from the analyses underscores the transdiagnostic relevance of the findings and is consistent with the hypothesis that psychotic thought processes are a sign of peak severity [54]. Thereby, adolescents experiencing both hallucinations and delusions appear to lie at the top end of the clinical severity continuum, which may not just be due to a coincidental cumulative effect of an additional psychotic symptom, but to a specific dynamic caused by higher etiological loading (i.e., higher levels of exposure to genetic and environmental risk factors). This interpretation is supported by studies showing that the co-occurrence of hallucinations and delusions is more common than expected by chance [62,63,64]. The differential results for hallucinations and delusional beliefs confirm earlier community-based findings demonstrating hallucinatory experiences being more consistently linked to self-harming behavior than other types of PPS [28, 65, 66]. Notably, auditory hallucinations in clinical samples have more negative content (e.g., commands to harm oneself) compared to non-clinical samples [67], substantially increasing the risk for self-harming behavior [65, 68, 69]. Strengths of this study include the large sample consisting of adolescent in- and outpatients of the primary public mental health service in the region; the comprehensive diagnostic assessment through standardized clinical interviews conducted by highly trained researchers or mental health professionals; the latent modeling approach allowing to simultaneously examine the relationship between several indicators of clinical severity and PPS that has to date mostly been examined in separate studies; and the consideration of personality pathology along with general psychopathology, self-harming behavior, perceived stress, and psychosocial functioning as indicators of clinical severity. In accordance with the new dimensional models for personality disorders outlined in DSM-5 and ICD-11 [37, 70], both the level of impairment in personality functioning (STiP-5.1) and the diagnostic criteria for BPD (SCID-II) were assessed. While the diagnosis of personality disorders in adolescents remains a subject of ongoing debate [71,72,73], compelling evidence suggests that (B) PD is reliable and valid diagnosis in adolescents and that early detection and intervention can exert a profound influence on the life trajectories of the affected young people, underscoring the significance of timely identification and support [74,75,76]. We also acknowledge several limitations: First, PPS were assessed using the MINI-KID, which is not a specialized instrument for psychotic symptoms or disorders and did not allow for the differentiation of variants of PPS. Second, due to the relatively small sample sizes of the group with only delusions (del; n = 32) and the group with delusional beliefs and hallucinations (del&hall; n = 53), smaller group differences may not have reached statistical significance due to low statistical power (Type II error). Third, although the BIC we used as criterion for model selection, which aims to strike a balance between goodness of fit and overfitting through a penalty term for the number of parameters [52], it does not eliminate the possibility of choosing an incorrect model [77]. We acknowledge that it can’t be ruled out that the high correlation of the factor’s error terms could be a sign of overfitting and want to emphasize that the latent modeling approach was explorative, meaning that the identified factor structure needs to be validated in other clinical samples to ensure robustness and generalizability. Finally, since we did not test for multiple hierarchies, we cannot rule out that a latent model with several hierarchical levels would better fit the data than the identified three-factor model. Future longitudinal studies are warranted to investigate the association between PPS and clinical severity over time, applying gold-standard measures of psychotic symptoms for clinical populations.
To conclude, we found PPS being a marker for greater clinical severity in help-seeking adolescents, with the presence of hallucinations being indicative for increased risk of self-harm, particularly NSSI. Clinically, this demonstrates the need for routine transdiagnostic assessment of psychotic symptoms, as it can help to identify youth with a more severe form of mental disorder and risk for self-harm who are in need of more intense treatment. Thus, in the context of clinical staging models, psychotic symptoms may serve as a transdiagnostic marker that informs treatment selection and planning, and improves allocation of limited resources in adolescent mental health services [32, 78].
Data availability
Can be requested from the corresponding author.
Code availability
Can be requested from the corresponding author.
References
Johns LC, Kompus K, Connell M et al (2014) Auditory verbal hallucinations in persons With and without a need for care. Schizophr Bull 40:S255–S264. https://doi.org/10.1093/schbul/sbu005
Moseley P, Powell A, Woods A et al (2022) Voice-hearing across the continuum: a phenomenology of spiritual voices. Schizophr Bull 48:1066–1074. https://doi.org/10.1093/schbul/sbac054
Stip E, Letourneau G (2009) Psychotic symptoms as a continuum between normality and pathology. Can J Psychiatry 54:140–151. https://doi.org/10.1177/070674370905400302
Verdoux H, van Os J (2002) Psychotic symptoms in non-clinical populations and the continuum of psychosis. Schizophr Res 54:59–65. https://doi.org/10.1016/S0920-9964(01)00352-8
Kelleher I, Connor D, Clarke MC et al (2012) Prevalence of psychotic symptoms in childhood and adolescence: a systematic review and meta-analysis of population-based studies. Psychol Med 42:1857–1863. https://doi.org/10.1017/S0033291711002960
Kelleher I, Keeley H, Corcoran P et al (2012) Clinicopathological significance of psychotic experiences in non-psychotic young people: evidence from four population-based studies. Br J Psychiatry 201:26–32. https://doi.org/10.1192/bjp.bp.111.101543
Linscott RJ, van Os J (2013) An updated and conservative systematic review and meta-analysis of epidemiological evidence on psychotic experiences in children and adults: on the pathway from proneness to persistence to dimensional expression across mental disorders. Psychol Med 43:1133–1149. https://doi.org/10.1017/S0033291712001626
Rubio JM, Sanjuán J, Flórez-Salamanca L, Cuesta MJ (2012) Examining the course of hallucinatory experiences in children and adolescents: a systematic review. Schizophr Res 138:248–254. https://doi.org/10.1016/j.schres.2012.03.012
Staines L, Healy C, Murphy F et al (2023) Incidence and persistence of psychotic experiences in the general population: systematic review and meta-analysis. Schizophr Bull 49:1007–1021. https://doi.org/10.1093/schbul/sbad056
Healy C, Brannigan R, Dooley N et al (2019) Childhood and adolescent psychotic experiences and risk of mental disorder: a systematic review and meta-analysis. Psychol Med 49:1589–1599. https://doi.org/10.1017/S0033291719000485
Healy C, Coughlan H, Clarke M et al (2020) What mediates the longitudinal relationship between psychotic experiences and psychopathology? J Abnorm Psychol 129:505–516. https://doi.org/10.1037/abn0000523
McGrath JJ, Saha S, Al-Hamzawi A et al (2016) The bidirectional associations between psychotic experiences and DSM-IV mental disorders. Am J Psychiatry 173:997–1006. https://doi.org/10.1176/appi.ajp.2016.15101293
Barragan M, Laurens KR, Navarro JB, Obiols JE (2011) Psychotic-like experiences and depressive symptoms in a community sample of adolescents. Eur Psychiatry 26:396–401. https://doi.org/10.1016/j.eurpsy.2010.12.007
Núñez D, Monjes P, Campos S, Wigman JTW (2021) Evidence for specific associations between depressive symptoms, psychotic experiences, and suicidal ideation in chilean adolescents from the general population. Front Psychiatry 11:552343. https://doi.org/10.3389/fpsyt.2020.552343
Peters EM, Yates K, DeVylder J et al (2022) Understanding the inverse relationship between age and psychotic symptoms: the role of borderline personality traits. Acta Psychiatr Scand 146:484–491. https://doi.org/10.1111/acps.13475
Turley D, Drake R, Killackey E, Yung AR (2019) Perceived stress and psychosis: the effect of perceived stress on psychotic-like experiences in a community sample of adolescents. Early Interv Psychiatry 13:1465–1469. https://doi.org/10.1111/eip.12795
Carey E, Gillan D, Healy C et al (2021) Early adult mental health, functional and neuropsychological outcomes of young people who have reported psychotic experiences: a 10-year longitudinal study. Psychol Med 51:1861–1869. https://doi.org/10.1017/S0033291720000616
Healy C, Campbell D, Coughlan H et al (2018) Childhood psychotic experiences are associated with poorer global functioning throughout adolescence and into early adulthood. Acta Psychiatr Scand 138:26–34. https://doi.org/10.1111/acps.12907
Kelleher I, Wigman JTW, Harley M et al (2015) Psychotic experiences in the population: association with functioning and mental distress. Schizophr Res 165:9–14. https://doi.org/10.1016/j.schres.2015.03.020
Bromet EJ, Nock MK, Saha S et al (2017) Association between psychotic experiences and subsequent suicidal thoughts and behaviors: A cross-national analysis from the world health organization world mental health surveys. JAMA Psychiat 74:1136. https://doi.org/10.1001/jamapsychiatry.2017.2647
Hielscher E, Connell M, Lawrence D et al (2019) Association between psychotic experiences and non-accidental self-injury: results from a nationally representative survey of adolescents. Soc Psychiatry Psychiatr Epidemiol 54:321–330. https://doi.org/10.1007/s00127-018-1629-4
Hielscher E, DeVylder J, Hasking P et al (2021) Mediators of the association between psychotic experiences and future non-suicidal self-injury and suicide attempts: results from a three-wave, prospective adolescent cohort study. Eur Child Adolesc Psychiatry 30:1351–1365. https://doi.org/10.1007/s00787-020-01593-6
Kelleher I, Ramsay H, DeVylder J (2017) Psychotic experiences and suicide attempt risk in common mental disorders and borderline personality disorder. Acta Psychiatr Scand 135:212–218. https://doi.org/10.1111/acps.12693
Steenkamp LR, De Neve-Enthoven NGM, João AM et al (2023) Psychotic experiences, suicidality and non-suicidal self-injury in adolescents: independent findings from two cohorts. Schizophr Res 257:50–57. https://doi.org/10.1016/j.schres.2023.05.006
Honings S, Drukker M, Groen R, van Os J (2016) Psychotic experiences and risk of self-injurious behaviour in the general population: a systematic review and meta-analysis. Psychol Med 46:237–251. https://doi.org/10.1017/S0033291715001841
Yates K, Lång U, Cederlöf M et al (2019) Association of psychotic experiences with subsequent risk of suicidal ideation, suicide attempts, and suicide deaths: a systematic review and meta-analysis of longitudinal population studies. JAMA Psychiat 76:180. https://doi.org/10.1001/jamapsychiatry.2018.3514
Sharifi V, Eaton WW, Wu LT et al (2015) Psychotic experiences and risk of death in the general population: 24–27 year follow-up of the epidemiologic catchment area study. Br J Psychiatry 207:30–36. https://doi.org/10.1192/bjp.bp.113.143198
Capra C, Kavanagh DJ, Hides L, Scott JG (2015) Subtypes of psychotic-like experiences are differentially associated with suicidal ideation, plans and attempts in young adults. Psychiatry Res 228:894–898. https://doi.org/10.1016/j.psychres.2015.05.002
van Os J, Reininghaus U (2016) Psychosis as a transdiagnostic and extended phenotype in the general population. World Psychiatry 15:118–124. https://doi.org/10.1002/wps.20310
Wigman JTW, van Nierop M, Vollebergh WAM et al (2012) Evidence that psychotic symptoms are prevalent in disorders of anxiety and depression, impacting on illness onset, risk, and severity-implications for diagnosis and ultra-high risk research. Schizophr Bull 38:247–257. https://doi.org/10.1093/schbul/sbr196
Schultze-Lutter F, Renner F, Paruch J et al (2014) Self-reported psychotic-like experiences are a poor estimate of clinician-rated attenuated and frank delusions and hallucinations. Psychopathology 47:194–201. https://doi.org/10.1159/000355554
Shah JL, Scott J, McGorry PD et al (2020) Transdiagnostic clinical staging in youth mental health: a first international consensus statement. World Psychiatry 19:233–242. https://doi.org/10.1002/wps.20745
Sheehan DV, Sheehan KH, Shytle RD et al (2010) Reliability and validity of the mini international neuropsychiatric interview for children and adolescents (MINI-KID). J Clin Psychiatry 71:313–326. https://doi.org/10.4088/JCP.09m05305whi
Chanen AM, Jovev M, Djaja D et al (2008) Screening for borderline personality disorder in outpatient youth. J Personal Disord 22:353–364. https://doi.org/10.1521/pedi.2008.22.4.353
First MB, Gibbon M (2004) The structured clinical interview for DSM-IV Axis I disorders (SCID-I) and the structured clinical interview for DSM-IV Axis II disorders (SCID-II). Comprehensive handbook of psychological assessment, Vol 2: personality assessment. John Wiley & Sons Inc., Hoboken, NJ, US, pp 134–143
Hutsebaut J, Berghuis H, De Saeger H, et al (2014) Semi-Structured Interview for Personality Functioning DSM-5 (STiP 5.1). Podium DSM-5 Res Group Neth Cent Expert Personal Disord Utrecht Neth Trimbos Inst 15 198 207
Association AP, Association AP (2013) Diagnostic and statistical manual of mental disorders: DSM-5, 5th edn. American Psychiatric Association, Washington, D.C.
Bender DS, Morey LC, Skodol AE (2011) Toward a model for assessing level of personality functioning in DSM–5, part I: a review of theory and methods. J Pers Assess 93:332–346. https://doi.org/10.1080/00223891.2011.583808
Poznanski EO, Mokros HB (1996) Children’s depression rating scale, revised (CDRS-R). West Psychol Serv Los Angel
Goldman HH, Skodol AE, Lave TR (1992) Revising axis V for DSM-IV: a review of measures of social functioning. Am J Psychiatry 149:9
Shaffer D (1983) A children’s global assessment scale (CGAS). Arch Gen Psychiatry 40:1228. https://doi.org/10.1001/archpsyc.1983.01790100074010
Cohen S, Kamarck T, Mermelstein R (1983) A global measure of perceived stress. J Health Soc Behav 24:385. https://doi.org/10.2307/2136404
Fischer G, Ameis N, Parzer P et al (2014) The German version of the self-injurious thoughts and behaviors interview (SITBI-G): a tool to assess non-suicidal self-injury and suicidal behavior disorder. BMC Psychiatry 14:265. https://doi.org/10.1186/s12888-014-0265-0
Boomsma A (2000) Reporting analyses of covariance structures. Struct Equ Model Multidiscip J 7:461–483. https://doi.org/10.1207/S15328007SEM0703_6
Muthén B (1984) A general structural equation model with dichotomous, ordered categorical, and continuous latent variable indicators. Psychometrika 49:115–132. https://doi.org/10.1007/BF02294210
Draak THP, De Greef BTA, Faber CG et al (2019) The minimum clinically important difference: which direction to take. Eur J Neurol 26:850–855. https://doi.org/10.1111/ene.13941
Norman GR, Sloan JA, Wyrwich KW (2003) Interpretation of changes in health-related quality of life: the remarkable universality of half a standard deviation. Med Care 41:582–592. https://doi.org/10.1097/01.MLR.0000062554.74615.4C
StataCorp (2021) Stata Statistical Software: Release 17. StataCorp LLC, College Station, TX
Muthén LK, Muthén B (2017) Mplus user’s guide: Statistical analysis with latent variables, User’s guide (Version 8). Muthén & Muthén, Los Angeles, CA
Hu L, Bentler PM (1999) Cutoff criteria for fit indexes in covariance structure analysis: conventional criteria versus new alternatives. Struct Equ Model Multidiscip J 6:1–55. https://doi.org/10.1080/10705519909540118
Hu L, Bentler PM (1998) Fit indices in covariance structure modeling: sensitivity to underparameterized model misspecification. Psychol Methods 3:424–453. https://doi.org/10.1037/1082-989X.3.4.424
Neath AA, Cavanaugh JE (2012) The bayesian information criterion: background, derivation, and applications. WIREs Comput Stat 4:199–203. https://doi.org/10.1002/wics.199
Raftery AE (1995) Bayesian model selection in social research. Sociol Methodol 25:111. https://doi.org/10.2307/271063
Caspi A, Moffitt TE (2018) All for one and one for all: mental disorders in one dimension. Am J Psychiatry 175:831–844. https://doi.org/10.1176/appi.ajp.2018.17121383
Haltigan JD, Aitken M, Skilling T et al (2018) “P” and “DP:” examining symptom-level bifactor models of psychopathology and dysregulation in clinically referred children and adolescents. J Am Acad Child Adolesc Psychiatry 57:384–396. https://doi.org/10.1016/j.jaac.2018.03.010
Murray AL, Eisner M, Ribeaud D (2016) The development of the general factor of psychopathology ‘p factor’ through childhood and adolescence. J Abnorm Child Psychol 44:1573–1586. https://doi.org/10.1007/s10802-016-0132-1
Ronald A (2019) Editorial: The psychopathology p factor: will it revolutionise the science and practice of child and adolescent psychiatry? J Child Psychol Psychiatry 60:497–499. https://doi.org/10.1111/jcpp.13063
Shields AN, Giljen M, España RA, Tackett JL (2021) The p factor and dimensional structural models of youth personality pathology and psychopathology. Curr Opin Psychol 37:21–25. https://doi.org/10.1016/j.copsyc.2020.06.005
Kaess M (2022) Self-harm: a transdiagnostic marker of psychopathology and suicide risk during the COVID-19 pandemic? Eur Child Adolesc Psychiatry 31:1–3. https://doi.org/10.1007/s00787-022-02044-0
Maciejewski DF, Creemers HE, Lynskey MT et al (2014) Overlapping genetic and environmental influences on nonsuicidal self-injury and suicidal ideation: different outcomes, same etiology? JAMA Psychiat 71:699. https://doi.org/10.1001/jamapsychiatry.2014.89
Bowling A (2005) Mode of questionnaire administration can have serious effects on data quality. J Public Health 27:281–291. https://doi.org/10.1093/pubmed/fdi031
Nuevo R, Van Os J, Arango C et al (2013) Evidence for the early clinical relevance of hallucinatory-delusional states in the general population: hallucinatory-delusional states. Acta Psychiatr Scand 127:482–493. https://doi.org/10.1111/acps.12010
Smeets F, Lataster T, van Winkel R et al (2013) Testing the hypothesis that psychotic illness begins when subthreshold hallucinations combine with delusional ideation: hallucinations, delusions and psychosis vulnerability. Acta Psychiatr Scand 127:34–47. https://doi.org/10.1111/j.1600-0447.2012.01888.x
Smeets F, Lataster T, Viechtbauer W, Delespaul P (2015) Evidence that environmental and genetic risks for psychotic disorder may operate by impacting on connections between core symptoms of perceptual alteration and delusional ideation. Schizophr Bull 41:687–697. https://doi.org/10.1093/schbul/sbu122
Hielscher E, DeVylder J, Hasking P et al (2021) Can’t get you out of my head: persistence and remission of psychotic experiences in adolescents and its association with self-injury and suicide attempts. Schizophr Res 229:63–72. https://doi.org/10.1016/j.schres.2020.11.019
Rogers P, Watt A, Gray NS et al (2002) Content of command hallucinations predicts self-harm but not violence in a medium secure unit. J Forensic Psychiatry 13:251–262. https://doi.org/10.1080/09585180210150096
de Boer JN, Corona Hernández H, Gerritse F et al (2022) Negative content in auditory verbal hallucinations: a natural language processing approach. Cognit Neuropsychiatry 27:139–149. https://doi.org/10.1080/13546805.2021.1941831
DeVylder J, Yamasaki S, Ando S et al (2023) Attributes of auditory hallucinations that are associated with self-harm: a prospective cohort study. Schizophr Res 251:30–36. https://doi.org/10.1016/j.schres.2022.12.008
Shawyer F, Mackinnon A, Farhall J et al (2003) Command hallucinations and violence: implications for detention and treatment. Psychiatry Psychol Law 10:97–107. https://doi.org/10.1375/pplt.2003.10.1.97
World Health Organization (2024) Clinical descriptions and diagnostic requirements for ICD-11 mental, behavioural and neurodevelopmental disorders. World Health Organization, Geneva
Tyrer P (2022) Debate: young people with personality disorder should be recognised and appropriately managed. Child Adolesc Ment Health. https://doi.org/10.1111/camh.12551
Ring D, Lawn S (2019) Stigma perpetuation at the interface of mental health care: a review to compare patient and clinician perspectives of stigma and borderline personality disorder. J Ment Health. https://doi.org/10.1080/09638237.2019.1581337
Cavelti M, Sharp C, Chanen AM, Kaess M (2023) Commentary: commentary on the twitter comments evoked by the may 2022 debate on diagnosing personality disorders in adolescents. Child Adolesc Ment Health 28:186–191. https://doi.org/10.1111/camh.12618
Chanen AM, Nicol K, Nicol K et al (2020) Diagnosis and treatment of borderline personality disorder in young people. Curr Psychiatry Rep 22:1–8. https://doi.org/10.1007/s11920-020-01144-5
Chanen AM, Sharp C, Hoffman P, Alliance G, for Prevention and Early Intervention for Borderline Personality Disorder, (2017) Prevention and early intervention for borderline personality disorder: a novel public health priority. World Psychiatry 16:215–216. https://doi.org/10.1002/wps.20429
Winsper C, Lereya ST, Marwaha S et al (2016) The aetiological and psychopathological validity of borderline personality disorder in youth: a systematic review and meta-analysis. Clin Psychol Rev 44:13–24. https://doi.org/10.1016/j.cpr.2015.12.001
Burnham KP, Anderson DR (2004) Multimodel inference: understanding AIC and BIC in model selection. Sociol Methods Res 33:261–304. https://doi.org/10.1177/0049124104268644
Shah JL, Jones N, van Os J et al (2022) Early intervention service systems for youth mental health: integrating pluripotentiality, clinical staging, and transdiagnostic lessons from early psychosis. Lancet Psychiatry 9:413–422. https://doi.org/10.1016/S2215-0366(21)00467-3
Funding
Open access funding provided by University of Bern. The study was funded from the internal research budget of the University Hospital of Child and Adolescent Psychiatry and Psychotherapy at the University of Bern. Additionally, Marialuisa Cavelti was supported by a grant from the Swiss National Science Foundation (PZ00P1_193279/1).
Author information
Authors and Affiliations
Contributions
J.M.K. and M.C. wrote the main manuscript text and J.M.K. prepared tables 1-3 and figure 1. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
No conflicts of interest present.
Ethical approval
Ethics approval obtained, see section Participants and procedures.
Informed consent
Informed consent obtained, see section Participants and Procedures.
Consent for publication
Not applicable.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kaeser, J.M., Lerch, S., Sele, S. et al. Positive psychotic symptoms as a marker of clinical severity in a transdiagnostic sample of help-seeking adolescents. Eur Child Adolesc Psychiatry (2024). https://doi.org/10.1007/s00787-024-02417-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00787-024-02417-7